Abstract
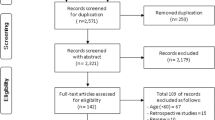
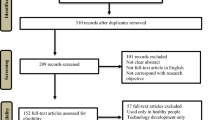
This review explores the effects of markerless motion capture technology-based rehabilitation programs targeting clinical populations and identifies the types of MMC systems used. A systematic search was conducted in the PubMed, Medline, CINAHL, CENTRAL, EMBASE, and IEEE databases. All eligible studies—single-group or controlled trial studies investigating the effectiveness of MMC technology-based rehabilitation programs—were selected. Single-group studies were qualitatively described; only controlled trial studies were included in the meta-analysis. Effects regarding the application of MMC technology for different types of patients and training body parts are summarized. Five single-group studies and 18 controlled trial studies were included. All studies applied MMC technology as a form of virtual reality training to provide rehabilitation programs. Most of the studies were conducted in regard to upper extremity training in stroke populations. Our meta-analysis revealed that there is no significant difference in the upper limb rehabilitation effects between VR training and control interventions. There is potential to apply MMC technology as an alternative way of providing rehabilitation to increase patients’ motivation and adherence. Future studies on the design of training programs and MMC systems in home settings, which are affordable and accessible for patients, are warranted. (This review is registered in PROSPERO, registration ID: CRD42022298189).


Similar content being viewed by others
References
Afsar SI, Mirzayev I, Yemisci OU, Saracgil SNC (2018) Virtual reality in upper extremity rehabilitation of stroke patients: a randomized controlled trial. J Stroke Cerebrovasc Dis 27(12):3473–3478. https://doi.org/10.1016/j.jstrokecerebrovasdis.2018.08.007
Alsinglawi B, Alnajjar F, Mubin O, Novoa M (2019) A framework for home-based stroke rehabilitation using interactive games and augmented reality feedback. In: converging clinical and engineering research on neurorehabilitation: proceedings of the 4th international conference on neurorehabilitation (Icnr2018), Pisa, Italy, p 252-255. https://doi.org/10.1007/978-3-030-01845-0_50
Avcil E, Tarakci D, Arman N, Tarakci E (2021) Upper extremity rehabilitation using video games in cerebral palsy: a randomized clinical trial. Acta Neurol Belg 121(4):1053–1060. https://doi.org/10.1007/s13760-020-01400-8
Bonato P (2005) Advances in wearable technology and applications in physical medicine and rehabilitation. J Neuroeng Rehabil 2(1):2. https://doi.org/10.1186/1743-0003-2-2
Burridge JH, Lee ACW, Turk R, Stokes M, Whitall J, Vaidyanathan R, Clatworthy P, Hughes AM, Meagher C, Franco E (2017) Telehealth, wearable sensors, and the internet: will they improve stroke outcomes through increased intensity of therapy, motivation, and adherence to rehabilitation programs? J Neurol Phys Ther 41(Suppl 3):S32–S38. https://doi.org/10.1097/NPT.0000000000000183
Cannell J, Jovic E, Rathjen A, Lane K, Tyson AM, Callisaya ML, Smith ST, Ahuja KD, Bird ML (2018) The efficacy of interactive, motion capture-based rehabilitation on functional outcomes in an inpatient stroke population: a randomized controlled trial. Clin Rehabil 32(2):191–200. https://doi.org/10.1177/0269215517720790
Capo AJ, Martinez-Bueso P, Moya-Alcover B, Varona J (2014) Interactive rehabilitation system for improvement of balance therapies in people with cerebral palsy. IEEE Trans Neural Sys Rehabil Eng 22(2):419–427. https://doi.org/10.1109/TNSRE.2013.2279155
Carr JH, Shepherd RB (2010) Neurological rehabilitation: optimizing motor performance. Churchill Livingstone, US
