Abstract
Objective
The objective of this study was to describe the clinical and laboratory manifestations, triggers factors, treatment, and outcome of MAS complicating SLE.
Methods
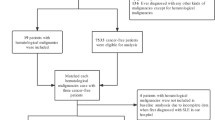
We retrospectively analyzed the medical records of adult patients with SLE for a period of 8 years (2009–2016) and identified patients who had developed MAS. We conducted statistical analysis to identify factors associated with MAS.
Results
Among 208 consecutive lupus patients, 20 patients (19 women) were identified having MAS. The mean age of patients was 35.4 ± 10 years. MAS revealed lupus in 7 patients. In the others, the delay between diagnosis of SLE and MAS was 33,3 months. All cases required hospital admission, and 2 patients were admitted to the intensive care unit. An anemia (hemoglobin < 10 g/dL) was found in all patients. A thrombopenia was observed in 19 (95%) cases. Hypertriglyceridemia and hyperferritinemia were present in all patients. All patients had anti-nuclear antibodies and anti-double-stranded DNA antibodies. Bone marrow aspiration showed hemophagocytosis in 15 (94%) cases. The mean SLEDAI was 20.95 corresponding to an SLE of a very high activity. The mean H-Score was 233.85. MAS was associated with a lupus flare in 13 patients. Documented bacterial infections, viral infections, and a breast cancer were respectively diagnosed in 4, 3, and 1 cases respectively. The corticosteroids were administered in all patients. Intravenous cyclophosphamide was used together with corticosteroids in 6 patients, mycophenolate mofetil in 2 cases and azathioprine in 2 cases. Intravenous immunoglobulin was given in 4 cases, etoposide in one case and rituximab was used as the third line treatment in one patient. All infectious episodes were also treated by broad spectrum antibiotics. All patients had a good outcome without any mortality at the management, with a mean follow-up of 24 months. The clinical parameters significantly associated with MAS were fever (p = 0,001), splenomegaly (p < 0.0001), lymphadenopathy (p < 0.0001), oral and/or nasopharyngeal ulceration (p = 0.04), arthritis (p = 0.017), and pulmonary signs (p = 0.003). Laboratory parameters associated with MAS were anemia (p < 0.0001), thrombopenia (p < 0.0001), hyperferritinemia (p < 0.0001), hypertriglyceridemia (p < 0.0001), SLEDAI (p < 0.0001), and H-Score (p < 0.0001). Receiver operating characteristic (ROC) analysis identified optimal cutoff values of ferritin (> 695 ng/mL) and SLEDAI (> 13.5) to predict the occurrence of MAS in SLE.
Conclusion
MAS was observed in 9.62% Moroccan adult patients with SLE. SLE flare and infection were the common triggers of MAS in our study. Our study indicates that the occurrence of unexplained fever, splenomegaly, lymphadenopathy, profound cytopenia, hyperferritinemia, hypertriglyceridemia, high SLEDAI, and H-Score should raises the possibility of the diagnosis of MAS in SLE patients. Early diagnosis and urgent therapeutic management improves the overall prognosis.
Key Points • Macrophage activation syndrome (MAS) is an underdiagnosed complication of systemic lupus erythematosus (SLE). The prevalence of this complication in this study is nearly 10%. • The diagnosis of MAS represents a major challenge for clinicians, as it could mimic a SLE flare up or be confused with infections. Validated diagnostic criteria for MAS in adults secondary to SLE are urgently needed. • In this study, the H-score calculate the individual risk of adult patients having reactive MAS. The cut-off value for the H-score was 190.5 (sensitivity 96.7%, specificity 97.6%). • The prognosis of MAS with SLE is good in our study. However, in the literature MAS may be a fatal condition in SLE patients. Prospective studies are necessary to confirm these results. |



Similar content being viewed by others
References
Minoia F, Davi S, Horne A, Demirkaya E, Bovis F, Li C et al (2014) Clinical features, treatment, and outcome of macrophage activation syndrome complicating systemic juvenile idiopathic arthritis: a multinational, multicenter study of 362 patients. Arthritis Rheumatol 66(11):3160–3169. https://doi.org/10.1002/art.38802
