Abstract
Background
Structural remodeling is a classic manifestation of disease decompensation. Facial synkinesis is the most troubling sequela of peripheral facial neuritis, and its structural remodeling, especially in white matter (WM), is still poorly understood. Therefore, understanding WM microstructure is important for predicting WM pathology and for early intervention in facial synkinesis patients.
Methods
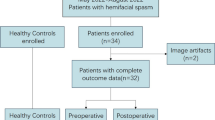
A total of 20 facial synkinesis patients (18 men and 2 women; mean age, 33.35 ± 6.97 years old) and 19 healthy controls (17 men and 2 women; mean age, 33.21 ± 6.75 years old) were enrolled in this study. rs-fMRI data, diffusion tensor imaging (DTI) data, and Beck’s Depression Inventory (BDI) data were collected, and tract-based spatial statistics (TBSS) and voxel-mirrored homotopic connectivity (VMHC) values were used to analyze changes in WM microstructure and interhemispheric coordination.
Results
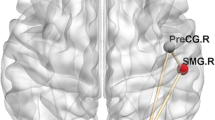
Compared with the healthy controls, facial synkinesis patients exhibited significantly lower regional fractional anisotropy (FA) in the genu of the corpus callosum and the body of the corpus callosum, significantly higher regional FA in the retrolenticular part of the internal capsule, and significantly decreased VMHC values bilaterally in the orbital inferior frontal gyri, the fusiform gyri, the superior temporal gyri, the superior frontal gyri, and the supplementary motor areas. Furthermore, a lower regional FA in the genu of the corpus callosum was correlated with higher BDI scores in facial synkinesis patients.
Conclusion
Structural remodeling, especially changes in white matter microstructure, may be the central mechanism for severe sequelae of peripheral facial neuritis.



Similar content being viewed by others
Data availability
The data that support the findings of this study are available from the corresponding author, Jian-guang Xu, upon reasonable request.
References
Honda N, Hato N, Takahashi H et al (2002) Pathophysiology of facial nerve paralysis induced by herpes simplex virus type 1 infection. Ann Otol Rhinol Laryngol 111(7 Pt 1):616–622
Baker RS, Stava MW, Nelson KR et al (1994) Aberrant reinnervation of facial musculature in a subhuman primate: a correlative analysis of eyelid kinematics, muscle synkinesis, and motoneuron localization. Neurology. 44(11):2165–2173
Nakamura K, Toda N, Sakamaki K, Kashima K, Takeda N (2003) Biofeedback rehabilitation for prevention of synkinesis after facial palsy. Otolaryngol Head Neck Surg 128:539–543
Oge AE, Yayla V, Demir GA, Eraksoy M (2005) Excitability of facial nucleus and related brain-stem reflexes in hemifacial spasm, post-facial palsy synkinesis and facial myokymia. Clin Neurophysiol 116(7):1542–1554
Azizzadeh B, Irvine LE, Diels J et al (2019) Modified selective neurectomy for the treatment of post-facial paralysis synkinesis. Plast Reconstr Surg 143(5):1483–1496
Múnera A, Cuestas DM, Troncoso J (2012) Peripheral facial nerve lesions induce changes in the firing properties of primary motor cortex layer 5 pyramidal cells. Neuroscience. 223:140–151
Wang Y, Yang L, Wang WW et al (2019) Decreased distance between representation sites of distinct facial movements in facial synkinesis-a task fmri study. Neuroscience. 15(397):12–17
Jonsson L, Hemmingsson A, Thomander L, Bergström K, Stålberg E, Thuomas KA (1989) Magnetic resonance imaging in patients with Bell’s palsy. Acta Otolaryngol Suppl 468:403–405
Lundborg G (2000) Brain plasticity and hand surgery: an overview. J Hand Surg (Br) 25(3):242–252
Wu JJ, Lu YC, Zheng MX et al (2019) Motor control deficits in facial synkinesis patients: neuroimaging evidences of cerebral cortex involvement. Neural Plast 7235808. https://doi.org/10.1155/2019/7235808
Shinn JR, Nwabueze NN, Du L et al (2019) Treatment patterns and outcomes in botulinum therapy for patients with facial synkinesis. JAMA Facial Plast Surg 21(3):244–251
