Abstract
Objective
To assess incidence, time-trends, and outcomes of serious infections in people with polymyalgia rheumatica (PMR) or giant cell arteritis (GCA).
Methods
We examined the 1998–2016 US National Inpatient Sample for serious infections in PMR or GCA, namely, opportunistic infections (OI), skin and soft tissue infections (SSTI), urinary tract infection (UTI), pneumonia, and sepsis/bacteremia. Multivariable-adjusted logistic regressions assessed association of the type of infection, demographics, comorbidity, and hospital characteristics with healthcare utilization and mortality.
Results
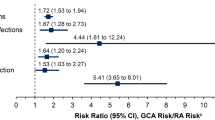
Hospitalized with serious infections, those with PMR or GCA were 2 decades older than people without PMR or GCA, and more likely to be female or white or have higher Deyo-Charlson index score or higher income. Sepsis rates in the general population, PMR, and GCA cohorts were 10.2%, 17.7%, and 18.9% in 2015–2016, respectively. Incidence rates of serious infections/100,000 NIS claims in PMR and GCA in 2015–2016 were as follows (rounded off): OI, < 1 and < 1; SSTI, 4 and 1; UTI, 4 and 1; pneumonia, 9 and 2; and sepsis, 20 and 4, respectively. Sepsis surpassed pneumonia as the most common serious infection in 2011–2012. In multivariable-adjusted analyses in the PMR cohort, sepsis, female sex, Deyo-Charlson comorbidity score ≥ 2, Medicare or Medicaid insurance, urban hospital location, and large hospital bed size were associated with significantly higher healthcare utilization and/or in-hospital mortality. Similar associations were noted in the GCA cohort.
Conclusions
Incidence of serious infections, especially sepsis, increased in both PMR and GCA cohorts over time. Interventions to improve serious infection outcomes in PMR/GCA are needed.
Key Points • PMR/GCA patients with hospitalized serious infections were 2 decades older than the general population. • Sepsis surpassed pneumonia as the commonest hospitalized serious infection in PMR/GCA in 2011–2012. • Sepsis, female sex, comorbidity, Medicare/Medicaid insurance, and urban location were associated with higher healthcare utilization and in-hospital mortality. |

Similar content being viewed by others
References
Gonzalez-Gay MA, Vazquez-Rodriguez TR, Lopez-Diaz MJ, Miranda-Filloy JA, Gonzalez-Juanatey C, Martin J, Llorca J (2009) Epidemiology of giant cell arteritis and polymyalgia rheumatica. Arthritis Rheum 61:1454–1461
Salvarani C, Cantini F, Boiardi L, Hunder GG (2002) Polymyalgia rheumatica and giant-cell arteritis. N Engl J Med 347:261–271
Raheel S, Shbeeb I, Crowson CS, Matteson EL (2017) Epidemiology of polymyalgia rheumatica 2000-2014 and examination of incidence and survival trends over 45 years: a population-based study. Arthritis Care Res (Hoboken) 69:1282–1285
Michet CJ, Matteson EL (2008) Polymyalgia rheumatica. BMJ 336:765–769
Gonzalez-Gay MA, Matteson EL, Castaneda S (2017) Polymyalgia rheumatica. Lancet 390:1700–1712
Gonzalez-Gay MA (2004) Giant cell arteritis and polymyalgia rheumatica: two different but often overlapping conditions. Semin Arthritis Rheum 33:289–293
Evans JM, Hunder GG (2000) Polymyalgia rheumatica and giant cell arteritis. Rheum Dis Clin N Am 26:493–515
de Worm S, Giot JB, Courtoy C, Gillet E, Amrane S, Huynen P, van Esbroeck M, Prudent E, Lepidi H, Million M, Moutschen M, Raoult D (2018) A case of giant cell arteritis associated with culture-proven Coxiella burnetii aortitis. Int J Infect Dis 69:50–54
Baymakova M, Demirev A, Kostadinova I, Andonova R, Popov GT, Plochev K (2018) Giant-cell arteritis without cranial manifestations presenting as fever of unknown origin: a diagnostic value of 18F-FDG PET/CT. Clin Ter 169:e274–e2e6
Buckingham EM, Foley MA, Grose C, Syed NA, Smith ME, Margolis TP, Thurtell MJ, Kardon R (2018) Identification of herpes zoster-associated temporal arteritis among cases of giant cell arteritis. Am J Ophthalmol 187:51–60
