Abstract
Introduction
Impaired gait is observed in patients with Parkinson’s disease (PD) in both single-task (ST) and dual-task (DT) conditions. Non-motor symptoms (NMSs), another vital symptom future experienced along the PD disease trajectory, contribute to gait performance in PD. However, whether DT gait performance is indicative of NMS burden (NMSB) remains unknown. This study investigated correlation between NMS and DT gait performance and whether NMSB is reflected in the DT effects (DTEs) of gait parameters in PD.
Methods
Thirty-three idiopathic PD participants were enrolled in this study; the median H-Y staging was 2.5. NMSB was assessed by Non-motor Symptoms Scale (NMSS). Spatiotemporal gait parameters under ST and DT conditions were evaluated by wearable sensors. Gait parameters under ST and DT conditions and DTEs of gait parameters were compared across NMSB groups. The associations between NMS and DTEs of gait parameters were analyzed by correlation analysis and linear regression models.
Results
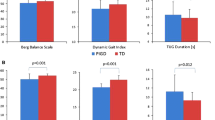
Compared to PD patients with mild-moderate NMSB, the severe-very severe NMSB group showed slower gait speed and shorter stride length under both ST and DT conditions (p < 0.05). DT had significantly negative effect on gait parameters in PD patients, including gait speed, stride length, and gait cycle duration (p < 0.05). PD patients with mild-moderate NMSB showed larger DTEs of cadence and bilateral gait cycle duration (p < 0.05). DTEs of bilateral gait cycle duration and swing phase on the more affected (MA) side were significantly correlated with NMSS scores (∣rSp∣ ≥ 0.3, p < 0.05). Gait cycle duration on the less affected (LA) side explained 43% of the variance in NMSS scores, when accounting for demographic and clinical confounders (β = − 1.095 95% CI − 4.061 ~ − 0.058, p = 0.044; adjusted R2 = 0.434).
Conclusion
DT gait performance could reflect NMSB in PD patients at early stage, and gait cycle duration is a valuable gait parameter to further investigate and to provide more evidence for PD management.

Similar content being viewed by others
References
Kalia LV, Lang AE (2015) Parkinson’s disease. Lancet 386:896–912. https://doi.org/10.1016/s0140-6736(14)61393-3
Nardello F, Bombieri F, Tinazzi M, Schena F, Pellegrini B (2017) Metabolic and kinematic parameters during walking with poles in Parkinson’s disease. J Neurol 264:1785–1790. https://doi.org/10.1007/s00415-017-8568-y
Glover A, Pillai L, Doerhoff S, Virmani T (2020) Differential gait decline in Parkinson’s disease enhances discrimination of gait freezers from non-freezers. J Parkinsons Dis 10:1657–1673. https://doi.org/10.3233/jpd-201961
Pistacchi M, Gioulis M, Sanson F, De Giovannini E, Filippi G, Rossetto F, ZambitoMarsala S (2017) Gait analysis and clinical correlations in early Parkinson’s disease. Funct Neurol 32:28–34. https://doi.org/10.11138/fneur/2017.32.1.028
Zanardi A, da Silva E, Costa R, Passos-Monteiro E, Dos Santos I, Kruel L, Peyré-Tartaruga L (2021) Gait parameters of Parkinson’s disease compared with healthy controls: a systematic review and meta-analysis. Sci Rep 11:752. https://doi.org/10.1038/s41598-020-80768-2
Iansek R, Danoudis M, Bradfield N (2013) Gait and cognition in Parkinson’s disease: implications for rehabilitation. Rev Neurosci 24:293–300. https://doi.org/10.1515/revneuro-2013-0006
Baiano C, Barone P, Trojano L, Santangelo G (2020) Prevalence and clinical aspects of mild cognitive impairment in Parkinson’s disease: a meta-analysis. Mov Disord : Off J Mov Disord Soc 35:45–54. https://doi.org/10.1002/mds.27902
Penko AL, Streicher MC, Koop MM, Dey T, Rosenfeldt AB, Bazyk AS, Alberts JL (2018) Dual-task interference disrupts Parkinson’s gait across multiple cognitive domains. Neuroscience 379:375–382. https://doi.org/10.1016/j.neuroscience.2018.03.021
