Abstract
Background
The incidence of incisional hernia after midline laparotomies ranges from 10 to 20%. The recurrence rate after this hernia surgery varies from 25 to 52% using autogenous tissue. The use of prosthetic meshes can decrease the postoperative hernia recurrence by up to 10%. The aim of this prospective randomized clinical study was to analyze and compare the results of three different incisional hernia surgical techniques.
Materials and methods
One hundred and sixty-one patients who underwent incisional hernia surgery were randomized into three groups. The Keel technique was used in the first group, the “Onlay” technique (prosthetic mesh is fixed on the external abdominal muscle slip) in the second group, and the “Sublay” technique (prosthetic mesh is placed on the posterior abdominal muscle sheath) in the third group. Age, sex, hospitalization time, body mass index (BMI), intraabdominal pressure, postoperative complications, postoperative pain, normal physical activity recovery time, and recurrence rate were compared between the groups. The postoperative follow-up period was 12 months.
Results
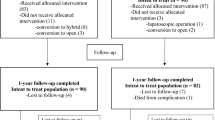
Fifty-four patients in the Keel group, 57 patients in the “Onlay” group, and 50 patients in the “Sublay” group were operated. Age, hospitalization time, and BMI were similar in all of the groups. The operative time was significantly longer in the prosthetic mesh groups compared with the Keel group. The intraabdominal pressure changes before and after surgery was significantly higher in the Keel group compared with the prosthetic mesh groups (5.66 ± 2.5 mmHg vs. 1.88 ± 1 mmHg vs. 1.76 ± 1 mmHg; P < 0.05). The postoperative wound complications rate was significantly higher in the “Onlay” technique group compared with the Keel and “Sublay” technique groups (49.1% vs. 22.2% vs. 24%; P < 0.05). Postoperative pain (VAS score) was significantly lower in the “Onlay” and “Sublay” groups (5.53 ± 1.59 vs. 3.96 ± 1.56 vs. 3.78 ± 1.97; P < 0.05). All of the patients in “Sublay” group recovered to normal physical activity during the 6 months follow-up period compared with 94.4% of patients in the Keel group and 98.3% of patients in the “Onlay” group. The recurrence rate was 22.2% in the Keel group, 10.5% in the “Onlay” group, and 2% in the “Sublay” group during the follow-up period. The general complications rate after hernia surgery was 5.6%. Postoperative pneumonia was the most frequent complication, which appeared in 4.3% of patients. There was no postoperative death in our prospective study.
Conclusions
Mesh repair is the first-choice technique for incisional hernia treatment. The results of the “Sublay” technique are better than the “Onlay” technique.







Similar content being viewed by others
References
Burger JW, van’t Riet M, Jeekel J (2002) Abdominal incisions: techniques and postoperative complications. Scand J Surg 91:315–321
Flum DR, Horvath K, Koepsell T (2003) Have outcomes of incisional hernia repair improved with time? A population-based analysis. Ann Surg 237:129–135
Kurzer M, Kark A, Selouk S, Belsham P (2008) Open mesh repair of incisional hernia using a sublay technique: long-term follow-up. World J Surg 32:31–36
van’t Riet M, Steyerberg EW, Nellensteyn J, Bonjer HJ, Jeekel J (2002) Meta-analysis of techniques for closure of midline abdominal incisions. Br J Surg 89:1350–1356
Cassar K, Munro A (2002) Surgical treatment of incisional hernia. Br J Surg 89:534–545
den Hartog D, Dur AH, Tuinebreijer WE, Kreis RW (2008) Open surgical procedures for incisional hernias. Cochrane Database Syst Rev (3):CD006438
Burger JW, Luijendijk RW, Hop WC, Halm JA, Verdaasdonk EG, Jeekel J (2004) Long-term follow-up of a randomized controlled trial of suture versus mesh repair of incisional hernia. Ann Surg 240:578–583
Luijendijk RW, Hop WC, van den Tol MP, de Lange DC, Braaksma MM, IJzermans JN, Boelhouwer RU, de Vries BC, Salu MK, Wereldsma JC, Bruijninckx CM, Jeekel J (2000) A comparison of suture repair with mesh repair for incisional hernia. N Engl J Med 343:392–398