Proven A, Gabriel SE, Orces C, O'Fallon WM, Hunder GG (2003) Glucocorticoid therapy in giant cell arteritis: duration and adverse outcomes. Arthritis Rheum 49:703–708
Dixon WG, Abrahamowicz M, Beauchamp ME, Ray DW, Bernatsky S, Suissa S, Sylvestre MP (2012) Immediate and delayed impact of oral glucocorticoid therapy on risk of serious infection in older patients with rheumatoid arthritis: a nested case-control analysis. Ann Rheum Dis 71:1128–1133
Jick SS, Lieberman ES, Rahman MU, Choi HK (2006) Glucocorticoid use, other associated factors, and the risk of tuberculosis. Arthritis Rheum 55:19–26
Singh JA, Hossain A, Kotb A, Wells G (2016) Risk of serious infections with immunosuppressive drugs and glucocorticoids for lupus nephritis: a systematic review and network meta-analysis. BMC Med 14:137
Durand M, Thomas SL (2012) Incidence of infections in patients with giant cell arteritis: a cohort study. Arthritis Care Res (Hoboken) 64:581–588
Schmidt J, Smail A, Roche B, Gay P, Salle V, Pellet H, Duhaut P (2016) Incidence of severe infections and infection-related mortality during the course of giant cell arteritis: a multicenter, prospective, double-cohort study. Arthritis Rheumatol 68:1477–1482
Udayakumar PD, Chandran AK, Crowson CS, Warrington KJ, Matteson EL (2014) Hospitalized infections in giant cell arteritis: a population-based retrospective cohort study. J Rheumatol 41:2447–2451
HCUP. Overview of the National (Nationwide) Inpatient Sample (NIS). https://www.hcup-us.ahrq.gov/nisoverview.jsp. Rockville, MD: AHRQ; 2018
HCUP Databases. Healthcare Cost and Utilization Project (HCUP). Overview of the Nationwide Inpatient Sample (NIS). http://www.hcup-us.ahrq.gov/nisoverview.jsp. Last modified 8/13/18 Rockville, MD: Agency for Healthcare Research and Quality; 2018 [cited 2019 04/26/2019]
Bernatsky S, Linehan T, Hanly JG (2011) The accuracy of administrative data diagnoses of systemic autoimmune rheumatic diseases. J Rheumatol 38:1612–1616
Jinno S, Lu N, Jafarzadeh SR, Dubreuil M (2018) Trends in hospitalizations for serious infections in patients with rheumatoid arthritis in the US between 1993 and 2013. Arthritis Care Res (Hoboken) 70:652–658
Tektonidou MG, Wang Z, Dasgupta A, Ward MM. Burden of serious infections in adults with systemic lupus erythematosus: a national population-based study, 1996-2011. Arthritis Care Res (Hoboken) 2015;67:1078–1085
Schneeweiss S, Robicsek A, Scranton R, Zuckerman D, Solomon DH (2007) Veteran’s affairs hospital discharge databases coded serious bacterial infections accurately. J Clin Epidemiol 60:397–409
Grijalva CG, Chung CP, Stein CM, Gideon PS, Dyer SM, Mitchel EF Jr, Griffin MR (2008) Computerized definitions showed high positive predictive values for identifying hospitalizations for congestive heart failure and selected infections in Medicaid enrollees with rheumatoid arthritis. Pharmacoepidemiol Drug Saf 17:890–895
Patkar NM, Curtis JR, Teng GG, Allison JJ, Saag M, Martin C et al (2009) Administrative codes combined with medical records based criteria accurately identified bacterial infections among rheumatoid arthritis patients. J Clin Epidemiol 62:321–327 7 e1-7
HCUP NIS Description of Data Elements. ZIPINC_QRTL - Median household income for patient's ZIP Code (based on current year). Healthcare Cost and Utilization Project (HCUP). September 2008. Agency for Healthcare Research and Quality, Rockville, MD. www.hcup-us.ahrq.gov/db/vars/zipinc_qrtl/nisnote.jsp Bethesda, MD: Agency for Health Care Research and Quality; 2017 [cited 2017 08/19/2017]
Deyo RA, Cherkin DC, Ciol MA (1992) Adapting a clinical comorbidity index for use with ICD-9-CM administrative databases. J Clin Epidemiol 45:613–619
