Abstract
Objective
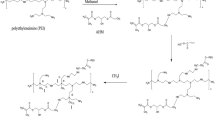
In this study, the developed bioactive dental implant (BDI) from epoxy resin (ER), hydroxyapatite (HA), and curcumin nanoparticles (CUNPs).
Materials and methods
The prepared BDI were characterized using their physicochemical, mechanical, antimicrobial, bioactive, and biocompatibility study. The scanning electron microscopy (SEM) morphology of the BDI was observed HA mineralized crystal layer after being immersed in the stimulated body fluids (SBF) solution.
Results
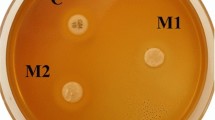
The mechanical properties of the BDI exhibited tensile strength (250.61 ± 0.43 MPa), elongation at break (215.66 ± 0.87%), flexural modulus (03.90 ± 0.12 GPa), water absorption (05.68 ± 0.15%), and water desorption (06.42 ± 0.14%). The antimicrobial activity of BDI was observed in excellent zone of inhibition against the gram-negative (15.33 ± 0.04%) and gram- positive (15.98 ± 0.07%) bacteria. The biocompatibility study of BDI on osteoblasts cell line (MG-63) was analyzed using MTT (3-[4, 5-dimethylthiazol-2-yl]-2,5 diphenyl tetrazolium bromide) assay. The results were observed 85% viable cells present in the BDI compared to the control (only ER) samples.
Conclusions
Based on the research outcome, the BDI could be used for biomaterials application, particularly tooth dental implantation.
Graphical Abstract





Similar content being viewed by others
Data availability
No datasets were generated or analysed during the current study.
References
Atsuomi S, Satoru Y, Keiji T (2022) Network formation and physical properties of Epoxy resins for future practical applications. J Am Chem Soc 2:1522–1542
Pratap B, Gupta RK, Bhardwaj B, Nag M (2019) Resin based restorative dental materials: characteristics and future perspectives. Japan Dent Sci Rev 55:126–138
Viguie G, Malquarti G, Vincent B, Bourgeois D (1994) Epoxy/carbon composite resins in dentistry: mechanical properties related to fiber reinforcement. J Prosthet Dent 72:245–249
Badami V, Ahuja B (2014) Biosmart materials: breaking new ground in dentistry. Sci World J 98:6912
Sodagar A, Bahador A, Pourhajibagher M, Ahmadi B, Baghaeian P (2016) Effect of Addition of Curcumin nanoparticles on Antimicrobial Property and Shear Bond Strength of Orthodontic Composite to bovine enamel. J Dent (Tehran) 13:373–382
Moraes G, Zambom C, Siqueira WL (2021) Nanoparticles in Dentistry: a Comprehensive Review. Pharmaceuticals (Basel) 14:752
Hamilton AE, Gilbert RJ (2023) Curcumin Release from Biomaterials for enhanced tissue regeneration following Injury or Disease. Bioeng 10:262
Yallapu MM, Nagesh PK, Jaggi M, Chauhan SC (2015) Therapeutic applications of Curcumin Nanoformulations. AAPS Pharm Sci 17:1341–1356
Monika N, Shaveta S (2013) Role of curcumin in systemic and oral health: an overview. J Nat Sci Biol Med 4:3–7
Meredith N (1998) Assessment of implant stability as a prognostic determinant. Int J Prosthodont 11:491–501
Andreotti AM, Goiato MC, Nobrega AS, Freitas da Silva EV, Filho HG, Pellizzer EP, Micheline Dos Santos D (2017) Relationship between Implant Stability measurements obtained by two different devices: a systematic review. J Periodontol 88:281–288
Pawar HA, Gavasane AJ, Choudhary PD (2018) A novel and simple Approach for extraction and isolation of Curcuminoids from Turmeric rhizomes. Adv Recycl Waste Manag 6:2
Sandhuli SH, Shashiprabha PD, Asiri ND, Gamini Rajapakse RM (2021) Synthesis of curcumin nanoparticles from raw turmeric rhizome. ACS Omega 6:8246–8252
De Rosa IM, Santulli C, Sarasini F (2010) Mechanical and thermal characterization of epoxy composites reinforced with random and quasi-unidirectional untreated Phormium tenax leaf fibers. Mater Des 31:2397–2405
Reinhart TJ (1990) Engineered materials handbook composites. In: McCarvill William T, Scardino Weldon M, editors. Wet lay-up resins and adhesives specifications, vol. 1. Ohio: ASM International 132–4, 689–701
