Abstract
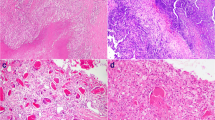
Rheumatoid nodules (RNs) are the most common extra-articular manifestation of rheumatoid arthritis and are also seen in patients with other autoimmune and inflammatory diseases. The development of RNs includes histopathological stages of acute unspecified inflammation, granulomatous inflammation with no or minimal necrosis, necrobiotic granulomas typically with central fibrinoid necrosis surrounded by palisading epithelioid macrophages and other cells, and likely an advanced stage of “ghost” lesions containing cystic or calcifying/calcified areas. In this article, we review RN pathogenesis, histopathological features in different stages, diagnostically related clinical manifestations, as well as diagnosis and differential diagnosis of RNs with an in-depth discussion about challenges in distinguishing RNs from their mimics. While the pathogenesis of RN formation remains elusive, it is hypothesized that some RNs with dystrophic calcification may be in transition and may be in coexistence or collision with another lesion in patients with RA or other soft tissue diseases and comorbidities. The diagnosis of typical or mature RNs in usual locations can be readily made by clinical findings often with classic RN histopathology, but in many cases, particularly with atypical or immature RNs and/or unusual locations, the clinical and histopathological diagnosis can be challenging requiring extensive examination of the lesional tissue with histological and immunohistochemical markers to identify unusual RNs in the clinical context or other lesions that may be coexisting with classic RNs. Proper diagnosis of RNs is critical for appropriate treatment of patients with RA or other autoimmune and inflammatory diseases.



Similar content being viewed by others
References
Tilstra JS, Lienesch DW (2015) Rheumatoid nodules. Dermatol Clin 33:361–371. https://doi.org/10.1016/j.det.2015.03.004
García-Patos V (2007) Rheumatoid nodule. Semin Cutan Med Surg 26:100–107. https://doi.org/10.1016/j.sder.2007.02.007
Sayah A, English JC 3rd (2005) Rheumatoid arthritis: a review of the cutaneous manifestations. J Am Acad Dermatol 53:191–209; quiz 210-2. https://doi.org/10.1016/j.jaad.2004.07.023
Prete M, Racanelli V, Digiglio L, Vacca A, Dammacco F, Perosa F (2011) Extra-articular manifestations of rheumatoid arthritis: an update. Autoimmun Rev 11:123–131. https://doi.org/10.1016/j.autrev.2011.09.001
Kaye BR, Kaye RL, Bobrove A (1984) Rheumatoid nodules. Review of the spectrum of associated conditions and proposal of a new classification, with a report of four seronegative cases. Am J Med 76:279–292. https://doi.org/10.1016/0002-9343(84)90787-3
Saito-Sasaki N, Sawada Y, Omoto D et al (2016) A possible pathogenetic role of IL-23/IL-17 axis in rheumatoid nodules in patients with rheumatoid arthritis. Clin Immunol 170:20–21. https://doi.org/10.1016/j.clim.2016.07.002
Young A, Koduri G (2007) Extra-articular manifestations and complications of rheumatoid arthritis. Best Pract Res Clin Rheumatol 21:907–927. https://doi.org/10.1016/j.berh.2007.05.007
Lu JQ, Popovic S, Provias J, Cenic A (2021) Collision lesions of calcifying pseudoneoplasm of the neuraxis and rheumatoid nodules: a case report with new pathogenic insights. Int J Surg Pathol 29:314–320. https://doi.org/10.1177/1066896920941939
Dubois EL, Friou GJ, Chandor S (1972) Rheumatoid nodules and rheumatoid granulomas in systemic lupus erythematosus. JAMA 220:515–518
Hahn BH, Yardley JH, Stevens MB (1970) “Rheumatoid” nodules in systemic lupus erythematosus. Ann Intern Med 72:49–58. https://doi.org/10.7326/0003-4819-72-1-49
Conforti A, Di Cola I, Pavlych V, et al (2021) Beyond the joints, the extra-articular manifestations in rheumatoid arthritis. Autoimmun Rev 20:102735. https://doi.org/10.1016/j.autrev.2020.102735.
