Abstract
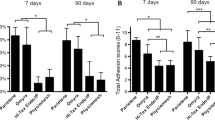
The aim of this study was to compare the effect of different kinds of surgical meshes on postoperative adhesion formation. Forty-two New Zealand White rabbits were studied. The rabbits were grouped into six groups, according to the type of surgical meshes (Prolene, Mersilene, Vypro, polytetraflouroethylene (PTFE), Proceed and control group) implanted into the peritoneum cavity. Thirty days after the operation, the relaparotomies were carried out, and any adhesions observed between the implanted mesh and tissues were evaluated and graded. The mean adhesion degree was 9.2 in the Mersilene mesh group, 9.5 in the Prolene mesh group, 9.7 and in the Vypro mesh group (P > 0.05). The mean adhesion degree was 1 in the control group, 2.75 in the Proceed mesh group and 2.25 in the PTFE mesh group. There was a significant difference in adhesion degree between the control, Proceed and PTFE groups and the Prolene, Mersilene and Vypro mesh groups. The adhesion degree was significantly lower in the Proceed and PTFE mesh groups when comparing them with the Prolene, Mersilene and Vypro meshes.
Similar content being viewed by others
References
Tyrell J, Silberman H, Chandrasoma P, Niland J, Shull J (1989) Absorbable versus permanent mesh in abdominal operations. Surg Gynecol Obstet 168:227–232
Fingerhut A, Oberlin P, Cotte JP, Aziz L, Etienne JC, Vinson-Bonnet B, Aubert JD, Rea S (1992) Splenic salvage using an absorbable mesh: feasibility, reliability and safety. Br J Surg 79:325–327
Ivatury RR, Simon RJ, Guignard J, Kazigo J, Gunduz Y, Stahl WM (1993) The spleen at risk after penetrating trauma. J Trauma 35:409–414
White RA, Ramos SM, Delany HM (1987) Renorrhaphy using knitted polyglycolic acid mesh. J Trauma 27:689–690
Winde G, Reers B, Nottberg H, Berns T, Meyer J, Bunte H (1993) Clinical and functional results of abdominal rectopexy with absorbable mesh graft for treatment of complete rectal prolapse. Eur J Surg 159:301
Barbaxoblou E, Campion JP, Landen S, Manganas D, Siriser F, Chareton B, Launois B (1994) Oesophageal perforation: primary suture repair reinforced with absorbable mesh and fibrin glue. Br J Surg 81:399
Jacobson LE, Kirton OC, Gomez GA (1992) The use of an absorbable mesh wrap in the management of major liver injuries. Surgery 111:455–461
Baltimore H. Peritoneal Adhesiolysis (1994) National inpatient profile 1993. HCIA 427:653–655
Klinge U, Klosterhalfen B, Müller M, Anurov M, Öttinger A, Schumpelick V (1999) Influence of polyglactin-coating on functional and morphological parameters of polypropylene-mesh modifications for abdominal wall repair. Biomaterials 20:613–623
Zieren J, Neuss H, Ablassmaier B, Muller JM (2002) Adhesions after intraperitoneal mesh repair in pigs: Prolene vs. Vypro. J Laparoendosc Adv Surg Tech A 12:249–252
Baykal A, Onat D, Rasa K, Renda N, Sayek I (1997) Effects of polyglycolic acid and polypropylene meshes on postoperative adhesion formation in mice. World J Surg 21:579–582
Vrijland WW, Bonthuis F, Steyerberg EW, Marquet RL, Jeekel J, Bonjer HJ (2000) Peritoneal adhesions to prosthetic materials: choice of mesh for incisional hernia repair. Surg Endosc 14:960–963
Butler CE, Prieto VG (2004) Reduction of adhesions with composite AlloDerm/polypropylene mesh implants for abdominal wall reconstruction. Plast Reconstr Surg 114:464–473
Borrazzo EC, Belmont MF, Boffa D, Fowler DL (2004) Effect of prosthetic material on adhesion formation after laparoscopic ventral hernia repair in a porcine model. Hernia 8:108–112
Matthews BD, Pratt BL, Pollinger HS, Backus CL, Kercher KW, Sing RF, Heniford BT (2003) Assessment of adhesion formation to intra-abdominal polypropylene mesh and polytetrafluoroethylene mesh. J Surg Res 114:126–132
Alimoglu O, Akcakaya A, Sahin M, Unlu Y, Ozkan OV, Sanli E, Eryilmaz R (2003) Prevention of adhesion formations following repair of abdominal wall defects with prosthetic materials (an experimental study). Hepatogastroenterology 50:725–728
van ‘t RM, de Vos van Steenwijk PJ, Bonthuis F, Marquet RL, Steyerberg EW, Jeekel J, Bonjer HJ (2003) Prevention of adhesion to prosthetic mesh: comparison of different barriers using an incisional hernia model. Ann Surg 237:123–128
Altuntas I, Tarhan O, Delibas N (2002) Seprafilm reduces adhesions to polypropylene mesh and increases peritoneal hydroxyproline. Am Surg 68:759–761
Besim H, Yalcin Y, Hamamci O, Arslan K, Sonisik M, Korkmaz A Erdogan S (2002) Prevention of intraabdominal adhesions produced by polypropylene mesh. Eur Surg Res 34:239–243
Kramer K, Senninger N, Herbst H, Probst W (2002) Effective prevention of adhesions with hyaluronate. Arch Surg 137:278–282
Sodji M, Rogier R, Durand-Fontanier S, Lachachi F, Cheynel N, Lombin L, de Laclause BP, Valleix D, Descottes B (2001) [Composite, non-resorbable parietal prosthesis with polyethylene terephtalate-polyurethane (HI-TEX PARP NT): prevention of intraperitoneal adhesions. Experimental study in rabbits]. Ann Chir 126:549–553
Amid PK (2001) Bioabsorbable membrane prevents adhesions to polypropylene in rats. Hernia 5:56
Naim JO, Pulley D, Scanlan K, Hinshaw JR, Lanzafame RJ (1993) Reduction of postoperative adhesions to Marlex mesh using experimental adhesion barriers in rats. J Laparoendosc Surg 3:187–190
LeBlanc KA, Bellanger D, Rhynes KV, Baker DG, Stout RW (2002) Tissue attachment strength of prosthetic meshes used in ventral and incisional hernia repair. A study in the New Zealand White rabbit adhesion model. Surg Endosc 16:1542–1546
LeBlanc KA, Booth WV, Whitaker JM, Baker D (1998) In vivo study of meshes implanted over the inguinal ring and external iliac vessels in uncastrated pigs. Surg Endosc 12:247–251
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kiudelis, M., Jonciauskiene, J., Deduchovas, O. et al. Effects of different kinds of meshes on postoperative adhesion formation in the New Zealand White rabbit. Hernia 11, 19–23 (2007). https://doi.org/10.1007/s10029-006-0139-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10029-006-0139-6