Abstract
Purpose
Pretreatment ischemic core volume is conceptually equal to follow-up infarct volume (FIV) in patients with successful recanalization. However, there is sometimes an absolute volume difference (AD) between pretreatment core volume and FIV. The aim was to compare the AD values between the Bayesian and the singular value decomposition (SVD) methods with time from onset-to-imaging in acute ischemic stroke (AIS) patients undergoing mechanical thrombectomy.
Methods
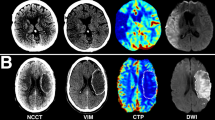
Consecutive AIS patients were included if they had the following: (1) anterior large vessel occlusion (internal carotid or middle cerebral artery); (2) within 24 h of onset; (3) pretreatment CT perfusion (CTP); (4) successful recanalization (mTICI ≥ 2b); and (5) 24-h diffusion-weighted imaging (DWI). FIV was measured on 24-h DWI. The AD value between FIV and the pretreatment core volume was calculated for Bayesian and SVD methods. Spearman’s rank correlation coefficient (rho) was calculated as appropriate.
Results
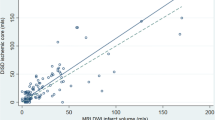
In the 47 patients enrolled (25 men; median age 78 years; median baseline National Institutes of Health Stroke Scale, 22), the median time from onset-to-imaging and onset-to-recanalization was 136 and 220 min, respectively. Shorter onset-to-imaging time was correlated with a larger AD value, and more trend was seen in the SVD method (rho = − 0.28, p = 0.05) compared with the Bayesian method (rho = − 0.08). A larger pretreatment core volume was correlated with a larger AD value, and this tendency was slightly stronger for the SVD (rho = 0.63, p < 0.01) than for the Bayesian (rho = 0.32, p = 0.03) method.
Conclusions
The Bayesian method might be more correlated with FIV than the SVD method in patients with a large ischemic lesion immediately after stroke onset, but not perfect.



Similar content being viewed by others
Data Availability
The anonymized data that support the findings of our study are available from the corresponding author upon reasonable request.
Abbreviations
- AIS:
-
Acute ischemic stroke
- AD:
-
Absolute volume difference
- CBF:
-
Cerebral blood flow
- CBV:
-
Cerebral blood volume
- CTP:
-
Computed tomography perfusion
- DT:
-
Delay time
- DWI:
-
Diffusion-weighted imaging
- FIV:
-
Follow-up infarct volume
- MT:
-
Mechanical thrombectomy
- mTICI:
-
Modified Treatment In Cerebral Infarction
- MTT:
-
Mean transit time
- SVD:
-
Singular value decomposition
- TTP:
-
Time to peak
References
Goyal M, Menon BK, van Zwam WH, Dippel DW, Mitchell PJ, Demchuk AM, Dávalos A, Majoie CB, van der Lugt A, de Miquel MA, Donnan GA, Roos YB, Bonafe A, Jahan R, Diener HC, van den Berg LA, Levy EI, Berkhemer OA, Pereira VM, Rempel J, Millán M, Davis SM, Roy D, Thornton J, Román LS, Ribó M, Beumer D, Stouch B, Brown S, Campbell BC, van Oostenbrugge RJ, Saver JL, Hill MD, Jovin TG, HERMES collaborators (2016) Endovascular thrombectomy after large-vessel ischaemic stroke: a meta-analysis of individual patient data from five randomised trials. Lancet 387:1723–1731
Nogueira RG, Jadhav AP, Haussen DC, Bonafe A, Budzik RF, Bhuva P, Yavagal DR, Ribo M, Cognard C, Hanel RA, Sila CA, Hassan AE, Millan M, Levy EI, Mitchell P, Chen M, English JD, Shah QA, Silver FL, Pereira VM, Mehta BP, Baxter BW, Abraham MG, Cardona P, Veznedaroglu E, Hellinger FR, Feng L, Kirmani JF, Lopes DK, Jankowitz BT, Frankel MR, Costalat V, Vora NA, Yoo AJ, Malik AM, Furlan AJ, Rubiera M, Aghaebrahim A, Olivot JM, Tekle WG, Shields R, Graves T, Lewis RJ, Smith WS, Liebeskind DS, Saver JL, Jovin TG, DAWN Trial Investigators (2018) Thrombectomy 6 to 24 hours after stroke with a mismatch between deficit and infarct. N Engl J Med 378:11–21
Albers GW, Marks MP, Kemp S, Christensen S, Tsai JP, Ortega-Gutierrez S, McTaggart RA, Torbey MT, Kim-Tenser M, Leslie-Mazwi T, Sarraj A, Kasner SE, Ansari SA, Yeatts SD, Hamilton S, Mlynash M, Heit JJ, Zaharchuk G, Kim S, Carrozzella J, Palesch YY, Demchuk AM, Bammer R, Lavori PW, Broderick JP, Lansberg MG, DEFUSE 3 Investigators (2018) Thrombectomy for stroke at 6 to 16 hours with selection by perfusion imaging. N Engl J Med. 378:708–718
Bivard A, Levi C, Krishnamurthy V, McElduff P, Miteff F, Spratt NJ, Bateman G, Donnan G, Davis S, Parsons M (2015) Perfusion computed tomography to assist decision making for stroke thrombolysis. Brain 138:1919–1931
Kudo K, Christensen S, Sasaki M, Ostergaard L, Shirato H, Ogasawara K, Wintermark M, Warach S (2013) Accuracy and reliability assessment of CT and MR perfusion analysis software using a digital phantom. Radiology 267:201–211