Cho GH, Hwangbo G, Shin HS (2014) The effects of virtual reality-based balance training on balance of the elderly. J Phys Ther Sci 26(4):615–617. https://doi.org/10.1589/jpts.26.615
Cuesta-Gómez A, Sánchez-Herrera-Baeza P, Oña-Simbaña ED, Martínez-Medina A, Ortiz-Comino C, Balaguer-Bernaldo-de-Quirós C, Jardón-Huete A, Cano-de-la-Cuerda R (2020) Effects of virtual reality associated with serious games for upper limb rehabilitation inpatients with multiple sclerosis: Randomized controlled trial. J Neuroeng Rehabil 17(1):90. https://doi.org/10.1186/s12984-020-00718-x
Dabholkar TY, Shah SS (2020) Effect of virtual reality training using leap motion controller on impairments and disability in patients with wrist and hand stiffness. Indian J Public Health Res Dev 11(11):210–219
de Los-Reyes-Guzmán A, Alvarez-Rodríguez M, Lozano-Berrio V, Domingo-García A, Ceruelo-Abajo S (2021) Low-cost virtual reality. A new application for upper extremity motor rehabilitation in neurological pathology: pilot study. Rehabil (Madr). https://doi.org/10.1016/j.rh.2021.07.001
Desrosiers J, Bravo G, Hébert R, Dutil É, Mercier L (1994) Validation of the box and block test as a measure of dexterity of elderly people: reliability, validity, and norms studies. Arch Phys Med Rehabil 75(7):751–755
Ding W, Zheng Y, Su Y, Li X (2018) Kinect-based virtual rehabilitation and evaluation system for upper limb disorders: a case study. J Back Musculoskelet Rehabil 31(4):611–621. https://doi.org/10.3233/BMR-140203
Fernández-González P, Carratalá-Tejada M, Monge-Pereira E, Collado-Vázquez S, Baeza PSH, Cuesta-Gómez A, Oña-Simbaña ED, Jardón-Huete A, Molina-Rueda F, de Quirós CBB (2019) Leap motion controlled video game-based therapy for upper limb rehabilitation in patients with parkinson’s disease: a feasibility study. J Neuroeng Rehabil 16(1):133. https://doi.org/10.1186/s12984-019-0593-x
Gramstad A, Storli SL, Hamran T (2013) “Do I need it? Do I really need it?” Elderly peoples experiences of unmet assistive technology device needs. Disabil Rehabil Assist Technol 8(4):287–293. https://doi.org/10.3109/17483107.2012.699993
Hess JA, Woollacott M (2005) Effect of high-intensity strength-training on functional measures of balance ability in balance-impaired older adults. Manip Physiol Ther 28(8):582–590. https://doi.org/10.1016/j.jmpt.2005.08.013
Higgins J (2011) Cochrane handbook for systematic reviews of interventions. Version 5.1. 0 [updated March 2011]. The cochrane collaboration. Wiley, New Jersey
Hughes AM, Meagher C, Burridge J (2017) Arm rehabilitation at home for people with stroke: staying safe: encouraging results from the co-designed lifeCIT programme. In: Kollak I (ed) Safe at home with assistive technology. Springer, Cham, pp 59–79
Hughes CML, Padilla A, Hintze A, Raymundo TM, Sera M, Weidner S, Ontiveros J, Peng T, Encarcion A, Cruz ZA (2020) Developing an mHealth app for post-stroke upper limb rehabilitation: feedback from US and ethiopian rehabilitation clinicians. Health Inform J 26(2):1104–1117. https://doi.org/10.1177/1460458219868356
Jonsdottir J, Perini G, Ascolese A, Bowman T, Montesano A, Lawo M, Bertoni R (2019) Unilateral arm rehabilitation for persons with multiple sclerosis using serious games in a virtual reality approach: Bilateral treatment effect? Mult Scler Relat Disord 35:76–82. https://doi.org/10.1016/j.msard.2019.07.010
Kharrazi H, Lu AS, Gharghabi F, Coleman W (2012) A scoping review of health game research: past, present, and future. Game Health J 1(2):153–164. https://doi.org/10.1089/g4h.2012.0011
Kizony R, Katz N, Weiss PL (2003) Adapting an immersive virtual reality system for rehabilitation. J Vis Comput Animat 14(5):261–268. https://doi.org/10.1002/vis.323