Raffegeau T, Krehbiel L, Kang N, Thijs F, Altmann L, Cauraugh J, Hass C (2019) A meta-analysis: Parkinson’s disease and dual-task walking. Parkinsonism Relat Disord 62:28–35. https://doi.org/10.1016/j.parkreldis.2018.12.012
Chaudhuri K, Martinez-Martin P, Brown R, Sethi K, Stocchi F, Odin P, Ondo W, Abe K, Macphee G, Macmahon D, Barone P, Rabey M, Forbes A, Breen K, Tluk S, Naidu Y, Olanow W, Williams A, Thomas S, Rye D, Tsuboi Y, Hand A, Schapira A (2007) The metric properties of a novel Non-Motor Symptoms Scale for Parkinson’s disease: results from an international pilot study. Mov Disord : Off J Mov Disord Soc 22:1901–1911. https://doi.org/10.1002/mds.21596
Ray Chaudhuri K, Rojo J, Schapira A, Brooks D, Stocchi F, Odin P, Antonini A, Brown R, Brown R, Martinez-Martin P (2013) A proposal for a comprehensive grading of Parkinson’s disease severity combining motor and non-motor assessments: meeting an unmet need. PLoS ONE 8:e57221. https://doi.org/10.1371/journal.pone.0057221
Gassner H, Marxreiter F, Steib S, Kohl Z, Schlachetzki JCM, Adler W, Eskofier BM, Pfeifer K, Winkler J, Klucken J (2017) Gait and cognition in Parkinson’s disease: cognitive impairment is inadequately reflected by gait performance during dual task. Front Neurol 8:550. https://doi.org/10.3389/fneur.2017.00550
Salazar RD, Ren X, Ellis TD, Toraif N, Barthelemy OJ, Neargarder S, Cronin-Golomb A (2017) Dual tasking in Parkinson’s disease: cognitive consequences while walking. Neuropsychology 31:613–623. https://doi.org/10.1037/neu0000331
Johansson H, Ekman U, Rennie L, Peterson DS, Leavy B, Franzen E (2021) Dual-task effects during a motor-cognitive task in Parkinson’s disease: patterns of prioritization and the influence of cognitive status. Neurorehabil Neural Repair 35:356–366. https://doi.org/10.1177/1545968321999053
Dragasevic-Miskovic NT, Bobic V, Kostic M, Stankovic I, Radovanovic S, Dimitrijevic K, Svetel M, Petrovic I, Duric-Jovicic M (2021) Impact of depression on gait variability in Parkinson’s disease. Clin Neurol Neurosurg 200:106324. https://doi.org/10.1016/j.clineuro.2020.106324
Ehgoetz Martens K, Silveira C, Intzandt B, Almeida Q (2018) Overload from anxiety: a non-motor cause for gait impairments in Parkinson’s disease. J Neuropsychiatry Clin Neurosci 30:77–80. https://doi.org/10.1176/appi.neuropsych.16110298
Postuma R, Berg D, Stern M, Poewe W, Olanow C, Oertel W, Obeso J, Marek K, Litvan I, Lang A, Halliday G, Goetz C, Gasser T, Dubois B, Chan P, Bloem B, Adler C, Deuschl G (2015) MDS clinical diagnostic criteria for Parkinson’s disease. Mov Disord : Off J Mov Disord Soc 30:1591–1601. https://doi.org/10.1002/mds.26424
Tomlinson C, Stowe R, Patel S, Rick C, Gray R, Clarke C (2010) Systematic review of levodopa dose equivalency reporting in Parkinson’s disease. Mov Disord : Off J Mov Disord Soc 25:2649–2653. https://doi.org/10.1002/mds.23429
Vítečková S, Horáková H, Poláková K, Krupička R, Růžička E, Brožová H (2020) Agreement between the GAITRite system and the wearable sensor BTS G-Walk for measurement of gait parameters in healthy adults and Parkinson’s disease patients. PeerJ 8:e8835. https://doi.org/10.7717/peerj.8835
Jagos H, Pils K, Haller M, Wassermann C, Chhatwal C, Rafolt D, Rattay F (2017) Mobile gait analysis via eSHOEs instrumented shoe insoles: a pilot study for validation against the gold standard GAITRite. J Med Eng Technol 41:375–386. https://doi.org/10.1080/03091902.2017.1320434
Kelly V, Janke A, Shumway-Cook A (2010) Effects of instructed focus and task difficulty on concurrent walking and cognitive task performance in healthy young adults. Exp Brain Res 207:65–73. https://doi.org/10.1007/s00221-010-2429-6
Vitorio R, Hasegawa N, Carlson-Kuhta P, Nutt JG, Horak FB, Mancini M, Shah VV (2021) Dual-task costs of quantitative gait parameters while walking and turning in people with Parkinson’s disease: beyond gait speed. J Parkinsons Dis 11:653–664. https://doi.org/10.3233/JPD-202289
