Abstract
Background and purpose
Neurological manifestations and neuroimaging abnormalities are common in patients with severe preeclampsia; however, the differences between these abnormal features occurring during early- and late-onset severe preeclampsia are unclear, and the factors associated with abnormal imaging changes in patients with neurological manifestations have not yet been fully elucidated.
Materials and methods
A retrospective study was conducted on 172 patients with severe preeclampsia from January 2017 to June 2018 in the Department of Neurology and Obstetrics, Shengjing Hospital of China Medical University. The neurological manifestations, clinical parameters, laboratory, and neuroimaging findings were analyzed.
Results
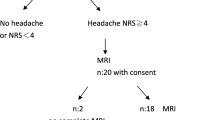
Early- and late-onset preeclampsia were diagnosed in 83 and 89 patients, respectively. Headache and dizziness were more common in patients with early-onset preeclampsia than in patients with late-onset preeclampsia (p = 0.013, p = 0.004, respectively). Serum uric acid, creatinine, and urea nitrogen were significantly elevated in the patients with early-onset preeclampsia (p < 0.001, p = 0.004, and p = 0.005, respectively). Neuroimaging was performed in 81 patients, of which 57 were positive. Findings indicating cerebral edema were the most common neuroimaging abnormality. Gestational weeks (p = 0.014), headache (p < 0.001), and blood urea nitrogen level (p = 0.027) may be associated with positive imaging findings. By multiple logistic regression, headache (OR = 10.2, 95% CI, 2.4–42.7; p = 0.002) proved to be an independent factor associated with neuroimaging abnormality.
Conclusions
Neurological symptoms such as headache and dizziness were more common in patients with early-onset preeclampsia. Renal dysfunction may also associate with early-onset severe preeclampsia. Cerebral edema was the most common neuroimaging abnormality, and headache might be independently associated with abnormal imagine changes.




Similar content being viewed by others
References
Frontera JA, Ahmed W (2014) Neurocritical care complications of pregnancy and puerperum. J Crit Care 29(6):1069–1081. https://doi.org/10.1016/j.jcrc.2014.07.010
Singh R, Hayaran N, Nagar D, Jain A (2018) Spectrum of neurological complications in eclampsia in a tertiary care hospital in India. J Obstet Gynaecol Can 40(7):876–882. https://doi.org/10.1016/j.jogc.2017.08.038
Di X, Mai H, Zheng Z, Guo K, Morse AN, Liu H (2018) Neuroimaging findings in women who develop neurologic symptoms in severe preeclampsia with or without eclampsia. Hypertens Res 41(8):598–604. https://doi.org/10.1038/s41440-018-0051-3
Abalos E, Cuesta C, Carroli G, Qureshi Z, Widmer M, Vogel JP, Souza JP, N WHOMSM (2014) Pre- eclampsia, eclampsia and adverse maternal and perinatal outcomes: a secondary analysis of the World Health Organization multicountry survey on maternal and newborn health. BJOG 121:14–24. https://doi.org/10.1111/1471-0528.12629
Duckitt K, Harrington D (2005) Risk factors for pre-eclampsia at antenatal booking: systematic review of controlled studies. Br Med J 330(7491):565–567. https://doi.org/10.1136/bmj.38380.674340.E0
Haddad B, Sibai BM (2009) Expectant management in pregnancies with severe pre-eclampsia. Semin Perinatol 33(3):143–151. https://doi.org/10.1053/j.semperi.2009.02.002
Li XL, Guo PL, Xue Y, Gou WL, Tong M, Chen Q (2016) An analysis of the differences between early and late preeclampsia with severe hypertension. Pregnancy Hypertens 6(1):47–52. https://doi.org/10.1016/j.preghy.2015.12.003
Huppertz B (2008) Placental origins of preeclampsia - challenging the current hypothesis. Hypertension 51(4):970–975. https://doi.org/10.1161/hypertensionaha.107.107607
Junewar V, Verma R, Sankhwar PL, Garg RK, Singh MK, Malhotra HS, Sharma PK, Parihar A (2014) Neuroimaging features and predictors of outcome in eclamptic encephalopathy: a prospective observational study. Am J Neuroradiol 35(9):1728–1734. https://doi.org/10.3174/ajnr.A3923
Roberts JM, August PA, Bakris G, Barton JR, Bernstein IM, Druzin M, Gaiser RR, Granger JP, Jeyabalan A, Johnson DD, Karumanchi SA, Lindheimer M, Owens MY, Saade GR, Sibai BM, Spong CY, Tsigas E, Joseph GF, O'Reilly N, Politzer A, Son S, Ngaiza K, Task Force Hypertension P, Amer Coll Obstetricians G (2013) Hypertension in pregnancy report of the American College of Obstetricians and Gynecologists’ task force on hypertension in pregnancy. Obstet Gynecol 122(5):1122–1131. https://doi.org/10.1097/01.aog.0000437382.03963.88
Tranquilli AL, Brown MA, Zeeman GG, Dekker G, Sibai BM (2013) The definition of severe and early-onset preeclampsia. Statements from the International Society for the Study of Hypertension in pregnancy (ISSHP). Pregnancy Hypertens 3(1):44–47. https://doi.org/10.1016/j.preghy.2012.11.001