Paul A, Korenkov M, Peters S, Köhler L, Fischer S, Troidl H (1998) Unacceptable results of the Mayo procedure for repair of abdominal incisional hernias. Eur J Surg 164:361–367
de Vries Reilingh TS, van Geldere D, Langenhorst B, de Jong D, van der Wilt GJ, van Goor H, Bleichrodt RP (2004) Repair of large midline incisional hernias with polypropylene mesh: comparison of three operative techniques. Hernia 8:56–59
Le H, Bender JS (2005) Retrofascial mesh repair of ventral incisional hernias. Am J Surg 189:373–375
Novitsky YW, Porter JR, Rucho ZC, Getz SB, Pratt BL, Kercher KW, Heniford BT (2006) Open preperitoneal retrofascial mesh repair for multiply recurrent ventral incisional hernias. J Am Coll Surg 203:283–289
Bauer JJ, Harris MT, Gorfine SR, Kreel I (2002) Rives–Stoppa procedure for repair of large incisional hernias: experience with 57 patients. Hernia 6:120–123
Iqbal CW, Pham TH, Joseph A, Mai J, Thompson GB, Sarr MG (2007) Long-term outcome of 254 complex incisional hernia repairs using the modified Rives–Stoppa technique. World J Surg 31:2398–2404
Schumpelick V, Klinge U, Junge K, Stumpf M (2004) Incisional abdominal hernia: the open mesh repair. Langenbecks Arch Surg 389:1–5
Korenkov M, Paul A, Sauerland S, Neugebauer E, Arndt M, Chevrel JP, Corcione F, Fingerhut A, Flament JB, Kux M, Matzinger A, Myrvold HE, Rath AM, Simmermacher RK (2001) Classification and surgical treatment of incisional hernia. Results of an experts’ meeting. Langenbecks Arch Surg 386:65–73
Israelsson LA, Smedberg S, Montgomery A, Nordin P, Spangen L (2006) Incisional hernia repair in Sweden 2002. Hernia 10:258–261
Langer C, Liersch T, Kley C, Flosman M, Süss M, Siemer A, Becker H (2003) Twenty-five years of experience in incisional hernia surgery. A comparative retrospective study of 432 incisional hernia repairs. Chirurg 74:638–645
Finan KR, Kilgore ML, Hawn MT (2009) Open suture versus mesh repair of primary incisional hernias: a cost–utility analysis. Hernia 13:173–182
Dur AH, den Hartog D, Tuinebreijer WE, Kreis RW, Lange JF (2009) Low recurrence rate of a two-layered closure repair for primary and recurrent midline incisional hernia without mesh. Hernia 13:421–426
Venclauskas L, Silanskaite J, Kanisauskaite J, Kiudelis M (2007) Long-term results of incisional hernia treatment. Medicina (Kaunas) 43:855–860
Korenkov M, Sauerland S, Arndt M, Bograd L, Neugebauer EA, Troidl H (2002) Randomized clinical trial of suture repair, polypropylene mesh or autodermal hernioplasty for incisional hernia. Br J Surg 89:50–56
Graça Neto L, Araújo LR, Rudy MR, Auersvald LA, Graf R (2006) Intraabdominal pressure in abdominoplasty patients. Aesthetic Plast Surg 30:655–658
Talisman R, Kaplan B, Haik J, Aronov S, Shraga A, Orenstein A (2002) Measuring alterations in intra-abdominal pressure during abdominoplasty as a predictive value for possible postoperative complications. Aesthetic Plast Surg 26:189–192
Cobb WS, Carbonell AM, Kalbaugh CL, Jones Y, Lokey JS (2009) Infection risk of open placement of intraperitoneal composite mesh. Am Surg 75:762–767
Conze J, Kingsnorth AN, Flament JB, Simmermacher R, Arlt G, Langer C, Schippers E, Hartley M, Schumpelick V (2005) Randomized clinical trial comparing lightweight composite mesh with polyester or polypropylene mesh for incisional hernia repair. Br J Surg 92:1488–1493
Schmidbauer S, Ladurner R, Hallfeldt KK, Mussack T (2005) Heavy-weight versus low-weight polypropylene meshes for open sublay mesh repair of incisional hernia. Eur J Med Res 10:247–253
Sørensen LT, Hemmingsen UB, Kirkeby LT, Kallehave F, Jørgensen LN (2005) Smoking is a risk factor for incisional hernia. Arch Surg 140:119–123
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Venclauskas, L., Maleckas, A. & Kiudelis, M. One-year follow-up after incisional hernia treatment: results of a prospective randomized study. Hernia 14, 575–582 (2010). https://doi.org/10.1007/s10029-010-0686-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10029-010-0686-8