Knippenberg E, Verbrugghe J, Lamers I, Palmaers S, Timmermans A, Spooren A (2017) Markerless motion capture systems as training device in neurological rehabilitation: a systematic review of their use, application, target population and efficacy. J Neuroeng Rehabil 14(1):61. https://doi.org/10.1186/s12984-017-0270-x
Knippenberg E, Lamers I, Timmermans A, Spooren A (2021) Motivation, usability, and credibility of an intelligent activity-based client-centred training system to improve functional performance in neurological rehabilitation: an exploratory cohort study. Int J Environ Res Public Health 18(14):7641. https://doi.org/10.3390/ijerph18147641
Lee JC (2008) Hacking the nintendo wii remote. IEEE Pervasive Comput 7(3):39–45
Lee G (2013) Effects of training using video games on the muscle strength, muscle tone, and activities of daily living of chronic stroke patients. J Phys Ther Sci 25(5):595–597. https://doi.org/10.1589/jpts.25.595
Lee M, Suh D, Son J, Kim J, Eun SD, Yoon B (2016) Patient perspectives on virtual reality-based rehabilitation after knee surgery: importance of level of difficulty. J Rehabil Res Dev 53(2):239–252. https://doi.org/10.1682/JRRD.2014.07.0164
Lee SI, Adans-Dester CP, Grimaldi M, Dowling AV, Horak PC, Black-Schaffer RM, Bonato P, Gwin JT (2018) Enabling stroke rehabilitation in home and community settings: a wearable sensor-based approach for upper-limb motor training. IEEE J Transl Eng Health Med 2(6):2100411. https://doi.org/10.1109/JTEHM.2018.2829208
Levin MF, Snir O, Liebermann DG, Weingarden H, Weiss PL (2012) Virtual reality versus conventional treatment of reaching ability in chronic stroke: clinical feasibility study. Neurol Ther 1(1):3. https://doi.org/10.1007/s40120-012-0003-9
Liang Q, Miao Z (2015) Markerless motion capture based on diffusion geometry and silhouettes. J Electron Imaging 24(5):051003. https://doi.org/10.1117/1.JEI.24.5.051003
Lloréns R, Gil-Gómez JA, Alcañiz M, Colomer C, Noé E (2015a) Improvement in balance using a virtual reality-based stepping exercise: a randomized controlled trial involving individuals with chronic stroke. Clin Rehabil 29(3):261–268. https://doi.org/10.1177/0269215514543333
Lloréns R, Noé E, Colomer C, Alcañiz M (2015b) Effectiveness, usability, and cost-benefit of a virtual reality–based telerehabilitation program for balance recovery after stroke: a randomized controlled trial. Arch Phys Med Rehabil 96(3):418-425.e2. https://doi.org/10.1016/j.apmr.2014.10.019
Lozano-Quilis JA, Gil-Gómez H, Gil-Gómez JA, Albiol-Pérez S, Palacios-Navarro G, Fardoun HM, Mashat AS (2014) Virtual rehabilitation for multiple sclerosis using a kinect-based system: randomized controlled trial. JMIR Serious Games. 2(2):e12. https://doi.org/10.2196/games.2933
Lu W, Tong Z, Chu J (2016) Dynamic hand gesture recognition with leap motion controller. IEEE Signal Process Lett 23(9):1188–1192. https://doi.org/10.1109/LSP.2016.2590470
Maceira-Elvira P, Popa T, Schmid AC, Hummel FC (2019) Wearable technology in stroke rehabilitation: towards improved diagnosis and treatment of upper-limb motor impairment. J Neuroeng Rehabil 16(1):142. https://doi.org/10.1186/s12984-019-0612-y
Moseley AM, Herbert RD, Sherrington C, Maher CG (2002) Evidence for physiotherapy practice: a survey of the physiotherapy evidence database (PEDro). Aust J Physiother 48(1):43–49. https://doi.org/10.1016/s0004-9514(14)60281-6
Mousavi Hondori H, Khademi M (2014) A review on technical and clinical impact of microsoft kinect on physical therapy and rehabilitation. J Med Eng 2014:846514. https://doi.org/10.1155/2014/846514
