Abstract
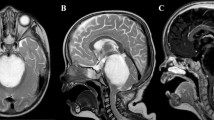
A 55-year-old man was admitted to our hospital complaining of left hemiparesis. Magnetic resonance imaging (MRI) showed a smooth ring-like enhanced cystic tumor in the right parietal lobe. He underwent gross total resection of the tumor under neuronavigation and 5-aminolevulinic acid (5-ALA) fluorescence guiding method. Histopathological examination of the tumor showed small cells formed epithelioid solid nests with some focus of duct-like structure. On the basis of the MRI and operative and histological findings, this tumor was diagnosed as a metastatic poorly differentiated carcinoma, although the primary cancer could not be detected by metastatic work-ups. Afterward, this tumor recurred repeatedly. Histopathological examination of specimen from the fourth surgery indicated that the tumor was a glioblastoma (GBM). In the review of the histology and immunohistochemistry of the first tumor, atypical fibrillary cells were seen between solid nests and positive for glial fibrillary acidic protein, therefore the tumor was retrospectively diagnosed as epithelioid GBM. We assessed whether the changes in histopathology were accompanied by changes in the methylation status of O6-methylguanine methyltransferase (MGMT) promoter and the status of 5-ALA fluorescence. The methylation status of the MGMT promoter was found to have changed from methylated to unmethylated and 5-ALA fluorescence became positive along with the histological change.




Similar content being viewed by others
Abbreviations
- CT:
-
Computed tomography
- MRI:
-
Magnetic resonance imaging
- GBM:
-
Glioblastoma
- 5-ALA:
-
5-Aminolevulinic acid
- PPIX:
-
Protoporphyrin IX
- MGMT:
-
O6-Methylguanine methyltransferase
References
Kepes JJ, Fulling KH, Garcia JH (1982) The clinical significance of “adenoid” formations of neoplastic astrocytes, imitating metastatic carcinoma, in gliosarcomas. A review of five cases. Clin Neuropathol 1:139–150
Akimoto J, Namatame H, Haraoka J et al (2005) Epithelioid glioblastoma: a case report. Brain Tumor Pathol 22:21–27
Miyata S, Sugimoto T, Kodama T et al (2005) Adenoid glioblastoma arising in a patient with neurofibromatosis type-1. Pathol Int 55:348–352
Mork SJ, Rubinstein LJ, Kepes JJ (1988) Patterns of epithelial metaplasia in malignant gliomas. I. Papillary formations mimicking medulloepithelioma. J Neuropathol Exp Neurol 47:93–100
Mork SJ, Rubinstein LJ, Kepes JJ et al (1988) Patterns of epithelial metaplasia in malignantgliomas. II. Squamous differentiation of epithelial-like formations in gliosarcomas and glioblastomas. J Neuropathol Exp Neurol 47:101–118
Shintaku M, Hirano A, Llena JF (1988) Fine structure of glioblastoma multiforme with “adenoid formation”. No Shinkei Geka 16:997–1003
Shintaku M, Nakatsu S, Okamoto S (2000) “Adenoid” glioblastoma. No Shinkei Geka 28:359–365
Rodriguez FJ, Scheithauer BW, Giannini C et al (2008) Epithelial and pseudoepithelial differentiation in glioblastoma and gliosarcoma: a comparative morphologic and molecular genetic study. Cancer 113:2779–2789
Kamide T, Nakada M, Hayashi Y et al (2010) Radiation-induced cerebellar high-grade glioma accompanied by meningioma and cavernoma 29 years after the treatment of medulloblastoma: a case report. J Neurooncol 2010 Mar 31 [Epub ahead of print]
Palmisano WA, Divine KK, Saccomanno G et al (2000) Predicting lung cancer by detecting aberrant promoter methylation in sputum. Cancer Res 60:5954–5958
Yoshida Y, Nakada M, Sugimoto N et al (2010) Sphingosine-1-phosphate receptor type 1 regulates glioma cell proliferation and correlates with patient survival. Int J Cancer 126:2341–2352
Ozolek JA, Finkelstein SD, Couce ME (2004) Gliosarcoma with epithelial differentiation: immunohistochemical and molecular characterization. A case report and review of the literature. Mod Pathol 17:739–745
Balasubramaniam A, Shannon P, Hodaie M et al (2007) Glioblastoma multiforme after stereotactic radiotherapy for acoustic neuroma: case report and review of the literature. Neuro Oncol 9:447–453
Pistollato F, Abbadi S, Rampazzo E et al (2010) Intratumoral hypoxic gradient drives stem cells distribution and MGMT expression in glioblastoma. Stem Cells 28(5):851–862
Singh SK, Hawkins C, Clarke ID et al (2004) Identification of human brain tumour initiating cells. Nature 432:396–401
Zhang M, Song T, Yang L et al (2008) Nestin and CD133: valuable stem cell-specific markers for determining clinical outcome of glioma patients. J Exp Clin Cancer Res 27:85
Strojnik T, Rosland GV, Sakariassen PO et al (2007) Neural stem cell markers, nestin and musashi proteins, in the progression of human glioma: correlation of nestin with prognosis of patient survival. Surg Neurol 68:133–143
Tamura K, Aoyagi M, Wakimoto H et al (2010) Accumulation of CD133-positive glioma cells after high-dose irradiation by gamma knife surgery plus external beam radiation. J Neurosurg 113:310–318
Stupp R, Mason WP, van den Bent MJ et al (2005) Radiotherapy plus concomitant and adjuvant temozolomide for glioblastoma. N Engl J Med 352:987–996
Brandes AA, Franceschi E, Tosoni A et al (2010) O(6)-Methylguanine DNA-methyltransferase methylation status can change between first surgery for newly diagnosed glioblastoma and second surgery for recurrence: clinical implications. Neuro Oncol 12:283–288
Parkinson JF, Wheeler HR, Clarkson A et al (2008) Variation of O(6)-methylguanine-DNA methyltransferase (MGMT) promoter methylation in serial samples in glioblastoma. J Neurooncol 87:71–78
Stummer W, Pichlmeier U, Meinel T et al (2006) Fluorescence-guided surgery with 5-aminolevulinic acid for resection of malignant glioma: a randomised controlled multicentre phase III trial. Lancet Oncol 7:392–401
Stummer W, Novotny A, Stepp H et al (2000) Fluorescence-guided resection of glioblastoma multiforme by using 5-aminolevulinic acid-induced porphyrins: a prospective study in 52 consecutive patients. J Neurosurg 93:1003–1013
Utsuki S, Miyoshi N, Oka H et al (2007) Fluorescence-guided resection of metastatic brain tumors using a 5-aminolevulinic acid-induced protoporphyrin IX: pathological study. Brain Tumor Pathol 24:53–55
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Tanaka, S., Nakada, M., Hayashi, Y. et al. Epithelioid glioblastoma changed to typical glioblastoma: the methylation status of MGMT promoter and 5-ALA fluorescence. Brain Tumor Pathol 28, 59–64 (2011). https://doi.org/10.1007/s10014-010-0009-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10014-010-0009-x