Medicare Eligibility: Who may enroll in Medicare. https://www.ehealthmedicare.com/about-medicare/eligibility/ Baltimore, MD: Centers for Medicare and Medicaid Services; 2017 [cited 2017 08/19/2017]
Sabesan VJ, Petersen-Fitts G, Lombardo D, Briggs D, Whaley J (2017) Medicaid payer status is linked to increased rates of complications after treatment of proximal humerus fractures. J Shoulder Elb Surg 26:948–953
Klein NC, Go CH, Cunha BA (2001) Infections associated with steroid use. Infect Dis Clin N Am 15:423–432 viii
Stuck AE, Minder CE, Frey FJ (1989) Risk of infectious complications in patients taking glucocorticosteroids. Rev Infect Dis 11:954–963
Role of the funder/supporter
The funding body did not play any role in design, in the collection, analysis, and interpretation of data; in the writing of the manuscript; and in the decision to submit the manuscript for publication.
Funding
This study is funded by the research funds from the Division of Rheumatology at the University of Alabama at Birmingham and the resources and use of facilities at the Birmingham VA Medical Center, Birmingham, Alabama, USA.
Author information
Authors and Affiliations
Contributions
Mr. Cleveland had full access to all of the data in the study and takes the responsibility for the integrity of the data and accuracy of the data analysis. He was supervised by Dr. Singh, who reviewed all results. Study concept and design: Singh. Data acquisition, analysis, and interpretation of results: Singh, Cleveland. Drafting of the manuscript: Singh. Critical revision of the manuscript for important intellectual content: Singh, Cleveland. Statistical analysis: Cleveland.
Obtained funding: Singh. Administrative, technical, or material support: Singh. Study supervision: Singh.
Corresponding author
Ethics declarations
Conflict of interest
JAS has received consultant fees from Crealta/Horizon, Medisys, Fidia, UBM LLC, Trio health, Medscape, WebMD, Clinical Care options, Clearview healthcare partners, Putnam associates, Focus forward, Navigant consulting, Spherix, Practice Point communications, the National Institutes of Health and the American College of Rheumatology. JAS owns stock options in Amarin pharmaceuticals and Viking therapeutics. JAS is on the speaker’s bureau of Simply Speaking. JAS is a member of the executive of OMERACT, an organization that develops outcome measures in rheumatology and receives arms-length funding from 12 companies. JAS serves on the FDA Arthritis Advisory Committee. JAS is the chair of the Veterans Affairs Rheumatology Field Advisory Committee. JAS is the editor and the Director of the UAB Cochrane Musculoskeletal Group Satellite Center on Network Meta-analysis. JAS previously served as a member of the following committees: member, the American College of Rheumatology’s (ACR) Annual Meeting Planning Committee (AMPC) and Quality of Care Committees, the Chair of the ACR Meet-the-Professor, Workshop and Study Group Subcommittee and the co-chair of the ACR Criteria and Response Criteria subcommittee. DC has no conflicts to declare. There are no non-financial competing interests for any of the authors.
Ethics/IRB approval and consent to participate
The University of Alabama at Birmingham’s Institutional Review Board approved this study and all investigations were conducted in conformity with ethical principles of research (UAB X120207004). The IRB waived the need for an informed consent for this database study.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(DOCX 31 kb)
Rights and permissions
About this article
Cite this article
Singh, J.A., Cleveland, J.D. Serious infections in people with polymyalgia rheumatica (PMR) or giant cell arteritis (GCA): a time-trend national US study. Clin Rheumatol 39, 3427–3438 (2020). https://doi.org/10.1007/s10067-020-05129-w
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10067-020-05129-w