Abstract
Introduction
In 2018, a renal risk score of antineutrophil cytoplasmic antibody (ANCA)–associated glomerulonephritis (AAGN) based on estimated glomerular filtration rate (eGFR), normal glomeruli, and tubular atrophy/interstitial fibrosis (TA/IF) was proposed to predict renal outcomes. We aimed to evaluate this renal risk score in a myeloperoxidase (MPO)–ANCA predominant population in Northeast China.
Methods
We retrospectively analyzed the clinicopathologic data of 65 patients biopsy-proven from a Chinese medical center. Each patient was assessed by eGFR, normal glomeruli, and TA/IF, and the renal outcome was evaluated using the renal risk score.
Results
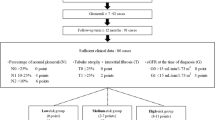
In our study, 95.4% of patients were ANCA positive (78.5% MPO-ANCA positive and 16.9% proteinase 3-ANCA positive). The average follow-up period was 14.3 months. Thirty-four patients (52.3%) reached end-stage renal disease (ESRD). Based on the renal risk score, 8 (12.3%), 31 (47.7%), and 26 (40%) patients were divided into the low-risk, medium-risk, and high-risk groups, respectively. Kaplan–Meier survival curves revealed the high-risk group had worse renal outcomes than the low-risk group (p<0.01) and the medium-risk group (p<0.01), but the renal outcome did not differ between the low-risk and medium-risk groups (p>0.017). Similar results were obtained by the competitive survival analysis. The AUC for 3-year overall ESRD predictions was 0.845. In the regression analysis, the renal risk score was a favorable predictor for the development of ESRD (HR 3.13, 95%CI 1.58–6.19, p=0.001).
Conclusion
The renal risk score is a preferred index that can predict ESRD in Chinese AAGN patients, especially in the high-risk group with worse renal outcomes.
Key Points • The eGFR and percentage of normal glomeruli were valuable predictors of renal outcome, whereas TA/IF was not. • We confirmed the renal risk score is a preferred index that can predict ESRD in Chinese AAGN patients. • Based on the renal risk score, the high-risk group had worse renal outcomes than the low-risk group and the medium-risk group. |



Similar content being viewed by others
Data availability
The data used to support the findings of this study are available from the corresponding author upon request.
Code availability
Not applicable.
Abbreviations
- ANCA:
-
Antineutrophil cytoplasmic antibody
- AAV:
-
Anti-neutrophil cytoplasmic antibody-associated vasculitis
- AAGN:
-
Antineutrophil cytoplasmic antibody-associated glomerulonephritis
- eGFR:
-
Estimated glomerular filtration rate
- TA/IF:
-
Tubular atrophy/interstitial fibrosis
- MPO:
-
Myeloperoxidase
- PR3:
-
Proteinase 3
- ESRD:
-
Reached end-stage renal disease
- AUC:
-
Area under curve
- IWGRP:
-
International working group of renal pathologists
- CHCC:
-
Chapel Hill consensus criteria
References
Geetha D, Jefferson JA (2020) ANCA-Associated Vasculitis: Core Curriculum 2020. Am J Kidney Dis 75(1):124–137
Haroun MK, Stone JH, Nair R, Racusen L, Hellmann DB, Eustace JA (2002) Correlation of percentage of normal glomeruli with renal outcome in Wegener's granulomatosis. Am J Nephrol 22(5-6):497–503
Bajema IM, Hagen EC, Hermans J, Noël LH, Waldherr R, Ferrario F, van der Woude FJ, Bruijn JA, for the EC/BCR Project for ANCA-Assay Standardisation (1999) Kidney biopsy as a predictor for renal outcome in ANCA-associated necrotizing glomerulonephritis. Kidney Int 56(5):1751–1758
de Lind van Wijngaarden RA, Hauer HA, Wolterbeek R, Jayne DR, Gaskin G, Rasmussen N et al (2006) Clinical and histologic determinants of renal outcome in ANCA-associated vasculitis: a prospective analysis of 100 patients with severe renal involvement. J Am Soc Nephrol : JASN 17(8):2264–2274
Neumann I, Kain R, Regele H, Soleiman A, Kandutsch S, Meisl FT (2005) Histological and clinical predictors of early and late renal outcome in ANCA-associated vasculitis. Nephrol Dial Transplant 20(1):96–104
Tanna A, Guarino L, Tam FW, Rodriquez-Cubillo B, Levy JB, Cairns TD et al (2015) Long-term outcome of anti-neutrophil cytoplasm antibody-associated glomerulonephritis: evaluation of the international histological classification and other prognostic factors. Nephrol Dial Transplant 30(7):1185–1192
