Abstract
Purpose
There is considerable variability among surgeons regarding the type of mesh used in ventral hernia repair. There has been an increasing incidence of mesh fractures with lightweight (LW) and mediumweight (MW) meshes. However, HW mesh has been associated with a greater foreign body sensation and chronic pain. This meta-analysis aims to compare the outcomes of HW and non-heavyweight (NHW) meshes in ventral hernia repair.
Methods
We systematically reviewed the PubMed, Embase, Cochrane, and Scopus databases to identify studies comparing HW with NHW meshes in hernia repair. Outcomes analyzed included hernia recurrence, seroma, hematoma, foreign body sensation, postoperative pain, and wound infection. We performed two subgroup analyses focusing on randomized controlled trials and open retromuscular repairs. Statistical analysis was performed using RevMan 5.4.
Results
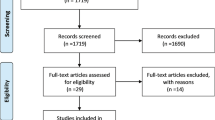
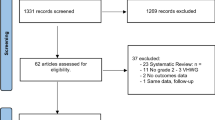
We screened 1704 studies. Nine studies were finally included in this meta-analysis and comprised 3001 patients from 4 RCTs and 5 non-randomized. The majority of patients (57.1%) underwent open retromuscular repair. HW mesh was significantly associated with increased in foreign body sensation (OR 3.71; 95% CI 1.40–9.84; p = 0.008), but there was no difference in other outcomes. In RCTs analysis, there was no difference between meshes. In open retromuscular repairs, HW mesh was associated with more seromas (OR 1.48; 95% CI 1.01–2.17; p = 0.05).
Conclusion
Our study found that HW mesh was associated with more foreign body sensation. Also, open retromuscular repairs analysis showed that HW was associated with more seromas. Further randomized studies are needed to understand better the role of HW mesh in ventral hernia repair.



Similar content being viewed by others
Data availability
The data extracted from individual studies included in this meta-analysis can be obtained from their respective original sources. A list of the studies along with their citations is provided in the references section of this article. Supplementary materials accompanying this article contain additional information about the bias assessment.
References
Liang MK, Holihan JL, Itani K, Alawadi ZM, Gonzalez JRF, Askenasy EP, Ballecer C, Chong HS, Goldblatt MI, Greenberg JA, Harvin JA, Keith JN, Martindale RG, Orenstein S, Richmond B, Roth JS, Szotek P, Towfigh S, Tsuda S, Berger DH (2017) Ventral hernia management: expert consensus guided by systematic review. Annals Surg 265(1):80–89. https://doi.org/10.1097/SLA.0000000000001701
Funk LM, Perry KA, Narula VK, Mikami DJ, Melvin WS (2013) Current national practice patterns for inpatient management of ventral abdominal wall hernia in the United States. Surg Endosc 27(11):4104–4112. https://doi.org/10.1007/s00464-013-3075-4
Luijendijk RW, Hop WCJ, Van Den Tol MP, De Lange DCD, Braaksma MMJ, IJzermans JNM, Boelhouwer RU, De Vries BC, Salu MKM, Wereldsma JCJ, Bruijninckx CMA, Jeekel J (2000) A comparison of suture repair with mesh repair for incisional hernia. New Eng J Med 343(6):392–398. https://doi.org/10.1056/NEJM200008103430603
Cobb WS (2018) A Current review of synthetic meshes in abdominal wall reconstruction. Plastic Reconstruct Surg 142:64S-71S. https://doi.org/10.1097/PRS.0000000000004857
Grubnik VV, Grubnik AV, Vorotyntseva KO (2014) Laparoscopic repair of incisional and ventral hernias with the new type of meshes: Randomized control trial. Videosurg Other Miniinvasive Tech 2:145–151. https://doi.org/10.5114/wiitm.2014.41623
Amid PK (1997) Classification of biomaterials and their related complications in abdominal wall hernia surgery. Hernia 1(1):15–21. https://doi.org/10.1007/BF02426382
Brown CN, Finch JG (2010) Which mesh for hernia repair? Ann R Coll Surg Engl 92(4):272–278. https://doi.org/10.1308/003588410X12664192076296
