Abstract
Purpose
Obturator Hernia (OH) is a rare type of abdominal wall hernia. It usually occurs in elderly women with late symptomatic presentation, increasing mortality rates. Surgery is the standard of care for OH, and laparotomy with simple suture closure of the defect is commonly used. Given the rarity of this disease, large studies are lacking, and data to drive management are still limited. This systematic review and meta-analysis aimed to describe current surgical options for OHs, with a focus on comparing the effectiveness and safety of mesh use with primary repair.
Methods
PubMed, EMBASE, and Cochrane were searched for studies comparing mesh and non-mesh repair for OH. Postoperative outcomes were assessed by pooled analysis and meta-analysis. Statistical analysis was performed using RevMan 5.4.
Results
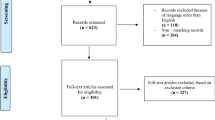
One thousand seven hundred and sixty studies were screened and sixty-seven were thoroughly reviewed. We included 13 observational studies with 351 patients surgically treated for OH with mesh or non-mesh repair. One hundred and twenty (34.2%) patients underwent mesh repair and two hundred and thirty-one (65.81%) underwent non-mesh repair. A total of 145 (41.3%) underwent bowel resection, with the majority having a non-mesh repair performed. Hernia recurrence was significantly higher in patients who underwent hernia repair without mesh (RR 0.31; 95% CI 0.11–0.94; p = 0.04). There were no differences in mortality (RR 0.64; 95% CI 0.25–1.62; p = 0.34; I2 = 0%) or complication rates (RR 0.59; 95% CI 0.28–1.25; p = 0.17; I2 = 50%) between both groups.
Conclusion
Mesh repair in OH was associated with lower recurrence rates without an increase in postoperative complications. While mesh in clean cases is more likely to offer benefits, an overall recommendation regarding its use in OH repair cannot be made due to potential bias across studies. Given that many OH patients are frail and present emergently, the decision to use mesh is complex and should consider the patient’s clinical status, comorbidities, and degree of intraoperative contamination.





Similar content being viewed by others
Data availability
Because this meta-analysis was based on data extracted from previously published research, all the data and study materials are available in the public domain. The authors of this meta-analysis do not have access to patient-level data of the individual studies. Researchers with an interest in individual-level data from the studies included in this meta-analysis are encouraged to contact the corresponding author from each study for such request.
References
Park J (2020) Obturator hernia: clinical analysis of 11 patients and review of the literature. Med (Baltimore). 99:e21701. https://doi.org/10.1097/MD.0000000000021701
Holm MA, Fonnes S, Andresen K, Rosenberg J (2021) Laparotomy with suture repair is the most common treatment for obturator hernia: a scoping review. Langenbecks Arch Surg 406:1733–1738. https://doi.org/10.1007/s00423-021-02293-8
Schizas D et al (2021) Obturator hernias: a systematic review of the literature. Hernia 25:193–204. https://doi.org/10.1007/s10029-020-02282-8
Li Z, Gu C, Wei M, Yuan X, Wang Z (2021) Diagnosis and treatment of obturator hernia: retrospective analysis of 86 clinical cases at a single institution. BMC Surg 21:124. https://doi.org/10.1186/s12893-021-01125-2
Poli M, de Figueiredo S, Tastaldi L, Mao RMD, Lu R, Tyler D (2021) A case report and a contemporary review of incarcerated and strangulated obturator hernia repair. Int J Abdom Wall Hernia Surg 4:166–173. https://doi.org/10.4103/ijawhs.ijawhs_60_21
Sterne JAC, Hernán MA, McAleenan A, Reeves BC, Higgins JPT (updated 2022) Cochrane Handbook for Systematic Reviews of Interventions. In: Higgins JPT, Thomas J, Chandler J, Cumpston M, Li T, Page MJ, Welch VA (editors) Chapter 25: Assessing risk of bias in a non-randomized study, version 6.3. Cochrane. Available from www.training.cochrane.org/handbook
Sterne JA et al (2016) ROBINS-I: a tool for assessing risk of bias in non-randomised studies of interventions. BMJ. https://doi.org/10.1136/bmj.i4919
Puhan MA, Schunemann HJ, Murad MH et al (2014) A GRADE Working Group approach for rating the quality of treatment effect estimates from network meta-analysis. BMJ 349:5630. https://doi.org/10.1136/bmj.g5630
Moher D, Liberati A, Tetzlaff J, Altman DG (2009) Preferred reporting items for systematic reviews and meta-analyses: The PRISMA statement. BMJ 339:332–336. https://doi.org/10.1136/bmj.b2535