Pearson ME, Kosco M, Huffer W, Winter W, Engelbrecht JA, Steigerwald JC (1987) Rheumatoid nodules of the spine: case report and review of the literature. Arthritis Rheum 30:709–713. https://doi.org/10.1002/art.1780300616
Kato K, Segami N, Fukuda H, Minato H (2014) Rheumatoid nodule in the lower lip of a patient with rheumatoid arthritis: a novel case report and review of literature. J Oral Maxillofac Surg 72:1532.e1–1532.e5. https://doi.org/10.1016/j.joms.2014.03.034
Kim RC, Collins GH (1981) The neuropathology of rheumatoid disease. Hum Pathol 12:5–15. https://doi.org/10.1016/s0046-8177(81)80236-5
Martins S, Fernandes BM, Bernardes M, Melo D, Neto T (2021) Rheumatoid nodule simulating a parotid tumor. Head Neck Pathol 15:334–340. https://doi.org/10.1007/s12105-020-01175-7
Choi T, Kim HK, Lee DG (2018) Rheumatoid nodule at the scrotum: a rare manifestation of rheumatoid arthritis. J Rheumatol 45:1198–1199. https://doi.org/10.3899/jrheum.171173
Nahm CB, Mittal A, Gill AJ, Samra J (2017) Pancreatic rheumatoid nodule: case report and review of the literature. Pancreas 46:e45–e47. https://doi.org/10.1097/MPA.0000000000000799
Levy Y, Stalley P, Bleasel J (2004) Thoracic spinal cord compression by a rheumatoid nodule. Intern Med J 34:137–138. https://doi.org/10.1111/j.1444-0903.2004.00553.x
Bang S, Kim Y, Jang K, Paik SS, Shin SJ (2019) Clinicopathologic features of rheumatoid nodules: a retrospective analysis. Clin Rheumatol 38:3041–3048. https://doi.org/10.1007/s10067-019-04668-1
Chaganti S, Joshy S, Hariharan K, Rashid M (2013) Rheumatoid nodule presenting as Morton’s neuroma. J Orthop Traumatol 14:219–222. https://doi.org/10.1007/s10195-012-0215-x
Groisman GM, Schafer I, Amar M, Sabo E (2002) Expression of the histiocytic marker PG-M1 in granuloma annulare and rheumatoid nodules of the skin. J Cutan Pathol 29:590–595. https://doi.org/10.1034/j.1600-0560.2002.291004.x
Knoess M, Krukemeyer MG, Kriegsmann J, Thabe H, Otto M, Krenn V (2008) Colocalization of C4d deposits/CD68+ macrophages in rheumatoid nodule and granuloma annulare: immunohistochemical evidence of a complement-mediated mechanism in fibrinoid necrosis. Pathol Res Pract 204:373–378. https://doi.org/10.1016/j.prp.2008.01.009
Lu JQ, Mohammadi WJB, Fong C et al (2022) Spinal calcifying pseudoneoplasm of the neuraxis (CAPNON) and CAPNON-like lesions: CAPNON overlapping with calcified synovial cysts. Pathology 54:573–579. https://doi.org/10.1016/j.pathol.2022.01.003
Gasparyan AY, Ayvazyan L, Blackmore H, Kitas GD (2011) Writing a narrative biomedical review: considerations for authors, peer reviewers, and editors. Rheumatol Int 31:1409–1417. https://doi.org/10.1007/s00296-011-1999-3
Highton J, Hessian PA, Stamp L (2007) The Rheumatoid nodule: peripheral or central to rheumatoid arthritis? Rheumatology (Oxford) 46:1385–1387. https://doi.org/10.1093/rheumatology/kem163
Hølund B, Clemmensen I (1984) Rheumatoid nodules: A lightmicroscopical study with special reference to fibrin and fibronectin. Histochemistry 80:463–467. https://doi.org/10.1007/BF00495435
Hügle T, Nasi S, Ehirchiou D, Omoumi P, So A, Busso N (2022) Fibrin deposition associates with cartilage degeneration in arthritis. EBioMedicine 81:104081. https://doi.org/10.1016/j.ebiom.2022.104081
Kato H, Yamakawa M, Ogino T (2000) Complement mediated vascular endothelial injury in rheumatoid nodules: a histopathological and immunohistochemical study. J Rheumatol 27:1839–1847
Miyasaka N, Sato K, Yamamoto K, Goto M, Nishioka K (1989) Immunological and immunohistochemical analysis of rheumatoid nodules. Ann Rheum Dis 48:220–226. https://doi.org/10.1136/ard.48.3.220
