Abstract
Background and purpose
The aim of this study is to observe the differences between fallers, common fallers, and non-fallers in stroke patients compared with the global ability in a rehabilitation setting.
Materials and methods
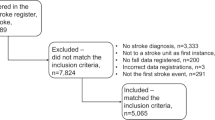
An observational and prospective study has been carried out. A total of 476 subacute stroke patients have been observed. The main outcome measures were assessed using the Canadian Neurological Scale (CNS), Barthel Index (BI), Functional Ambulatory Category (FAC), and Trunk Control Test (TCT) at admission to the rehabilitation unit and after 90 days of the rehabilitation treatment (nearly 3 h for day for 5 days for week) at the discharge with intermediate evaluations after the first and second months.
Results
Out of 397 patients, 109 reported 1 or more falls (27.5%), of whom 67 fell 1 time (fallers) in the hospital (16.9%) and 42 fell 2 or more times (common fallers) (10.6%). For fallers, BI and FAC scores had a significant effect (p = 0.003 for both). Common fallers had statistically significant differences in BI (p = 0.002), FAC (p = 0.012), and TCT scores (0.023) compared with non-fallers.
Conclusions
The severity of stroke may directly increase the risk of fall, and also indirectly, lengthening the hospitalization. Our study seems to suggest that patients with BI scores of between 21 and 30 on admission are more prone to fall in the first period of hospitalization, whereas in the second month, those with scores of between 11 and 20 on admission have a higher risk of falls. In the third month, patients with BI scores below 10 on admission are more susceptible to falls.


Similar content being viewed by others
References
Teasell R, McRae M, Foley N, Bhardwaj A (2002) The incidence and consequences of falls in stroke patients during inpatient rehabilitation: factors associated with high risk. Arch Phys Med Rehabil 83(3):329–333
Divani AA, Vazquez G, Barrett AM, Asadollahi M, Luft AR (2009) Risk factors associated with injury attributable to falling among elderly population with history of stroke. Stroke. 40(10):3286–3292
Verheyden GS, Weerdesteyn V, Pickering RM et al (2013) Interventions for preventing falls in people after stroke. Cochrane Database Syst Rev 5:CD008728
Ash KL, MacLeod P, Clark L (1998) A case control study of falls in the hospital setting. J Gerontol Nurs 24(12):7–15
Saverino E, Benevolo M, Ottonello E, Zsirai P (2006) Sessarego. Falls in rehabilitation setting; functional independence and fall risk. EURA MEDICOPYHS 42(3):179–184
Campbell GB, Matthews JT (2010) An integrative review of factors associated with falls during post-stroke rehabilitation. J Nurs Scholarsh 42(4):395–404
Langhorne P, Stott DJ, Robertson L, MacDonald J, Jones L, McAlpine C (2000) Medical complications after stroke. Stroke. 31(6):1223–1229
Oliver D, Daly F, Martin FC, McMurdo ME (2004) Risk factors and risk assessment tools for falls in hospital in-patients: a systematic review. Age Ageing 33(2):122–130
Damián J, Pastor-Barriuso R, Valderrama-Gama E, de Pedro-Cuesta J (2013) Factors associated with falls among older adults living in institutions. BMC Geriatr 13:6
Tsur A, Segal Z (2010) Falls in stroke patients: risk factors and risk management. Isr Med Assoc J 12(4):216–219
Morone G, Iosa M, Pratesi L, Paolucci S (2014) Can overestimation of walking ability increase the risk of falls in people in the subacute stage after stroke on their return home? Gait Posture 39(3):965–970
Mackintosh SF, Hill KD, Dodd KJ, Goldie PA, Culham EG (2006) Balance score and a history of falls in hospital predict recurrent falls in the 6 months following stroke rehabilitation. Arch Phys Med Rehabil 87(12):1583–1589
Forster A, Young J (1995) Incidence and consequences of falls due to stroke: a systematic inquiry. BMJ 311(6997):83–86
Nevitt MC, Cummings SR (1991) Risk factors for injurious falls: a prospective study. J Gerontol 46(5):M164–M170
Kellogg International Work Group on the Prevention of Falls by the Elderly (1987) The prevention of falls in later life. Dan Med Bull 34(Suppl. 4):1–24
Zecevic AA, Salmoni AW, Speechley M, Vandervoort AA (2006 Jun) Defining a fall and reasons for falling: comparisons among the views of seniors, health care providers, and the research literature. Gerontologist. 46(3):367–376
Paolucci S, Bragoni M, Coiro P, de Angelis D, Fusco FR, Morelli D, Venturiero V, Pratesi L (2008) Quantification of the probability of reaching mobility independence at discharge from a rehabilitation hospital in nonwalking early ischemic stroke patients: a multivariate study. Cerebrovasc Dis 26(1):16–22
Shah S, Vanclay F, Cooper B (1990) Efficiency, effectiveness, and duration of stroke rehabilitation. Stroke. 21(2):241–246
Blennerhassett JM, Dite W, Ramage ER, Richmond ME (2012) Changes in balance and walking from stroke rehabilitation to the community: a follow-up observational study. Arch Phys Med Rehabil 93(10):1782–1787
Oliver D, Hopper A, Seed P (2000) Do hospital fall prevention programs work? A systematic review. J Am Geriatr Soc 48(12):1679–1689
van der Kooi E, Schiemanck SK, Nollet F, Kwakkel G, Meijer JW, van de Port I (2017) Falls are associated with lower self-reported functional status in patients after stroke. Arch Phys Med Rehabil 98(12):2393–2398. https://doi.org/10.1016/j.apmr.2017.05.003
Wong JS, Brooks D, Mansfield A (2016) Do falls experienced during inpatient stroke rehabilitation affect length of stay, functional status, and discharge destination? Arch Phys Med Rehabil 97(4):561–566
Jalayondeja C, Sullivan PE, Pichaiyongwongdee S (2014) Six-month prospective study of fall risk factors identification in patients post-stroke. Geriatr Gerontol Int 14(4):778–785. https://doi.org/10.1111/ggi.12164
Duffy L, Gajree S, Langhorne P, Stott DJ, Quinn TJ (2013) Reliability (inter-rater agreement) of the Barthel Index for assessment of stroke survivors: systematic review and meta-analysis. Stroke. 44(2):462–468
Funding
This work is supported by the Italian Ministry of Health with the Grant Number RC2013G and by IRCCS Santa Lucia foundation.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare they have no conflict of interest.
Ethical approval
The protocol was approved by the local independent ethics committee, and all participants provided written informed consent.
Disclaimer
The funder had no role in the design and conduct of the study; collection, management, analysis, and interpretation of the data; preparation, review, or approval of the manuscript; and decision to submit the manuscript for publication.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Morone, G., Martino Cinnera, A., Paolucci, T. et al. Clinical features of fallers among inpatient subacute stroke: an observational cohort study. Neurol Sci 41, 2599–2604 (2020). https://doi.org/10.1007/s10072-020-04352-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10072-020-04352-2