Abstract
Objective
To assess short- and long-term outcomes and predictors of juvenile idiopathic arthritis (JIA) children treated with contemporary therapy and compare those with reports elsewhere.
Methods
Children with JIA were recruited from our web-based REgistry for Childhood Onset Rheumatic Diseases (RECORD) from 1997 to 2015. Disease status was defined using modified Wallace criteria. Nonparametric statistics described the data. Kaplan-Meier survival and logistic regression analyses were used to estimate probabilities and to determine predictors of outcomes.
Results
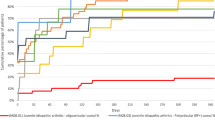
A total of 251 children with JIA (62% males, 71% Chinese) were included. Median follow-up duration was 2.9 years (range 0.1–17.5). Short-term clinical inactive disease (CID) was attained in 37% with 62% systemic JIA (sJIA) and 47% persistent oligoarthritis (oJIA). Methotrexate (OR 0.34) decreased but sJIA (OR 3.25) increased chance of attaining CID at 6 months. Overall, 79% of patients achieved CID within 2 years (sJIA 92%, the highest, and RF+ polyarthritis 50%, the lowest probability). Biologics were associated with CID attainment (OR 2.73). One-half of patients flare after CID, median 1.2 years (IQR 0.71–1.97). Late CID achievement predicted flare (OR 2.15). Only 15% had clinical remission off medication (none RF+ polyarthritis and 7% ERA). Only 13% of patients had active arthritis as young adults and 22% had active arthritis at last visit.
Conclusion
Despite high proportion of JIA patients attaining CID, only one-fourth could stop all medications for at least 1 year. Persistent oJIA patients were less likely to achieve clinical remission on medication and ERA patients had the least chance stopping medications. One-tenth of patients had active arthritis as young adults.
Key Points • Majority of Asian children with JIA attained inactive disease within 2 years after diagnosis. • Outcome predictors were different from reports from the West. • Despite high inactive disease numbers, only one-in-four JIA patients discontinued treatment within 5 years. |

Similar content being viewed by others
References
Chhabra A, Robinson C, Houghton K, Cabral DA, Morishita K, Tucker LB, Petty RE, Larché M, Batthish M, Guzman J (2020) Long-term outcomes and disease course of children with juvenile idiopathic arthritis in the ReACCh-Out cohort: a two-centre experience. Rheumatology May 13:keaa118. https://doi.org/10.1093/rheumatology/keaa118
Gare BA, Fasth A (1995) The natural history of juvenile chronic arthritis: a population based cohort study. II. Outcome. J Rheumatol 22(2):308–319
Oen K (2002) Long-term outcomes and predictors of outcomes for patients with juvenile idiopathic arthritis. Best practice & research. Clin Rheumatol 16(3):347–360
Ringold S, Angeles-Han ST, Beukelman T, Lovell D, Cuello CA, Becker ML, Colbert RA, Feldman BM, Ferguson PJ, Gewanter H, Guzman J, Horonjeff J, Nigrovic PA, Ombrello MJ, Passo MH, Stoll ML, Rabinovich CE, Schneider R, Halyabar O, Hays K, Shah AA, Sullivan N, Szymanski AM, Turgunbaev M, Turner A, Reston J (2019) 2019 American College of Rheumatology/Arthritis Foundation guideline for the treatment of juvenile idiopathic arthritis: therapeutic approaches for non-systemic polyarthritis, sacroiliitis, and enthesitis. Arthritis Rheum 71(6):846–863
Ringold S, Weiss PF, Beukelman T et al (2013) 2013 update of the 2011 American College of Rheumatology recommendations for the treatment of juvenile idiopathic arthritis: recommendations for the medical therapy of children with systemic juvenile idiopathic arthritis and tuberculosis screening among children receiving biologic medications. Arthritis Rheum 65(10):2499–2512
Ruperto N, Martini A (2018) Current and future perspectives in the management of juvenile idiopathic arthritis. Lancet Child Adolesc Health 2(5):360–370
