Abstract
Purpose
The outcomes of utilizing anti-adhesive barrier-coated mesh in the retrorectus position during open ventral hernia repair are unknown. We compared the wound-related outcomes between non-coated (NCM) and coated mesh (CM) placed in the retrorectus space.
Methods
Patients undergoing elective, open, clean ventral hernia repair with retrorectus mesh were retrospectively identified in the Americas Hernia Society Quality Collaborative. Propensity score matching was performed based on clinically relevant demographic and operative covariates. The primary outcome was wound morbidity, defined as surgical site infection (SSI), surgical site occurrence (SSO), and SSO requiring procedural intervention (SSOPI).
Results
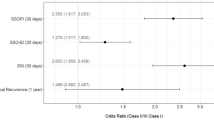
3609 patients were included (3281 NCM, 328 CM). Following 2:1 propensity score matching, rates of myofascial release remained the only statistically different matching parameter; external oblique releases were performed more frequently in the CM group (8% vs. 15%; p = 0.03). Rates of SSI (3% vs. 4%; p = 0.16) were similar between groups. Increased rates of SSO (13% vs. 18%; p = 0.045) and SSOPI (4% vs. 8%; p = 0.038) were observed in the CM group. The CM group had a higher rate of postoperative seroma (3% vs. 7%; p = 0.027) compared to the NCM group.
Conclusion
Barrier-coated mesh in the retrorectus position was associated with increased wound morbidity requiring procedural intervention. Due to a lack of clinical benefit, the use of more costly barrier-coated mesh in the retrorectus position is not justified for routine, open ventral hernia repairs at this time.


Similar content being viewed by others
References
Burger JWA, Luijendijk RW, Hop WCJ et al (2004) Long-term follow-up of a randomized controlled trial of suture versus mesh repair of incisional hernia. Ann Surg 240:578–583. https://doi.org/10.1097/01.sla.0000141193.08524.e7(discussion 583-585)
Nguyen MT, Berger RL, Hicks SC et al (2014) Comparison of outcomes of synthetic mesh vs suture repair of elective primary ventral herniorrhaphy: a systematic review and meta-analysis. JAMA Surg 149:415–421. https://doi.org/10.1001/jamasurg.2013.5014
Mathes T, Walgenbach M, Siegel R (2016) Suture versus mesh repair in primary and incisional ventral hernias: a systematic review and meta-analysis. World J Surg 40:826–835. https://doi.org/10.1007/s00268-015-3311-2
Fafaj A, Petro CC, Tastaldi L et al (2020) Intraperitoneal versus retromuscular mesh placement for open incisional hernias: an analysis of the Americas Hernia Society Quality Collaborative. Br J Surg. https://doi.org/10.1002/bjs.11560
Sosin M, Nahabedian MY, Bhanot P (2018) The perfect plane: a systematic review of mesh location and outcomes, update 2018. Plast Reconstr Surg 142:107S–116S. https://doi.org/10.1097/PRS.0000000000004864
Holihan JL, Nguyen DH, Nguyen MT et al (2016) Mesh location in open ventral hernia repair: a systematic review and network meta-analysis. World J Surg 40:89–99. https://doi.org/10.1007/s00268-015-3252-9
Liang MK, Holihan JL, Itani K et al (2017) Ventral hernia management: expert consensus guided by systematic review. Ann Surg 265:80–89. https://doi.org/10.1097/SLA.0000000000001701
van’t Riet M, de Vos van Steenwijk PJ, Bonthuis F et al (2003) Prevention of adhesion to prosthetic mesh: comparison of different barriers using an incisional hernia model. Ann Surg 237:123–128. https://doi.org/10.1097/00000658-200301000-00017
Pauli EM, Rosen MJ (2013) Open ventral hernia repair with component separation. Surg Clin North Am 93:1111–1133. https://doi.org/10.1016/j.suc.2013.06.010
Kalaba S, Gerhard E, Winder JS et al (2016) Design strategies and applications of biomaterials and devices for hernia repair. Bioact Mater 1:2–17. https://doi.org/10.1016/j.bioactmat.2016.05.002
Zolin SJ, Fafaj A, Krpata DM (2020) Transversus abdominis release (TAR): what are the real indications and where is the limit? Hernia 24:333–340. https://doi.org/10.1007/s10029-020-02150-5
Poulose BK, Roll S, Murphy JW et al (2016) Design and implementation of the Americas Hernia Society Quality Collaborative (AHSQC): improving value in hernia care. Hernia 20:177–189. https://doi.org/10.1007/s10029-016-1477-7
Haskins IN, Horne CM, Krpata DM et al (2018) A call for standardization of wound events reporting following ventral hernia repair. Hernia 22:729–736. https://doi.org/10.1007/s10029-018-1748-6
Surgical Site Infection (SSI) Event. Centers for disease control and prevention. https://www.cdc.gov/nhsn/pdfs/pscmanual/9pscssicurrent.pdf.
