Abstract
Background and purpose
Conflicts exist regarding relationship between prior/new statin use, cholesterol, and early poststroke intracranial hemorrhage (ICH) in acute ischemic stroke (AIS) patients. This meta-analysis is aimed at evaluating the safety of prior/new statin use, cholesterol level and risk of ICH in AIS patients.
Methods
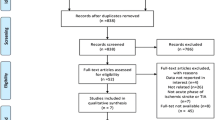
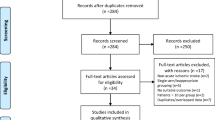
We searched PubMed and Embase for studies examining relation between statin use, cholesterol level, and early poststroke ICH in AIS. Included studies should report risk of early poststroke symptomatic ICH (sICH) or overall ICH. A random-effects model was used to pool the data.
Results
Twenty-five articles involving 26,327 participants were included, among whom 925 had sICH. Prior statin use was not associated with overall ICH (adjusted odds ratio (OR), 1.478; 95% confidence interval (CI), 0.924–2.362; p = 0.103) and sICH in patients who received thrombolysis (adjusted OR, 1.567; 95% CI, 0.994–2.471; p = 0.053) or overall ICH in patients, most of whom had not received recanalization therapy (crude OR, 1.342; 95% CI, 0.872–2.065; p = 0.181). New statin use was associated with decreased sICH after recanalization therapy (crude OR, 0.292; 95% CI, 0.168–0.507; p < 0.001).Cholesterol level was not associated with overall ICH.
Conclusion
Prior/new statin use and lower cholesterol level are not risk factors for sICH and overall ICH in AIS patients, whether or not the patient has received recanalization therapy. New statin use is likely associated with decreased sICH.



Similar content being viewed by others
References
Whiteley WN, Emberson J, Lees KR et al (2016) Risk of intracerebral haemorrhage with alteplase after acute ischaemic stroke: a secondary analysis of an individual patient data meta-analysis. Lancet Neurol 15(9):925–933. https://doi.org/10.1016/S1474-4422(16)30076-X
Ní Chróinín D, Asplund K, Åsberg S et al (2013) Statin therapy and outcome after ischemic stroke: systematic review and meta-analysis of observational studies and randomized trials. Stroke 44:448–456. https://doi.org/10.1161/STROKEAHA.112.668277
Martinez-Ramirez S, Delgado-Mederos R, Marín R et al (2012) Statin pretreatment may increase the risk of symptomatic intracranial haemorrhage in thrombolysis for ischemic stroke: results from a case-control study and a meta-analysis. J Neurol 259(1):111–118. https://doi.org/10.1007/s00415-011-6137-3
Scheitz JF, Seiffge DJ, Tütüncü S et al (2014) Dose-related effects of statins on symptomatic intracerebral hemorrhage and outcome after thrombolysis for ischemic stroke. Stroke 45(2):509–514. https://doi.org/10.1161/STROKEAHA.113.002751
Engelter ST, Soinne L, Ringleb P et al (2011) IV thrombolysis and statins. Neurology 77(9):888–895. https://doi.org/10.1212/WNL.0b013e318281cc83
Meseguer E, Mazighi M, Lapergue B et al (2012) Outcomes after thrombolysis in AIS according to prior statin use: a registry and review. Neurology 79(17):1817–1823. https://doi.org/10.1212/WNL.0b013e318270400b
Thrift A, McNeil J, Donnan G (2002) Reduced frequency of high cholesterol levels among patients with intracerebral haemorrhage. J Clin Neurosci 9:376–380
Bang OY, Saver JL, Liebeskind DS et al (2007) Cholesterol level and symptomatic hemorrhagic transformation after ischemic stroke thrombolysis. Neurology 68(10):737–742. https://doi.org/10.1212/01.wnl.0000252799.64165.d5
D'Amelio M, Terruso V, Famoso G et al (2011) Cholesterol levels and risk of hemorrhagic transformation after acute ischemic stroke. Cerebrovasc Dis 32(3):234–238. https://doi.org/10.1159/000329315
Kim BJ, Lee SH, Ryu WS et al (2009) Low level of low-density lipoprotein cholesterol increases hemorrhagic transformation in large artery atherothrombosis but not in cardioembolism. Stroke 40(5):1627–1632. https://doi.org/10.1161/STROKEAHA.108.539643
Nardi K, Leys D, Eusebi P et al (2011) Influence of lipid profiles on the risk of hemorrhagic transformation after ischemic stroke: systematic review. Cerebrovasc Dis Extra 1(1):130–141. https://doi.org/10.1159/000335014
Uyttenboogaart M, Koch MW, Koopman K et al (2008) Lipid profile, statin use, and outcome after intravenous thrombolysis for acute ischaemic stroke. J Neurol 255(6):875–880. https://doi.org/10.1007/s00415-008-0797-7
Makihara N, Okada Y, Koga M et al (2012) Effect of serum lipid levels on stroke outcome after rt-PA therapy: SAMURAI rt-PA registry. Cerebrovasc Dis 33(3):240–247. https://doi.org/10.1159/000334664
Nardi K, Engelter S, Strbian D et al (2012) Lipid Profile in Thrombolysis Study Group. Lipid profiles and outcome in patients treated by intravenous thrombolysis for cerebral ischemia. Neurology 79(11):1101–1108. https://doi.org/10.1212/wnl.0b013e3182608c82
Rocco A, Sykora M, Ringleb P, Diedler J (2012) Impact of statin use and lipid profile on symptomatic intracerebral haemorrhage, outcome and mortality after intravenous thrombolysis in acute stroke. Cerebrovasc Dis 33(4):362–368. https://doi.org/10.1159/000335840
Stroup DF, Berlin JA, Morton SC et al (2000) Meta-analysis of observational studies in epidemiology: a proposal for reporting. Meta-analysis Of Observational Studies in Epidemiology (MOOSE) group. JAMA 283(15):2008–2012
The Newcastle-Ottawa Scale (NOS) for assessing the quality of non-randomised studies in meta-analyses. http://www.ohri.ca/programs/clinical_epidemiology/oxford.asp. Accessed December 15, 2012.
