Abstract
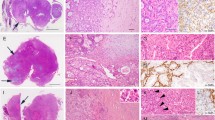
Ghost cell is one of several unique cellular morphologies associated with aberrant keratinization. We encountered a novel parotid tumor containing numerous ghost cells and herein describe its histological features and discuss diagnostic problems. The patient was a 90-year-old Japanese male, who complained of swelling of the left parotid area for four months. Positron emission tomography indicated no cervical lymph node metastasis or distant metastasis. The tumor was successfully resected with no signs of recurrence or metastasis for six months after surgery. Histologically, the tumor was mainly composed of squamous cells forming irregularly shaped nests with a mixture of pleomorphic giant or multinucleated cells and bland basaloid cell. Keratinized areas were occupied by a prominent ghost cell population. Immunohistochemically, CK5/6 and CK19 were widely positive as well as AE1/AE3, p40 and p63. Nuclear expression of β-catenin was also observed. The present case can be regarded as a particular form of squamous cell carcinoma and is believed to contain a large number of ghost cells resulting from an unclear mechanism. However, it seems difficult to consider such tumors as a clinicopathologically independent entity at present. Applying a term such as “salivary ghost cell carcinoma” would be premature.




Similar content being viewed by others
References
Rajesh E, Jimson S, Masthan KM, Balachander N (2015) Ghost cell lesions. J Pharm Bioallied Sci 7:S142-144. https://doi.org/10.4103/0975-7406.155864
Del Corso G, Tardio ML, Gissi DB, Marchetti C, Montebugnoli L, Tarsitano A (2015) Ki-67 and p53 expression in ghost cell odontogenic carcinoma: a case report and literature review. Oral Maxillofac Surg 19:85–89
Lee SK, Kim YS (2014) Current concepts and occurrence of epithelial odontogenic tumors: II. Calcifying epithelial odontogenic tumor versus ghost cell odontogenic tumors derived from calcifying odontogenic cyst. Korean J Pathol 48:175–187. https://doi.org/10.4132/KoreanJPathol.2014.48.3.175
Ihrler S, Mollenhauer M, Weitmayr B, Haas CJ (2020) Salivary ghost cell carcinoma: case report and proposal of a new entity. Virchows Arch 476:465–468. https://doi.org/10.1007/s00428-019-02657-y
Sato K, Akiba J, Nakamura K, Abe H, Kawahara A, Aso T, Umeno H, Harada H, Yano H (2017) Mucoepidermoid carcinoma of the sublingual gland harboring a translocation of the MAML2 gene: a case report. Oncol Lett 14:2970–2974. https://doi.org/10.3892/ol.2017.6550
Grodjesk JE, Dolinsky HB, Schneider LC, Dolinsky EH, Doyle JL (1987) Odontogenic ghost cell carcinoma. Oral Surg Oral Med Oral Pathol 63:576–581
Alcalde RE, Sasaki A, Misaki M, Matsumura T (1996) Odontogenic ghost cell carcinoma: report of a case and review of the literature. J Oral Maxillofac Surg 54:108–111
Folpe AL, Tsue T, Rogerson L, Weymuller E, Oda D, True LD (1998) Odontogenic ghost cell carcinoma: a case report with immunohistochemical and ultrastructural characterization. J Oral Pathol Med 27:185–189. https://doi.org/10.1111/j.1600-0714.1998.tb01938.x
Lu Y, Mock D, Takata T, Jordan RC (1999) Odontogenic ghost cell carcinoma: Report of four new cases and review of the literature. J Oral Pathol Med 28:323–329
Kim J, Lee EH, Yook JI, Han JY, Yoon JH, Ellis GL (2000) Odontogenic ghost cell carcinoma: a case report with reference to the relation between apoptosis and ghost cells. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 90:630–635
Richardson MS, Muller S (2014) Malignant odontogenic tumors: an update on selected tumors. Head Neck Pathol 8:411–420. https://doi.org/10.1007/s12105-014-0584-y
Vijayakumar G, Kamboj M, Narwal A, Devi A (2021) Ghost cell odontogenic carcinoma of anterior mandible: a rare case report with review of literature. J Oral Maxillofac Pathol 25:S99–S108. https://doi.org/10.4103/jomfp.JOMFP_195_20
Motosugi U, Ogawa I, Yoda T, Abe T, Sugasawa M, Murata S, Yasuda M, Sakurai T, Shimizu Y, Shimizu M (2009) Ghost cell odontogenic carcinoma arising in calcifying odontogenic cyst. Ann Diagn Pathol 13:394–397. https://doi.org/10.1016/j.anndiagpath.2009.02.008
Arashiyama T, Kodama Y, Kobayashi T, Hoshina H, Takagi R, Hayashi T, Cheng J, Saku T (2012) Ghost cell odontogenic carcinoma arising in the background of a benign calcifying cystic odontogenic tumor of the mandible. Oral Surg Oral Med Oral Pathol Oral Radiol 114:e35–40
Zhu ZY, Chu ZG, Chen Y, Zhang WP, Lv D, Geng N, Yang MZ (2012) Ghost cell odontogenic carcinoma arising from calcifying cystic odontogenic tumor: a case report. Korean J Pathol 46:478–482
Nel C, Robinson L, van Heerden WFP (2020) Ghost cell odontogenic carcinoma arising in the background of a calcifying odontogenic cyst. Oral Radiol. https://doi.org/10.1007/s11282-020-00492-5
Li BB, Gao Y (2009) Ghost cell odontogenic carcinoma transformed from a dentinogenic ghost cell tumor of maxilla after multiple recurrences. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 107:691–695. https://doi.org/10.1016/j.tripleo.2009.01.008
