Abstract
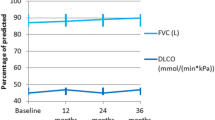
the aim of this study was to evaluate the safety and efficacy of azathioprine in the treatment of interstitial lung disease (ILD) associated with systemic sclerosis (SSc). The records of patients with SSc with ILD who were treated with azathoprine were reviewed. Patients were treated with azathioprine and low-dose prednisone if they had progressive pulmonary symptoms (deterioration in the dyspnea score) or poor or deteriorating lung function. Response was classified as improved if the FVC increased more than 10% from baseline, and stable if it remained within 10% of baseline. Serial dyspnea scores were recorded. Eleven patients were treated with azathioprine, three of whom received treatment for 6 months or less owing to adverse effects (nausea, leukopenia and pulmonary tuberculosis in one patient each). The remaining eight patients received at least 12 months’ treatment and the results suggested an improvement in the mean percent predicted FVC from a baseline value of 54.25±3.53 to 63.38±6.15 after 12 months (p=0.101). Overall, five patients improved and three remained stable. The mean dyspnea score (n=8) improved from a baseline of 1.55±0.19 to 0.50±0.19 at 12 months (p=0.011). This is the first case series of patients with SSc-associated ILD treated with azathioprine. Our results suggest that azathioprine may have a role in stabilizing lung function and improving symptoms in SSc, although this needs confirmation by a randomized controlled trial.

Similar content being viewed by others
Abbreviations
- ILD:
-
Interstitial lung disease
- SSc:
-
Systemic sclerosis
References
McCune JW, Vallance DK, Lynch JP (1994) Immuno-suppressive drug therapy. Curr Opin Rheumatol 6:262–272
DeClerck LS, Dequeker J, Francx L, Demedts M (1987) D-Penicillamine therapy and interstitial lung disease in scleroderma: a long term follow-up study. Arthritis Rheum 30:643–650
Akesson A, Wollheim FA, Thysell H et al. (1988) Visceral improvement following combined plasmapheresis and immuno-suppressive drug therapy in progressive systemic sclerosis. Scand J Rheumatol 17:313–323
Silver RM, Warrick JH, Kinsella MB, Staudt LS, Baumann MH, Strange C (1993) Cyclophosphamide and low-dose prednisolone therapy in patients with systemic sclerosis (scleroderma) with interstitial lung disease. J Rheumatol 20:834–844
Akesson A, Scheja A, Lundin A, Wollheim FA (1994) Improved pulmonary function in systemic sclerosis after treatment with cyclophosphamide. Arthritis Rheum 37:729–735
Steen VD, Lanz JK, Conte C, Owens GR, Medsger TA Jr (1994) Therapy for severe interstitial lung disease in systemic sclerosis. Arthritis Rheum 37:1290–1296
Schnabel A, Reuter M, Gross WL (1998) Intravenous pulse cyclophosphamide in the treatment of interstitial lung disease due to collagen vascular diseases. Arthritis Rheum 41:1215–1220
Varai G, Earle L, Jimenez SA, Steiner RM, Varga J (1998) A pilot study of intermittent intravenous cyclophosphamide for the treatment of systemic sclerosis associated lung disease. J Rheumatol 25:1325–1329
Davas EM, Peppas C, Maragou M, Alvanou E, Hondros D, Dantis PC (1999) Intravenous cyclophosphamide pulse therapy for treatment of lung disease associated with scleroderma. Clin Rheumatol 18:455–461
White B, Moore WC, Wigley FM et al. (2000) Cyclophosphamide is associated with pulmonary function and survival benefit in patients with scleroderma and alveolitis. Ann Intern Med 132:947–954
Fox DA, McCune J (1994) Immuno-suppressive drug therapy of systemic lupus erythematosis. Rheum Dis Clin North Am 20:265–299
Boumpas DT, Austin HA III, Vaughn EM, Yarboro CH, Klippel JH, Barlow JE (1993) Risk of sustained amenorrhoea in patients with systemic lupus erythematosis receiving intermittent pulse cyclophosphamide therapy. Ann Intern Med 119:366–369
Raghu G, DePaso WJ, Cain K et al. (1991) Azathioprine combined with prednisone in the treatment of idiopathic pulmonary fibrosis: A prospective, double blind, randomized, placebo-controlled trial. Am Rev Respir Dis 144:291–296
Zisman DA, Lynch JP 3rd, Toews GB, Kazerooni EA, Flint A, Martinez FJ (2000) Cyclophosphamide in the treatment of idiopathic pulmonary fibrosis: A prospective study in patients who failed to respond to corticosteroids. Chest 117:1619–1626
Watters LC, King TE, Schwarz MI, Waldron JA, Stanford RE,Cherniack RM (1986). A clinical, radiographic, and physiologic scoring system for the longitudinal assessment of patients with idiopathic pulmonary fibrosis. Am Rev Respir Dis 133:97–103
Mahler DA, Weinberg DH, Wells CK, Feinstein AR (1984) The measurement of dyspnea. Contents, interobserver agreement, and physiologic correlates of two new clinical indexes. Chest 85:751–758
Collard HR, King TE Jr, Bartelson BB, Vourlekis JS, Schwarz MI, Brown KK (2003) Changes in clinical and physiologic variables predict survival in idiopathic pulmonary fibrosis. Am J Respir Crit Care Med 168:538–542
Martinez TY, Pereira CA, dos Santos ML, Ciconelli RM, Guimaraes SM, Martinez JA (2000) Evaluation of the short-form 36-item questionnaire to measure health-related quality of life in patients with idiopathic pulmonary fibrosis. Chest 117:1627–1632
Mosca M, Ruiz-Irastorza G, Khamashta MA, Hughes GR (2001) Treatment of systemic lupus erythematosus. Int Immunopharmacol 1:1065–1075
Present DH, Meltzer SJ, Krumholz MP, Wolke A, Korelitz BI (1989). 6-mercaptopurine in the management of inflammatory bowel disease: short- and long-term toxicity. Ann Intern Med 111:641–649
British Thoracic Society, Standards of Care Committee. The diagnosis, assessment and treatment of diffuse parenchymal lung disease in adults, British Thoracic Society recommendations. Thorax 1999; 54: S1–S30
Acknowledgements
We wish to thank Mrs Moganamba Govender and Sister NG Mkhize for their help in collecting the data, and Dr J. Maharaj and Dr F. Bassa for reviewing the CT scans.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Dheda, K., Lalloo, U.G., Cassim, B. et al. Experience with azathioprine in systemic sclerosis associated with interstitial lung disease. Clin Rheumatol 23, 306–309 (2004). https://doi.org/10.1007/s10067-004-0906-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10067-004-0906-7