Ruperto N, Ravelli A, Levinson JE, Shear ES, Murray K, Link Tague B, Martini A, Glass DN, Giannini EH (1997) Long-term health outcomes and quality of life in American and Italian inception cohorts of patients with juvenile rheumatoid arthritis. II. Early predictors of outcome. J Rheumatol 24(5):952–958
Oen K, Malleson PN, Cabral DA, Rosenberg AM, Petty RE, Cheang M (2002) Disease course and outcome of juvenile rheumatoid arthritis in a multicenter cohort. J Rheumatol 29(9):1989–1999
Shoop-Worrall SJW, Kearsley-Fleet L, Thomson W, Verstappen SMM, Hyrich KL (2017) How common is remission in juvenile idiopathic arthritis: a systematic review. Semin Arthritis Rheum 47(3):331–337
Shoop-Worrall SJW, Wu Q, Davies R, Hyrich KL, Wedderburn LR (2019) Predicting disease outcomes in juvenile idiopathic arthritis: challenges, evidence, and new directions. Lancet Child Adolesc Health 3(10):725–733
van Dijkhuizen EH, Wulffraat NM (2015) Early predictors of prognosis in juvenile idiopathic arthritis: a systematic literature review. Ann Rheum Dis 74(11):1996–2005
Guzman J, Henrey A, Loughin T, Berard RA, Shiff NJ, Jurencak R, Benseler SM, Tucker LB (2017) Predicting which children with juvenile idiopathic arthritis will have a severe disease course: results from the ReACCh-Out cohort. J Rheumatol 44(2):230–240
Guzman J, Henrey A, Loughin T, Berard RA, Shiff NJ, Jurencak R, Huber AM, Oen K, Gerhold K, Feldman BM, Scuccimarri R, Houghton K, Chédeville G, Morishita K, Lang B, Dancey P, Rosenberg AM, Barsalou J, Bruns A, Watanabe Duffy K, Benseler S, Duffy CM, Tucker LB, ReACCh-Out Investigators (2019) Predicting which children with juvenile idiopathic arthritis will not attain early remission with conventional treatment: results from the ReACCh-Out cohort. J Rheumatol 46(6):628–635
Rypdal V, Arnstad ED, Aalto K et al (2018) Predicting unfavorable long-term outcome in juvenile idiopathic arthritis: results from the Nordic cohort study. Arthritis Res Ther 20(1):91
Henrey A, Rypdal V, Rypdal M et al (2020) Validation of prediction models of severe disease course and non-achievement of remission in juvenile idiopathic arthritis part 2: results of the Nordic model in the Canadian cohort. Arthritis Res Ther 22(1):10
Rypdal V, Guzman J, Henrey A et al (2019) Validation of prediction models of severe disease course and non-achievement of remission in juvenile idiopathic arthritis: part 1-results of the Canadian model in the Nordic cohort. Arthritis Res Ther 21(1):270
Arkachaisri T, Tang SP, Daengsuwan T, Phongsamart G, Vilaiyuk S, Charuvanij S, Hoh SF, Tan JH, Das L, Ang E, Lim W, Chan YH, Bernal CB, Asia Pacific Pediatric Rheumatology Education and Research Network (2017) Paediatric rheumatology clinic population in Southeast Asia: are we different? Rheumatology 56(3):390–398
Dave M, Rankin J, Pearce M, Foster HE (2020) Global prevalence estimates of three chronic musculoskeletal conditions: club foot, juvenile idiopathic arthritis and juvenile systemic lupus erythematosus. Pediatr Rheumatol Online J 18(1):49
Shen CC, Yeh KW, Ou LS, Yao TC, Chen LC, Huang JL (2013) Clinical features of children with juvenile idiopathic arthritis using the ILAR classification criteria: a community-based cohort study in Taiwan. J Microbiol Immunol Infect 46(4):288–294
Vilaiyuk S, Soponkanaporn S, Jaovisidha S, Benjaponpitak S, Manuyakorn W (2016) A retrospective study on 158 Thai patients with juvenile idiopathic arthritis followed in a single center over a 15-year period. Int J Rheum Dis 19(12):1342–1350
Consolaro A, Giancane G, Alongi A, van Dijkhuizen E, Aggarwal A, al-Mayouf SM, Bovis F, de Inocencio J, Demirkaya E, Flato B, Foell D, Garay SM, Lazăr C, Lovell DJ, Montobbio C, Miettunen P, Mihaylova D, Nielsen S, Orban I, Rumba-Rozenfelde I, Magalhães CS, Shafaie N, Susic G, Trachana M, Wulffraat N, Pistorio A, Martini A, Ruperto N, Ravelli A, Paediatric Rheumatology International Trials Organisation (2019) Phenotypic variability and disparities in treatment and outcomes of childhood arthritis throughout the world: an observational cohort study. Lancet Child Adolesc Health 3(4):255–263
