Abstract
Objective
To evaluate the performance of the 2019 European League Against Rheumatism/American College of Rheumatology (EULAR/ACR-2019) classification criteria for systemic lupus erythematosus (SLE) compared with the ACR-1997 and Systemic Lupus International Collaborating Clinics (SLICC) 2012 criteria in childhood-onset SLE (cSLE) and adult-onset SLE (aSLE) patients.
Methods
We conducted a retrospective study of SLE patients (221 children and 221 adults) and controls (214 children and 214 adults) with defined rheumatic diseases to establish each ACR-1997, SLICC-2012, and EULAR/ACR-2019 criterion fulfilled. Demographic, clinical, and laboratory features were evaluated through chart review.
Results
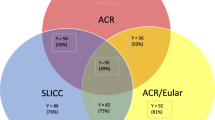
For cSLE, sensitivities of ACR-1997, SLICC-2012, and EULAR/ACR-2019 criteria were 63.3%, 94.6%, and 98.2%, with specificities 99.5%, 98.6%, and 93.5%, respectively. For aSLE, sensitivities of ACR-1997, SLICC-2012, and EULAR/ACR-2019 criteria were 72.9%, 96.8%, and 99.1%, with specificities 97.2%, 92.5%, and 90.2%, respectively. When including only ANA positive patients, receiver operating characteristics analysis demonstrated that the cutoff value for EULAR/ACR-2019 criteria in cSLE and aSLE patients was 13 (sensitivity, 92.2%; specificity, 93.1%) and 10 (sensitivity, 99.1%; specificity, 85.1%), respectively. Twelve cSLE patients and seven aSLE patients only met the EULAR/ACR-2019 criteria, among whom eleven and four cases had single organ involvement, respectively.
Conclusion
The EULAR/ACR-2019 criteria showed similar sensitivity to cSLE and aSLE patients and was more sensitive than ACR-1997 and SLICC-2012 criteria, allowing earlier recognition of patients with single or major organ involvement. The adoption of a EULAR/ACR total score ≥ 13 in this study, instead of the initially proposed ≥ 10 points, could further improve the diagnostic performance of the EULAR/ACR-2019 criteria in cSLE.
Key Points • Sensitivity of the EULAR/ACR-2019 criteria was high in both cSLE and aSLE patients. • The EULAR/ACR-2019 criteria allowed earlier recognition of patients with single or major organ damage. • The adoption of a EULAR/ACR total score ≥13 could further improve the diagnostic performance of the EULAR/ACR-2019 criteria in cSLE. |




Similar content being viewed by others
Data availability
The data availability underlying this article will be shared on reasonable request to the corresponding author.
Change history
06 August 2022
A Correction to this paper has been published: https://doi.org/10.1007/s10067-022-06316-7
References
Livingston B, Bonner A, Pope J (2011) Differences in clinical manifestations between childhood-onset lupus and adult-onset lupus: a meta-analysis. Lupus 20(13):1345–1355. https://doi.org/10.1177/0961203311416694
Tan EM, Cohen AS, Fries JF et al (1982) The 1982 revised criteria for the classification of systemic lupus erythematosus. Arthritis Rheum 25(11):1271–1277. https://doi.org/10.1002/art.1780251101
Hochberg MC (1997) Updating the American College of Rheumatology revised criteria for the classification of systemic lupus erythematosus. Arthritis Rheum 40(9):1725. https://doi.org/10.1002/art.1780400928
Petri M, Orbai AM, Alarcón GS et al (2012) Derivation and validation of the Systemic Lupus International Collaborating Clinics classification criteria for systemic lupus erythematosus. Arthritis Rheum 64(8):2677–2686. https://doi.org/10.1002/art.34473
Hartman EAR, van Royen-Kerkhof A, Jacobs JWG et al (2018) Performance of the 2012 Systemic Lupus International Collaborating Clinics classification criteria versus the 1997 American College of Rheumatology classification criteria in adult and juvenile systemic lupus erythematosus. A systematic review and meta-analysis. Autoimmun Rev 17(3):316–322. https://doi.org/10.1016/j.autrev.2018.01.007
Fonseca AR, Gaspar-Elsas MI, Land MG, de Oliveira SK (2015) Comparison between three systems of classification criteria in juvenile systemic lupus erythematous. Rheumatology (Oxford) 54(2):241–247. https://doi.org/10.1093/rheumatology/keu278
Fonseca AR, Gaspar-Elsas MIC, Land M et al (2014) Performance of the new SLICC classification criteria in juvenile systemic lupus erythematosus, in two observation periods: a Brazilian study. Pediatr Rheumatol 12(1):1–2. https://doi.org/10.1186/1546-0096-12-S1-P318
Lythgoe H, Morgan T, Heaf E et al (2017) Evaluation of the ACR and SLICC classification criteria in juvenile-onset systemic lupus erythematosus: a longitudinal analysis. Lupus 26(12):1285–1290. https://doi.org/10.1177/0961203317700484
Aringer M, Costenbader K, Daikh D et al (2019) 2019 European League Against Rheumatism/American College of Rheumatology Classification Criteria for Systemic Lupus Erythematosus. Arthritis Rheumatol 71(9):1400–1412. https://doi.org/10.1002/art.40930
