Abstract
Background
Preoperative prognostication of 30-day mortality in patients with carotid endarterectomy (CEA) can optimize surgical risk stratification and guide the decision-making process to improve survival. This study aims to develop and validate a set of predictive variables of 30-day mortality following CEA.
Methods
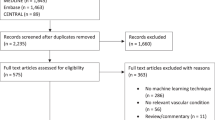
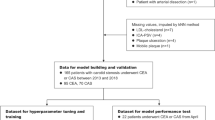
The patient cohort was identified from the American College of Surgeons National Surgical Quality Improvement Program (2005–2016). We performed logistic regression (enter, stepwise, and forward) and least absolute shrinkage and selection operator (LASSO) method for the selection of variables, which resulted in 28-candidate models. The final model was selected based upon clinical knowledge and numerical results.
Results
Statistical analysis included 65,807 patients with 30-day mortality in 0.7% (n = 466) patients. The median age of our cohort was 71.0 years (range, 16–89 years). The model with 9 predictive factors which included age, body mass index, functional health status, American Society of Anesthesiologist grade, chronic obstructive pulmonary disorder, preoperative serum albumin, preoperative hematocrit, preoperative serum creatinine, and preoperative platelet count—performed best on discrimination, calibration, Brier score, and decision analysis to develop a machine learning algorithm. Logistic regression showed higher AUCs than LASSO across these different models. The predictive probability derived from the best model was converted into an open-accessible scoring system.
Conclusion
Machine learning algorithms show promising results for predicting 30-day mortality following CEA. These algorithms can be useful aids for counseling patients, assessing preoperative medical risks, and predicting survival after surgery.




Similar content being viewed by others
Abbreviations
- AE:
-
Adverse events
- AUC:
-
Area under the curve
- BMI:
-
Body mass index
- CEA:
-
Carotid endarterectomy
- CI:
-
Confidence interval
- ICD-CM:
-
International Classification of Disease Clinical Modification
- LASSO:
-
Least absolute shrinkage and selection operator
- NSQIP:
-
National Surgical Quality Improvement Program
- ROC:
-
Receiver operating characteristics
- TRIPOD:
-
Transparent reporting of a multivariable prediction model for individual prognosis or diagnosis
- USA:
-
United States of America
References
Poorthuis MHF, Herings RAR, Dansey K et al (2022) External validation of risk prediction models to improve selection of patients for carotid endarterectomy. Stroke 53(1):87–99. https://doi.org/10.1161/STROKEAHA.120.032527
Rothwell PM, Slattery J, Warlow CP (1997) Clinical and angiographic predictors of stroke and death from carotid endarterectomy: systematic review. BMJ 315(7122):1571–1577. https://doi.org/10.1136/bmj.315.7122.1571
Naylor AR, Ricco JB, de Borst GJ et al (2018) Editor’s choice – management of atherosclerotic carotid and vertebral artery disease: 2017 clinical practice guidelines of the European Society for Vascular Surgery (ESVS). Eur J Vasc Endovasc Surg 55(1):3–81. https://doi.org/10.1016/j.ejvs.2017.06.021
McCrory DC, Goldstein LB, Samsa GP et al (1993) Predicting complications of carotid endarterectomy. Stroke 24(9):1285–1291. https://doi.org/10.1161/01.STR.24.9.1285
Hobson RW, Weiss DG, Fields WS et al (1993) Efficacy of carotid endarterectomy for asymptomatic carotid stenosis. N Engl J Med 328(4):221–227. https://doi.org/10.1056/NEJM199301283280401
Mayberg MR, Wilson SE, Yatsu F et al (1991) Carotid endarterectomy and prevention of cerebral ischemia in symptomatic carotid stenosis. Veterans Affairs Cooperative Studies Program 309 Trialist Group. JAMA 266(23):3289–3294
