Abstract
Objectives
The objectives of this study included using the cone beam computed tomography (CBCT) technology to assess: (1) intra- and inter-observer reliability of the volume measurement of the nasal cavity; (2) the accuracy of the segmentation protocol for evaluation of the nasal cavity.
Materials and methods
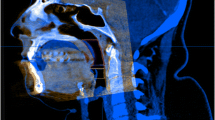
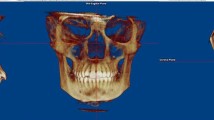
This study used test–retest reliability and accuracy methods within two different population sample groups, from Eastern Asia and North America. Thirty obstructive sleep apnea (OSA) patients were randomly selected from administrative and research oral health data archived at two dental faculties in China and Canada. To assess the reliability of the protocol, two observers performed nasal cavity volume measurement twice with a 10-day interval, using Amira software (v4.1, Visage Imaging Inc., Carlsbad, CA). The accuracy study used a computerized tomography (CT) scan of an OSA patient, who was not included in the study sample, to fabricate an anthropomorphic phantom of the nasal cavity volume with known dimensions (18.9 ml, gold standard). This phantom was scanned using one NewTom 5G (QR systems, Verona, Italy) CBCT scanner. The nasal cavity was segmented based on CBCT images and converted into standard tessellation language (STL) models. The volume of the nasal cavity was measured on the acquired STL models (18.99 ± 0.066 ml).
Results
The intra-observer and inter-observer intraclass correlation coefficients for the volume measurement of the nasal cavity were 0.980–0.997 and 0.948–0.992 consecutively. The nasal cavity volume measurement was overestimated by 1.1%-3.1%, compared to the gold standard.
Conclusions
The semi-automatic segmentation protocol of the nasal cavity in patients with sleep apnea and by using cone beam computed tomography is reliable and accurate.
Clinical relevance
This study provides a reliable and accurate protocol for segmentation of nasal cavity, which will facilitate the clinician to analyze the images within nasoethmoidal region.




Similar content being viewed by others
Data Availability
The datasets generated and/or analyzed during the current study are available from the corresponding author upon reasonable request.
References
Patel RG (2017) Nasal anatomy and function. Facial Plast Surg 33(1):3–8. https://doi.org/10.1055/s-0036-1597950
Tingelhoff K, Moral AI, Kunkel ME, Rilk M, Wagner I, Eichhorn KG, Wahl FM, Bootz F (2007) Comparison between manual and semi-automatic segmentation of nasal cavity and paranasal sinuses from CT images. Conf Proceed: Annu Int Conf IEEE Eng Med Biol Soc. Annual Conference 2007:5505–8. https://doi.org/10.1109/iembs.2007.4353592
Lofaso F, Coste A, d’Ortho MP, Zerah-Lancner F, Delclaux C, Goldenberg F, Harf A (2000) Nasal obstruction as a risk factor for sleep apnoea syndrome. Eur Respir J 16(4):639–643
McNicholas WT (2008) The nose and OSA: variable nasal obstruction may be more important in pathophysiology than fixed obstruction. European Respir J 32(1):3–8. https://doi.org/10.1183/09031936.00050208
Kohler M, Bloch KE, Stradling JR (2007) The role of the nose in the pathogenesis of obstructive sleep apnoea and snoring. Eur Respir J 30(6):1208–15. https://doi.org/10.1183/09031936.00032007
Sériès F, St Pierre S, Carrier G (1993) Surgical correction of nasal obstruction in the treatment of mild sleep apnoea: importance of cephalometry in predicting outcome. Thorax 48(4):360–3. https://doi.org/10.1136/thx.48.4.360
Pang KP (2013) The role of nasal surgery in the treatment of OSA. Curr Otorhinolaryngol Rep 1(1):20–4. https://doi.org/10.1007/s40136-012-0007-0
Hoel HC, Kvinnesland K, Berg S (2020) Impact of nasal resistance on the distribution of apneas and hypopneas in obstructive sleep apnea. Sleep Med 71:83–8. https://doi.org/10.1016/j.sleep.2020.03.024
Parks ET (2014) Cone beam computed tomography for the nasal cavity and paranasal sinuses. Dent Clin North Am 58(3):627–51. https://doi.org/10.1016/j.cden.2014.04.003
