Abstract
Objectives
To generate and validate algorithms for the identification of individuals with dementia in the community setting, by the interrogation of administrative records, an inexpensive and already available source of data.
Methods
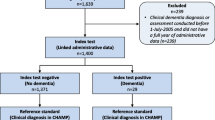
We collected and anonymized information on demented individuals 65 years of age or older from ten general practitioners (GPs) in the district of Brianza (Northern Italy) and compared this with the administrative data of the local health protection agency (Agenzia per la Tutela della Salute). Indicators of the disease in the administrative database (diagnosis of dementia in the hospital discharge records; use of cholinesterase inhibitors/memantine; neuropsychological tests; brain CT/MRI; outpatient neurological visits) were used separately and in different combinations to generate algorithms for the detection of patients with dementia.
Results
When used individually, indicators of dementia showed good specificity, but low sensitivity. By their combination, we generated different algorithms: I-therapy with ChEI/memantine or diagnosis of dementia at discharge or neuropsychological tests (specificity 97.9%, sensitivity 52.5%); II-therapy with ChEI/memantine or diagnosis of dementia at discharge or neuropsychological tests or brain CT/MRI or neurological visit (sensitivity 90.8%, specificity 70.6%); III-therapy with ChEI/memantine or diagnosis of dementia at discharge or neuropsychological tests or brain CT/MRIMRI and neurological visit (specificity 89.3%, sensitivity 73.3%).
Conclusions
These results show that algorithms obtained from administrative data are not sufficiently accurate in classifying patients with dementia, whichever combination of variables is used for the identification of the disease. Studies in large patient cohorts are needed to develop further strategies for identifying patients with dementia in the community setting.

Similar content being viewed by others
References
Scheltens P, Blennow K, Breteler MM, de Strooper B, Frisoni GB, Salloway S et al (2016) Alzheimer’s disease. Lancet 388(10043):505–517
Mazzola P, Rimoldi SM, Rossi P, Noale M, Rea F, Facchini C et al (2016) Aging in Italy: the need for new welfare strategies in an old country. Gerontologist 56(3):383–390
Collaborators GD (2018) Global, regional, and national burden of Alzheimer’s disease and other dementias, 1990–2016: a systematic analysis for the Global Burden of Disease Study 2016. Lancet Neurol
Chan KY, Wang W, Wu JJ, Liu L, Theodoratou E, Car J et al (2013) Epidemiology of Alzheimer’s disease and other forms of dementia in China, 1990-2010: a systematic review and analysis. Lancet 381(9882):2016–2023
Fiest KM, Jetté N, Roberts JI, Maxwell CJ, Smith EE, Black SE et al (2016) The prevalence and incidence of dementia: a systematic review and meta-analysis. Can J Neurol Sci 43(Suppl 1):S3–S50
Weuve J, Barnes LL, Mendes de Leon CF, Rajan KB, Beck T, Aggarwal NT et al (2018) Cognitive aging in Black and White Americans: cognition, cognitive decline, and incidence of Alzheimer disease dementia. Epidemiology 29(1):151–159
Salmon DP, Bondi MW (2009) Neuropsychological assessment of dementia. Annu Rev Psychol 60:257–282
Ritchie C, Smailagic N, Noel-Storr AH, Ukoumunne O, Ladds EC, Martin S (2017) CSF tau and the CSF tau/Abeta ratio for the diagnosis of Alzheimer’s disease dementia and other dementias in people with mild cognitive impairment (MCI). Cochrane Database Syst Rev 3:CD010803
Hornberger J, Bae J, Watson I, Johnston J, Happich M (2017) Clinical and cost implications of amyloid beta detection with amyloid beta positron emission tomography imaging in early Alzheimer’s disease - the case of florbetapir. Curr Med Res Opin 33(4):675–685