Zhang K, Biroschak J, Glass DN, Thompson SD, Finkel T, Passo MH et al (2008) Macrophage activation syndrome in patients with systemic juvenile idiopathic arthritis is associated with MUNC13-4 polymorphisms. Arthritis Rheum 58(9):2892–2896. https://doi.org/10.1002/art.23734
Henter JI, Horne A, Arico M et al (2007) HLH-2004:´ diagnostic and therapeutic guidelines for hemophagocytic lymphohistiocytosis’. Pediatr Blood Cancer 48(2):124–131. https://doi.org/10.1002/pbc.21039
Janka GE, Lehmberg K (2014) Hemophagocytic syndromes—an update. Blood Rev 28(4):135–142. https://doi.org/10.1016/j.blre.2014.03.002
Ramos-Casals M, Brito-Zeron P, López-Guillermo A, Khamashta MA, Bosch X (2014) Adult haemophagocytic syndrome. Lancet 383(9927):1503–1516. https://doi.org/10.1016/S0140-6736(13)61048-X
Stepp SE, Dufourcq-Lagelouse R, LeDeist F et al (1999) Perforin gene defects in familial hemophagocytic lymphohistiocytosis. Science 286(5446):1957–1959. https://doi.org/10.1126/science.286.5446.1957
Fukaya S, Yasuda S, Hashimoto T et al (2008) Clinical features of haemophagocytic syndrome in patients with systemic autoimmune diseases: analysis of 30 cases. Rheumatology (Oxford) 47(11):1686–1691. https://doi.org/10.1093/rheumatology/ken342
Lehmberg K, Sprekels B, Nichols KE, Woessmann W, Muller I, Suttorp M et al (2015) Malignancy-associated haemophagocytic lymphohistiocytosis in children and adolescents. Br J Haematol 170(4):539–549. https://doi.org/10.1111/bjh.13462
Daver N, McClain K, Allen CE et al (2017) A consensus review on malignancy-associated hemophagocytic lymphohistiocytosis in adults. Cancer 123(17):3229–3240. https://doi.org/10.1002/cncr.30826
Rouphael NG, Talati NJ, Vaughan C, Cunningham K, Moreira R, Gould C (2007) Infections associated with haemophagocytic syndrome. Lancet Infect Dis 7(12):814–822. https://doi.org/10.1016/S1473-3099(07)70290-6
La Rosée P, Horne A, Hines M et al (2019) Recommendations for the management of hemophagocytic lymphohistiocytosis in adults. Blood 133(23):2465–2477. https://doi.org/10.1182/blood.2018894618
Kim JM, Kwok SK, Ju JH, Kim HY, Park SH (2012) Reactive hemophagocytic syndrome in adult Korean patients with systemic lupus erythematosus: a case-control study and literature review. J Rheumatol 39(1):86–93. https://doi.org/10.3899/jrheum.110639
QianJ YangCD (2007) Hemophagocytic syndromeasone of main manifestations in untreated systemic lupus erythematosus: two case reports and literature review. Clin Rheumatol 26(5):807–810. https://doi.org/10.1007/s10067-006-0245-y
Parodi A, Davì S, Pringe AB et al (2009) Lupus Working Group of the Paediatric Rheumatology European Society Macrophage activation syndrome in juvenile systemic lupus erythematosus: a multinational multicenter study of thirty-eight patients. Arthritis Rheum 60(11):3388–3399. https://doi.org/10.1002/art.24883
Gavand PE, Serio I, Arnaud L et al (2017) Clinical spectrum and therapeutic management of systemic lupus erythematosus-associated macrophage activation syndrome: A study of 103 episodes in 89 adult patients. Autoimmun Rev 16(7):743–749. https://doi.org/10.1016/j.autrev.2017.05.010
Dall’Ara F, Cavazzana I, Frassi M et al (2018) Macrophage activation syndrome in adult systemic lupus erythematosus: report of seven adult cases from a single Italian rheumatology center. Reumatismo 70(2):100–105. https://doi.org/10.4081/reumatismo.2018.1023
Hochberg MC (1997) Updating the American College of Rheumatology revised criteria for the classification of systemic lupus erythematosus. Arthritis Rheum 40(9):1725. https://doi.org/10.1002/art.1780400928
Petri M, Orbai AM, Alarcón GS et al (2012) Derivation and validation of the Systemic Lupus International Collaborating Clinics classification criteria for systemic lupus erythematosus. Arthritis Rheum 64:2677–2686. https://doi.org/10.1002/art.34473
Henter JI, Horne A, Arico M et al (2007) HLH-2004: diagnostic and therapeutic guidelines for hemophagocytic lymphohistiocytosis. Pediatr Blood Cancer 48(2):124–213. https://doi.org/10.1002/pbc.21039
Bombardier C, Gladman DD, Urowitz MB, Caron D, Chang CH (1992) Derivation of the SLEDAI. A disease activity index for lupus patients. The Committee on Prognosis Studies in SLE. Arthritis Rheum 35(6):630–640. https://doi.org/10.1002/art.1780350606