Keeler JA, Patki A, Woodard CR, Frank-Ito DO (2016) A computational study of nasal spray deposition pattern in four ethnic groups. J Aerosol Med Pulm Drug Deliv 29(2):153–66. https://doi.org/10.1089/jamp.2014.1205
Niu X, Madhan S, Cornelis MA, Cattaneo PM (2021) Novel three-dimensional methods to analyze the morphology of the nasal cavity and pharyngeal airway. Angle Orthod 91(3):320–8. https://doi.org/10.2319/070620-610.1
Guijarro-Martínez R, Swennen GR (2011) Cone-beam computerized tomography imaging and analysis of the upper airway: a systematic review of the literature. Int J Oral Maxillofac Surg 40(11):1227–37. https://doi.org/10.1016/j.ijom.2011.06.017
Dawood A, Patel S, Brown J (2009) Cone beam CT in dental practice. Br Dent J 207:23. https://doi.org/10.1038/sj.bdj.2009.560
Tsolakis IA, Kolokitha OE, Papadopoulou E, Tsolakis AI, Kilipiris EG, Palomo JM (2022) Artificial intelligence as an aid in CBCT airway analysis: a systematic review. Life (Basel) 12(11):1894. https://doi.org/10.3390/life12111894
Maken P, Gupta A, Gupta MK (2023) A systematic review of the techniques for automatic segmentation of the human upper airway using volumetric images. Med Biol Eng Comput 61(8):1901–27. https://doi.org/10.1007/s11517-023-02842-x
Shujaat S, Jazil O, Willems H, Van Gerven A, Shaheen E, Politis C et al (2021) Automatic segmentation of the pharyngeal airway space with convolutional neural network. J Dent 111:103705. https://doi.org/10.1016/j.jdent.2021.103705
de Bataille C, Bernard D, Dumoncel J, Vaysse F, Cussat-Blanc S, Telmon N et al (2022) Machine learning analysis of the anatomical parameters of the upper airway morphology: a retrospective study from cone-beam CT examinations in a French population. J Clin Med 12(1):84. https://doi.org/10.3390/jcm12010084
Alsufyani NA, Hess A, Noga M, Ray N, Al-Saleh MAQ, Lagravère MO, Major PW (2016) New algorithm for semiautomatic segmentation of nasal cavity and pharyngeal airway in comparison with manual segmentation using cone-beam computed tomography. Am J Orthod Dentofacial Orthop 150(4):703–712. https://doi.org/10.1016/j.ajodo.2016.06.024
Bui NL, Ong SH, Foong KWC (2015) Automatic segmentation of the nasal cavity and paranasal sinuses from cone-beam CT images. Int J CARS 10(8):1269–77. https://doi.org/10.1007/s11548-014-1134-5
Sin Ç, Akkaya N, Aksoy S, Orhan K, Öz U (2021) A deep learning algorithm proposal to automatic pharyngeal airway detection and segmentation on CBCT images. Orthod Craniofac Res 24(Suppl 2):117–23. https://doi.org/10.1111/ocr.12480
Keustermans W, Huysmans T, Schmelzer B, Sijbers J, Dirckx JJ (2019) Matlab(®) toolbox for semi-automatic segmentation of the human nasal cavity based on active shape modeling. Comput Biol Med 105:27–38. https://doi.org/10.1016/j.compbiomed.2018.12.008
Chen H, van Eijnatten M, Wolff J, de Lange J, van der Stelt PF, Lobbezoo F, Aarab G (2017) Reliability and accuracy of three imaging software packages used for 3D analysis of the upper airway on cone beam computed tomography images. Dentomaxillofac Radiol 46(6):20170043. https://doi.org/10.1259/dmfr.20170043
Emami E, Lavigne G, Feine JS, Karp I, Rompré PH, Almeida FR, Huynh NT (2021) Effects of nocturnal wearing of dentures on the quality of sleep and oral-health-related quality in edentate elders with untreated sleep apnea: a randomized cross-over trial. Sleep 44(10):zsab101. https://doi.org/10.1093/sleep/zsab101
Shi X, Chen H, Lobbezoo F, de Lange J, van der Stelt P, Berkhout E et al (2023) Comparison of the upper airway morphology between Dutch and Chinese adults with obstructive sleep apnea. Sleep Breath. https://doi.org/10.1007/s11325-023-02834-z
Weissheimer A, Menezes LM, Sameshima GT, Enciso R, Pham J, Grauer D (2012) Imaging software accuracy for 3-dimensional analysis of the upper airway. Am J Orthod Dentofacial Orthop 142(6):801–13. https://doi.org/10.1016/j.ajodo.2012.07.015
Walter SDEM, Donner A (1998) Sample size and optimal designs for reliability studies. Stat Med 17:101–110. https://doi.org/10.1002/(sici)1097-0258(19980115)17:1%3c101::aid-sim727%3e3.0.co;2-e