Wikaningrum R, Highton J, Parker A et al (1998) Pathogenic mechanisms in the rheumatoid nodule: comparison of proinflammatory cytokine production and cell adhesion molecule expression in rheumatoid nodules and synovial membranes from the same patient. Arthritis Rheum 41:1783–1797. https://doi.org/10.1002/1529-0131(199810)41:10<1783::AID-ART10>3.0.CO;2-W
Stamp LK, Easson A, Lehnigk U, Highton J, Hessian PA (2008) Different T cell subsets in the nodule and synovial membrane: absence of interleukin-17A in rheumatoid nodules. Arthritis Rheum 58:1601–1608. https://doi.org/10.1002/art.23455
Millier MJ, Lazaro K, Stamp LK, Hessian PA (2020) The contribution from interleukin-27 towards rheumatoid inflammation: insights from gene expression. Genes Immun 21:249–259. https://doi.org/10.1038/s41435-020-0102-z
Hessian PA, Highton J, Kean A, Sun CK, Chin M (2003) Cytokine profile of the rheumatoid nodule suggests that it is a Th1 granuloma. Arthritis Rheum 48:334–338. https://doi.org/10.1002/art.10776
Iwaszko M, Biały S, Bogunia-Kubik K (2021) Significance of interleukin (IL)-4 and IL-13 in inflammatory arthritis Cells 10:3000. https://doi.org/10.3390/cells10113000
Sarkar S, Tesmer LA, Hindnavis V, Endres JL, Fox DA (2007) Interleukin-17 as a molecular target in immune-mediated arthritis: immunoregulatory properties of genetically modified murine dendritic cells that secrete interleukin-4. Arthritis Rheum 56:89–100. https://doi.org/10.1002/art.22311
Petrelli A, van Wijk F (2016) CD8(+) T cells in human autoimmune arthritis: the unusual suspects. Nat Rev Rheumatol 12:421–428. https://doi.org/10.1038/nrrheum.2016.74
Weyand CM, Xie C, Goronzy JJ (1992) Homozygosity for the HLA-DRB1 allele selects for extraarticular manifestations in rheumatoid arthritis. J Clin Invest 89:2033–2039. https://doi.org/10.1172/JCI115814
Mattey DL, Dawes PT, Fisher J et al (2002) Nodular disease in rheumatoid arthritis: association with cigarette smoking and HLA-DRB1/TNF gene interaction. J Rheumatol 29:2313–2318
Hirohashi N, Sakai T, Sairyo K et al (2007) Lumbar radiculopathy caused by extradural rheumatoid nodules. Case report J Neurosurg Spine 7:352–356. https://doi.org/10.3171/SPI-07/09/352
Tsegaye M, Bassi S, Ashpole RD (2003) Extradural spinal cord compression by rheumatoid nodule. Br J Neurosurg 17:255–257. https://doi.org/10.1080/0268869031000153170
Sasaki S, Nakamura K, Oda H, Fukasawa K, Kurokawa T (1997) Thoracic myelopathy due to intraspinal rheumatoid nodules. Scand J Rheumatol 26:227–228. https://doi.org/10.3109/03009749709065688
Richmond I, Jones AW (1989) Rheumatoid nodule formation within the lumbar extradural space. J Neurol Neurosurg Psychiatry 52:414. https://doi.org/10.1136/jnnp.52.3.414
Palmer DG, Hogg N, Denholm I, Allen CA, Highton J, Hessian PA (1987) Comparison of phenotype expression by mononuclear phagocytes within subcutaneous gouty tophi and rheumatoid nodules. Rheumatol Int 7:187–193. https://doi.org/10.1007/BF00541376
Fairburn B (1975) Spinal cord compression by a rheumatoid nodule. J Neurol Neurosurg Psychiatry 38:1056–1058. https://doi.org/10.1136/jnnp.38.11.1056
Sokoloff L, Mccluskey RT, Bunim JJ (1953) The vascularity of the early subcutaneous nodules of rheumatoid arthritis. Bull N Y Acad Med 29:733–734
Boulman N, Slobodin G, Rozenbaum M, Rosner I (2005) Calcinosis in rheumatic diseases. Semin Arthritis Rheum 34:805–812. https://doi.org/10.1016/j.semarthrit.2005.01.016
