Abstract
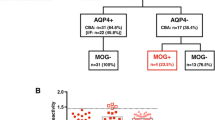
Headache and visual disturbances are the main presenting symptoms of idiopathic intracranial hypertension (IIH) characterized by increased intracranial pressure (ICP) with an unknown cause. We aimed to investigate the antibodies against optic neuritis-associated glial antigens, aquaporin-4 (AQP4) and myelin oligodendrocyte glycoprotein (MOG) and uncharacterized neuronal membrane antigens in IIH patients. Consecutive patients diagnosed according to Friedman revised diagnostic criteria and control subjects were included after their consent. All serum samples were analyzed for antibodies against AQP4 and MOG using cell-based immunofluorescent assays and for uncharacterized neuronal membrane antigens by indirect immunocytochemistry utilizing live neurons. Sera of 34 patients with IIH and 40 control subjects were investigated but none of the patients showed AQP4 and MOG antibodies. However, serum IgG of five IIH patients showed reactivity against membrane antigens of rat hippocampal and cortical neurons. Interestingly, three out of these five patients had nonspecific white matter lesions on MRI, whereas only four of all other patients had these lesions (p = 0.048). AQP4 and MOG antibodies do not seem to have a role in the pathophysiology of IIH. However, association of immunocytochemistry findings with the presence of white matter lesions may suggest that immunological factors contribute to the pathogenesis of IIH in at least some of the patients.


Similar content being viewed by others
References
Wakerley BR, Tan MH, Ting EY (2015) Idiopathic intracranial hypertension. Cephalalgia 35:248–261. doi:10.1177/0333102414534329
Friedman DI, Liu GT, Digre KB (2013) Revised diagnostic criteria for the pseudotumor cerebri syndrome in adults and children. Neurology 81:1159–1165. doi:10.1212/WNL.0b013e3182a55f17
Baykan B, Ekizoglu E, Altiokka Uzun G (2015) An update on the pathophysiology of idiopathic intracranial hypertension alias pseudotumor cerebri. Agri 27:63–72. doi:10.5505/agri.2015.22599
Sinclair AJ, Woolley R, Mollan SP (2014) Idiopathic intracranial hypertension. JAMA 312:1059–1060. doi:10.1001/jama.2014.8894
Sinclair AJ, Ball AK, Burdon MA, Clarke CE, Stewart PM, Curnow SJ, Rauz S (2008) Exploring the pathogenesis of IIH: an inflammatory perspective. J Neuroimmunol 201-202:212–220. doi:10.1016/j.jneuroim.2008.06.029
Edwards LJ, Sharrack B, Ismail A, Tench CR, Gran B, Dhungana S, Brettschneider J, Tumani H, Constantinescu CS (2013) Increased levels of interleukins 2 and 17 in the cerebrospinal fluid of patients with idiopathic intracranial hypertension. Am J Clin Exp Immunol 2:234–244
Samanci B, Samanci Y, Tuzun E, Altiokka-Uzun G, Ekizoglu E, Icoz S, Sahin E, Kucukali CI, Baykan B (2016) Evidence for potential involvement of pro-inflammatory adipokines in the pathogenesis of idiopathic intracranial hypertension. Cephalalgia. doi:10.1177/0333102416650705
Altiokka-Uzun G, Tuzun E, Ekizoglu E, Ulusoy C, Yentur S, Kurtuncu M, Saruhan-Direskeneli G, Baykan B (2015) Oligoclonal bands and increased cytokine levels in idiopathic intracranial hypertension. Cephalalgia 35:1153–1161. doi:10.1177/0333102415570762
Verkman AS (2008) Mammalian aquaporins: diverse physiological roles and potential clinical significance. Expert Rev Mol Med 10:e13. doi:10.1017/S1462399408000690
Papadopoulos MC, Manley GT, Krishna S, Verkman AS (2004) Aquaporin-4 facilitates reabsorption of excess fluid in vasogenic brain edema. FASEB J 18:1291–1293. doi:10.1096/fj.04-1723fje
Amiry-Moghaddam M, Ottersen OP (2003) The molecular basis of water transport in the brain. Nat Rev Neurosci 4:991–1001. doi:10.1038/nrn1252
Dhungana S, Waters P, Ismail A, Woodroofe N, Vincent A, Sharrack B (2010) Absence of aquaporin-4 antibodies in patients with idiopathic intracranial hypertension. J Neurol 257:1211–1212. doi:10.1007/s00415-010-5499-2
Ekizoglu E, Icoz S, Tuzun E, Birisik O, Kocasoy-Orhan E, Akman-Demir G, Baykan B (2012) Aquaporin-4 antibodies are not present in patients with idiopathic intracranial hypertension. Cephalalgia 32:198–202. doi:10.1177/0333102411434167
Doppler K, Schutt M, Sommer C (2016) Decreased levels of aquaporin-4 in the cerebrospinal fluid of patients with idiopathic intracranial hypertension. Cephalalgia. doi:10.1177/0333102416630592
