Abstract
Purpose
The advantages of minimally invasive inguinal hernia repair (MIHR) over open hernia repair (OHR) continue to be debated. We compared MIHR to OHR by utilizing the Army Physical Fitness Test (APFT) as an outcome measure.
Methods
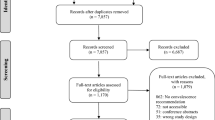
The APFT is a three-component test scored on a normalized 300 point scale taken semiannually by active-duty military. We identified 1119 patients who met inclusion criteria: 588 in the OHR group and 531 in the MIHR group. Changes in APFT scores, time on post-operative duty restrictions (military profile), and time interval to first post-operative APFT were compared using regression analysis.
Results
Postoperatively, no APFT score change difference was observed between the OHR or MIHR groups (− 7.3 ± 30 versus − 5.5 ± 27.7, p = 0.2989). Service members undergoing OHR and MIHR underwent their first post-operative APFT at equal mean timeframes (6.6 ± 5 months versus 6.7 ± 5.1, p = 0.74). No difference was observed for time in months spent on an official temporary duty restriction (military profile) for either OHR or MIHR (0.16 ± 0.16 versus 0.15 ± 0.17, p = 0.311). On adjusted regression analysis, higher pre-operative APFT scores and BMI ≥ 30 were independently associated with reduction in post-operative APFT scores. Higher-baseline APFT scores were independently associated with less time on a post-operative profile, whereas higher BMI (≥ 30) and lower rank were independently associated with longer post-operative profile duration. Higher-baseline APFT scores and lower rank were independently associated with shorter time intervals to the first post-operative APFT.
Conclusion
Overall, no differences in post-operative APFT scores, military profile time, or time to first post-operative APFT were observed between minimally invasive or open hernioplasty in this military population.
Similar content being viewed by others
References
Simons MP, Smietanski M, Bonjer HJ et al (2018) International guidelines for groin hernia management. Hernia 22:1–165. https://doi.org/10.1007/s10029-017-1668-x
Stahlman S, Fan M (2020) Incidence of inguinal hernia and repair procedures and rate of subsequent pain diagnoses, active component service members, U.S. Armed Forces, 2010–2019. Msmr 27:11–16
van Veenendaal N, Simons M, Hope W et al (2020) Consensus on international guidelines for management of groin hernias. Surg Endosc 34:2359–2377. https://doi.org/10.1007/s00464-020-07516-5
Fitzgibbons RJ, Giobbie-Hurder A, Gibbs JO et al (2006) Watchful waiting vs repair of inguinal hernia in minimally symptomatic men: a randomized clinical trial. JAMA 295:285–292. https://doi.org/10.1001/JAMA.295.3.285
Khan LR, Liong S, de Beaux AC et al (2010) Lightweight mesh improves functional outcome in laparoscopic totally extra-peritoneal inguinal hernia repair. Hernia 14:39–45. https://doi.org/10.1007/s10029-009-0558-2
Currie A, Andrew H, Tonsi A et al (2012) Lightweight versus heavyweight mesh in laparoscopic inguinal hernia repair: a meta-analysis. Surg Endosc 26:2126–2133. https://doi.org/10.1007/s00464-012-2179-6
Arnold MR, Coakley KM, Fromke EJ et al (2019) Long-term assessment of surgical and quality-of-life outcomes between lightweight and standard (heavyweight) three-dimensional contoured mesh in laparoscopic inguinal hernia repair. Surgery 165:820–824. https://doi.org/10.1016/j.surg.2018.10.016
Bullinger M, Quitmann J (2014) Quality of life as patient-reported outcomes: principles of assessment. Dialogues Clin Neurosci 16(2):137–145
Knapik JJ, East WB. History of United States Army physical fitness and physical readiness training. US Army Med Dep J. 2014 Apr-Jun:5-19. PMID: 24706237
Taylor-Clark TM, Loan LA, Swiger PA et al (2022) Predictors of Temporary Profile Days Among U.S. Army Active Duty Soldiers. Mil Med. https://doi.org/10.1093/milmed/usab558
Army S of the (2020) Army Directive 2020–06 (Army Combat Fitness Test)
Gutlic N, Gutlic A, Petersson U et al (2019) Randomized clinical trial comparing total extraperitoneal with lichtenstein inguinal hernia repair (TEPLICH trial). Brit J Surg 106:845–855. https://doi.org/10.1002/bjs.11230
Köckerling F, Bittner R, Kofler M et al (2019) Lichtenstein versus total extraperitoneal patch plasty versus transabdominal patch plasty technique for primary unilateral inguinal hernia repair. Ann Surg 269:351–357. https://doi.org/10.1097/sla.0000000000002541
