Abstract
Objective
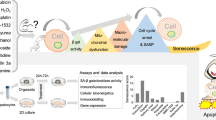
Autophagy in the immune and autoimmune diseases has been concerned more and more. We investigated the potential role of cell autophagy of B cells generating IgM in primary biliary cholangitis (PBC), and explored the relationship between the cell autophagy of hepatic stellate cells (HSCs) and hepatic fibrosis in PBC.
Methods
We examined the aggregation degree of microtubule-associated protein light chain 3II (LC3II) in B cells of PBC (n = 21), health control (HC, n = 15) and disease control (DC, n = 8, active hepatitis B). The expression level of p62/SQSTM1 (p62) in B cells was detected by flow cytometry. ELISA was adopted to detect the level of IgM in the B cell culture supernatant under the basal condition, activated condition(stimulated by pokeweed mitogen, PWM) and inhibited condition(inhibited by autophagy inhibitor, 3-methyladenine, 3-MA) respectively. We detected the expression of α-smooth muscle actin (α-SMA), the infiltration level of LC3II, transforming growth factor-β (TGF-β), platelet-derived growth factor-bb (PDGF-bb), and collagen I in the hepatic tissues of five PBC patients and two HC individuals.
Results
When B cells were stimulated and activated by PWM, the expression of p62 increased, and the mean fluorescence intensity (MFI, 2404.8 ± 689.0) of p62 in PBC was lower than that in HC (2966.8 ± 488.9,P = 0.0227). Under 3-MA treatment, the MFI expressed of p62 in B cells weakened. The reduction difference in PBC (466.4 ± 214.9) was smaller than that in HC (1166.6 ± 231.2, P = 0.0000) and DC (1184.8 ± 197.7, P = 0.0001). The level of generating IgM in the PBC group was obviously higher than that in the HC group (65.7 ± 15.4 vs. 49.5 ± 20.4 ng/ml, P = 0.0357). Before and after B cells were treated with 3-MA, the peak level of IgM did not significantly diminish in PBC and DC (65.7 ± 15.4 vs. 59.6 ± 18.7 ng/ml, P = 0.2965; 50.1 ± 17.4 vs. 48.4 ± 12.3 ng/ml, P = 0.8336). The immunohistochemical result revealed that the expression level of collagen I, α-SMA, TGF-β and PDGF-bb in PBC was higher than that in HC, but the expression of LC3II was lower. Similarly, immunofluorescence assay revealed that the fluorescence intensity of collagen I was higher but LC3II was lower in PBC than that in HC.
Conclusion
The high level autophagy of B cells from PBC patients is one important factor to synthesize and secrete IgM. Hepatic fibrosis of PBC is probably associated with the weakened autophagy of HSCs.
Key Points | |
• High-level autophagy of B cells in PBC patients is an important factor to synthesize and secrete IgM. | |
• Pro-fibrogenic cytokines in PBC influence the increase of collagen-I through HSC autophagy, and promote the occurrence and development of hepatic fibrosis. |





Similar content being viewed by others
References
Beuers U, Gershwin ME, Gish RG, Invernizzi P, Jones DEJ, Lindor K, Ma X, Mackay IR, Parés A, Tanaka A, Vierling JM, Poupon R (2015) Changing nomenclature for PBC: from ‘cirrhosis’ to ‘cholangitis’. Hepatology. 62(5):1620–1622
Carey EJ, Ali AH, Lindor KD (2015) Primary biliary cirrhosis. Lancet 386(10003):1565–1575
Pengo N, Scolari M, Oliva L, Milan E, Mainoldi F, Raimondi A, Fagioli C, Merlini A, Mariani E, Pasqualetto E, Orfanelli U, Ponzoni M, Sitia R, Casola S, Cenci S (2013) Plasma cells require autophagy for sustainable immunoglobulin production. Nat Immunol 14(3):298–305
Kimura S, Fujita N, Noda T et al (2009) Monitoring autophagy in mammalian cultured cells through the dynamics of LC3. Methods Enzymol 452:1–12
Popov Y, Schuppan D (2009) Targeting liver fibrosis: strategies for development and validation of antifibrotic therapies. Hepatology. 50(4):1294–1306
DeLeve LD (2015) Liver sinusoidal endothelial cells in hepatic fibrosis. Hepatology. 61(5):1740–1746
Hidvegi T, Ewing M, Hale P, Dippold C, Beckett C, Kemp C, Maurice N, Mukherjee A, Goldbach C, Watkins S, Michalopoulos G, Perlmutter DH (2010) An autophagy-enhancing drug promotes degradation of mutant alpha1-antitrypsin Z and reduces hepatic fibrosis. Science 329:229–232
Thoen LF, Guimaraes EL, Dolle L et al (2011) A role for autophagy during hepatic stellate cell activation. J Hepatol 55(6):1353–1360
Shuai Z, Wang J, Badamagunta M et al (2017) The fingerprint of antimitochondrial antibodies and the etiology of primary biliary cholangitis. Hepatology 65(5):1670–1682