Lechner C, Baumann M, Hennes EM, Schanda K, Marquard K, Karenfort M, Leiz S, Pohl D, Venkateswaran S, Pritsch M, Koch J, Schimmel M, Hausler M, Klein A, Blaschek A, Thiels C, Lucke T, Gruber-Sedlmayr U, Kornek B, Hahn A, Leypoldt F, Sandrieser T, Gallwitz H, Stoffels J, Korenke C, Reindl M, Rostasy K (2016) Antibodies to MOG and AQP4 in children with neuromyelitis optica and limited forms of the disease. J Neurol Neurosurg Psychiatry 87:897–905. doi:10.1136/jnnp-2015-311743
Ramanathan S, Dale RC, Brilot F (2016) Anti-MOG antibody: the history, clinical phenotype, and pathogenicity of a serum biomarker for demyelination. Autoimmun Rev 15:307–324. doi:10.1016/j.autrev.2015.12.004
Sadaba MC, Gonzalez Porque P, Masjuan J, Alvarez-Cermeno JC, Bootello A, Villar LM (2004) An ultrasensitive method for the detection of oligoclonal IgG bands. J Immunol Methods 284:141–145
Petzold A (2013) Intrathecal oligoclonal IgG synthesis in multiple sclerosis. J Neuroimmunol 262:1–10. doi:10.1016/j.jneuroim.2013.06.014
Waters P, Woodhall M, O'Connor KC, Reindl M, Lang B, Sato DK, Jurynczyk M, Tackley G, Rocha J, Takahashi T, Misu T, Nakashima I, Palace J, Fujihara K, Leite MI, Vincent A (2015) MOG cell-based assay detects non-MS patients with inflammatory neurologic disease. Neurol Neuroimmunol Neuroinflamm 2:e89. doi:10.1212/NXI.0000000000000089
Irani SR, Bera K, Waters P, Zuliani L, Maxwell S, Zandi MS, Friese MA, Galea I, Kullmann DM, Beeson D, Lang B, Bien CG, Vincent A (2010) N-methyl-D-aspartate antibody encephalitis: temporal progression of clinical and paraclinical observations in a predominantly non-paraneoplastic disorder of both sexes. Brain 133:1655–1667. doi:10.1093/brain/awq113
Gezen-Ak D, Dursun E, Yilmazer S (2011) The effects of vitamin D receptor silencing on the expression of LVSCC-A1C and LVSCC-A1D and the release of NGF in cortical neurons. PLoS One 6:e17553. doi:10.1371/journal.pone.0017553
Dursun E, Gezen-Ak D, Yilmazer S (2013) A new mechanism for amyloid-beta induction of iNOS: vitamin D-VDR pathway disruption. J Alzheimers Dis 36:459–474. doi:10.3233/JAD-130416
Lyra TG, Martin Mda G, Carvalho Rdo C, Oliveira CR, Godoy LF, Delgado Dde S, Cerri GG, Leite Cda C (2013) Pseudotumoral presentation of primary central nervous system vasculitis. Arq Neuropsiquiatr 71:333–335
Ekizoglu E, Tuzun E, Woodhall M, Lang B, Jacobson L, Icoz S, Bebek N, Gurses C, Gokyigit A, Waters P, Vincent A, Baykan B (2014) Investigation of neuronal autoantibodies in two different focal epilepsy syndromes. Epilepsia 55:414–422. doi:10.1111/epi.12528
Paul L, Madan M, Rammling M, Chigurupati S, Chan SL, Pattisapu JV (2011) Expression of aquaporin 1 and 4 in a congenital hydrocephalus rat model. Neurosurgery 68:462–473. doi:10.1227/NEU.0b013e3182011860
Skjolding AD, Holst AV, Broholm H, Laursen H, Juhler M (2013) Differences in distribution and regulation of astrocytic aquaporin-4 in human and rat hydrocephalic brain. Neuropathol Appl Neurobiol 39:179–191. doi:10.1111/j.1365-2990.2012.01275.x
Zador Z, Bloch O, Yao X, Manley GT (2007) Aquaporins: role in cerebral edema and brain water balance. Prog Brain Res 161:185–194. doi:10.1016/S0079-6123(06)61012-1
Friedman DI (2012) Aquaporin-4 antibodies and idiopathic intracranial hypertension: the jury is in and the channels are out. Cephalalgia 32:183–184. doi:10.1177/0333102411436124
Jarius S, Ruprecht K, Kleiter I, Borisow N, Asgari N, Pitarokoili K, Pache F, Stich O, Beume LA, Hummert MW, Ringelstein M, Trebst C, Winkelmann A, Schwarz A, Buttmann M, Zimmermann H, Kuchling J, Franciotta D, Capobianco M, Siebert E, Lukas C, Korporal-Kuhnke M, Haas J, Fechner K, Brandt AU, Schanda K, Aktas O, Paul F, Reindl M, Wildemann B and in cooperation with the Neuromyelitis Optica Study G (2016) MOG-IgG in NMO and related disorders: a multicenter study of 50 patients. Part 2: epidemiology, clinical presentation, radiological and laboratory features, treatment responses, and long-term outcome. J Neuroinflammation 13:280. doi: 10.1186/s12974-016-0718-0
Acknowledgements
The authors thank the participants for taking part in the study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
This study was supported by the Istanbul University Scientific Research Fund (project number: 2016-21774) and by a grant from the Hellenic Neuroimmunology Academy.
Conflict of interest
J. Tzartos has shares in the research and diagnostic center Tzartos NeuroDiagnostics. All others declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Altıokka-Uzun, G., Erdağ, E., Baykan, B. et al. Glial and neuronal antibodies in patients with idiopathic intracranial hypertension. Neurol Sci 38, 1817–1822 (2017). https://doi.org/10.1007/s10072-017-3066-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10072-017-3066-7