May BH, Feng M, Hyde AJ, Hügel H, Chang SY, Dong L et al (2018) Comparisons between traditional medicines and pharmacotherapies for Alzheimer disease: a systematic review and meta-analysis of cognitive outcomes. Int J Geriatr Psychiatry 33(3):449–458
Anand A, Patience AA, Sharma N, Khurana N (2017) The present and future of pharmacotherapy of Alzheimer’s disease: a comprehensive review. Eur J Pharmacol 815:364–375
Riley GF (2009) Administrative and claims records as sources of health care cost data. Med Care 47(7 Suppl 1):S51–S55
Willis AW (2015) Using administrative data to examine health disparities and outcomes in neurological diseases of the elderly. Curr Neurol Neurosci Rep 15(11):75
Kosteniuk JG, Morgan DG, O'Connell ME, Kirk A, Crossley M, Teare GF et al (2015) Incidence and prevalence of dementia in linked administrative health data in Saskatchewan, Canada: a retrospective cohort study. BMC Geriatr 15:73
Goodman RA, Lochner KA, Thambisetty M, Wingo TS, Posner SF, Ling SM (2017) Prevalence of dementia subtypes in United States Medicare fee-for-service beneficiaries, 2011–2013. Alzheimers Dement 13(1):28–37
Jaakkimainen RL, Bronskill SE, Tierney MC, Herrmann N, Green D, Young J et al (2016) Identification of physician-diagnosed Alzheimer’s disease and related dementias in population-based administrative data: a validation study using family physicians’ electronic medical records. J Alzheimers Dis 54(1):337–349
Amra S, O'Horo JC, Singh TD, Wilson GA, Kashyap R, Petersen R et al (2017) Derivation and validation of the automated search algorithms to identify cognitive impairment and dementia in electronic health records. J Crit Care 37:202–205
Takada T, Fukuma S, Yamamoto Y, Tsugihashi Y, Nagano H, Hayashi M et al (2018) Development and validation of a prediction model for functional decline in older medical inpatients. Arch Gerontol Geriatr 77:184–188
Hoogerduijn JG, Buurman BM, Korevaar JC, Grobbee DE, de Rooij SE, Schuurmans MJ (2012) The prediction of functional decline in older hospitalised patients. Age Ageing 41(3):381–387
Tay L, Lim WS, Chan M, Ali N, Mahanum S, Chew P et al (2015) New DSM-V neurocognitive disorders criteria and their impact on diagnostic classifications of mild cognitive impairment and dementia in a memory clinic setting. Am J Geriatr Psychiatry 23(8):768–779
American Medical Association Hospital (2005) International classification of diseases, 9th revision
Miller GC, Britt H (1995) A new drug classification for computer systems: the ATC extension code. Int J Biomed Comput 40(2):121–124
François M, Sicsic J, Elbaz A, Pelletier Fleury N (2017) Trends in drug prescription rates for dementia: an observational population-based study in France, 2006–2014. Drugs Aging 34(9):711–721
Albrecht JS, Hanna M, Kim D, Perfetto EM (2018) Predicting diagnosis of Alzheimer’s disease and related dementias using administrative claims. J Manag Care Spec Pharm 24(11):1138–1145
Mar J, Arrospide A, Soto-Gordoa M, Machón M, Iruin Á, Martinez-Lage P et al (2018) Validity of a computerized population registry of dementia based on clinical databases. Neurologia
Acknowledgments
The authors are extremely grateful to the General Practitioners who participated in the study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical statements
All the data included in this research were managed according to the current Italian law on privacy and authorization was obtained from the ATS Brianza to obtain and use the administrative data for the purposes of this study.
No experiments on animals have been conducted for the present study.
Conflict of interest
The authors declare that they have no conflicts of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
DiFrancesco, J.C., Pina, A., Giussani, G. et al. Generation and validation of algorithms to identify subjects with dementia using administrative data. Neurol Sci 40, 2155–2161 (2019). https://doi.org/10.1007/s10072-019-03968-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10072-019-03968-3