Hayama S, Ohtaka K, Takahashi Y, Ichimura T, Senmaru N, Hirano S (2015) Laparoscopic reduction and repair for incarcerated obturator hernia: comparison with open surgery. Hernia 19:809–814. https://doi.org/10.1007/s10029-014-1328-3
Hisamatsu Y, Yamagata M, Miyazaki M et al (2019) Impact of bowel resection on postoperative mortality in patients with obturator hernias. Hernia 23:317–322. https://doi.org/10.1007/s10029-018-1835-8
Karasaki T, Nomura Y, Tanaka N (2014) Long-term outcomes after obturator hernia repair: retrospective analysis of 80 operations at a single institution. Hernia 18:393–397. https://doi.org/10.1007/s10029-013-1159-
Karashima R, Kimura M, Taura N, Shimokawa Y, Nishimura T, Baba H (2016) Total extraperitoneal approach for incarcerated obturator hernia repair. Hernia 20:479–482. https://doi.org/10.1007/s10029-015-1437-7
Kawanaka H, Hiroshige S, Kubo N, Hirashita T, Masuda T, Kaisyakuji Y, Tajiri T, Egashira A, Matsumoto T, Yano T (2018) Therapeutic strategy for incarcerated obturator hernia using preoperative manual reduction and laparoscopic repair. J Am Coll Surg 226:891–901. https://doi.org/10.1016/j.jamcollsurg.2018.02.009
Leung ALH, Yang GPC, Chan OCY, Lai ECH, Tang C-N, Li MKW (2012) Emergency laparoscopic repair. Surg Pract 16:90–93. https://doi.org/10.1111/j.1744-1633.2012.00597.x
Liu J, Zhu Y, Shen Y et al (2017) The feasibility of laparoscopic management of incarcerated obturator hernia. Surg Endosc 31:656–660. https://doi.org/10.1007/s00464-016-5016-5
Mantoo SK, Mak K, Tan TJ (2009) Obturator hernia: diagnosis and treatment in the modern era. Singapore Med J 50:866–870
Mena A et al (2002) Hernia obturatriz: análisis de nuestra serie y revisión de la enfermedad. Cir Esp 72:67–71. https://doi.org/10.1016/S0009-739X(02)72012-5
Nasir BS, Zendejas B, Ali SM, Groenewald CB, Heller SF, Farley DR (2012) Obturator hernia: the mayo clinic experience. Hernia 16:315–319. https://doi.org/10.1007/s10029-011-0895-9
Ng DC, Tung KL, Tang CN, Li MK (2014) Fifteen-year experience in managing obturator hernia: from open to laparoscopic approach. Hernia 18:381–386. https://doi.org/10.1007/s10029-013-1080-0
Rodríguez-Hermosa JI, Codina-Cazador A, Maroto-Genover A et al (2008) Obturator hernia: clinical analysis of 16 cases and algorithm for its diagnosis and treatment. Hernia 12:289–297. https://doi.org/10.1007/s10029-007-0328-y
Chihara N, Suzuki H, Sukegawa M, Nakata R, Nomura T, Yoshida H (2019) Is the laparoscopic approach feasible for reduction and herniorrhaphy in cases of acutely incarcerated/strangulated groin and obturator Hernia?: 17-year experience from open to laparoscopic approach. J Laparoendosc Adv Surg Tech A 29:631–637. https://doi.org/10.1089/lap.2018.0506
Kohga A, Kawabe A, Okumura T, Yamashita K, Isogaki J, Suzuki K (2018) Laparoscopic repair is a treatment of choice for selected patients with incarcerated obturator hernia. Hernia 22:887–895. https://doi.org/10.1007/s10029-018-1747-7
HerniaSurge Group (2018) International guidelines for groin hernia management. Hernia 22:1–165. https://doi.org/10.1007/s10029-017-1668-x
Oida T, Kawasaki A, Mimatsu K et al (2012) Mesh vs. non-mesh repair for inguinal hernias in emergency operations. Hepatogastroenterology 59:2112–2114
Acknowledgements
The authors would like to thank Rhanderson Cardoso M.D. for supporting this research.
Funding
The authors did not receive support from any organization for the submitted work.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study's conception and design. MMB, CPG, and IC performed material preparation, data collection, and analysis. The first draft of the manuscript was written by MMB, CPG, IC, SMPF, and R-MDM. All authors critically reviewed previous versions of the manuscript. All authors read and approved the final manuscript. All authors agree to be accountable for all aspects of the work.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no relevant financial or non-financial interests to disclose. Dr. Sergio Mazzola Poli de Figueiredo and Dr. Rui-Min Diana Mao have no disclosures. Dr. Richard Lu received payment/honoraria for lectures and presentations from Intuitive Surgical that are unrelated to this work.
Ethical approval
Not applicable.
Consent to participate
Not applicable.
Consent to publish
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Burla, M.M., Gomes, C.P., Calvi, I. et al. Management and outcomes of obturator hernias: a systematic review and meta-analysis. Hernia 27, 795–806 (2023). https://doi.org/10.1007/s10029-023-02808-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10029-023-02808-w