Mubin O, Alnajjar F, Al Mahmud A, Jishtu N, Alsinglawi B (2020) Exploring serious games for stroke rehabilitation: a scoping review. Disabil Rehabil Assist Technol 17(2):159–165-7. https://doi.org/10.1080/17483107.2020.1768309
Mündermann L, Corazza S, Andriacchi TP (2006) The evolution of methods for the capture of human movement leading to markerless motion capture for biomechanical applications. J Neuroeng Rehabil 3:6. https://doi.org/10.1186/1743-0003-3-6
Norouzi-Gheidari N, Hernandez A, Archambault PS, Higgins J, Poissant L, Kairy D (2020) Feasibility, safety and efficacy of a virtual reality exergame system to supplement upper extremity rehabilitation post-stroke: a pilot randomized clinical trial and proof of principle. Int J of Environ Res Public Health 17(1):113. https://doi.org/10.3390/ijerph17010113
Palacios-Navarro G, García-Magariño I, Ramos-Lorente P (2015) A Kinect-based system for lower limb rehabilitation in parkinson’s disease patients: a pilot study. J Med Syst 39(9):103. https://doi.org/10.1007/s10916-015-0289-0
Paneroni M, Colombo F, Papalia A, Colitta A, Borghi G, Saleri M, Cabiaglia A, Azzalini E, Vitacca M (2015) Is telerehabilitation a safe and viable option for patients with COPD? A Feasibility Study. COPD 12(2):217–225. https://doi.org/10.3109/15412555.2014.933794
Pastor I, Hayes HA, Bamberg SJ (2012) A feasibility study of an upper limb rehabilitation system using kinect and computer games. Annu Int Conf IEEE Eng Med Biol Soc 2012:1286–1289. https://doi.org/10.1109/EMBC.2012.6346173
Pereira MF, Prahm C, Kolbenschlag J, Oliveira E, Rodrigues NF (2020) Application of AR and VR in hand rehabilitation: a systematic review. J Biomed Inform 111:103584. https://doi.org/10.1016/j.jbi.2020.103584
Pompeu JE, Arduini L, Botelho A, Fonseca M, Pompeu SAA, Torriani-Pasin C, Deutsch J (2014) Feasibility, safety and outcomes of playing Kinect Adventures!™ for people with Parkinson’s disease: a pilot study. Physiother 100(2):162–168
Pusztai Z, Hajder L (2017) Accurate calibration of LiDAR-camera systems using ordinary boxes. In: Proceedings of the IEEE international conference on computer vision workshops. https://openaccess.thecvf.com/content_ICCV_2017_workshops/papers/w6/Pusztai_Accurate_Calibration_of_ICCV_2017_paper.pdf
Qiu Q, Cronce A, Patel J, Fluet GG, Mont AJ, Merians AS, Adamovich SV (2020) Development of the home based virtual rehabilitation system (hovrs) to remotely deliver an intense and customized upper extremity training. J Neuroeng Rehabil 17(1):155. https://doi.org/10.1186/s12984-020-00789-w
Rodríguez-Hernández M, Polonio-López B, Corregidor-Sánchez AI, Martín-Conty JL, Mohedano-Moriano A, Criado-Álvarez JJ (2021) Effects of specific virtual reality-based therapy for the rehabilitation of the upper limb motor function post-ictus??: randomized controlled trial. Brain Sci 11(5):555. https://doi.org/10.3390/brainsci11050555
Saposnik G, Cohen LG, Mamdani M, Pooyania S, Ploughman M, Cheung D, Shaw J, Hall J, Nord P, Dukelow S (2016) Efficacy and safety of non-immersive virtual reality exercising in stroke rehabilitation (EVREST): a randomised, multicentre, single-blind, controlled trial. Lancet Neurol 15(10):1019–1027. https://doi.org/10.1016/S1474-4422(16)30121-1
Sarfo FS, Ulasavets U, Opare-Sem OK, Ovbiagele B (2018) Tele-rehabilitation after stroke: an updated systematic review of the literature. J Stroke Cerebrovasc Dis 27(9):2306–2318. https://doi.org/10.1016/j.jstrokecerebrovasdis.2018.05.013
Seo NJ, Crocher V, Spaho E, Ewert CR, Fathi MF, Hur P, Lum SA, Humanitzki EM, Kelly AL, Ramakrishnan V (2019) Capturing upper limb gross motor categories using the kinect® sensor. Am J Occup Ther 73(4):1–10. https://doi.org/10.5014/ajot.2019.031682