Ellis CL, Manno RL, Havill JP, Racusen LC, Geetha D (2013) Validation of the new classification of pauci-immune glomerulonephritis in a United States cohort and its correlation with renal outcome. BMC Nephrol 14:210
Muso E, Endo T, Itabashi M, Kakita H, Iwasaki Y, Tateishi Y, Komiya T, Ihara T, Yumura W, Sugiyama T, Joh K, Suzuki K (2013) Evaluation of the newly proposed simplified histological classification in Japanese cohorts of myeloperoxidase-anti-neutrophil cytoplasmic antibody-associated glomerulonephritis in comparison with other Asian and European cohorts. Clin Exp Nephrol 17(5):659–662
Berden AE, Ferrario F, Hagen EC, Jayne DR, Jennette JC, Joh K, Neumann I, Noël LH, Pusey CD, Waldherr R, Bruijn JA, Bajema IM (2010) Histopathologic classification of ANCA-associated glomerulonephritis. J Am Soc Nephrol : JASN 21(10):1628–1636
Iwakiri T, Fujimoto S, Kitagawa K, Furuichi K, Yamahana J, Matsuura Y, Yamashita A, Uezono S, Shimao Y, Hisanaga S, Tokura T, Wada T, Kitamura K, Asada Y (2013) Validation of a newly proposed histopathological classification in Japanese patients with anti-neutrophil cytoplasmic antibody-associated glomerulonephritis. BMC Nephrol 14:125
Quintana LF, Perez NS, De Sousa E, Rodas LM, Griffiths MH, Sole M et al (2014) ANCA serotype and histopathological classification for the prediction of renal outcome in ANCA-associated glomerulonephritis.Nephrol Dial Transplant 29(9):1764–1769
Lee T, Gasim A, Derebail VK, Chung Y, McGregor JG, Lionaki S et al (2014) Predictors of treatment outcomes in ANCA-associated vasculitis with severe kidney failure. Clin J Am Soc Nephrol : CJASN 9(5):905–913
Huang S, Shen Q, Yang R, Lai H, Zhang J (2018) An evaluation of the 2010 histopathological classification of anti-neutrophil cytoplasmic antibody (ANCA)-associated glomerulonephritis: a Bayesian network meta-analysis. Int Urol Nephrol 50(10):1853–1861
Brix SR, Noriega M, Tennstedt P, Vettorazzi E, Busch M, Nitschke M, Jabs WJ, Özcan F, Wendt R, Hausberg M, Sellin L, Panzer U, Huber TB, Waldherr R, Hopfer H, Stahl RAK, Wiech T (2018) Development and validation of a renal risk score in ANCA-associated glomerulonephritis. Kidney Int 94(6):1177–1188
Hong Y, Shi P, Liu X, Yang L, Li K, Xu F, Liang S, Liu Z, Zhang H, Chen Y, Hu W (2019) Distinction between MPO-ANCA and PR3-ANCA-associated glomerulonephritis in Chinese patients: a retrospective single-center study. Clin Rheumatol 38(6):1665–1673
Pearce FA, Craven A, Merkel PA, Luqmani RA, Watts RA (2017) Global ethnic and geographic differences in the clinical presentations of anti-neutrophil cytoplasm antibody-associated vasculitis. Rheumatology (Oxford, England) 56(11):1962–1969
Jennette JC, Falk RJ, Bacon PA, Basu N, Cid MC, Ferrario F, Flores-Suarez LF, Gross WL, Guillevin L, Hagen EC, Hoffman GS, Jayne DR, Kallenberg CGM, Lamprecht P, Langford CA, Luqmani RA, Mahr AD, Matteson EL, Merkel PA, Ozen S, Pusey CD, Rasmussen N, Rees AJ, Scott DGI, Specks U, Stone JH, Takahashi K, Watts RA (2013) 2012 revised International Chapel Hill Consensus Conference Nomenclature of Vasculitides. Arthritis Rheum 65(1):1–11
Levey AS, Stevens LA, Schmid CH, Zhang YL, Castro AF 3rd, Feldman HI et al (2009) A new equation to estimate glomerular filtration rate. Ann Intern Med 150(9):604–612
Mukhtyar C, Lee R, Brown D, Carruthers D, Dasgupta B, Dubey S, Flossmann O, Hall C, Hollywood J, Jayne D, Jones R, Lanyon P, Muir A, Scott D, Young L, Luqmani RA (2009) Modification and validation of the Birmingham Vasculitis Activity Score (version 3). Ann Rheum Dis 68(12):1827–1832
Racusen LC, Solez K, Colvin RB, Bonsib SM, Castro MC, Cavallo T, Croker BP, Demetris AJ, Drachenberg CB, Fogo AB, Furness P, Gaber LW, Gibson IW, Glotz D, Goldberg JC, Grande J, Halloran PF, Hansen HE, Hartley B, Hayry PJ, Hill CM, Hoffman EO, Hunsicker LG, Lindblad AS, Marcussen N, Mihatsch MJ, Nadasdy T, Nickerson P, Olsen TS, Papadimitriou JC, Randhawa PS, Rayner DC, Roberts I, Rose S, Rush D, Salinas-Madrigal L, Salomon DR, Sund S, Taskinen E, Trpkov K, Yamaguchi Y (1999) The Banff 97 working classification of renal allograft pathology. Kidney Int 55(2):713–723