MRC European Carotid Surgery Trial (1991) interim results for symptomatic patients with severe (70–99%) or with mild (0–29%) carotid stenosis. European Carotid Surgery Trialists’ Collaborative Group. Lancet (London, England) 337(8752):1235–1243
Muuronen A (1984) Outcome of surgical treatment of 110 patients with transient ischemic attack. Stroke 15(6):959–964. https://doi.org/10.1161/01.STR.15.6.959
Nunn DB (1975) Carotid endarterectomy: an analysis of 234 operative cases. Ann Surg 182(6):733–738. https://doi.org/10.1097/00000658-197512000-00014
Ojemann RG, Crowell RM, Roberson GH, Fisher CM (1975) Surgical treatment of extracranial carotid occlusive disease. Clin Neurosurg 22:214–263. https://doi.org/10.1093/neurosurgery/22.cn_suppl_1.214
Whisnant JP, Sandok BA, Sundt TM (1983) Carotid endarterectomy for unilateral carotid system transient cerebral ischemia. Mayo Clin Proc 58(3):171–175
Reddy RP, Karnati T, Massa RE, Thirumala PD (2019) Association between perioperative stroke and 30-day mortality in carotid endarterectomy: a meta-analysis. Clin Neurol Neurosurg 181:44–51. https://doi.org/10.1016/j.clineuro.2019.03.028
Bissacco D, Malloggi C, Domanin M et al (2022) Role of risk scoring systems in predicting life expectancy after carotid endarterectomy in asymptomatic patients. J Vasc Surg 75(3):906-914.e4. https://doi.org/10.1016/j.jvs.2021.08.099
Zhou F, Hua Y, Ji X, Jia L (2021) A systemic review into carotid plaque features as predictors of restenosis after carotid endarterectomy. J Vasc Surg 73(6):2179-2188.e4. https://doi.org/10.1016/j.jvs.2020.10.084
Patel K, Zil-E-Ali A, Aziz F (2022) Asymptomatic preoperative leukocytosis before carotid endarterectomy is associated with increased risk of stroke: a study from NSQIP database. Ann Vasc Surg 79:46–55. https://doi.org/10.1016/j.avsg.2021.07.011
Pereira-Neves A, Saramago S, Duarte-Gamas L et al (2022) Mean platelet volume predicts restenosis after carotid endarterectomy. Ann Vasc Surg 81:216–224. https://doi.org/10.1016/j.avsg.2021.08.054
Casanova N, Diaz-Duran C, Nieto L, Llort C, Elosua R, Clara A (2022) Predictive value of complete blood count-derived inflammatory markers for 5-year survival after carotid endarterectomy: implications for practice. Angiology 2022:33197211067581. https://doi.org/10.1177/00033197211067581
Karhade AV, Larsen AMG, Cote DJ, Dubois HM, Smith TR (2018) National databases for neurosurgical outcomes research: options, strengths, and limitations. Clin Neurosurg. https://doi.org/10.1093/neuros/nyx408
DePasse JM, Durand W, Daniels AH (2018) Predictors of nonneurologic complications and increased length of stay after cervical spine osteotomy. World Neurosurgery 118:e727–e730. https://doi.org/10.1016/j.wneu.2018.07.029
Collins GS, Reitsma JB, Altman DG, Moons KGM (2015) Transparent reporting of a multivariable prediction model for individual prognosis or diagnosis (TRIPOD): the TRIPOD statement. European Urology. https://doi.org/10.1016/j.eururo.2014.11.025
Luo W, Phung D, Tran T et al (2016) Guidelines for developing and reporting machine learning predictive models in biomedical research: a multidisciplinary view. J Med Internet Res https://doi.org/10.2196/jmir.5870
Neeman T (2009) Clinical prediction models: a practical approach to development, validation, and updating by Ewout W Steyerberg. Int Statistic Rev. https://doi.org/10.1111/j.1751-5823.2009.00085_22.x
Finkelstein JA, Zaveri G, Wai E, Vidmar M, Kreder H, Chow E (2003) A population-based study of surgery for spinal metastases. Survival rates and complications. J Bone Joint Surg Br. https://doi.org/10.1302/0301-620X.85B7.14201
