Abstract
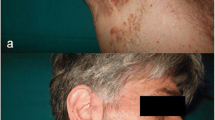
SAPHO, an acronym for synovitis, acne, pustulosis, hyperostosis and osteitis, is a heterogeneous entity with myriad presentations and features overlapping with other entities. It is a differential in patients presenting with skin and bone symptoms, either singly or in combination. Often misdiagnosed radiologically as a malignancy or infection, the diagnosis is seldom thought of. We present three cases referred to us for evaluation of findings unrelated to the presenting symptoms. After evaluation, a 99Tc bone scan was ordered, which showed the ‘bull’s head sign’ in all the three cases, confirming the diagnosis. We review the literature for SAPHO. It has a few features which point to its diagnosis and can help us to distinguish it from other seronegative arthritis. The clinician should be aware of this entity and should not hesitate to order a 99Tc bone scan. We conclude that SAPHO is not rare, but rather, it is underdiagnosed. High index of suspicion is necessary for diagnosis. A 99Tc bone scan is diagnostic and should be ordered in patients having any of the presenting features of the syndrome. We put forward the suggestion of using 99Tc bone scintigraphy to define a ‘pre-MRI’ stage of ankylosing spondylitis.



Similar content being viewed by others
References
Kahn MF, Khan MA (1994) The SAPHO syndrome. Bailliere Clin Rheumatol 8(2):333–362
Cotten Anne F-R-M, Mentre A et al (1995) SAPHO syndrome. Radiographics 15:1147–1154
Chamot AM, Benhamon CL (1987) Kahn MF et al [Acne-pustulosis-hyperostosis-osteitis syndrome: result of a national survey 85 cases]. Rev Rheum Mal Osteoartic 54:187–196
Benhamou CL, Chamot AM, Kahn MF (1988) SAPHO—a new syndrome among spondyloarthritis. Clin Exp Rheum 6(2):109–112
Schilling F. SAPHO syndrome. Orphanet encyclopedia. Available via http://orphanet.infobiogen.fr/data/patho/GB/uk-sapho.html. Accessed 9 Feb 2012
Kahn MF, Bouvier MB, Palazzo E et al (1991) Sternoclavicular pustulotic osteitis (SAPHO): 20-year interval between skin and bone lesions. J Rheumat 18:1104–1108
Sallés M, Olivé A, Perez-Andres R, Holgado S, Mateo L, Riera E, Tena X (2011) The SAPHO syndrome: a clinical and imaging study. Clin Rheumatol 30(2):245–249
Mehmat O, Kalyoncu U (2011) SAPHO syndrome may be treated effectively with combined drug regimens—a case report. IJCRI 2(1):8–11
Hayem G, Bouchad-Chabot A, Benali K et al (1999) SAPHO syndrome: a long-term follow-up study of 120 cases. Semin Arthritis Rheum 29(3):159–171
Grosjean C, Hurtado-Nedelec M, Nicaise-Roland P et al (2010) Prevalence of autoantibodies in SAPHO syndrome—a single centre study of 90 patients. J Rheum 37(3):639–643
Gunter Assmann (2012). SAPHO syndrome. In: Jose O'Daly (ed) Psoriasis—a systemic disease. Available via http://www.intechopen.com/books/psoriasis-a-systemic-disease/sapho-syndrome. Accessed 20 Apr 2012
Colina M, Govoni M, Orzincolo C, Trotta F (2009) Clinical and radiologic evolution of synovitis, acne, pustulosis, hyperostosis, and osteitis syndrome: a single center study of a cohort of 71 subjects. Arthritis Rheum 61(6):813–821
Hiwatani Y, Miwa H, Kondo T (2008) Aseptic meningitis as a rare manifestation of SAPHO syndrome. Neurology 71(20):1645–1647
Smith M, Buller A, Radford R, Laitt R, Leatherbarrow B (2005) Ocular presentation of the SAPHO syndrome. Br J Ophthalmol 89(8):1069–1070
Assman G, Simon P (2011) The SAPHO syndrome—are microbes involved? Best Pract Res Clin Rheum 25(3):423–434