Hacke W, Kaste M, Fieschi C et al (1998) Randomised double-blind placebo-controlled trial of thrombolytic therapy with intravenous alteplase in acute ischaemic stroke (ECASS II). Second European-Australasian Acute Stroke Study Investigators. Lancet 352(9136):1245–1251
Higgins JP, Thompson SG, Deeks JJ, Altman DG (2003) Measuring inconsistency in meta-analyses. BMJ 327(7414):557–560. https://doi.org/10.1136/bmj.327.7414.557
Egger M, Davey Smith G, Schneider M, Minder C (1997) Bias in meta-analysis detected by a simple, graphical test. BMJ 315:629–634
Scheitz JF, Endres M, Heuschmann PU et al (2015) Reduced risk of poststroke pneumonia in thrombolyzed stroke patients with continued statin treatment. Int J Stroke 10(1):61–66. https://doi.org/10.1111/j.1747-4949.2012.00864.x
Zhao HD, Zhang YD (2014) The effects of previous statin treatment on plasma matrix metalloproteinase-9 level in Chinese stroke patients undergoing thrombolysis. J Stroke Cerebrovasc Dis 23(10):2788–2793. https://doi.org/10.1016/j.jstrokecerebrovasdis.2014.07.001
Meier N, Nedeltchev K, Brekenfeld C et al (2009) Prior statin use, intracranial hemorrhage, and outcome after intra-arterial thrombolysis for acute ischemic stroke. Stroke 40(5):1729–1737. https://doi.org/10.1161/STROKEAHA.108.532473
Yi X, Han Z, Wang C, Zhou Q, Lin J (2017) Statin and Aspirin Pretreatment Are Associated with Lower Neurological Deterioration and Platelet Activity in Patients with Acute Ischemic Stroke. J Stroke Cerebrovasc Dis 26(2):352–359. https://doi.org/10.1016/j.jstrokecerebrovasdis.2016.09.030
Restrepo L, Bang OY, Ovbiagele B et al (2009) Impact of hyperlipidemia and statins on ischemic stroke outcomes after intra-arterial fibrinolysis and percutaneous mechanical embolectomy. Cerebrovasc Dis 28(4):384–390. https://doi.org/10.1159/000235625
Miedema I, Uyttenboogaart M, Koopman K et al (2010) Statin use and functional outcome after tissue plasminogen activator treatment in acute ischaemic stroke. Cerebrovasc Dis 29(3):263–267. https://doi.org/10.1159/000275500
Georgiadis AL, Hussein HM, Vazquez G et al (2009) Premorbid use of statins is associated with higher recanalization rates in patients with acute ischemic stroke undergoing endovascular treatment. J Neuroimaging 19(1):19–22. https://doi.org/10.1111/j.1552-6569.2008.00319.x
Cappellari M, Bovi P, Moretto G et al (2013) The THRombolysis and Statins (THRaST) study. Neurology 80(7):655–661. https://doi.org/10.1212/WNL.0b013e318281cc83
Kang J, Kim N, Park TH et al (2015) Early statin use in ischemic stroke patients treated with recanalization therapy: retrospective observational study. BMC Neurol 15(122). https://doi.org/10.1186/s12883-015-0367-4
Tong LS, Hu HT, Zhang S et al (2015) Statin withdrawal beyond acute phase affected outcome of thrombolytic stroke patients: an observational retrospective study. Medicine (Baltimore) 94(17):1–7. https://doi.org/10.1097/MD.0000000000000779
Tsivgoulis G, Kadlecová P, Kobayashi A et al (2015) Safety of Statin Pretreatment in Intravenous Thrombolysis for Acute Ischemic Stroke. Stroke 46(9):2681–2684. https://doi.org/10.1161/STROKEAHA.115.010244
Scheitz JF, MacIsaac RL, Abdul-Rahim AH et al (2016) Statins and risk of poststroke hemorrhagic complications. Neurology 86(17):1590–1596. https://doi.org/10.1212/WNL.0000000000002606
Paciaroni M, Agnelli G, Corea F et al (2008) Early hemorrhagic transformation of brain infarction: rate, predictive factors, and influence on clinical outcome: results of a prospective multicenter study. Stroke 39(8):2249–2256. https://doi.org/10.1161/STROKEAHA.107.510321