Arakawa H, Honma K, Shida H, Saito Y, Morikubo H (2003) Computed tomography findings of Caplan syndrome. J Comput Assist Tomogr 27:758–760. https://doi.org/10.1097/00004728-200309000-00013
Srinivas S, Dhelaria R, Pai D, Black F, Cooper R (2007) Multiple calcified pulmonary nodules: an unusual presentation of rheumatoid lung. Clin Radiol 62:274–276. https://doi.org/10.1016/j.crad.2006.10.001
Mjaavatten MD, Bykerk VP (2013) Early rheumatoid arthritis: the performance of the 2010 ACR/EULAR criteria for diagnosing RA. Best Pract Res Clin Rheumatol 27:451–466. https://doi.org/10.1016/j.berh.2013.09.001
Nyhäll-Wåhlin BM, Turesson C, Jacobsson LT et al (2011) The presence of rheumatoid nodules at early rheumatoid arthritis diagnosis is a sign of extra-articular disease and predicts radiographic progression of joint destruction over 5 years. Scand J Rheumatol 40:81–87. https://doi.org/10.3109/03009742.2010.509103
Patatanian E, Thompson DF (2002) A review of methotrexate-induced accelerated nodulosis. Pharmacotherapy 22:1157–1162. https://doi.org/10.1592/phco.22.13.1157.33525
Kerstens PJ, Boerbooms AM, Jeurissen ME, Fast JH, Assmann KJ, van de Putte LB (1992) Accelerated nodulosis during low dose methotrexate therapy for rheumatoid arthritis. J Rheumatol 19:867–871
Veys EM, De Keyser F (1993) Rheumatoid nodules: differential diagnosis and immunohistological findings. Ann Rheum Dis 52:625–626. https://doi.org/10.1136/ard.52.9.625
Falcini F, Taccetti G, Ermini M et al (1997) Methotrexate-associated appearance and rapid progression of rheumatoid nodules in systemic-onset juvenile rheumatoid arthritis. Arthritis Rheum 40:175–178. https://doi.org/10.1002/art.1780400122
Kremer JM, Lee JK (1986) The safety and efficacy of the use of methotrexate in long-term therapy for rheumatoid arthritis. Arthritis Rheum 29:822–831. https://doi.org/10.1002/art.1780290702
Couret M, Combe B, Chuong VT et al (1988) Rheumatoid nodulosis: report of two new cases and discussion of diagnostic criteria. J Rheumatol 15:1427–1430
Roux F, Wattiaux MJ, Hayem G, Palazzo E, Kahn MF, Meyer O (2006) Rheumatoid nodulosis. Two cases with destructive polyarthritis after 20 years. Joint Bone Spine 73:208–211. https://doi.org/10.1016/j.jbspin.2005.05.007
Maldonado I, Eid H, Rodriguez GR, Rillo OL, Barcat JA, Reginato AJ (2003) Rheumatoid nodulosis: is it a different subset of rheumatoid arthritis? J Clin Rheumatol 9:296–305. https://doi.org/10.1097/01.rhu.0000090260.82835.64
Sienknecht CW, Urowitz MB, Pruzanski W, Stein HB (1977) Felty’s syndrome. Clinical and serological analysis of 34 cases. Ann Rheum Dis 36:500–507. https://doi.org/10.1136/ard.36.6.500
Gabriel SE, Crowson CS, Kremers HM et al (2003) Survival in rheumatoid arthritis: a population-based analysis of trends over 40 years. Arthritis Rheum 48:54–58. https://doi.org/10.1002/art.10705
Sanders TG, Linares R, Su A (1998) Rheumatoid nodule of the foot: MRI appearances mimicking an indeterminate soft tissue mass. Skelet Radiol 27:457–460. https://doi.org/10.1007/s002560050418
El-Noueam KI, Giuliano V, Schweitzer ME, O'Hara BJ (1997) Rheumatoid nodules: MR/pathological correlation. J Comput Assist Tomogr 21:796–799. https://doi.org/10.1097/00004728-199709000-00027
Koslow M, Young JR, Yi ES et al (2019) Rheumatoid pulmonary nodules: clinical and imaging features compared with malignancy. Eur Radiol 29:1684–1692. https://doi.org/10.1007/s00330-018-5755-x
Kumar V, Abbas AK, Aster JC (2020) Robbins and Cotran pathologic basis of disease, 10th edn. Elsevier, Philadelphia