Tanya M, Teh KL, Das L, Hoh SF, Gao X, Arkachaisri T (2020) Juvenile idiopathic arthritis in Southeast Asia: the Singapore experience over two decades. Clin Rheumatol 39:3455–3464
Petty RE, Southwood TR, Manners P et al (2004) International League of Associations for Rheumatology classification of juvenile idiopathic arthritis: second revision, Edmonton, 2001. J Rheumatol 31(2):390–392
Lambert RG, Bakker PA, van der Heijde D et al (2016) Defining active sacroiliitis on MRI for classification of axial spondyloarthritis: update by the ASAS MRI working group. Ann Rheum Dis 75(11):1958–1963
Wallace CA, Giannini EH, Huang B, Itert L, Ruperto N, Childhood Arthritis Rheumatology Research Alliance (CARRA), Pediatric Rheumatology Collaborative Study Group (PRCSG), Paediatric Rheumatology International Trials Organisation (PRINTO) (2011) American College of Rheumatology provisional criteria for defining clinical inactive disease in select categories of juvenile idiopathic arthritis. Arthritis Care Res 63(7):929–936
Wallace CA, Ruperto N, Giannini E, Childhood Arthritis and Rheumatology Research Alliance, Pediatric Rheumatology International Trials Organization, Pediatric Rheumatology Collaborative Study Group (2004) Preliminary criteria for clinical remission for select categories of juvenile idiopathic arthritis. J Rheumatol 31(11):2290–2294
Braun J, van den Berg R, Baraliakos X, Boehm H, Burgos-Vargas R, Collantes-Estevez E, Dagfinrud H, Dijkmans B, Dougados M, Emery P, Geher P, Hammoudeh M, Inman RD, Jongkees M, Khan MA, Kiltz U, Kvien TK, Leirisalo-Repo M, Maksymowych WP, Olivieri I, Pavelka K, Sieper J, Stanislawska-Biernat E, Wendling D, Özgocmen S, van Drogen C, van Royen B, van der Heijde D (2011) 2010 update of the ASAS/EULAR recommendations for the management of ankylosing spondylitis. Ann Rheum Dis 70(6):896–904
Mandl P, Navarro-Compan V, Terslev L et al (2015) EULAR recommendations for the use of imaging in the diagnosis and management of spondyloarthritis in clinical practice. Ann Rheum Dis 74(7):1327–1339
Weiss PF, Xiao R, Biko DM, Chauvin NA (2016) Assessment of sacroiliitis at diagnosis of juvenile spondyloarthritis by radiography, magnetic resonance imaging, and clinical examination. Arthritis Care Res 68(2):187–194
Oen K, Tucker L, Huber AM, Miettunen P, Scuccimarri R, Campillo S, Cabral DA, Feldman BM, Tse S, Chédeville G, Spiegel L, Schneider R, Lang B, Ellsworth J, Ramsey S, Dancey P, Silverman E, Chetaille AL, Cameron B, Johnson N, Dorval J, Petty RE, Duffy KW, Boire G, Haddad E, Houghton K, Saint-Cyr C, Turvey SE, Benseler S, Cheang M, Yeung RSM, Duffy CM (2009) Predictors of early inactive disease in a juvenile idiopathic arthritis cohort: results of a Canadian multicenter, prospective inception cohort study. Arthritis Rheum 61(8):1077–1086
Ringold S, Seidel KD, Koepsell TD, Wallace CA (2009) Inactive disease in polyarticular juvenile idiopathic arthritis: current patterns and associations. Rheumatology 48(8):972–977
Anink J, Dolman KM, Merlijn van den Berg J, van Veenendaal M, Kuijpers TW, van Rossum MA (2012) Two-year outcome of juvenile idiopathic arthritis in current daily practice: what can we tell our patients? Clin Exp Rheumatol 30(6):972–978
Fernandes TA, Corrente JE, Magalhaes CS (2007) Remission status follow-up in children with juvenile idiopathic arthritis. J Pediatr 83(2):141–148
Guzman J, Oen K, Tucker LB, Huber AM, Shiff N, Boire G, Scuccimarri R, Berard R, Tse SML, Morishita K, Stringer E, Johnson N, Levy DM, Duffy KW, Cabral DA, Rosenberg AM, Larché M, Dancey P, Petty RE, Laxer RM, Silverman E, Miettunen P, Chetaille AL, Haddad E, Houghton K, Spiegel L, Turvey SE, Schmeling H, Lang B, Ellsworth J, Ramsey S, Bruns A, Campillo S, Benseler S, Chédeville G, Schneider R, Yeung R, Duffy CM (2015) The outcomes of juvenile idiopathic arthritis in children managed with contemporary treatments: results from the ReACCh-Out cohort. Ann Rheum Dis 74(10):1854–1860