Shiri S, Feintuch U, Lorber-Haddad A, Moreh E, Twito D, Tuchner-Arieli M, Meiner Z (2012) A novel virtual reality system integrating online self-face viewing and mirror visual feedback for stroke rehabilitation: rationale and feasibility. Top Stroke Rehabil 19(4):277–286. https://doi.org/10.1310/tsr1904-277
Sin H, Lee G (2013) Additional virtual reality training using Xbox Kinect in stroke survivors with hemiplegia. Am J Phys Med Rehabil 92(10):871–880. https://doi.org/10.1097/PHM.0b013e3182a38e40
Tan CO (2020) Is remote rehabilitation after stroke as effective as conventional therapy. Neurology 95(17):e2462–e2464
Tarakci E, Arman N, Tarakci D, Kasapcopur O (2020) Leap Motion Controller–based training for upper extremity rehabilitation in children and adolescents with physical disabilities: a randomized controlled trial. J Hand Ther 33(2):220-228.e1. https://doi.org/10.1016/j.jht.2019.03.012
Tarakci E, Arman SN, Tarakci D, Akgul Y (2016) Invention of rehabilitative games using the leap motion controller for hand rehabilitation iin children with juvenile idiopathic arthritis and investigation of its’ effectiveness. 23rd PReS 2016 Congress, Genoa, Italy. https://www.researchgate.net/publication/311713678_Invention_of_Rehabilitative_Games_Using_The_Leap_Motion_Controller_For_Hand_Rehabilitation_In_Children_With_Juvenile_Idiopathic_Arthritis_And_Investigation_of_Its'_Effectiveness#fullTextFileContent
Teasell RW, Foley NC, Bhogal SK, Speechley MR (2003) An evidence-based review of stroke rehabilitation. Top Stroke Rehabil 10(1):29–58. https://doi.org/10.1310/8YNA-1YHK-YMHB-XTE1
This is Why Microsoft Kinect was a Complete Failure (2021) Retrieved 30 november from. <https://www.looper.com/301470/this-is-why-microsoft-kinect-was-a-complete-failure/>
Tsekleves E, Paraskevopoulos IT, Warland A, Kilbride C (2016) Development and preliminary evaluation of a novel low cost VR-based upper limb stroke rehabilitation platform using Wii technology. Disabil Rehabil Assist Technol 11(5):413–422. https://doi.org/10.3109/17483107.2014.981874
Vanbellingen T, Filius SJ, Nyffeler T, van Wegen EE (2017) Usability of videogame-based dexterity training in the early rehabilitation phase of stroke patients: a pilot study. Front Neurol 8(8):654. https://doi.org/10.3389/fneur.2017.00654
Waliño-Paniagua CN, Gomez-Calero C, Jiménez-Trujillo MI, Aguirre-Tejedor L, Bermejo-Franco A, Ortiz-Gutiérrez RM, Cano-de-la-Cuerda R (2019) Effects of a game-based virtual reality video capture training program plus occupational therapy on manual dexterity in patients with multiple sclerosis: a randomized controlled trial. J Healthc Eng 2019:9780587. https://doi.org/10.1155/2019/9780587
Wang ZR, Wang P, Xing L, Mei LP, Zhao J, Zhang T (2017) Leap Motion-based virtual reality training for improving motor functional recovery of upper limbs and neural reorganization in subacute stroke patients. Neural Regen Res 12(11):1823–1831. https://doi.org/10.4103/1673-5374.219043
Zhang Z (2012) Microsoft kinect sensor and its effect. IEEE Multimed 19(2):4–10
Funding
This work was partially supported by the Research Impact Fund (Grant No.: R5028-20), Research Grants Council, University Grants Committee, Hong Kong SAR.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interest
The authors report no competing interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Lam, W.W.T., Fong, K.N.K. The application of markerless motion capture (MMC) technology in rehabilitation programs: a systematic review and meta-analysis. Virtual Reality 27, 3363–3378 (2023). https://doi.org/10.1007/s10055-022-00696-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10055-022-00696-6