Abstract
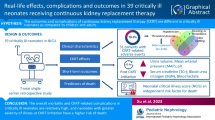
We hypothesized that patients with sepsis and AKI, especially patients without preserved renal function, and treated with continuous veno-venous hemodiafiltration (CVVHDF), have lower risk for mortality than patients treated with continuous veno-venous hemofiltration (CVVH). Patients were included if they fulfilled the diagnosis of severe sepsis or septic shock, suffered AKI and received continuous renal replacement therapy (CRRT) in intensive care unit. There were 62 patients treated by CVVH and 75 treated by CVVHDF. Mean survival time was longer in CVVHDF group with oliguric/anuric patients than in CVVH group. CVVH, and not classic risk factors, was associated with higher overall mortality in oliguric/anuric patients. In the linear regression model, hourly urine output was the strongest and positive predictor of longer survival. CVVHDF is according to our results a CRRT modality of choice for the treatment and lower mortality of septic patients with AKI where renal function is no longer preserved. CRRT has been associated with improved renal recovery, but it should be started earlier in AKI evolution with still preserved hourly urine output which is the most sensitive and prognostic marker of survival in septic patients with AKI.



Similar content being viewed by others
References
Bone RC, Balk RA, Cerra FB, et al. American College of Chest Physicians/Society of Critical Care Medicine Consensus Conference: definitions for sepsis and organ failure and guidelines for the use of innovative therapies in sepsis. Crit Care Med. 1992;20:864–74.
Vincent J-L, Opal SM, Marshall JC, Tracey KJ. Sepsis definitions: time for change. Lancet. 2013;381:774–5.
Singer M, Deutschman CS, Seymour CW, et al. The third international consensus definitions for sepsis and septic shock (sepsis-3). JAMA. 2016;315:801–10.
Lafrance JP, Miller DR. Acute kidney injury associates with increased long-term mortality. J Am Soc Nephrol. 2010;21:345–52.
Zarjou A, Agarwal A. Sepsis and acute kidney injury. J Am Soc Nephrol. 2011;22:999–1006.
Uchino S, Kellum JA, Bellomo R, Doig GS, Morimatsu H, Morgera S, Schetz M, Tan I, Bouman C, Macedo E, Gibney N, Tolwani A, Ronco C. Acute renal failure in critically ill patients: a multinational, multicenter study. JAMA. 2005;294:813–8.
Wan L, Bagshaw SM, Langenberg C, Saotome T, May C, Bellomo R. Pathophysiology of septic acute kidney injury: what do we really know? Crit Care Med. 2008;36:S198–203.
Smilde TD, van Veldhuisen DJ, Navis G, Voors AA, Hillege HL. Drawbacks and prognostic value of formulas estimating renal function in patients with chronic heart failure and systolic dysfunction. Circulation. 2006;114:1572–80.
Kidney Disease Outcomes Quality Initiative. KDIGO clinical practice guideline for acute kidney injury. Kidney Int Suppl. 2012;2:8.
Andrikos E, Tseke P, Balafa O, Cruz DN, Tsinta A, Androulaki M, et al. Epidemiology of acute renal failure in ICUs: a multi-center prospective study. Blood Purif. 2009;28:239–44.
Bagshaw SM, George C, Bellomo R. ANZICS database management committee early acute kidney injury and sepsis: a multicentre evaluation. Crit Care. 2008;12:R47.
Alobaidi R, Basu RK, Goldstein SL, Bagshaw SM. Sepsis-associated acute kidney injury. Semin Nephrol. 2015;35:2–11.
Bagshaw SM, Uchino S, Bellomo R, Morimatsu H, Morgera S, Schetz M, et al. Septic acute kidney injury in critically ill patients: clinical characteristics and outcomes. Clin J Am Soc Nephrol. 2007;2:431–9.
Prowle JR, Bellomo B. Sepsis-associated acute kidney injury: macrohemodynamic and microhemodynamic alterations in the renal circulation. Semin Nephrol. 2015;35:64–74.