Maniega SM, Valdés Hernández MC, Clayden JD et al (2015) White matter hyperintensities and normal-appearing white matter integrity in the aging brain. Neurobiol Aging 36(2):909–918
Jacome DE (2003) Catamenial synkinetic retroauricular pain. Cephalalgia. 23(3):214–217
de Groot M, Verhaaren BF, de Boer R et al (2013) Changes in normal-appearing white matter precede development of white matter lesions. Stroke. 44(4):1037–1042
Smith SM, Jenkinson M, Johansen-Berg H et al (2006) Tract-based spatial statistics: voxelwise analysis of multi-subject diffusion data. Neuroimage. 31:1487–1505
Hua K, Zhang J, Wakana S, Jiang H, Li X, Reich DS, Calabresi PA, Pekar JJ, van Zijl P, Mori S (2008) Tract probability maps in stereotaxic spaces: analyses of white matter anatomy and tract-specific quantification. Neuroimage. 39(1):336–347
BECK AT (1961) An Inventory for Measuring Depression. Arch Gen Psychiatry 4(6):561
Chao-Gan Y, Yu-Feng Z (2010) DPARSF: A MATLAB toolbox for “Pipeline” data analysis of resting-state fMRI. Front Syst Neurosci 4:13
Zhang Y, Zhu Y, Pei Y et al (2019) Disrupted interhemispheric functional coordination in patients with chronic low back-related leg pain: a multiscale frequency-related homotopic connectivity study. J Pain Res. 12:2615–2626
Zuo XN, Kelly C, Di Martino A et al (2010) Growing together and growing apart: regional and sex differences in the lifespan developmental trajectories of functional homotopy. J Neurosci 30(45):15034–15043
Smith SM, Nichols TE (2009) Threshold-free cluster enhancement: addressing problems of smoothing, threshold dependence and localisation in cluster inference. Neuroimage. 44(1):83–98
Song XW, Dong ZY, Long XY et al (2011) REST: a toolkit for resting-state functional magnetic resonance imaging data processing. PLoS One 6(9):e25031
Oya R, Takenaka Y, Imai T, Sato T, Oshima K, Ohta Y, Inohara H (2019) Neutrophil-to-lymphocyte ratio and platelet-to-lymphocyte ratio as prognostic hematologic markers of Bell’s palsy: a meta-analysis. Otol Neurotol 40(5):681–687
Volpe JJ (2009) Brain injury in premature infants: a complex amalgam of destructive and developmental disturbances. Lancet Neurol 8(1):110–124
Kovács T, Szirmai I, Papp M (2005) Clinico-pathology and differential diagnosis of Binswanger’s disease. Ideggyogy Sz 58(3–4):78–87
Wersching H, Duning T, Lohmann H, Mohammadi S, Stehling C, Fobker M, Conty M, Minnerup J, Ringelstein EB, Berger K, Deppe M, Knecht S (2010) Serum C-reactive protein is linked to cerebral microstructural integrity and cognitive function. Neurology 74:1022–1029
Altendahl M, Maillard P, Harvey D et al (2020) An IL-18-centered inflammatory network as a biomarker for cerebral white matter injury. PLoS One 15(1):e0227835
Wixey JA, Sukumar KR, Pretorius R et al (2019) Ibuprofen treatment reduces the neuroinflammatory response and associated neuronal and white matter impairment in the growth restricted newborn. Front Physiol 10:541
Hartmann G, Tschop M, Fischer R et al (2000) High altitude increases circulating interleukin-6, interleukin-1 receptor antagonist and C-reactive protein. Cytokine. 12(3):246–252
Haddad JJ, Harb HL (2005) Cytokines and the regulation of hypoxia-inducible factor (HIF)-1alpha. Int Immunopharmacol 5(3):461–483
Yuen TJ, Silbereis JC, Griveau A et al (2014) Oligodendrocyte-encoded HIF function couples postnatal myelination and white matter angiogenesis. Cell 158(2):383–396
Le Moan N, Baeten KM, Rafalski VA et al (2015) Hypoxia inducible factor-1α in astrocytes and/or myeloid cells is not required for the development of autoimmune demyelinating disease. eNeuro. 2(2):1–12
Nellis JC, Ishii M, Byrne PJ et al (2017) Association among facial paralysis, depression, and quality of life in facial plastic surgery patients. JAMA Facial Plast Surg 19(3):190–196
Konnerth V, Mohr G, von Piekartz H (2016) Emotion recognition in patients with peripheral facial paralysis-a pilot study. Rehabilitation (Stuttg) 55(1):19–25