Basniwal RK, Buttar HS, Jain VK, Jain N (2011) Curcumin nanoparticles: Preparation, characterization, and Antimicrobial Study. J Agri Food Chem 59:2056–2061
Ferraz MP (2004) Hydroxyapatite nanoparticles: a review of preparation methodology. J Appl Biomater Biomech 2:74–80
Albasarah S, Al Abdulghani H, Alaseef N, Al-Qarni FD, Akhtar S, Khan SQ, Ateeq IS, Gad MM (2021) Impact of ZrO2 nanoparticles addition on flexural properties of denture base resin with different thickness. J Adv Prosthodont 13:226–236
Darwish MSA, Mostafa MH, Al-Harbi LM (2022) Polymeric nanocomposites for Environmental and Industrial Applications. Int J Mol Sci 23:1023
Fadilah NIM, Isa ILM, Zaman WSWK, Tabata Y, Fauzi MP (2022) The effect of nanoparticle-incorporated natural-based biomaterials towards cells on activated pathways: a systematic review. Polym 14:476
Zhang Z, Lu W, Tony KFC, Zigui C, Margaret IP, Paul KSC, Joseph JYS, Li Z (2022) Micro-/Nanorobots in antimicrobial applications: recent progress, challenges, and opportunities. Adv Healthc Mater 11:2101991
Pinto RM, Soares FA, Reis S, Nunes C, Van Dijck P (2020) Innovative strategies toward the Disassembly of the EPS Matrix in Bacterial Biofilms. Front Microbiol 11:952
Jerri Al-Bakhsh BA, Shafiei F, Pour Hajibagher M, Shekofteh K, Hashemian A, Behroozi Bakhsh M (2019) The antibacterial activity of an epoxy resin-based dental sealercontaining bioactive glass, hydroxyapatite, and fluorohydroxyapatite nanoparticles against enterococcus faecalis and streptococcus mitis. Nanomed J. ; 6(3)
El-Nashar DE, Rozik NN, Soliman AM, Helaly F (2016) Study the release kinetics of curcumin released from PVA/Curcumin composites and its evaluation towards hepatocarcinoma. J Appl Pharm Sci 6:67–72
Senthil R, Çakır S (2023) Nano apatite growth on demineralized bone matrix capped with curcumin and silver nanoparticles: Dental implant mechanical stability and optimal cell growth analysis. J Oral Biosci. https://doi.org/10.1016/j.job.2023.12.004
Senthil R, Sinem Ç, Batıkan Kavukcu S, Wilson Aruni A (2022) Fabrication of cylindrical bone graft substitute supported by reduced graphene-oxide and nanocurcumin to promotes the bone tissue development. Mater Lett 322:132475
Mondschein RJ, Kanitkar A, Williams CB, Verbridge SS, Long TE (2017) Polymer structure-property requirements for stereolithographic 3D printing of soft tissue engineering scaffolds. Biomater 140:170–188
Leonhardt S, Klare M, Scheer M, Fischer T, Cordes B, Eblenkamp M (2016) Biocompatibility of photopolymers for additive manufacturing. Curr Dir Biomed Eng 2:113–116
Frasheri I, Aumer K, Keßler A, Miosge N, Folwaczny M (2022) Effects of resin materials dedicated for additive manufacturing of temporary dental restorations on human gingival keratinocytes. J Esthet Restor Dent 34:1105–1112
Baqain ZH, Moqbel WY, Sawair FA (2012) Early dental implant failure: risk factors. Br J Oral Maxillofac Surg 50:239–243
Le Guéhennec L, Soueidan A, Layrolle P, Amouriq Y (2007) Surface treatments of titanium dental implants for rapid osseointegration. Dent Mater 23:844–854
Funding
The authors declare that no funds, grants, or other support were received during the preparation of this manuscript.
Author information
Authors and Affiliations
Contributions
Rethinam Senthil – Methodology, Characterization, Formal analysis, writing the original draft, and revision.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethical approval
This article does not contain any studies with human participants or animals performed.
by author.
Clinical trial number in the manuscript
Not Applicable.
Consent to participate
Not Applicable.
Consent to publish
Not Applicable.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Senthil, R. Epoxy resin bioactive dental implant capped with hydroxyapatite and curcumin nanoparticles: a novel approach. Oral Maxillofac Surg (2024). https://doi.org/10.1007/s10006-024-01252-z
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s10006-024-01252-z