Wallace ZS, Miloslavsky EM (2020) Management of ANCA associated vasculitis. BMJ (Clinical research ed) 368:m421
Flossmann O, Berden A, de Groot K, Hagen C, Harper L, Heijl C, Höglund P, Jayne D, Luqmani R, Mahr A, Mukhtyar C, Pusey C, Rasmussen N, Stegeman C, Walsh M, Westman K, for the European Vasculitis Study Group (2011) Long-term patient survival in ANCA-associated vasculitis. Ann Rheum Dis 70(3):488–494
Villacorta J, Diaz-Crespo F, Guerrero C, Acevedo M, Cavero T, Fernandez-Juarez G (2021) Long-term validation of the renal risk score for vasculitis in a Southern European population. Clin Kidney J 14(1):220–225
Ge Y, Yang G, Yu X, Sun B, Zhang B, Yuan Y, Zeng M, Wang N, Mao H, Xing C (2021) Outcome predictors of biopsy-proven myeloperoxidase-anti-neutrophil cytoplasmic antibody-associated glomerulonephritis. Front Immunol 11:607261
Lim JH, Han MH, Kim YJ, Jeon Y, Jung HY, Choi JY, Cho JH, Kim CD, Kim YL, Lee H, Kim DK, Moon KC, Park SH (2021) Histopathologic and clinicopathologic classifications of antineutrophil cytoplasmic antibody-associated glomerulonephritis: a validation study in a Korean cohort. Kidney Res Clin Pract 40(1):77–88
Gercik O, Bilgin E, Solmaz D, Cakalagaoglu F, Saglam A, Aybi O, Kardas RC, Soypacaci Z, Kabadayi G, Yildirim T, Kurut Aysin I, Karadag O, Akar S (2020) Histopathological subgrouping versus renal risk score for the prediction of end-stage renal disease in ANCA-associated vasculitis. Ann Rheum Dis 79(5):675–676
Wu T, Shen C, Zhong Y, Ooi JD, Zhou YO, Chen JB, Meng T, Xiao Z, Lin W, Ao X, Xiao X, Zhou Q, Xiao P (2021) Differences between myeloperoxidase-antineutrophil cytoplasmic autoantibody (ANCA) and proteinase 3-ANCA associated vasculitis: A retrospective study from a single center in China. Exp Ther Med 21(6):561
Funding
This study was funded in part by grants from the National Natural Science Foundation of China (81970628), Science and Technology Development Plan Project of Jilin province (20200201488JC, 20190304042YY), and the Jilin Province Sanitation and Health Technology Innovation Project (2018J048).
Author information
Authors and Affiliations
Contributions
Xue Bai: investigation, software, data analysis, writing—original draft.
Qiaoyan Guo: revision.
Yan Lou: resources, investigation.
Ping Nie: resources, investigation.
Yuexin Zhu: data analysis.
Bing Li: pathological diagnosis, supervision, funding acquisition.
Ping Luo: pathological diagnosis, supervision, funding acquisition, resources.
Corresponding authors
Ethics declarations
Statement of ethics
The protocol was approved by the Ethics Committee of The Second Hospital of Jilin University (No. 2020-100), and the research was conducted ethically in accordance with the World Medical Association Declaration of Helsinki.
Disclosures
None.
Consent to participate
Informed consent was obtained from all the participants.
Consent for publication
Written informed consent for publication was obtained from all the participants.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Supplementary Fig. S1
Organ system involvement beyond the kidney in different ANCA subtypes (TIF 950 kb)
Supplementary Fig. S2
Comparison of cumulative incidence of ESRD or Death of different renal risk score group. ESRD, low-risk: low-risk group progress to ESRD; ESRD, medium-risk: medium-risk group progress to ESRD; ESRD, high-risk: high-risk group progress to ESRD; Death, low-risk: low-risk group progress to death; Death, medium-risk: medium-risk group progress to death; Death, high-risk: high-risk group progress to death. CIF: cumulative incidence function. (TIF 5541 kb)
Rights and permissions
About this article
Cite this article
Bai, X., Guo, Q., Lou, Y. et al. Validation of the renal risk score for antineutrophil cytoplasmic antibody-associated glomerulonephritis in a Chinese population. Clin Rheumatol 40, 5009–5017 (2021). https://doi.org/10.1007/s10067-021-05862-w
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10067-021-05862-w