Vitorio R, Stuart S, Mancini M (2020) Executive control of walking in people with Parkinson’s disease with freezing of gait. Neurorehabil Neural Repair 34:1138–1149. https://doi.org/10.1177/1545968320969940
Huang C, Chen Y, Hwang I, Wu R (2018) Improving dual-task control with a posture-second strategy in early-stage parkinson disease. Arch Phys Med Rehabil 99:1540-1546.e1542. https://doi.org/10.1016/j.apmr.2018.02.013
Huang X, Ng SY, Chia NS, Setiawan F, Tay KY, Au WL, Tan EK, Tan LC (2019) Non-motor symptoms in early Parkinson’s disease with different motor subtypes and their associations with quality of life. Eur J Neurol 26:400–406. https://doi.org/10.1111/ene.13803
Ren J, Hua P, Pan C, Li Y, Zhang L, Zhang W, Xu P, Zhang M, Liu W (2020) Non-motor symptoms of the postural instability and gait difficulty subtype in de novo Parkinson’s disease patients: a cross-sectional study in a single center. Neuropsychiatr Dis Treat 16:2605–2612. https://doi.org/10.2147/ndt.S280960
Onder H, Ozyurek O (2021) The impact of distinct cognitive dual-tasks on gait in Parkinson’s disease and the associations with the clinical features of Parkinson’s disease. Neurol Sci 42:2775–2783. https://doi.org/10.1007/s10072-020-04874-9
Amundsen-Huffmaster SL, Petrucci MN, Linn-Evans ME, Chung JW, Howell MJ, Videnovic A, Tuite PJ, Cooper SE, MacKinnon CD (2021) REM sleep without atonia and gait impairment in people with mild-to-moderate Parkinson’s disease. J Parkinsons Dis 11:767–778. https://doi.org/10.3233/JPD-202098
Al-Yahya E, Dawes H, Smith L, Dennis A, Howells K, Cockburn J (2011) Cognitive motor interference while walking: a systematic review and meta-analysis. Neurosci Biobehav Rev 35:715–728. https://doi.org/10.1016/j.neubiorev.2010.08.008
Cho C, Kunin M, Kudo K, Osaki Y, Olanow C, Cohen B, Raphan T (2010) Frequency-velocity mismatch: a fundamental abnormality in parkinsonian gait. J Neurophysiol 103:1478–1489. https://doi.org/10.1152/jn.00664.2009
Rietdijk CD, Perez-Pardo P, Garssen J, van Wezel RJ, Kraneveld AD (2017) Exploring Braak’s hypothesis of Parkinson’s disease. Front Neurol 8:37. https://doi.org/10.3389/fneur.2017.00037
Kim S, Kwon S, Kam T, Panicker N, Karuppagounder S, Lee S, Lee J, Kim W, Kook M, Foss C, Shen C, Lee H, Kulkarni S, Pasricha P, Lee G, Pomper M, Dawson V, Dawson T, Ko H (2019) Transneuronal propagation of pathologic α-synuclein from the gut to the brain models Parkinson’s disease. Neuron 103:627-641.e627. https://doi.org/10.1016/j.neuron.2019.05.035
Donoghue O, O’Hare C, King-Kallimanis B, Kenny R (2015) Antidepressants are independently associated with gait deficits in single and dual task conditions. Am J Geriatr Psychiatry : Off J Am Assoc Geriatr Psychiatry 23:189–199. https://doi.org/10.1016/j.jagp.2014.04.005
Acknowledgements
The authors thank all the participants who were enrolled in this study.
Funding
The study was supported by grants from the National Key Technology Research and Development Program of China (2018YFC2002300, 2018YFC2002302, 2020YFC2004102), and the National Nature Science Foundation of China (NSFC:81972144, 31872785, 81972148).
Author information
Authors and Affiliations
Contributions
All the authors listed have made a substantial, direct, and intellectual contribution to the work, and approved it for publication.
Corresponding authors
Ethics declarations
Ethical approval
The studies involving human participants were reviewed and approved by the Ethics Committee of the Beijing Tiantan Hospital. The participants provided their written informed consent to participate in this study.
Conflict of interest
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Zhang, M., Gan, Y., Wang, X. et al. Gait performance and non-motor symptoms burden during dual-task condition in Parkinson’s disease. Neurol Sci 44, 181–190 (2023). https://doi.org/10.1007/s10072-022-06411-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10072-022-06411-2