Batu ED, Akca UK, Ksaarslan AP et al (2021) The performances of the ACR 1997, SLICC 2012, and EULAR/ACR 2019 classification criteria in pediatric systemic lupus erythematosus. J Rheumatol 48(6):907–914. https://doi.org/10.3899/jrheum.200871
Aljaberi N, Nguyen K, Strahle C et al (2021) Performance of the new 2019 European League Against Rheumatism/American College of Rheumatology classification criteria for systemic lupus erythematosus in children and young adults. Arthritis Care Res (Hoboken) 73(4):580–585. https://doi.org/10.1002/acr.24430
Ma M, Hui-Yuen JS, Cerise JE et al (2020) Validation of the 2019 European League Against Rheumatism/American College of Rheumatology criteria compared to the 1997 American College of Rheumatology Criteria and the 2012 Systemic Lupus International Collaborating Clinics Criteria in Pediatric Systemic Lupus Erythematosus. Arthritis Care Res (Hoboken) 72(11):1597–1601. https://doi.org/10.1002/acr.24057
Rodrigues Fonseca A, Felix Rodrigues MC, Sztajnbok FR et al (2019) Comparison among ACR1997, SLICC and the new EULAR/ACR classification criteria in childhood-onset systemic lupus erythematosus. Adv Rheumatol 59(1):20. https://doi.org/10.1186/s42358-019-0062-z
Smith EMD, Rasul S, Ciurtin C et al (2021) Limited sensitivity and specificity of ACR/EULAR-2019 classification criteria for SLE in JSLE? - observations from the UK JSLE Cohort Study. Rheumatology (Oxford). https://doi.org/10.1093/rheumatology/keab210
Levinsky Y, Broide M, Kagan S et al (2021) Performance of 2019 EULAR/ACR classification criteria for systemic lupus erythematosus in a pediatric population - a multicenter study. Rheumatology (Oxford). https://doi.org/10.1093/rheumatology/keab140
Gladman DD, Ibañez D, Urowitz MB (2002) Systemic lupus erythematosus disease activity index 2000. J Rheumatol 29(2):288–291
Dahlström Ö, Sjöwall C (2019) The diagnostic accuracies of the 2012 SLICC criteria and the proposed EULAR/ACR criteria for systemic lupus erythematosus classification are comparable. Lupus 28(6):778–782. https://doi.org/10.1177/0961203319846388
Suda M, Kishimoto M, Ohde S, Okada M (2020) Validation of the 2019 ACR/EULAR classification criteria of systemic lupus erythematosus in 100 Japanese patients: a real-world setting analysis. Clin Rheumatol 39(6):1823–1827. https://doi.org/10.1007/s10067-019-04848-z
Nashi RA, Shmerling RH (2021) Antinuclear antibody testing for the diagnosis of systemic lupus erythematosus. Med Clin North Am 105(2):387–396. https://doi.org/10.1016/j.mcna.2020.10.003
Leuchten N, Hoyer A, Brinks R et al (2018) Performance of antinuclear antibodies for classifying systemic lupus erythematosus: a systematic literature review and meta-regression of diagnostic data. Arthritis Care Res (Hoboken) 70(3):428–438. https://doi.org/10.1002/acr.23292
Radin M, Schreiber K, Cecchi I et al (2021) Impact of the new 2019 EULAR/ACR classification criteria for systemic lupus erythematosus in a multicenter cohort study of 133 women with undifferentiated connective tissue disease. Arthritis Care Res (Hoboken) 73(12):1804–1808. https://doi.org/10.1002/acr.24391
Drehmel KR, Erickson AR, England BR et al (2021) Applying SLICC and ACR/EULAR systemic lupus erythematosus classification criteria in a cohort of patients with undifferentiated connective tissue disease. Lupus 30(2):280–284. https://doi.org/10.1177/0961203320976939
Oglesby A, Korves C, Laliberté F et al (2014) Impact of early versus late systemic lupus erythematosus diagnosis on clinical and economic outcomes. Appl Health Econ Health Policy 12(2):179–190. https://doi.org/10.1007/s40258-014-0085-x
Adamichou C, Nikolopoulos D, Genitsaridi I et al (2020) In an early SLE cohort the ACR-1997, SLICC-2012 and EULAR/ACR-2019 criteria classify non-overlapping groups of patients: use of all three criteria ensures optimal capture for clinical studies while their modification earlier classification and treatment. Ann Rheum Dis 79(2):232–241. https://doi.org/10.1136/annrheumdis-2019-216155
Funding
This work was supported by the Youth Program of National Natural Science Foundation of China [82001709].
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval
The protocol of this study was approved by the Ethics Committee of Renji Hospital, Shanghai Jiao Tong University, School of Medicine.
Informed consents
Informed consents were obtained from all parents/patients before inclusion in the study.
Disclosures
None.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The original online version of this article was revised: The placement of data in Table 1 has been corrected.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Cheng, S., Ding, H., Xue, H. et al. Evaluation of the 2019 EULAR/ACR classification criteria for systemic lupus erythematosus in children and adults. Clin Rheumatol 41, 2995–3003 (2022). https://doi.org/10.1007/s10067-022-06293-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10067-022-06293-x