Lambotte O, Khellaf M, Harmouche H et al (2006) Characteristics and long-term outcome of 15 episodes of systemic lupus erythematosus-associated hemophagocytic syndrome. Medicine (Baltimore) 85(3):169–182. https://doi.org/10.1097/01.md.0000224708.62510.d1
Fardet L, Galicier L, Lambotte O et al (2014) Development and validation of a score for the diagnosis of reactive hemophagocytic syndrome (HScore). Arthritis Rheumatol 66:2613–2620. https://doi.org/10.1002/art.38690
Carter SJ, Tattersall RS, Ramanan AV (2019) Macrophage activation syndrome in adults: recent advances in pathophysiology, diagnosis and treatment. Rheumatology 58(1):5–17. https://doi.org/10.1093/rheumatology/key006
Liu AC, Yang Y, Li MT et al (2018) Macrophage activation syndrome in systemic lupus erythematosus: a multicenter, case-control study in China. Clin Rheumatol 37(1):93–100. https://doi.org/10.1007/s10067-017-3625-6
Machowicz R, Janka G, Wiktor-Jedrzejczak W (2017) Similar but not the same: Differential diagnosis of HLH and sepsis. Crit Rev Oncol Hematol 114:1–12. https://doi.org/10.1016/j.critrevonc.2017.03.023
Kumakura S, Murakawa Y (2014) Clinical characteristics and treatment outcomes of autoimmune associated hemophagocytic syndrome in adults. Arthritis Rheumatol 66:2297–2307. https://doi.org/10.1002/art.38672
Cohen EM, D’Silva K, Kreps D, Son MB, Costenbader KH (2018) Arthritis and use of hydroxychloroquine associated with a decreased risk of macrophage activation syndrome among adult patients hospitalized with systemic lupus erythematosus. Lupus 27(7):1065–1071. https://doi.org/10.1177/0961203318759428
Eberhard OK, Haubitz M, Brunkhorst FM, Kliem V, Koch KM, Brunkhorst R (1997) Usefulness of procalcitonin for differentiation between activity of systemic autoimmune disease (systemic lupus erythematosus/systemic antineutrophil cytoplasmic antibody-associated vasculitis) and invasive bacterial infection. Arthritis Rheum 40(7):1250–1256. https://doi.org/10.1002/1529-0131(199707)40:7%3c1250::AID-ART9%3e3.0.CO;2-A
Bador KM, Intan S, Hussin S, Gafor AHA (2012) Serum procalcitonin has negative predictive value for bacterial infection in active systemic lupus erythematosus. Lupus 21(11):1172–1177. https://doi.org/10.1177/0961203312450085
Quintana G, Medina YF, Rojas C, Fernandez A, Restrepo JF, Rondon F et al (2008) The use of procalcitonin determinations in evaluation of systemic lupus erythematosus. J Clin Rheumatol Pract Rep Rheum Musculoskelet Dis 14(3):138–142. https://doi.org/10.1097/RHU.0b013e3181772cca
Beça S, Rodríguez-Pintó I, Alba MA, Cervera R, Espinosa G (2015) Development and validation of a risk calculator to differentiate flares from infections in systemic lupus erythematosus patients with fever. Autoimmun Rev 14(7):586–593. https://doi.org/10.1016/j.autrev.2015.02.005
Pepys MB (2003) Hirschfield GM (2003) C-reactive protein: a critical update. J Clin Invest 111:1805–1812. https://doi.org/10.1172/JCI18921
Grom AA (2004) Natural killer cell dysfunction: a common pathway in systemic-onset juvenile rheumatoid arthritis, macrophage activation syndrome, and hemophagocytic lymphohistiocytosis? Arthritis Rheum 50:689–698. https://doi.org/10.1002/art.20198
Usami M, Shimizu M, Mizuta M, Inoue N, Irabu H, Sakumura N, Nakagishi Y, Yachie A (2019) Extensive serum biomarker analysis in patients with macrophage activation syndrome associated with systemic lupus erythematosus. Clin Immunol 208:108255. https://doi.org/10.1016/j.clim.2019.108255
Batu ED, Erden A, Seyhoğlu E et al (2017) Assessment of the H Score for reactive haemophagocytic syndrome in patients with rheumatic diseases. Scand J Rheumatol 46:44–48. https://doi.org/10.3109/03009742.2016.1167951
Ravelli A, Minoia F, Davi S et al (2016) 2016 Classification criteria for macrophage activation syndrome complicating systemic juvenile idiopathic arthritis: a European League Against Rheumatism/American College of Rheumatology/Paediatric Rheumatology International Trials Organisation Collaborative Initiative. Arthritis Rheumatol 68:566–576. https://doi.org/10.1002/art.39332
