Abstract
Purpose
The purpose of this study was to find a suitable anesthetic combination for complicated and protracted minor oral surgical procedures.
Methods
Fifty patients with bilaterally impacted deep-seated mandibular third molars were included in this study and randomly divided on the basis of anesthetic used into two groups. Group A received 2% lignocaine with 1:200,000 adrenaline while in group B, amalgamated mixture of 2% lignocaine and 0.5% bupivacaine was used. The onset time, duration of anesthetic effect, supplementary injections, pain (during local anesthetic deposition, intra and postoperatively), and postoperative analgesia were the study parameters. Chi-square and unpaired t tests were used to compare means.
Results
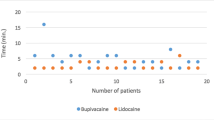
The onset time in both the groups was comparable and showed statistically significant difference between the duration of anesthetic effect with notable requirement of supplemental anesthetic injections in group A (54%) (p < 0.05). Pain scores also revealed a statistically significant intergroup difference (p < 0.05). Requirement of postoperative analgesics was delayed in group B.
Conclusions
The amalgamated mixture of lignocaine and bupivacaine had equivocally rational onset and provided a more profound and in-depth anesthesia especially in complicated and protracted minor oral surgical procedures. Though this mixture is widely used in other surgical fields, its efficacy still remains unexploited and undocumented in oral and maxillofacial surgical procedures.
Similar content being viewed by others
Abbreviations
- CBCT:
-
Cone beam computed tomography
- OPG:
-
Orthopantomogram
- IAN:
-
Inferior alveolar nerve
References
Löfgren N (1948) Studies on local anesthetics: xylocaine: a new synthetic drug (inaugural dissertation). Ivar Heggstroms, Stockholm, Sweden
Malamed S (2008) Pharmacology of local anesthetics. In: Malamed S (ed) handbook of local anesthesia. Fifth edition. Mosby, St Louis, pp 61–65 73, 74
Babst CR, Gilling BN (1978) Bupivacaine: A review. Anesth Prog 25(3):87–91
Brummett CM, Williams BA (2011) Additives to local anesthetics for peripheral nerve blockade. Int Anesthesiol Clin 49(4):104–116. https://doi.org/10.1097/AIA.0b013e31820e4a49
Biradar PA, Kaimar P, Gopalkrishna K (2013) Effect of dexamethasone added to lidocaine in supraclavicular brachial plexus block: a prospective, randomized, double-blind study. Indian J Anaesth 57:180–184
Almajali Z, Batarseh E, Daameh S, Qabha A, Haddadin A (2014) Comparison of postoperative pain relief impact between caudal bupivacaine alone and caudal bupivacaine-dexamethasone mixture Administration for Pediatric Local Tube Urethroplasty. JRMS 21(4):19–24. https://doi.org/10.12816/0008061
Mahmoud MS, Al Alim AA, Hefni AF (2013) Dexamethasone bupivacaine versus bupivacaine for peribulbar block in posterior segment eye surgery. Eg J Anaesth 29(4):407–411. https://doi.org/10.1016/j.egja.2013.07.003
Sisk AL (1992) Long-acting local anesthetics in dentistry. Anesth Prog 39(3):53–60
Oka S, Shimamoto C, Kyoda N, Misaki T (1997) Comparison of lidocaine with and without bupivacaine for local dental anesthesia. Anesth Prog 44(3):83–86
Collins JB, Song J, Mahabir RC (2013) Onset and duration of intradermal mixtures of bupivacaine and lidocaine with epinephrine. Can J Plast Surg 21(1):51–53
Ribotsky BM, Berkowitz KD, Montague JR (1996) Local anesthetics. Is there an advantage to mixing solutions? J Am Podiatr Med Assoc 86(10):487–491. https://doi.org/10.7547/87507315-86-10-487
Özmen Ö, Ahmet Alici H, Çelik M, Dostbil A, Cesur M (2013) The effect of addition of lidocaine to bupivacaine on anesthesia beginning time, block time, and block quality in lateral sagittal Infraclavicular block. Turk J Med Sci 43:542–547
Valvano MN, Leffler S (1996) Comparison of bupivacaine and lidocaine/bupivacaine for local anesthesia/digital nerve block. Ann Emerg Med 27(4):490–492. https://doi.org/10.1016/S0196-0644(96)70239-1