Nelson CA, Zhong CS, Hashemi DA et al (2020) A multicenter cross-sectional study and systematic review of necrobiotic xanthogranuloma with proposed diagnostic criteria. JAMA Dermatol 156:270–279. https://doi.org/10.1001/jamadermatol.2019.4221
Lindberg MR (2019) Diagnostic pathology: soft tissue tumors, 3rd edn. Elsevier, Philadelphia
Benedek TG (1984) Subcutaneous nodules and the differentiation of rheumatoid arthritis from rheumatic fever. Semin Arthritis Rheum 13:305–321. https://doi.org/10.1016/0049-0172(84)90011-8
Moore CP, Willkens RF (1977) The subcutaneous nodule: its significance in the diagnosis of rheumatic disease. Semin Arthritis Rheum 7:63–79. https://doi.org/10.1016/s0049-0172(77)80005-x
Jiménez-Gallo D, Ossorio-García L, Linares-Barrios M (2015) Calcinosis cutis and calciphylaxis. Actas Dermosifiliogr 106:785–794. https://doi.org/10.1016/j.ad.2015.09.001
Reiter N, El-Shabrawi L, Leinweber B, Berghold A, Aberer E (2011) Calcinosis cutis: part I. Diagnostic pathway. J Am Acad Dermatol 65:1–12; quiz 13-4. https://doi.org/10.1016/j.jaad.2010.08.038
Elahmar H, Feldman BM (2022) Johnson SR (2022) Management of calcinosis cutis in rheumatic diseases. J Rheumatol 49:980–989. https://doi.org/10.3899/jrheum.211393
Figus FA, Piga M, Azzolin I, McConnell R, Iagnocco A (2021) Rheumatoid arthritis: extra-articular manifestations and comorbidities. Autoimmun Rev 20:102776. https://doi.org/10.1016/j.autrev.2021.102776
Olaru L, Soong L, Dhillon S, Yacyshyn E (2017) Coexistent rheumatoid arthritis and gout: a case series and review of the literature. Clin Rheumatol 36:2835–2838. https://doi.org/10.1007/s10067-017-3856-6
Strader KW, Agudelo CA (1986) Coexistence of rheumatoid nodulosis and gout. J Rheumatol 13:818–820
Zielaskowski LA, Kruljac SJ, DiStazio JJ, Bastacky S (2000) Multiple neuromas coexisting with rheumatoid synovitis and a rheumatoid nodule. J Am Podiatr Med Assoc 90:252–255. https://doi.org/10.7547/87507315-90-5-252
Yang K, Reddy K, Chebib I, Hammond R, Lu JQ (2021) Calcifying pseudoneoplasm of the neuraxis: from pathogenesis to diagnostic and therapeutic considerations. World Neurosurg 148:165–176. https://doi.org/10.1016/j.wneu.2021.01.076
Hornick JL, Patel RM (2022) Epithelioid sarcoma. In: WHO Classification of Tumours Editorial Board. WHO classification of tumours of soft tissue and bone, 5th edn. IARC Press, Lyon, France
Rosen Y (2022) Pathology of granulomatous pulmonary diseases. Arch Pathol Lab Med 146:233–251. https://doi.org/10.5858/arpa.2020-0543-RA
Sibbald C, Reid S, Alavi A (2015) Necrobiosis lipoidica. Dermatol Clin 33:343–360. https://doi.org/10.1016/j.det.2015.03.003
Chhana A, Dalbeth N (2015) The gouty tophus: a review. Curr Rheumatol Rep 17:19. https://doi.org/10.1007/s11926-014-0492-x
Author information
Authors and Affiliations
Contributions
FF, JM, and JQL contributed to the conception and design of the study, as well as the collection of the data. All authors contributed to the writing, critical review, revision, and approval of the manuscript. The authors meet the criteria for authorship as recommended by the International Committee of Medical Journal Editors (ICMJE).
Corresponding author
Ethics declarations
This article is based on a review of published literature and complies with the Institutional Ethical Standards.
Disclosures
None
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Fareez, F., Moodley, J., Popovic, S. et al. Rheumatoid nodules: a narrative review of histopathological progression and diagnostic consideration. Clin Rheumatol 42, 1753–1765 (2023). https://doi.org/10.1007/s10067-023-06589-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10067-023-06589-6