Boned S, Padroni M, Rubiera M, Tomasello A, Coscojuela P, Romero N, Muchada M, Rodríguez-Luna D, Flores A, Rodríguez N, Juega J, Pagola J, Alvarez-Sabin J, Molina CA, Ribó M (2017) Admission CT perfusion may overestimate initial infarct core: the ghost infarct core concept. J Neurointerv Surg 9:66–69
d’Esterre CD, Boesen ME, Ahn SH, Pordeli P, Najm M, Minhas P, Davari P, Fainardi E, Rubiera M, Khaw AV, Zini A, Frayne R, Hill MD, Demchuk AM, Sajobi TT, Forkert ND, Goyal M, Lee TY, Menon BK (2015) Time-dependent computed tomographic perfusion thresholds for patients with acute ischemic stroke. Stroke 46:3390–3397
Bivard A, Kleinig T, Miteff F, Butcher K, Lin L, Levi C, Parsons M (2017) Ischemic core thresholds change with time to reperfusion: a case control study. Ann Neurol 82:995–1003
Bouslama M, Ravindran K, Rodrigues GM, Pisani L, Haussen DC, Frankel MR, Nogueira RG (2023) Falsely normal CT perfusion ischemic core readings are common and often associated with deep infarcts. J Neurointerv Surg 15:183–187
Rava RA, Snyder KV, Mokin M, Waqas M, Zhang X, Podgorsak AR, Allman AB, Senko J, Bhurwani MMS, Hoi Y, Davies JM, Levy EI, Siddiqui AH, Ionita CN (2021) Assessment of computed tomography perfusion software in predicting spatial location and volume of infarct in acute ischemic stroke patients: a comparison of Sphere, Vitrea, and RAPID. J Neurointerv Surg 13:130–135
Mouridsen K, Friston K, Hjort N, Gyldensted L, Østergaard L, Kiebel S (2006) Bayesian estimation of cerebral perfusion using a physiological model of microvasculature. Neuroimage 33:570–579
Boutelier T, Kudo K, Pautot F, Sasaki M (2012) Bayesian hemodynamic parameter estimation by bolus tracking perfusion weighted imaging. IEEE Trans Med Imaging 31:1381–1395
Sakai Y, Delman BN, Fifi JT, Tuhrim S, Wheelwright D, Doshi AH, Mocco J, Nael K (2018) Estimation of ischemic core volume using computed tomographic perfusion. Stroke 49:2345–2352
Ichikawa S, Yamamoto H, Morita T (2021) Comparison of a Bayesian estimation algorithm and singular value decomposition algorithms for 80-detector row CT perfusion in patients with acute ischemic stroke. Radiol Med 126:795–803
Rava RA, Snyder KV, Mokin M, Waqas M, Allman AB, Senko JL, Podgorsak AR, Shiraz Bhurwani MM, Hoi Y, Siddiqui AH, Davies JM, Levy EI, Ionita CN (2020) Assessment of a Bayesian Vitrea CT perfusion analysis to predict final infarct and penumbra volumes in patients with acute ischemic stroke: a comparison with RAPID. AJNR Am J Neuroradiol 41:206–212
Benson J, Payabvash S, Salazar P, Jagadeesan B, Palmer CS, Truwit CL, McKinney AM (2015) Comparison of CT perfusion summary maps to early diffusion-weighted images in suspected acute middle cerebral artery stroke. Eur J Radiol 84:682–689
Goyal M, Fargen KM, Turk AS, Mocco J, Liebeskind DS, Frei D, Demchuk AM (2014) 2C or not 2C: defining an improved revascularization grading scale and the need for standardization of angiography outcomes in stroke trials. J Neurointerv Surg 6:83–86
Sasaki M, Kudo K, Boutelier T, Pautot F, Christensen S, Uwano I, Goodwin J, Higuchi S, Ito K, Yamashita F (2013) Assessment of the accuracy of a Bayesian estimation algorithm for perfusion CT by using a digital phantom. Neuroradiology 55:1197–1203
Kudo K, Boutelier T, Pautot F, Honjo K, Hu JQ, Wang HB, Shintaku K, Uwano I, Sasaki M (2014) Bayesian analysis of perfusion-weighted imaging to predict infarct volume: comparison with singular value decomposition. Magn Reson Med Sci 13:45–50
Lansberg MG, O’Brien MW, Tong DC, Moseley ME, Albers GW (2001) Evolution of cerebral infarct volume assessed by diffusion-weighted magnetic resonance imaging. Arch Neurol 58:613–617
Wheeler HM, Mlynash M, Inoue M, Tipirnini A, Liggins J, Bammer R, Lansberg MG, Kemp S, Zaharchuk G, Straka M, Albers GW, DEFUSE 2 Investigators (2015) The growth rate of early DWI lesions is highly variable and associated with penumbral salvage and clinical outcomes following endovascular reperfusion. Int J Stroke 10:723–729
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval and Informed consent
This study protocol was approved by the Faculty of Medicine Research Ethics Committee, Kyorin University, with waiver of informed consent.
Competing interests
This study was supported by the Japan Society for the Promotion of Science KAKENHI (JP21K07468) and SENSHIN Medical Research Foundation. The authors have no competing interests to declare that are relevant to the content of this article.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Kawano, H., Adachi, T., Saito, M. et al. Correlation between pretreatment and follow-up infarct volume using CT perfusion imaging: the Bayesian versus singular value decomposition method. Neurol Sci 44, 2041–2047 (2023). https://doi.org/10.1007/s10072-023-06627-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10072-023-06627-w