Abstract
Objective
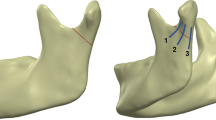
This study aimed to evaluate the resistance of four fixation techniques used to treat subcondylar fractures. The following techniques were evaluated: fixation with one 4-hole single straight plate; fixation with one 2-mm 4-hole system plate and one 1.5-mm 3-hole system plate; fixation with two 2-mm plates with a 3-hole anterior plate; and fixation with two 2-mm plates with four holes each.
Study design
Each fixation technique was subjected to a resistance test. The load values were measured when displacement of 1, 2, and 5 mm was reached. Load values were compared for statistically significant differences using analysis of variance (ANOVA; p < 0.5) and Tukey’s test.
Results
Statistically significant differences were observed, when the load was applied to the first molar on the side of the fracture. The group treated with a 4-hole, 2-mm, one plate system showed resistance to lower load values than the groups treated with two plates in any combination.
Conclusions
When the fracture was fixed using two plates, regardless of the kind of plates used, no statistically significant difference between the groups was observed. However, two plate systems showed better resistance than one plate systems.






Similar content being viewed by others
References
Asprino L, Consani S, De Moraes M (2006) A comparative biomechanical evaluation of mandibular fracture plating techniques. J Oral Maxillofac Surg 64(3):452–456. https://doi.org/10.1016/j.joms.2005.11.017
Chrcanovic BR (2015) Surgical versus non-surgical treatment of mandibular condylar fractures: a meta-analysis. Int J Oral Maxillofac Surg 44(2):158–179. https://doi.org/10.1016/j.ijom.2014.09.024
Chen CT, Feng CH, Tsay PK, Lai JP, Chen YR (2011) Functional outcomes following surgical treatment of bilateral mandibular condylar fractures. Int J Oral Maxillofac Surg 40(1):38–44. https://doi.org/10.1016/j.ijom.2010.09.002
Ehrenfeld M, Manson PN (2012) Prein J. Thieme, Principles of Internal Fixation of the Craniomaxillofacial Skeleton Trauma and Orthognathic Surgery
Abdel-Galil K, Loukota R (2010) Review: Fractures of the mandibular condyle: evidence base and current concepts management. Br J Oral Maxillofac Surg 48:520–526
Al-Moraissi EA, Ellis E III (2015) Surgical treatment of adult mandibular condylar fractures provides better outcomes than closed treatment: a systematic review and meta-analysis. J Oral Maxillofac Surg 73(3):482–493. https://doi.org/10.1016/j.joms.2014.09.027
Neff A, Chossegros C, Blanc J, Chanpsaur P, Cheynet F, Devauchelle B, Eckelt U, Ferri J, Gabrielli MFR, Guyot L, Koppel DA, Meyer C, Muller B, Peltomaki T, Spallacia F, Varoquaux A, Wilk A, Pitak-Arnnop P (2014) Position paper from the IBRA symposium on surgery of the head-the 2nd international Simposium for condylar fracture Osteosynthesis, Marseille, France 2012. J Craniomaxillofac Surg 42(7):1234–1249. https://doi.org/10.1016/j.jcms.2014.03.005
Bredbenner TL, Haug RH (2000) Substitutes for human cadaveric bone in maxillofac rigid fixation research. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 90(5):574–580. https://doi.org/10.1067/moe.2000.111025
Montazem AH, Anastassov G (2009) Management of Condylar Fractures. Atlas Oral Maxillofacial Surg Clin N Am 17(1):55–69. https://doi.org/10.1016/j.cxom.2008.11.002
Hammer B, Schier P, Prein J (1997) Osteosynthesis of condylar neck fractures: a review of 30 patients. Br J Oral Maxillofac Surg 35(4):288–295. https://doi.org/10.1016/S0266-4356(97)90050-4