Moreno-Egea A, Carrillo-Alcaraz A, Soria-Aledo V (2013) Randomized clinical trial of laparoscopic hernia repair comparing titanium-coated lightweight mesh and medium-weight composite mesh. Surg Endosc 27(1):231–239. https://doi.org/10.1007/s00464-012-2425-y
Nguyen PT, Asarias JR, Pierce LM (2012) Influence of a new monofilament polyester mesh on inflammation and matrix remodeling. J Invest Surg 25(5):330–339. https://doi.org/10.3109/08941939.2011.639848
Lake SP, Ray S, Zihni AM, Thompson DM, Gluckstein J, Deeken CR (2015) Pore size and pore shape – but not mesh density – alter the mechanical strength of tissue ingrowth and host tissue response to synthetic mesh materials in a porcine model of ventral hernia repair. J Mech Behav Biomed Mater 42:186–197. https://doi.org/10.1016/j.jmbbm.2014.11.011
Petro CC, Nahabet EH, Criss CN, Orenstein SB, Von Recum HA, Novitsky YW, Rosen MJ (2015) Central failures of lightweight monofilament polyester mesh causing hernia recurrence: a cautionary note. Hernia 19(1):155–159. https://doi.org/10.1007/s10029-014-1237-5
Li J, Ji Z, Zhang W, Li L (2015) The comparison of lightweight mesh and standard mesh in incisional hernia repair with the open sublay technique: the results of a meta-analysis. Surg Laparoscopy, Endoscopy & Percutaneous Techniques 25(3):238–244. https://doi.org/10.1097/SLE.0000000000000144
Krpata DM, Petro CC, Prabhu AS, Tastaldi L, Zolin S, Fafaj A, Rosenblatt S, Poulose BK, Pierce RA, Warren JA, Carbonell AM, Goldblatt MI, Stewart TG, Olson MA, Rosen MJ (2021) Effect of hernia mesh weights on postoperative patient-related and clinical outcomes after open ventral hernia repair: a randomized clinical trial. JAMA Surg 156(12):1085. https://doi.org/10.1001/jamasurg.2021.4309
Kroh A, Zufacher M, Eickhoff R, Heise D, Helmedag M, Ulmer F, Neumann UP, Conze J, Hilgers R-D, Binnebösel M (2023) No difference in outcomes between large- and small-pore meshes in a prospective, randomized, multicenter trial investigating open retromuscular meshplasty for incisional hernia repair. Langenbeck’s Archives of Surgery 408(1):22. https://doi.org/10.1007/s00423-022-02751-x
Moher D, Liberati A, Tetzlaff J, Altman DG, The PRISMA Group (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med 6(7):e1000097. https://doi.org/10.1371/journal.pmed.1000097
Sterne JA, Hernán MA, Reeves BC, Savović J, Berkman ND, Viswanathan M, Henry D, Altman DG, Ansari MT, Boutron I, Carpenter JR, Chan A-W, Churchill R, Deeks JJ, Hróbjartsson A, Kirkham J, Jüni P, Loke YK, Pigott TD, Higgins JP (2016) ROBINS-I: A tool for assessing risk of bias in non-randomised studies of interventions. BMJ. https://doi.org/10.1136/bmj.i4919
Higgins JPT, Altman DG, Gotzsche PC, Juni P, Moher D, Oxman AD, Savovic J, Schulz KF, Weeks L, Sterne JAC, Cochrane Bias Methods Group, & Cochrane Statistical Methods Group (2011) The cochrane collaboration’s tool for assessing risk of bias in randomised trials. BMJ 343(2):d5928–d5928. https://doi.org/10.1136/bmj.d5928
Welty G, Klinge U, Klosterhalfen B, Kasperk R, Schumpelick V (2001) Functional impairment and complaints following incisional hernia repair with different polypropylene meshes. Hernia 5(3):142–147. https://doi.org/10.1007/s100290100017
Schmidbauer S, Ladurner R, Hallfeldt KK, Mussack T (2005) Heavy-weight versus low-weight polypropylene meshes for open sublay mesh repair of incisional hernia. Eur J Med Res 10(6):247–253
Conze J, Kingsnorth AN, Flament JB, Simmermacher R, Arlt G, Langer C, Schippers E, Hartley M, Schumpelick V (2005) Randomized clinical trial comparing lightweight composite mesh with polyester or polypropylene mesh for incisional hernia repair. Br J Surg 92(12):1488–1493. https://doi.org/10.1002/bjs.5208