Miwako S, Hiroto I, Takahumi N, Junichi H, Tadahide N, Yoshinori J et al (2017) Ghost cell odontogenic carcinoma transformed from dentinogenic ghost cell tumor of the maxilla after recurrences. J Oral Maxillofac Surg Med Pathol 29:438–442
Sekine S, Sato S, Takata T, Fukuda Y, Ishida T, Kishino M, Shibata T, Kanai Y, Hirohashi S (2003) Beta-catenin mutations are frequent in calcifying odontogenic cysts, but rare in ameloblastomas. Am J Pathol 163:1707–1712. https://doi.org/10.1016/s0002-9440(10)63528-6
Dutra SN, Pires FR, Armada L, Azevedo RS (2017) Immunoexpression of Wnt/β-catenin signaling pathway proteins in ameloblastoma and calcifying cystic odontogenic tumor. J Clin Exp Dent 9:e136–e140. https://doi.org/10.4317/jced.53100
Kawahara A, Harada H, Abe H, Yamaguchi T, Taira T, Nakashima K, Mihashi H, Akiba J, Kage M (2011) Nuclear β-catenin expression in basal cell adenomas of salivary gland. J Oral Pathol Med 40:460–466. https://doi.org/10.1111/j.1600-0714.2011.01010.x
Jo VY, Sholl LM, Krane JF (2016) Distinctive patterns of CTNNB1 (β-Catenin) alterations in salivary gland basal cell adenoma and basal cell adenocarcinoma. Am J Surg Pathol 40:1143–1150. https://doi.org/10.1097/PAS.0000000000000669
Eversole LR, Rovin S, Sabes WR (1972) Mucoepidermoid carcinoma of minor salivary glands: report of 17 cases with follow-up. J Oral Surg 30:107–112
Ide F, Ito Y, Nishimura M, Kikuchi K, Kusama K (2020) Ghost/shadow cell differentiation in salivary gland tumors. Virchows Arch 477:609–610. https://doi.org/10.1007/s00428-020-02749-0
Ihrler S, Mollenhauer M, Weitmayr B, Haas CJ (2020) Response to the commentary of Ide et al. “Ghost/shadow cell differentiation in salivary gland tumors”. Virchows Arch 477:611. https://doi.org/10.1007/s00428-020-02784-x
Rumayor A, Carlos R, Kirsch HM, de Andrade BA, Romañach MJ, de Almeida OP (2015) Ghost cells in pilomatrixoma, craniopharyngioma, and calcifying cystic odontogenic tumor histological, immunohistochemical, and ultrastructural study. J Oral Pathol Med 44:284–290. https://doi.org/10.1111/jop.12234
Kikuchi K, Ito S, Inoue H, González-Alva P, Miyazaki Y, Sakashita H, Yoshino A, Katayama Y, Terui T, Ide F, Kusama K (2012) Immunohistochemical expression of podoplanin in so-called hard α-keratin-expressing tumors, including calcifying cystic odontogenic tumor, craniopharyngioma, and pilomatrixoma. J Oral Sci 54:165–175. https://doi.org/10.2334/josnusd.54.165
Antonescu CR, Katabi N, Zhang L, Sung YS, Seethala RR, Jordan RC, Perez-Ordoñez B, Have C, Asa SL, Leong IT, Bradley G, Klieb H, Weinreb I (2011) EWSR1-ATF1 fusion is a novel and consistent finding in hyalinizing clear-cell carcinoma of salivary gland. Genes Chromosomes Cancer 50:559–570. https://doi.org/10.1002/gcc.20881
Dardick I, Leong I (2009) Clear cell carcinoma: review of its histomorphogenesis and classification as a squamous cell lesion. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 108:399–405. https://doi.org/10.1016/j.tripleo.2009.03.033
Harada H, Toyozumi Y, Sasaguri T, Kuyama K, Nakatsuka SI, Kurose A (2021) Sclerosing mucoepidermoid carcinoma of the salivary glands: report of three cases with special concern to the counterpart accompanied by eosinophilia. Med Mol Morphol. https://doi.org/10.1007/s00795-021-00285-7 (Epub ahead of print)
Harada H, Matsumoto H, Nakatsuka SI, Kurose A (2021) Lymphoepithelial carcinoma of the parotid gland: a unique example showing p16 immunoreactivity. Med Mol Morphol. https://doi.org/10.1007/s00795-021-00295-5 (Epub ahead of print)
Candido GA, Viana KA, Watanabe S, Vencio EF (2009) Peripheral dentinogenic ghost cell tumor: a case report and review of the literature. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 108:e86-90. https://doi.org/10.1016/j.tripleo.2009.04.033
da Silva Barros CC, de Souto Medeiros MR, de Azevedo RA, da Costa Miguel MC, Dos Santos JN, da Silveira ÉJD (2021) Peripheral dentinogenic ghost cell tumor-report of two cases and review of the literature. Oral Maxillofac Surg. https://doi.org/10.1007/s10006-021-00947-x (Epub ahead of print)
Alwaheeb S, Rambaldini G, Boerner S, Coiré C, Fiser J, Asa SL (2006) Worrisome histologic alterations following fine-needle aspiration of the parathyroid. J Clin Pathol 59:1094–1096
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflicts of interest to declare.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Note: In addition to being a research fellow at Hirosaki University Graduate School of Medicine, the primary author (HH) is also a visiting staff pathologist at Kindai University Hospital.
Rights and permissions
About this article
Cite this article
Harada, H., Sato, M.P., Otsuki, N. et al. A novel parotid carcinoma with a prominent ghost cell population: a masquerading tumor or “salivary ghost cell carcinoma”?. Med Mol Morphol 55, 76–83 (2022). https://doi.org/10.1007/s00795-021-00302-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00795-021-00302-9