Wallace CA, Huang B, Bandeira M, Ravelli A, Giannini EH (2005) Patterns of clinical remission in select categories of juvenile idiopathic arthritis. Arthritis Rheum 52(11):3554–3562
Sengler C, Klotsche J, Niewerth M, Liedmann I, Föll D, Heiligenhaus A, Ganser G, Horneff G, Haas JP, Minden K (2015) The majority of newly diagnosed patients with juvenile idiopathic arthritis reach an inactive disease state within the first year of specialised care: data from a German inception cohort. RMD Open 1(1):e000074
Wallace CA, Giannini EH, Spalding SJ, Hashkes PJ, O’Neil KM, Zeft AS, Szer IS, Ringold S, Brunner HI, Schanberg LE, Sundel RP, Milojevic DS, Punaro MG, Chira P, Gottlieb BS, Higgins GC, Ilowite NT, Kimura Y, Johnson A, Huang B, Lovell DJ, Childhood Arthritis and Rheumatology Research Alliance (CARRA) (2014) Clinically inactive disease in a cohort of children with new-onset polyarticular juvenile idiopathic arthritis treated with early aggressive therapy: time to achievement, total duration, and predictors. J Rheumatol 41(6):1163–1170
Guzman J, Oen K, Huber AM, Watanabe Duffy K, Boire G, Shiff N, Berard RA, Levy DM, Stringer E, Scuccimarri R, Morishita K, Johnson N, Cabral DA, Rosenberg AM, Larché M, Dancey P, Petty RE, Laxer RM, Silverman E, Miettunen P, Chetaille AL, Haddad E, Houghton K, Spiegel L, Turvey SE, Schmeling H, Lang B, Ellsworth J, Ramsey SE, Bruns A, Roth J, Campillo S, Benseler S, Chédeville G, Schneider R, Tse SM, Bolaria R, Gross K, Feldman B, Feldman D, Cameron B, Jurencak R, Dorval J, LeBlanc C, St Cyr C, Gibbon M, Yeung RS, Duffy CM, Tucker LB, ReACCh-Out investigators (2016) The risk and nature of flares in juvenile idiopathic arthritis: results from the ReACCh-Out cohort. Ann Rheum Dis 75(6):1092–1098
Nordal E, Zak M, Aalto K, Berntson L, Fasth A, Herlin T, Lahdenne P, Nielsen S, Straume B, Rygg M, Nordic Study Group of Pediatric Rheumatology (2011) Ongoing disease activity and changing categories in a long-term Nordic cohort study of juvenile idiopathic arthritis. Arthritis Rheum 63(9):2809–2818
Foell D, Wulffraat N, Wedderburn LR et al (2010) Methotrexate withdrawal at 6 vs 12 months in juvenile idiopathic arthritis in remission: a randomized clinical trial. Jama 303(13):1266–1273
Acknowledgments
We thank our JIA children and families participating in the inception cohort and registry. Their physical and mental supports to the rheumatology team and among those JIA families in need of support throughout the past decade are much grateful and appreciated.
Funding
This work was supported by grants from the National Arthritis Foundation of Singapore and International Leagues of Associations for Rheumatology (ILAR 2011).
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Data collection and interpretation were performed by MT, KLT, LD, SFH, XG, and TA. Data analysis was done by MT and TA. The funding was granted to TA. The first draft of the manuscript was written by MT, KLT, and TA; and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Disclosures
None.
Ethics approval
The SingHealth Centralised Institutional Review Board (CIRB) approved this study and waived the need for informed consent for this database study (CIRB 2019/2274).
Disclaimer
The funding body did not play any role in design and in the collection, analysis, and interpretation of data; in the writing of the manuscript; and in the decision to submit the manuscript for publication.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
ESM 1
(DOCX 20 kb)
Rights and permissions
About this article
Cite this article
Teh, K.L., Tanya, M., Das, L. et al. Outcomes and predictors of juvenile idiopathic arthritis in Southeast Asia: a Singapore longitudinal study over a decade. Clin Rheumatol 40, 2339–2349 (2021). https://doi.org/10.1007/s10067-020-05520-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10067-020-05520-7