Cougo-Pinto PT, Santos BL, Dias FA et al (2012) Frequency and predictors of symptomatic intracranial hemorrhage after intravenous thrombolysis for acute ischemic stroke in a Brazilian public hospital. Clinics (Sao Paulo) 67(7):739–743
Erdur H, Polymeris A, Grittner U et al (2018) A Score for Risk of Thrombolysis-Associated Hemorrhage Including Pretreatment with Statins. Front Neurol 9(74). https://doi.org/10.3389/fneur.2018.00074
Heo JH, Song D, Nam HS et al (2016) Effect and Safety of Rosuvastatin in Acute Ischemic Stroke. Stroke 18(1):87–95. https://doi.org/10.5853/jos.2015.01578
Montaner J, Bustamante A, García-Matas S et al (2016) Combination of Thrombolysis and Statins in Acute Stroke Is Safe: Results of the STARS Randomized Trial (Stroke Treatment With Acute Reperfusion and Simvastatin). Stroke 47(11):2870–2873. https://doi.org/10.1161/strokeaha.116.014600
Hong KS, Lee JS (2015) Statins in Acute Ischemic Stroke: A Systematic Review. Stroke 17(3):282–301. https://doi.org/10.5853/jos.2015.17.3.282
Liu Y, Gong P, Sun H, Zhang S, Zhou J, Zhang Y (2019 Mar) Leukoaraiosis is associated with poor outcomes after successful recanalization for large vessel occlusion stroke. Neurol Sci 40(3):585–591. https://doi.org/10.1007/s10072-018-3698-2
Lansberg MG, Albers GW, Wijman CA (2007) Symptomatic intracerebral hemorrhage following thrombolytic therapy for acute ischemic stroke: a review of the risk factors. Cerebrovasc Dis 24(1):1–10. https://doi.org/10.1159/000103110
Minhas JS, Wang X, Arima H et al (2018) Lipid-Lowering Pretreatment and Outcome Following Intravenous Thrombolysis for Acute Ischaemic Stroke: A Post Hoc Analysis of the Enhanced Control of Hypertension and Thrombolysis Stroke Study Trial. Cerebrovasc Dis 45(5-6):213–220. https://doi.org/10.1159/000488911
Cappellari M, Deluca C, Tinazzi M et al (2011) Does statin in the acute phase of ischemic stroke improve outcome after intravenous thrombolysis? A retrospective study. J Neurol Sci 308(1-2):128–134. https://doi.org/10.1016/j.jns.2011.05.026
Wang S, Lee SR, Guo SZ et al (2006) Reduction of tissue plasminogen activator-induced matrix metalloproteinase-9 by simvastatin in astrocytes. Stroke 37:1910–1912. https://doi.org/10.1161/01.str.0000226923.48905.39
Montaner J, Molina CA, Monasterio J et al (2003) Matrix metalloproteinase-9 pretreatment level predicts intracranial hemorrhagic complications after thrombolysis in human stroke. Circulation 107:598–603
Ovbiagele B, Saver JL, Starkman S et al (2007) Statin enhancement of collateralization in acute stroke. Neurology 68:2129–2131. https://doi.org/10.1212/01.wnl.0000264931.34941.f0
Cimino M, Gelosa P, Gianella A et al (2007) Statins: multiple mechanisms of action in the ischemic brain. Neuroscientist. 13(3):208–213. https://doi.org/10.1177/1073858406297121
Wang X, Dong Y, Qi X et al (2013) Cholesterol levels and risk of hemorrhagic stroke: a systematic review and meta-analysis. Stroke 44(7):1833–1839. https://doi.org/10.1161/STROKEAHA.113.001326
Sabatine MS, Wiviott SD, Im K et al (2018) Efficacy and Safety of Further Lowering of Low-Density Lipoprotein Cholesterol in Patients Starting With Very Low Levels: A Meta-analysis. JAMA Cardiol 3(9):823–828. https://doi.org/10.1001/jamacardio.2018.2258
Funding
Lifen Chen received a grant from the National Natural Science Foundation of China (grant number: 81771391).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Tan, C., Liu, X., Mo, L. et al. Statin, cholesterol, and sICH after acute ischemic stroke: systematic review and meta-analysis. Neurol Sci 40, 2267–2275 (2019). https://doi.org/10.1007/s10072-019-03995-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10072-019-03995-0