Karhade AV, Thio QCBS, Ogink PT et al (2019) Development of machine learning algorithms for prediction of 30-day mortality after surgery for spinal metastasis. Neurosurgery. https://doi.org/10.1093/neuros/nyy469
Bertrand P V., Sakamoto Y, Ishiguro M, Kitagawa G (1988) Akaike information criterion statistics. J R Stat Soc Ser A (Stat Soc). https://doi.org/10.2307/2983028
Chiang AY (2007) Generalized additive models: an introduction with R. Technometrics. https://doi.org/10.1198/tech.2007.s505
Gauraha N (2018) Introduction to the LASSO. Resonance. https://doi.org/10.1007/s12045-018-0635-x
Han SS, Azad TD, Suarez PA, Ratliff JK (2019) A machine learning approach for predictive models of adverse events following spine surgery. Spine J. https://doi.org/10.1016/j.spinee.2019.06.018
Barnett HJM, Taylor DW, Eliasziw M et al (1998) Benefit of carotid endarterectomy in patients with symptomatic moderate or severe stenosis. N Engl J Med 339(20):1415–1425. https://doi.org/10.1056/NEJM199811123392002
(2004) Prevention of disabling and fatal strokes by successful carotid endarterectomy in patients without recent neurological symptoms: randomised controlled trial. Lancet 363(9420):1491–1502. https://doi.org/10.1016/S0140-6736(04)16146-1
Ball S, Ball A, Antoniou GA (2020) Editor’s choice – prognostic role of pre-operative symptom status in carotid endarterectomy: a systematic review and meta-analysis. Eur J Vasc Endovasc Surg 59(4):516–524. https://doi.org/10.1016/j.ejvs.2020.01.022
Tu JV, Wang H, Bowyer B, Green L, Fang J, Kucey D (2003) Risk factors for death or stroke after carotid endarterectomy: observations from the Ontario Carotid Endarterectomy Registry. Stroke 34(11):2568–2573. https://doi.org/10.1161/01.STR.0000092491.45227.0F
Kondo T, Ota N, Göhre F et al (2020) High Cervical carotid endarterectomy–outcome analysis. World Neurosurg 136:e108–e118. https://doi.org/10.1016/j.wneu.2019.12.002
Mas JL, Trinquart L, Leys D et al (2008) Endarterectomy versus angioplasty in patients with symptomatic severe carotid stenosis (EVA-3S) trial: results up to 4 years from a randomised, multicentre trial. Lancet Neurol 7(10):885–892. https://doi.org/10.1016/S1474-4422(08)70195-9
(2006) 30 day results from the SPACE trial of stent-protected angioplasty versus carotid endarterectomy in symptomatic patients: a randomised non-inferiority trial. Lancet 368(9543):1239–1247. https://doi.org/10.1016/S0140-6736(06)69122-8
Yadav JS, Wholey MH, Kuntz RE et al (2004) Protected carotid-artery stenting versus endarterectomy in high-risk patients. N Engl J Med 351(15):1493–1501. https://doi.org/10.1056/NEJMoa040127
Thompson JE, Talkington CM (1976) Carotid endarterectomy. Ann Surg 184(1):1–15. https://doi.org/10.1097/00000658-197607000-00001
Modrall JG, Tsai S, Ramanan B et al (2020) Defining the threshold surgeon volume associated with improved patient outcomes for carotid endarterectomy. J Vasc Surg 72(1):209-218.e1. https://doi.org/10.1016/j.jvs.2019.10.057
Easton JD, Sherman DG (1977) Stroke and mortality rate in carotid endarterectomy: 228 consecutive operations. Stroke 8(5):565–568. https://doi.org/10.1161/01.STR.8.5.565
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval
The de-identified NSQIP data is exempt from review by our Institutional Review Board.
Conflict of interest
None of the authors has any conflict of interest.
Informed Consent
Not applicable as it is a retrospective study from a de-identified data.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Mohamed, A., Shuaib, A., Ahmed, A.Z. et al. Predictors of 30-day mortality using machine learning approach following carotid endarterectomy. Neurol Sci 44, 253–261 (2023). https://doi.org/10.1007/s10072-022-06392-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10072-022-06392-2