Heij GJ, Penninx BWHJ, van Velzen LS et al (2019) White matter architecture in major depression with anxious distress symptoms. Prog Neuro-Psychopharmacol Biol Psychiatry 4:109664
Yassin W, Callahan BL, Ubukata S, Sugihara G, Murai T, Ueda K (2017) Facial emotion recognition in patients with focal and diffuse axonal injury. Brain Inj 31(5):624–630
Kim MJ, Whalen PJ (2009) The structural integrity of an amygdala-prefrontal pathway predicts trait anxiety. J Neurosci 29(37):11614–11618
Baur V, Hanggi J, Rufer M, Delsignore A, Jancke L, Herwig U, Beatrix BA (2011) White matter alterations in social anxiety disorder. J Psychiatr Res 45(10):1366–1372
Pelizzari L, Di Tella S, Laganà MM et al (2020) White matter alterations in early Parkinson’s disease: role of motor symptom lateralization. Neurol Sci 41(2):357–364
Shen XY, Fan ZX, Wang L, Cui S, Niu JL (2019) Altered white matter microstructure in patients with post-stroke depression detected by diffusion kurtosis imaging. Neurol Sci 40(10):2097–2103
Dubner SE, Dodson CK, Marchman VA et al (2019) White matter microstructure and cognitive outcomes in relation to neonatal inflammation in 6-year-old children born preterm. Neuroimage Clin 23:101832
Doron KW, Gazzaniga MS (2008) Neuroimaging techniques offer new perspectives on callosal transfer and interhemispheric communication. Cortex 44(8):1023–1029
Berlucchi G (2012) Frontal callosal disconnection syndromes. Cortex 48(1):36–45
Schulte T, Müller-Oehring EM, Rohlfing T, Pfefferbaum A, Sullivan EV (2010) White matter fiber degradation attenuates hemispheric asymmetry when integrating visuomotor information. J Neurosci 30(36):12168–12178
Di Paola M, Di Iulio F, Cherubini A, Blundo C, Casini AR, Sancesario G et al (2010) When, where, and how the corpus callosum changes in MCI and AD: a multimodal MRI study. Neurology 74:1136–1142
Arnone D, McIntosh AM, Chandra P, Ebmeier KP (2008) Meta-analysis of magnetic resonance imaging studies of the corpus callosum in bipolar disorder. Acta Psychiatr Scand 118:357–362
Cyprien F, Courtet P, Poulain V, Maller J, Meslin C, Bonafe A et al (2014) Corpus callosum size may predict late-life depression in women: a 10-year follow-up study. J Affect Disord 165:16–23
Cyprien F, Courtet P, Malafosse A, Maller J, Meslin C, Bonafe A et al (2011) Suicidal behavior is associated with reduced corpus callosum area. Biol Psychiatry 70:320–326
Lábadi B, Beke AM (2017) Mental state understanding in children with agenesis of the corpus callosum. Front Psychol 8:94
Lebel C, Gee M, Camicioli R, Wieler M, Martin W, Beaulieu C (2012) Diffusion tensor imaging of white matter tract evolution over the lifespan. Neuroimage 60:340–352
Witelson SF (1989) Hand and sex differences in the isthmus and genu of the human corpus callosum. A postmortem morphological study. Brain 112(3):799–835
Byrne ML, Whittle S, Allen NB (2016) The role of brain structure and function in the association between inflammation and depressive symptoms: a systematic review. Psychosom Med 78(4):389–400
Funding
This work was supported by the National Key R&D Program of China (Grant No. 2018YFC2001600), the Shanghai Science and Technology Committee (Grants 18511108300, 18441903903900, and 18441903800), and the Shanghai Jiaotong University Multidisciplinary Research Fund of Medicine and Engineering (YG 2016QN13).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
The study was approved by the local ethics committee at the Ninth People's Hospital (approval no. 2017-365-T267), and all patients provided written informed consent according to the Helsinki Declaration.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Ma, J., Hua, XY., Zheng, MX. et al. Structural remodeling secondary to functional remodeling in advanced-stage peripheral facial neuritis. Neurol Sci 41, 2453–2460 (2020). https://doi.org/10.1007/s10072-020-04325-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10072-020-04325-5