RENAL Study Investigators, Bellomo R, Cass A, Cole L, Finfer S, Gallagher M, et al. Intensity of continuous renal- replacement therapy in critically ill patients. N Engl J Med. 2009;361:1627–38.
Palevsky PM, Zhang JH, O’Connor TZ, Chertow GM, Choudhury D, et al. Intensity of renal support in critically ill patients with acute kidney injury. N Engl J Med. 2008;359:7–20.
Silvester W, Bellomo R, Cole L. Epidemiology, management, and outcome of severe acute renal failure of critical illness in Australia. Crit Care Med. 2001;29:1910–5.
AlEnezi F, Alhazzani W, Ma J, Alanazi S, Salib M, Attia M, Thabane L, Fox-Robichaud A. Continuous venovenous hemofiltration versus continuous venovenous hemodiafiltration in critically ill patients: a retrospective cohort study from a Canadian tertiary centre. Can Resp J. 2014;21:176–80.
Prowle JR, Liu YL, Licari E, Bagshaw SM, Egi M, Haase M, et al. Oliguria as predictive biomarker of acute kidney injury in critically ill patients. Crit Care. 2011;15:R172.
Macedo E, Malhotra R, Claure-Del Granado R, Fedullo P, Mehta RL. Defining urine output criterion for acute kidney injury in critically ill patients. Nephrol Dial Transpl. 2011;26:509–15.
Joannes-Boyau O, Honore PM, Perez P, Bagshaw SM, Grand H, Canivet JL, et al. High-volume versus standard-volume haemofiltration for septic shock patients with acute kidney injury (IVOIRE study): a multicentre randomized controlled trial. Intensive Care Med. 2013;39:1535–46.
Zhang P, Yang Y, Lv R, Zhang Y, Xie W, Chen J. Effect of the intensity of continuous renal replacement therapy in patients with sepsis and acute kidney injury: a single-center randomized clinical trial. Nephrol Dial Transplant. 2012;27:967–73.
Grootendorst AF. The potential role of hemofiltration in the treatment of patients with septic shock and multiple organ dysfunction syndrome. Adv Renal Replace Ther. 1994;1:176–84.
Wakabayashi Y, Kamijou Y, Soma K, Ohwada T. Removal of circulating cytokines by continuous haemofiltration in patients with systemic inflammatory response syndrome or multiple organ dysfunction syndrome. Br J Surg. 1996;83:393–4.
Braun N, Giolai M, Rosenfeld S, Banzhaff W, Fretschner R, Weinstock C, Erley C, Muller GA, Warth H, Northoff H, Risler T. Clearance of interleukin-6 during continuous veno-venous hemofiltration in patients with septic shock: a prospective, controlled clinical study [Abstract]. J Am Soc Nephrol. 1993;4:336.
Graziani G, Bordone G, Bellato V, Finazzi S, Angelini C, Badalamenti S. Role of the kidney in plasma cytokine removal in sepsis syndrome: a pilot study. J Nephrol. 2006;19:176–82.
Goldfarb S, Golper TA. Proinflammatory cytokines and hemofiltration membranes. J Am Soc Nephrol. 1994;5:228–32.
Ronco C, Tetta C, Lupi A, Galloni E, Bettini MC, Sereni L, Mariano F, DeMartino A, Montrucchio G, Camussi G, La Greca G. Removal of platelet-activating factor in experimental continuous arteriovenous hemofiltration. Crit Care Med. 1995;23:99–107.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Rights and permissions
About this article
Cite this article
Premuzic, V., Basic-Jukic, N., Jelakovic, B. et al. Differences in CVVH vs. CVVHDF in the management of sepsis-induced acute kidney injury in critically ill patients. J Artif Organs 20, 326–334 (2017). https://doi.org/10.1007/s10047-017-0970-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10047-017-0970-9