Berrevoet F, Maes L, De Baerdemaeker L, Rogiers X, Troisi R, de Hemptinne B (2010) Comparable results with 3-year follow-up for large-pore versus small-pore meshes in open incisional hernia repair. Surgery 148(5):969–975. https://doi.org/10.1016/j.surg.2010.02.011
Groene SA, Prasad T, Lincourt AE, Augenstein VA, Sing R, Heniford BT (2016) Prospective, multi-institutional surgical and quality-of-life outcomes comparison of heavyweight, midweight, and lightweight mesh in open ventral hernia repair. Am J of Surg 212(6):1054–1062. https://doi.org/10.1016/j.amjsurg.2016.09.003
Rogmark P, Ekberg O, Montgomery A (2017) Long-term retromuscular and intraperitoneal mesh size changes within a randomized controlled trial on incisional hernia repair, including a review of the literature. Hernia : J Hern Abdominal Wall Surg 21(5):687–696. https://doi.org/10.1007/s10029-017-1624-9
Heniford BT, Ross SW, Wormer BA, Walters AL, Lincourt AE, Colavita PD, Kercher KW, Augenstein VA (2020) Preperitoneal ventral hernia repair: a decade long prospective observational study with analysis of 1023 patient outcomes. Ann Surg 271(2):364–374. https://doi.org/10.1097/SLA.0000000000002966
Makam R, Chamany T, Nagur B, Bilchod S, Kulkarni A (2023) Laparoscopic subcutaneous onlay mesh repair for ventral hernia: our early experience. J Minimal Access Surg 19(2):223. https://doi.org/10.4103/jmas.jmas_225_22
Poulose BK, Shelton J, Phillips S, Moore D, Nealon W, Penson D, Beck W, Holzman MD (2012) Epidemiology and cost of ventral hernia repair: making the case for hernia research. Hernia 16(2):179–183. https://doi.org/10.1007/s10029-011-0879-9
Burger JWA, Luijendijk RW, Hop WCJ, Halm JA, Verdaasdonk EGG, Jeekel J (2004) Long-term follow-up of a randomized controlled trial of suture versus mesh repair of incisional hernia. Ann Surg 240(4):578–585. https://doi.org/10.1097/01.sla.0000141193.08524.e7
Maskal S, Miller B, Ellis R, Phillips S, Prabhu A, Beffa L, Krpata D, Rosenblatt S, Rosen M, Petro C (2023) Mediumweight polypropylene mesh fractures after open retromuscular ventral hernia repair: Incidence and associated risk factors. Surg Endosc. https://doi.org/10.1007/s00464-023-10039-4
Miller BT, Baier KF, Zolin SJ, Huang L-C, Phillips S, Petro CC, Beffa LRA, Krpata DM, Rosen MJ, Prabhu AS (2023) Long-term outcomes of seromas after ventral hernia repair: A propensity score-matched analysis of the abdominal core health quality collaborative. Hernia J Hernias Abd Wall Surg 27(2):373–378. https://doi.org/10.1007/s10029-022-02613-x
Marcolin P, de Figueiredo SMP, Constante MM, de Melo VMF, de Araújo SW, Mao R-MD, Lu R (2023) Drain placement in retromuscular ventral hernia repair: a systematic review and meta-analysis. Hernia J Hernias Abd Wall Surg. https://doi.org/10.1007/s10029-023-02792-1
Rickert A, Kienle P, Kuthe A, Baumann P, Engemann R, Kuhlgatz J, von Frankenberg M, Knaebel HP, Büchler MW (2012) A randomised, multi-centre, prospective, observer and patient blind study to evaluate a non-absorbable polypropylene mesh vs a partly absorbable mesh in incisional hernia repair. Langenbeck’s Arch Surg 397(8):1225–1234. https://doi.org/10.1007/s00423-012-1009-6
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Dr. Richard Lu received payment/honoraria for lectures and presentations from Intuitive Surgical that are unrelated to this work. Bruna Oliveira Trindade, Patrícia Marcolin, Gabriela Rangel Brandão, Sarah Bueno Motter, Sérgio Mazzola Poli de Figueiredo, and Rui-Min Diana Mao declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Oliveira Trindade, B., Marcolin, P., Brandao, G. et al. Heavyweight versus non-heavyweight mesh in ventral hernia repair: a systematic review and meta-analysis. Hernia 28, 291–300 (2024). https://doi.org/10.1007/s10029-023-02865-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10029-023-02865-1