Ravelli A, Minoia F, Davi S et al (2016) 2016 Classification criteria for macrophage activation syndrome complicating systemic juvenile idiopathic arthritis: a European League Against Rheumatism/American College of Rheumatology/Paediatric Rheumatology International Trials Organisation Collaborative Initiative. Ann Rheum Dis 75:481–489. https://doi.org/10.1136/annrheumdis-2015-208982
Ahn SS, Yoo BW, Jung SM, Lee SW, Park YB, Song JJ (2017) In-hospital mortality in febrile lupus patients based on 2016 EULAR/ACR/PRINTO classification criteria for macrophage activation syndrome. Semin Arthritis Rheum 47(2):216–221. https://doi.org/10.1016/j.semarthrit.2017.02.002
Hines Melissa R, von Bahr Tatiana, Greenwood Gernot Beutel et al (2021) Consensus-based guidelines for the recognition, diagnosis, and management of hemophagocytic lymphohistiocytosis in critically ill children and adults. Crit Care Med. https://doi.org/10.1097/CCM.0000000000005361
Nakagishi Y, Shimizu M, Kasai K, Miyoshi M, Yachie A (2016) Successful therapy of macrophage activation syndrome with dexamethasone palmitate. Mod Rheumatol 26(4):617–620. https://doi.org/10.3109/14397595.2014.906053
Vilaiyuk S, Sirachainan N, Wanitkun S, Pirojsakul K, Vaewpanich J (2013) Recurrent macrophage activation syndrome as the primary manifestation in systemic lupus erythematosus and the benefit of serial ferritin measurements: a case-based review. Clin Rheumatol 3(6):899–904. https://doi.org/10.1007/s10067-013-2227-1
Gouda Wesam, Alsaqabi Faisal, Moshrif Abdelhfeez et al (2021) Macrophage activation syndrome triggered by systemic lupus erythematosus flare: successful treatment with a combination of dexamethasone sodium phosphate, intravenous immunoglobulin, and cyclosporine: a case report. J Med Case Rep 15(1):497. https://doi.org/10.1186/s13256-021-03072-1
Ueda Y, Yamashita H, Takahashi Y, Kaneko H, Kano T, Mimori A (2014) Refractory hemophagocytic syndrome in systemic lupus erythematosus successfully treated with intermittent intravenous cyclophosphamide: three case reports and literature review. Clin Rheumatol 33(2):281–286. https://doi.org/10.1007/s10067-013-2451-8
Ravelli A, Viola S, De Benedetti F et al (2001) Dramatic efficacy of cyclosporine A in macrophage activation syndrome. Clin Exp Rheumatol 19:108
Emmenegger U, Frey U, Reimers A, Fux C, Semela D, Cottagnoud P, Spaeth PJ, Neftel KA (2001) Hyperferritinemia as indicator for intravenous immunoglobulin treatment in reactive macrophage activation syndromes. Am J Hematol 68(1):4–10. https://doi.org/10.1002/ajh.1141
So MW, Koo BS, Kim YJ et al (2014) Successful rituximab treatment of refractory hemophagocytic lymphohistiocytosis and autoimmune hemolytic anemia associated with systemic lupus erythematosus. Mod Rheumatol 24:855–857. https://doi.org/10.3109/14397595.2013.874740
Bakshi J, Hassan S, D’Cruz D et al (2013) Rituximab therapy in refractory macrophage activation syndrome secondary to systemic lupus erythematosus. Lupus 22:1544–1546. https://doi.org/10.1177/0961203313504634
Ruscitti P, Cipriani P, Ciccia F et al (2017) Prognostic factors of macrophage activation syndrome, at the time of diagnosis, in adult patients affected by autoimmune disease : Analysis of 41 cases collected in 2 rheumatologic centers. Autoimmun Rev 16(1):16–21. https://doi.org/10.1016/j.autrev.2016.09.016
Ke Y, Lv C, Xuan W et al (2020) Clinical analysis of macrophage activation syndrome in adult rheumatic disease: a multicenter retrospective study. Int J Rheum Dis 00:1–9. https://doi.org/10.1111/1756-185X.13955
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship and/or publication of this article.
Author information
Authors and Affiliations
Contributions
All authors were involved in drafting or revising this article, and all authors approved the final version to be published.
Corresponding author
Ethics declarations
Disclosures
None.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Wafa, A., Hicham, H., Naoufal, R. et al. Clinical spectrum and therapeutic management of systemic lupus erythematosus-associated macrophage activation syndrome: a study of 20 Moroccan adult patients. Clin Rheumatol 41, 2021–2033 (2022). https://doi.org/10.1007/s10067-022-06055-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10067-022-06055-9