Rozin AP (2009) SAPHO syndrome: is a range of pathogen-associated rheumatic diseases extended? Arthritis Res Ther 11:131
Assmann G, Kueck O, Kirchhoff T et al (2009) Efficacy of antibiotic therapy for SAPHO syndrome is lost after its discontinuation: an interventional study. Arthritis Re Ther 11:R140
Hurtado-Nedelec M, Chollet-Martin S, Nicaise-Roland P et al (2008) Characterization of the immune response in the synovitis, acne, pustulosis, hyperostosis, osteitis (SAPHO) syndrome. Rheumatol (Oxford) 47(8):1160–1167
Colina M, Pizzirani C, Khodeir M, Simonetta F, Marco B, Francesco T et al (2010) Dysregulation of P2X7–inflammasome axis in SAPHO syndrome: successful treatment with anakinra. Rheumatology 49:1416–1418
Wendling D, Prati C, Aubin F (2012) Anakinra treatment of SAPHO syndrome: short term results of an open study. Ann Rheum Dis 71:1098–1100
Golla A, Jansson A, Ramser J et al (2002) CRMO evidence for susceptibility gene on Chr 18q21.3-18q22. Eur J Hum Gen 10:217–221
Rohekar G, Inman RD (2006) Conundrums in nosology: synovitis, acne, pustolosis, hyperostosis, and osteitis syndrome and spondyloarthritis. Arthritis Rheum 55(4):665–669
Hurtado-Nedelec M, Chollet-Martin S, Chapeton D, Hugot JP, Hayem G, Gérard B (2010) Genetic susceptibility factors in a cohort of 38 patients with SAPHO syndrome: a study of PSTPIP2, NOD2, and LPIN2 genes. J Rheumatol 37(2):401–409
Vermaat M, De Schepper AM, Bloem JL (2005) Sternoclavicular hyperostosis in SAPHO syndrome. JBR-BTR 88:158–159
Sugimoto H, Tamura K, Fujii T (1998) The SAPHO syndrome: defining the radiological spectrum of diseases comprising the syndrome. Eur Radiol 8:800–806
Earwalker JWS, Cotton A (2003) SAPHO: syndrome or concept? Imaging findings. Skeletal Radiol 32:311–327
Laredo JD, Vuillemin-Bodaghi V, Boutry N, Cotten A, Parlier-Cuau C (2007) SAPHO syndrome: MR appearance of vertebral involvement. Radiology 242(3):825–831
Rodriguez QM, Tormo IC, Redal Pena MC, Castillo VL (2010) The importance of bone scintigraphy in diagnosis of SAPHO syndrome. Rev Esp Med Nucl 29(3):127–130
Bhosale P, Barron B, Lamki L (2001) The “SAPHO” syndrome: a case report of a patient with unusual bone scans findings. Clin Nucl Med 26(7):619–621
Depasquale R, Kumar N, Lalam RK (2012) SAPHO: what radiologists should know. Clin Radiology 67(3):195–206
Pichler R, Weiglein K, Schmekal B, Sfetsos K, Maschek W (2003) Bone scintigraphy using Tc-99m DPD and F18-FDG in a patient with SAPHO syndrome. Scand J Rheum 32(1):58–60
Olivieri I, Padula A, Ciancio G, Salvarani C, Niccoli L, Cantini F (2002) Successful treatment of SAPHO syndrome with infliximab: report of two cases. Ann Rheum Dis 61:375–376
Iqbal M, Koldney MS (2005) Acne fulminans with synovitis-acne-pustulosis-hyperostosis-osteitis (SAPHO) syndrome treated with infliximab. J Am Acad Derm 52(5):S118–S120, Supplement
Wagner AD, Andersen J, Jendro MC, Hulsemann JL, Zeidler H (2002) Sustained response to TNF-α blocking agents in two patients with SAPHO syndrome. Arth and Rheum 46(7):1965–1968
Massara A, Cavazzini PL, Trotta F (2006) In SAHO syndrome anti TNF-α may induce persistent amelioration of osteoarticular complaints, but may exacerbate cutaneous manifestations. Rheumatology 45(6):730–733
Disclosures
None
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kundu, B.K., Naik, A.K., Bhargava, S. et al. Diagnosing the SAPHO syndrome: a report of three cases and review of literature. Clin Rheumatol 32, 1237–1243 (2013). https://doi.org/10.1007/s10067-013-2251-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10067-013-2251-1