von Dadelszen P, Magee LA (2014) Pre-eclampsia: an update. Curr Hypertens Rep 16(8):454. https://doi.org/10.1007/s11906-014-0454-8
Stanek J (2018) Histological features of shallow placental implantation unify early-onset and late-onset preeclampsia. Pediatr Dev Pathol. https://doi.org/10.1177/1093526618803759
Phipps EA, Thadhani R, Benzing T, Karumanchi SA (2019) Pre-eclampsia: pathogenesis, novel diagnostics and therapies. Nat Rev Nephrol. https://doi.org/10.1038/s41581-019-0119-6
Seeho SK, Algert CS, Roberts CL, Ford JB (2016) Early-onset preeclampsia appears to discourage subsequent pregnancy but the risks may be overestimated. Am J Obstet Gynecol 215(6):785.e1–785.e8. https://doi.org/10.1016/j.ajog.2016.07.038
El-Sayed AAF (2017) Preeclampsia: a review of the pathogenesis and possible management strategies based on its pathophysiological derangements. Taiwan J Obstet Gynecol 56(5):593–598. https://doi.org/10.1016/j.tjog.2017.08.004
Lisonkova S, Joseph KS (2013) Incidence of preeclampsia: risk factors and outcomes associated with early- versus late-onset disease. Am J Obstet Gynecol 209(6):544.e1–544.e12. https://doi.org/10.1016/j.ajog.2013.08.019
Terry AR, Merker VL, Barker FG II, Leffert L, Bateman BT, Souter I, Plotkin SR (2015) Pregnancy complications in women with rare tumor suppressor syndromes affecting central and peripheral nervous system. Am J Obstet Gynecol 213(1):108–109. https://doi.org/10.1016/j.ajog.2015.02.013
Edlow JA, Caplan LR, O'Brien K, Tibbles CD (2013) Diagnosis of acute neurological emergencies in pregnant and post-partum women. Lancet Neurol 12(2):175–185. https://doi.org/10.1016/s1474-4422(12)70306-x
Junus K, Wikstrom A-K, Larsson A, Olovsson M (2014) Placental expression of proBNP/NT-proBNP and plasma levels of NT-proBNP in early- and late-onset preeclampsia. Am J Hypertens 27(9):1225–1230. https://doi.org/10.1093/ajh/hpu033
Maghsoudlou S, Cnattingius S, Stephansson O, Aarabi M, Semnani S, Montgomery SM, Bahmanyar S (2016) Maternal haemoglobin concentrations before and during pregnancy and stillbirth risk: a population-based case-control study. BMC Pregnancy Childbirth 16:135. https://doi.org/10.1186/s12884-016-0924-x
McCartney CP, Spargo B, Lorincz AB, Lefebvre Y, Newton RE (1964) Renal structure and function in pregnant patients with acute hypertension; OSMOLAR concentration. Am J Obstet Gynecol 90:579–592. https://doi.org/10.1016/s0002-9378(16)34985-7
Min Z, Gnann JW Jr (2014) Reversible posterior leukoencephalopathy syndrome. Intern Emerg Med 9(3):341–342. https://doi.org/10.1007/s11739-013-1011-1
Kutlesic MS, Kutlesic RM, Koratevic GP (2015) Posterior reversible encephalopathy syndrome in eclamptic patients: neuroradiological manifestation, pathogenesis and management. Med Pregl 68(1–2):53–58
Kiroglu Y, Calli C, Yunten N, Kitis O, Kocaman A, Karabulut N, Isaev H, Yagci B (2006) Diffusion-weighted MR imaging of viral encephalitis. Neuroradiology 48(12):875–880. https://doi.org/10.1007/s00234-006-0143-7
Kalaiselvan MS, Renuka MK, Arunkumar AS (2017) Clinical features and outcomes of patients with posterior reversible encephalopathy syndrome. Indian J Crit Care Med 21(7):453–456. https://doi.org/10.4103/ijccm.IJCCM_79_17
Singh RR, Ozyilmaz N, Waller S, U-King-Im J-M, Lim M, Siddiqui A, Sinha MD (2014) A study on clinical and radiological features and outcome in patients with posterior reversible encephalopathy syndrome (PRES). Eur J Pediatr 173(9):1225–1231. https://doi.org/10.1007/s00431-014-2301-y
Miller EC, Gatollari HJ, Too G, Boehme AK, Leffert L, Marshall RS, Elkind MSV, Willey JZ (2017) Risk factors for pregnancy-associated stroke in women with preeclampsia. Stroke 48(7):1752–175+. https://doi.org/10.1161/strokeaha.117.017374
Robbins MS, Farmakidis C, Dayal AK, Lipton RB (2015) Acute headache diagnosis in pregnant women. Neurology 85(12):1024–1030. https://doi.org/10.1212/wnl.0000000000001954
Ramchandren S, Cross BJ, Liebeskind DS (2007) Emergent headaches during pregnancy: correlation between neurologic examination and neuroimaging. Am J Neuroradiol 28(6):1085–1087. https://doi.org/10.3174/ajnr.A0506
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclaimer
The authors alone are responsible for the content and writing of the paper.
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical standards
This study conformed to the Ethical Guidelines for Medical and Health Research Involving Human Subjects endorsed by the Chinese government.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Dong, X., Nao, J. Neurological manifestations and neuroimaging presentations in patients with severe preeclampsia: predisposing factors and clinical implications. Neurol Sci 40, 1245–1253 (2019). https://doi.org/10.1007/s10072-019-03833-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10072-019-03833-3