Invernizzi P, Ransom M, Raychaudhuri S et al (2012) Classical HLA-DRB1 and DPB1 alleles account for HLA associations with primary biliary cirrhosis. Genes Immun 13:461–468
Tanaka A, Leung PSC, Gershwin ME (2018) The genetics and epigenetics of primary biliary cholangitis. [J]. Clin Liver Dis 22:443–455
Boonstra K, Beuers U, Ponsioen CY (2012) Epidemiology of primary sclerosing cholangitis and primary biliary cirrhosis: a systematic review. J Hepatol 56(5):1181–1188
Liu H, Liu Y, Wang L, Xu D, Lin B, Zhong R, Gong S, Podda M, Invernizzi P (2010) Prevalence of primary biliary cirrhosis in adults referring hospital for annual health check-up in Southern China. BMC Gastroenterol 10:100
Lindor KD, Gershwin ME, Poupon R, Kaplan M, Bergasa NV, Heathcote EJ, American Association for Study of Liver Diseases (2009) Primary biliary cirrhosis. Hepatology 50:291–308
Sakauchi F, Mori M, Zeniya M et al (2006) Antimitochondrial antibody negative primary biliary cirrhosis in Japan: utilization of clinical data when patients applied to receive public financial aid. J Epidemiol 16:30–34
Lindgren S, Eriksson S (1982) IgM in primary biliary cirrhosis. Physicochemical and complement activating properties. J Lab Clin Med 99(5):636–645
Hilscher M, Hernandez-Gea V, Friedman SL (2012) Autophagy and mesenchymal cell fibrogenesis. Biochim Biophys Acta 1831(7):972–978
Kim SI, Na HJ, Ding Y, Wang Z, Lee SJ, Choi ME (2012) Autophagy promotes intracellular degradation of type I collagen induced by transforming growth factor (TGF)-beta1. J Biol Chem 287(15):11677–11688
Melton AC, Yee HF (2007) Hepatic stellate cell protrusions couple platelet-derived growth factor-BB to chemotaxis. Hepatology 45(6):1446–1453
Seki E, De Minicis S, Osterreicher CH et al (2007) TLR4 enhances TGF-beta signaling and hepatic fibrosis. Nat Med 13(11):1324–1332
Friedman SL (2008) Mechanisms of hepatic fibrogenesis. Gastroenterology. 134(6):1655–1669
Leask A, Abraham DJ (2004) TGF-beta signaling and the fibrotic response. FASEB J 18(7):816–827
Xu Y, Yang S, Huang J, Ruan S, Zheng Z, Lin J (2012) Tgf-beta1 induces autophagy and promotes apoptosis in renal tubular epithelial cells. Int J Mol Med 29(5):781–790
Harris J (2011) Autophagy and cytokines. Cytokine. 56(2):140–144
M NSaT (2012) The role of TGF-β receptors in firosis. Open Rheumatol 6:156–162
Suzuki HI, Kiyono K, Miyazono K (2010) Regulation of autophagyby transforming growth factor-β (TGF-β) signaling. Autophagy. 6:645–647
Wang RC, Levine B (2010) Autophagy in cellular growth control. FEBS Lett 584(7):1417–1426
Pinzani MMS, Grappone C et al (1994) Expression of platelet-derived growth factor in a model of acute liver injury. Hepatology 19:701–707
Borkham-Kamphorst E, van Roeyen CR, Ostendorf T et al (2007) Pro-fibrogenic potential of PDGF-D in liver fibrosis. J Hepatol 46(6):1064–1074
Kazlauskas A (2017) PDGFs and their receptors. Gene. 614:1–7
Salabei JK, Cummins TD, Singh M, Jones SP, Bhatnagar A, Hill BG (2013) PDGF-mediated autophagy regulates vascular smooth muscle cell phenotype and resistance to oxidative stress. Biochem J 451(3):375–388
Bataller R, Brenner DA (2005) Liver fibrosis. J Clin Investig 115(2):209–218
Hernandez-Gea V, Ghiassi-Nejad Z, Rozenfeld R et al (2012) Autophagy releases lipid that promotes fibrogenesis by activated hepatic stellate cells in mice and in human tissues. Gastroenterology 142(4):938–946
Funding
This work was supported by The National Natural Science Foundation of China [No.81571594, No.81771764].
Author information
Authors and Affiliations
Contributions
Chaofeng Lian drafted the manuscript, Chaofeng Lian and Yun Zhao designed and analyzed data, Jinlei Sun and Liling Zhao revised the manuscript, Fengchun Zhang designed the study and drafted and revised the manuscript. All authors approved submission of the manuscript. We agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Corresponding author
Ethics declarations
Disclosures
None.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Lian, C., Zhao, Y., Sun, J. et al. Role of cell autophagy in the generation of IgM and hepatic fibrosis in primary biliary cholangitis. Clin Rheumatol 39, 3499–3506 (2020). https://doi.org/10.1007/s10067-020-05111-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10067-020-05111-6