Baucom RB, Ousley J, Feurer ID et al (2016) Patient reported outcomes after incisional hernia repair-establishing the ventral hernia recurrence inventory. Am J Surg 212:81–88. https://doi.org/10.1016/j.amjsurg.2015.06.007
Krpata DM, Schmotzer BJ, Flocke S et al (2012) Design and initial implementation of HerQLes: a hernia-related quality-of-life survey to assess abdominal wall function. J Am Coll Surg 215:635–642. https://doi.org/10.1016/j.jamcollsurg.2012.06.412
Kanters AE, Krpata DM, Blatnik JA et al (2012) Modified hernia grading scale to stratify surgical site occurrence after open ventral hernia repairs. J Am Coll Surg 215:787–793. https://doi.org/10.1016/j.jamcollsurg.2012.08.012
Wegdam JA, Thoolen JMM, Nienhuijs SW et al (2019) Systematic review of transversus abdominis release in complex abdominal wall reconstruction. Hernia 23:5–15. https://doi.org/10.1007/s10029-018-1870-5
Albino FP, Patel KM, Nahabedian MY et al (2013) Does mesh location matter in abdominal wall reconstruction? A systematic review of the literature and a summary of recommendations. Plast Reconstr Surg 132:1295–1304. https://doi.org/10.1097/PRS.0b013e3182a4c393
Lehr SC, Schuricht AL (2001) A minimally invasive approach for treating postoperative seromas after incisional hernia repair. JSLS 5:267–271
Hafezi F, Nouhi AH (2002) Abdominoplasty and seroma. Ann Plast Surg 48:109–110. https://doi.org/10.1097/00000637-200201000-00022
Plymale MA, Harris JW, Davenport DL et al (2016) Abdominal wall reconstruction: the uncertainty of the impact of drain duration upon outcomes. Am Surg 82:207–211
Nockolds CL, Hodde JP, Rooney PS (2014) Abdominal wall reconstruction with components separation and mesh reinforcement in complex hernia repair. BMC Surg 14:25. https://doi.org/10.1186/1471-2482-14-25
Aho JM, Nickerson TP, Thiels CA et al (2016) Prevention of postoperative seromas with dead space obliteration. Int J Surg Lond Engl 29:70–73. https://doi.org/10.1016/j.ijsu.2016.03.004
Baroudi R, Ferreira CAA (1998) Seroma: how to avoid it and how to treat it. Aesthet Surg J 18:439–441. https://doi.org/10.1016/S1090-820X(98)70073-1
Brown CN, Finch JG (2010) Which mesh for hernia repair? Ann R Coll Surg Engl 92:272–278. https://doi.org/10.1308/003588410X12664192076296
Salgaonkar H, Lomanto D (2018) Mesh technology—an update. Ann Laparos Endos Surg. https://doi.org/10.21037/ales.2018.09.10
Heller L, McNichols CH, Ramirez OM (2012) Component separations. Semin Plast Surg 26:25–28. https://doi.org/10.1055/s-0032-1302462
de Vries Reilingh TS, van Goor H, Rosman C et al (2003) “Components separation technique” for the repair of large abdominal wall hernias. J Am Coll Surg 196:32–37. https://doi.org/10.1016/s1072-7515(02)01478-3
Krpata DM, Blatnik JA, Novitsky YW, Rosen MJ (2012) Posterior and open anterior components separations: a comparative analysis. Am J Surg 203:318–322. https://doi.org/10.1016/j.amjsurg.2011.10.009(discussion 322)
Lowe JB, Lowe JB, Baty JD, Garza JR (2003) Risks associated with “components separation” for closure of complex abdominal wall defects. Plast Reconstr Surg 111:1276–1283. https://doi.org/10.1097/01.PRS.0000047021.36879.FD(quiz 1284-1285; discussion 1286-1288)
Singhal V, Szeto P, VanderMeer TJ, Cagir B (2012) Ventral hernia repair: outcomes change with long-term follow-up. JSLS 16:373–379. https://doi.org/10.4293/108680812X13427982377067
Guzman MJ, Gitelis ME, Linn JG et al (2015) A model of cost reduction and standardization: improved cost savings while maintaining the quality of care. Dis Colon Rectum 58:1104–1107. https://doi.org/10.1097/DCR.0000000000000463
Krpata DM, Haskins IN, Rosenblatt S et al (2018) Development of a disease-based hernia program and the impact on cost for a hospital system. Ann Surg 267:370–374. https://doi.org/10.1097/SLA.0000000000002093
Funding
The authors report no external funding source for this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
AF declares a resident research grant from the AHSQC that is not related to the submitted work. DMK has received an educational grant from W.L Gore that is not related to the submitted work. ASP has received a research grant from Intuitive Inc. and personal fees from Intuitive Inc. and Medtronic Inc. that are not related to the submitted work. MJR declares to receive salary support from the AHSQC, research grants from Intuitive Inc. and Pacira Pharmaceuticals Inc., and to be a board member and have stock options from Ariste Medical; none of these conflicts of interest are related to the submitted work. All other authors declare no conflicts of interest.
Ethical approval
This study was approved by the Institution Review Board (IRB) at Cleveland Clinic.
Human and animal rights
This study does not contain any studies with participants or animals performed by any of the authors.
Informed consent
For this type of study, formal consent was not required.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Thomas, J.D., Fafaj, A., Zolin, S.J. et al. Non-coated versus coated mesh for retrorectus ventral hernia repair: a propensity score-matched analysis of the Americas Hernia Society Quality Collaborative (AHSQC). Hernia 25, 665–672 (2021). https://doi.org/10.1007/s10029-020-02229-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10029-020-02229-z