LeBlanc K, Dickens E, Gonzalez A et al (2020) Prospective, multicenter, pairwise analysis of robotic-assisted inguinal hernia repair with open and laparoscopic inguinal hernia repair: early results from the prospective hernia study. Hernia 24:1069–1081. https://doi.org/10.1007/s10029-020-02224-4
Prabhu AS, Carbonell A, Hope W et al (2020) Robotic inguinal vs transabdominal laparoscopic inguinal hernia repair. JAMA Surg 155:380–387. https://doi.org/10.1001/JAMAsurg.2020.0034
Tatarian T, Nie L, McPartland C et al (2021) Comparative perioperative and 5-year outcomes of robotic and laparoscopic or open inguinal hernia repair: a study of 153,727 patients in the state of New York. Surg Endosc 35:7209–7218. https://doi.org/10.1007/s00464-020-08211-1
Holleran TJ, Napolitano MA, Sparks AD et al (2021) Trends and outcomes of open, laparoscopic, and robotic inguinal hernia repair in the veterans affairs system. Hernia. https://doi.org/10.1007/s10029-021-02419-3
Abdelmoaty WF, Dunst CM, Neighorn C et al (2019) Robotic-assisted versus laparoscopic unilateral inguinal hernia repair: a comprehensive cost analysis. Surg Endosc 33:3436–3443. https://doi.org/10.1007/s00464-018-06606-9
Schaaf S, Willms A, Schwab R, Güsgen C (2021) Recommendations on postoperative strain and physical labor after abdominal and hernia surgery: an expert survey of attendants of the 41st EHS annual international congress of the European hernia society. Hernia. https://doi.org/10.1007/s10029-021-02377-w
Wood KL, Haider SF, Bui A, Leitman IM (2020) Access to common laparoscopic general surgical procedures: do racial disparities exist? Surg Endosc 34:1376–1386. https://doi.org/10.1007/s00464-019-06912-w
Vu JV, Gunaseelan V, Dimick JB et al (2019) Mechanisms of age and race differences in receiving minimally invasive inguinal hernia repair. Surg Endosc 33:4032–4037. https://doi.org/10.1007/s00464-019-06695-0
Vu JV, Gunaseelan V, Krapohl GL et al (2019) Surgeon utilization of minimally invasive techniques for inguinal hernia repair: a population-based study. Surg Endosc 33:486–493. https://doi.org/10.1007/s00464-018-6322-x
Gram-Hanssen A, Christophersen C, Rosenberg J (2021) Results from patient-reported outcome measures are inconsistently reported in inguinal hernia trials: a systematic review. Hernia. https://doi.org/10.1007/s10029-021-02492-8
Heniford BT, Lincourt AE, Walters AL et al (2018) Carolinas comfort scale as a measure of hernia repair quality of life. Ann Surg 267:171–176. https://doi.org/10.1097/sla.0000000000002027
Forester B, Attaar M, Lach M et al (2021) Inguinal hernia mesh is safe in 1720 patients. Surg Endosc. https://doi.org/10.1007/s00464-021-08442-w
Knox JA, Nelson DA, Latham KP, Kurina LM (2018) Objective effects of breast reduction surgery on physical fitness. Ann Plas Surg 80:14–17. https://doi.org/10.1097/sap.0000000000001167
DeGroot DW, Sitler CA, Lustik MB et al (2021) The effect of pregnancy and the duration of postpartum convalescence on the physical fitness of healthy women: a cohort study of active duty servicewomen receiving 6 weeks versus 12 weeks convalescence. PLoS ONE 16:e0255248. https://doi.org/10.1371/journal.pone.0255248
Balazs LGC, Donohue MMA, Brelin CAM et al (2019) Outcomes of revision arthroscopic anterior shoulder stabilization in a military population: a prospective cohort study. J Surg Orthop Adv 28:189–195
Balazs G, Grimm P, Donohue M et al (2015) Revision anterior cruciate ligament reconstruction in military personnel. J Knee Surg 29:464–470. https://doi.org/10.1055/s-0035-1564725
Chan AG, Balazs GC, Haley CA et al (2019) Pectoralis major rupture in military academy athletes. Orthop J Sports Medicine 7:2325967119860157. https://doi.org/10.1177/2325967119860157
Funding
No funding was obtained for this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflict of interest to declare.
Human and animal rights and Ethical approval
This was a retrospect and de-identified study. No patient consent was obtained nor deemed necessary by our Institutional Review Board. No animals were used for this study.
Informed consent
This was a retrospect and de-identified study. No patient consent was obtained nor deemed necessary by our Institutional Review Board.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Bozzay, J.D., Nelson, D.A., Clifton, D.R. et al. Comparing functional outcomes in minimally invasive versus open inguinal hernia repair using the army physical fitness test. Hernia 27, 105–111 (2023). https://doi.org/10.1007/s10029-022-02650-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10029-022-02650-6