Chen H, Aarab G, Parsa A, de Lange J, van der Stelt PF, Lobbezoo F (2016) Reliability of three-dimensional measurements of the upper airway on cone beam computed tomography images. Oral Surg Oral Med Oral Pathol Oral Radiol 122(1):104–10. https://doi.org/10.1016/j.oooo.2016.04.005
Venkatesh E, Elluru SV (2017) Cone beam computed tomography: basics and applications in dentistry. J Istanb Univ Fac Dent 51(3 Suppl 1):S102-s21. https://doi.org/10.17096/jiufd.00289
von Arx T, Lozanoff S, Bornstein MM (2019) Extraoral anatomy in CBCT - a literature review. Part 1: Nasoethmoidal region. Swiss Dent J 129(10):804–15
Cai Y, Goldberg AN, Chang JL (2020) The nose and nasal breathing in sleep apnea. Otolaryngol Clin North Am 53(3):385–95. https://doi.org/10.1016/j.otc.2020.02.002
Mekhitarian Neto L, Fava AS, Lopes HC, Stamm A (2005) Epidemiological analysis of structural alterations of the nasal cavity associated with obstructive sleep apnea syndrome (OSA). Braz J Otorhinolaryngol 71(4):464–6. https://doi.org/10.1016/s1808-8694(15)31200-3
Hafezeqoran A, Rahbar M, Koodaryan R, Molaei T (2021) Comparing the dimensional accuracy of casts obtained from two types of silicone impression materials in different impression techniques and frequent times of cast preparation. Int J Dent 2021:9977478. https://doi.org/10.1155/2021/9977478
Pham DL, Xu C, Prince JL (2000) Current methods in medical image segmentation. Annu Rev Biomed Eng 2:315–37. https://doi.org/10.1146/annurev.bioeng.2.1.315
Ogawa T, Enciso R, Shintaku WH, Clark GT (2007) Evaluation of cross-section airway configuration of obstructive sleep apnea. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 103(1):102–8. https://doi.org/10.1016/j.tripleo.2006.06.008
El H, Palomo JM (2010) Measuring the airway in 3 dimensions: a reliability and accuracy study. Am J Orthod Dentofacial Orthop 137(4 Suppl):S50.e1-9. https://doi.org/10.1016/j.ajodo.2010.01.014. discussion S50-2
Stratemann S, Huang JC, Maki K, Hatcher D, Miller AJ (2011) Three-dimensional analysis of the airway with cone-beam computed tomography. Am J Orthod Dentofacial Orthop 140(5):607–15. https://doi.org/10.1016/j.ajodo.2010.12.019
Funding
This work was supported by Canadian Institutes of Health Research (grant 325899), the Canadian Foundation of Innovation (CFI 28236), Chinese Stomatological Association Clinical Research Fund (CSA-O2022-08), Shandong Provincial Natural Science Foundation (grant N.ZR2020QH161), China Oral Health Foundation (grant A2021-102), China Postdoctoral Science Foundation, grant number(2020M682173).
Author information
Authors and Affiliations
Contributions
Hui Chen, study design, wrote the manuscript, prepared figures and tables;
Tao Lv, study design, revise the manuscript;
Qing Luo, analyzed the images, statistical analysis;
Lei Li, 3D printing; prepared the phantom;
Qing Wang, analyzed the data;
Yanzhong Li, 3D analysis of nasal cavity; prepared figures and tables;
Debo Zhou, analyzed the data, prepared the phantom;
Elham Emami, wrote and revised the manuscript;
Matthieu Schmittbuhl, wrote and revise the manuscript;
Paul van der Stelt, wrote the manuscript;
Nelly Huynh, study design, wrote and revise the manuscript.
Corresponding authors
Ethics declarations
Ethics approval and consent to participate
This is a retrospective study based on the CBCT images of both Canadian and Chinese OSA patients.
The protocol of recruiting Canadian OSA patients was approved by the Research Ethics Board of Health of the Université de Montréal (13-076-CERES-D).
The protocol of recruiting patients from China was approved by the Medical Ethic Committee of the Dental School of Shandong University (NO.GR201814).
Competing interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Chen, H., Lv, T., Luo, Q. et al. Reliability and accuracy of a semi-automatic segmentation protocol of the nasal cavity using cone beam computed tomography in patients with sleep apnea. Clin Oral Invest 27, 6813–6821 (2023). https://doi.org/10.1007/s00784-023-05295-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-023-05295-6