Pederson GW (1988) Surgical removal of tooth. In: Pederson GW (ed) Oral surgery. WB Saunders, Philadelphia, pp 47–81
Maglione M, Costantinides F, Bazzocchi G (2015) Classification of impacted mandibular third molars on cone-beam CT images. J Clin Exp Dent 7(2):224–231
McCaffery M, Pasero C (1999) 0–10 numeric pain rating scale. Pain: clinical manual. Mosby, St. Louis Inc, p 16
Balakrishnan K, Ebenezer V, Dakir A, Kumar S, Prakash D (2015) Bupivacaine versus lignocaine as the choice of local anesthetic agent for impacted third molar surgery a review. J Pharm Bioallied Sci 7(1):230–233
Best CA, Best AA, Best TJ, Hamilton DA (2015) Buffered lidocaine and bupivacaine mixture – the ideal local anesthetic solution? Plast Surg 23(2):87–90
Kouba DJ, LoPiccolo MC, Alam M, Bordeaux JS, Cohen B, Hanke CW et al (2016) Guidelines for the use of local anesthesia in office-based dermatologic surgery. J Am Acad Dermatol 74(6):1201–1219. https://doi.org/10.1016/j.jaad.2016.01.022
Kaukinen S, Kaukinen L, Eerola F (1980) Epidural anaesthesia with mixtures of bupivacaine-lidocaine an etidocaine-lidocaine. Acta Chir Gynaecol 69:281–286
Seow LT, Lips FJ, Cousins MJ, Mather LE (1982) Lidocaine and bupivacaine mixtures for epidural blockade. Anesthesiology 56(3):177–183. https://doi.org/10.1097/00000542-198203000-00004
Kaplan JA, Miller ER, Gallagher EG (1975) Post operative analgesia for thoracotomy patients. Anesthe Analg 54(6):773–777
Oguntoye CO, Adetunji A (2009) Evaluation of lignocaine/bupivacaine mixture for central neural blockade in goats. IJVM 64(4):122–127
Duocaine-FDA prescribing information, side effects and uses.(2009) Duocaine–FDA prescribing information, side effects and uses Amphastar Pharmaceuticals. https://www.drugs.com/pro/duocaine.html [Accessibility verified September 3, 2016]
El-Adawy S, Abd-El Alim A, El-Hamamsy M (2012) Effect of intrathecal bupivacaine–lidocaine combination on motor block and analgesia period. Bull Fac Pharm, Cairo Univ 50:61–65
Mesgarzadeh AH, Afsari H, Pourkhamne S, Shahamfar M (2014) Efficacy of Bilateral Mental Nerve Block with Bupivacaine for Postoperative Pain Control in Mandibular Parasymphysis Fractures. J Dent Res Dent Clin Dent Prospect 8(3):172–175
Chapman PJ, Ganendran A (1987) Prolonged annalgesia following preoperative bupivacaine neural blockade for oral surgery performed under general anesthesia. J Oral Maxillofac Surg 45(3):233–235. https://doi.org/10.1016/0278-2391(87)90120-0
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Dr. Akshay Mishra, Dr. Monica Mahajan, Dr. C. R. Bande, Dr. Ajit Joshi Dr. Mayur Gawande, and Dr. M. K. Gupta declare that they have no conflict of interest.
Patient informed consent
Informed consent was taken from all the participants who agreed to be a part of this study.
Ethical approval
Ethical approval was given by Institutional Research and Ethical Committee (Institutional Review Board). All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Additional information
DRUGS
- LOX 2% adrenaline 1: 200,000 (lignocaine hydrochloride and adrenaline bitartrate injection I.P. manufactured by Neon Laboratories Limited; 28 Mahal Ind. Est., M. Caves Road, Andheri (East), Mumbai-400093)
- LOX 2% (lignocaine hydrochloride injection I.P. manufactured by Neon Laboratories Limited; 28 Mahal Ind. Est., M. Caves Road, Andheri (East), Mumbai-400093)
- ANAWIN 0.5% (bupivacaine hydrochloride injection I.P. manufactured by Neon Laboratories Limited; 28 Mahal Ind. Est., M. Caves Road, Andheri (East), Mumbai-400093)
Rights and permissions
About this article
Cite this article
Mishra, A., Mahajan, M., Bande, C. et al. Is amalgamated ligno-bupivacaine an answer to complicated minor oral surgical anesthesia? A randomized split-mouth double-blind clinical trial. Oral Maxillofac Surg 22, 97–104 (2018). https://doi.org/10.1007/s10006-018-0676-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10006-018-0676-z