Lindhal L (1977) Condylar fractures of the mandible. I. Classification and relation to age, occlusion and concomitant injuries in the teeth and teeth-supporting structures and fractures of the mandibular body. Int J Oral Surg 6:12–21
Haug RH, Hevtvedt AK, Michaels GC, Beals DW (1994) Comparison of the resistance of miniplates and micropaltes to various in vitro forces [discussion]. J Oral Maxillofac Surg 52:257–258
Ziccardi VB, Schneider RE, Kummer FJ (1997) Wurzburg lag screw plate versus four-hole minipalte for the treatment of condylar process fractures. J Oral Maxillofac Surg 55(6):602–607. https://doi.org/10.1016/S0278-2391(97)90492-4
Rozema FR, Otten E, Bos RRM, Boering G, Van Willigen JD (1992) Computer aided optimization of choice and positioning of bone plates and screws used for internal fixation of mandibular fractures. Int J Oral Maxillofac Surg 21(6):373–377. https://doi.org/10.1016/S0901-5027(05)80766-0
Rudderman RH, Mullen RL (1992) Biomechanics of the facial skeleton. Clin Plast Surg 19:11–29
Throckmorton GS, Dechow PC (1994) In vitro strain measurements in the condykar process of the human mandible. Arch Oral Biol 39(10):853–867. https://doi.org/10.1016/0003-9969(94)90017-5
Parascandolo S, Spinza A, Parascandolo S, Piombino P, Califano L (2010) Two load sharing plates in mandibular condylar fractures: biomechanical basis. J Craniomaxillofac 38(5):385–390. https://doi.org/10.1016/j.jcms.2009.10.014
Haug RH, Peterson GP, Goltz M (2002) A biomechanical evaluation of mandibular condyle fracture plating techniques. J Oral Maxillofac Surg 60:71–80
Choi BH, Yi CK, Yoo JH (2001) Clinical evaluation of 3 types of plate osteosynthesis for fixation of condylar neck fractures. J Oral Maxillofac Surg 59(7):734–737. https://doi.org/10.1053/joms.2001.24283
Tominaga K, Habu M, Khanal A, Mimori Y, Yoshioka I, Fukuda J (2006) Biomechanical evaluation of different types of rigid internal fixation techniques for subcondylar fractures. J Oral Maxillofac Surg 64(10):1510–1516. https://doi.org/10.1016/j.joms.2006.03.038
Hakim SG, Wolf M, Wendlandt R, Kimmerle H, Sieg P, Jacobsen H (2014) Comparative biomechanical study on three miniplates osteosynthesis system for stabilization of low condylar fractures of the mandible. Br J Oral Maxillofac Surg 52(4):317–322. https://doi.org/10.1016/j.bjoms.2014.02.002
Throckmorton GS, Dechow PC (1994) In vitro strain measurements in the condylar process of the human mandible. Arch Oral Biol 39(10):853–867. https://doi.org/10.1016/0003-9969(94)90017-5
Meyer C, Kahn JL, Boutemi P, Wilk A (2002) Photoelastic analysis of bone deformation in the region of the mandibular condyle during mastication. J Cranio Maxillofac 30(3):160–169. https://doi.org/10.1054/jcms.2002.0297
Darwich MA, Albogha MH, Abdelmajeed A, Darwich K (2016) Assessment of the Biomechanical Performance of 5 Plating Techniques in Fixation of Mandibular Subcondylar Fracture Using Finite Element Analysis. J Oral Maxillofac Surg 1.e1–1.e8
Wagner A, Krach W, Undt G, Ploder O, Ewers R (2002) A 3-dimensional finite-element analysis investigating the biomechanical behavior of the mandible and plate osteosynthesis in cases of fractures of the condylar process. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 94:678–686
Funding sources
Capes (Coordenação de Aperfeiçoamento de Pessoal de Nível Superior).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Cavalieri-Pereira, L., Spagnol, G., Sverzut, C.E. et al. Resistance of four fixation techniques used to treat subcondylar fractures. Oral Maxillofac Surg 22, 91–96 (2018). https://doi.org/10.1007/s10006-018-0675-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10006-018-0675-0