Abstract
Objectives
The study was aimed at comparing implants installed with guided and conventional surgery.
Material and methods
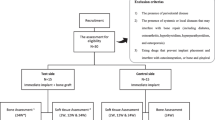
Twenty-nine total edentulous patients were selected, and maxillary contralateral quadrants were randomly assigned to static computer-aided implant surgery (S-CAIS): flapless computer-guided surgery, and conventional surgery (CS): flap surgery with conventional planning. Tomography scans were performed at baseline and 10 days after the surgery for deviation measurement, and radiography was done at baseline and after 6 and 12 months, for peri-implant bone level (PIBL) analysis. Peri-implant fluid and subgingival biofilm were collected to evaluate bone markers and periodontal pathogens.
Results
S-CAIS showed less linear deviation at the apical point and at the midpoint and, less angular deviation (p < 0.05), with greater depth discrepancy in the positioning of the platform (p < 0.05). Higher values of vertical PIBL were observed for the S-CAIS group at baseline (p < 0.05), while lower values of horizontal PIBL were observed for CS (p < 0.05). Bone markers presented higher levels in CS (p < 0.05).
Conclusion
Flapless S-CAIS allowed smaller linear and angular deviations than the conventional technique. However, PIBL was higher in S-CAIS; the conventional technique led to a greater angiogenic and bone remodeling activity by elevating the angiogenic and bone markers levels.
Clinical relevance
Evaluating the different implant insertion techniques can guide clinical and surgical regarding the accuracy, the release pattern of bone markers, and the peri-implant bone level.
Trial registration
ReBEC-RBR-8556fzp.







Similar content being viewed by others
Data availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
Change history
10 May 2023
A Correction to this paper has been published: https://doi.org/10.1007/s00784-023-05045-8
References
Adell R, Lekholm U, Rockler B, Brånemark PI (1981) A 15-year study of osseointegrated implants in the treatment of the edentulous jaw. Int J Oral Surg 10:387–416. https://doi.org/10.1016/s0300-9785(81)80077-4
Zarb GA, Schmitt A (1990) Terminal dentition in elderly patients and implant therapy alternatives. Int Dent J 40:67–73
Lindquist LW, Carlsson GE, Jemt T (1996) A prospective 15-year follow-up study of mandibular fixed prostheses supported by osseointegrated implants. Clinical results and marginal bone loss. Clin Oral Implants Res 7:329–336. https://doi.org/10.1034/j.1600-0501.1996.070405.x
Naert I, Koutsikakis G, Duyck J, Quirynen M, Jacobs R, van Steenberghe D (2000) Biologic outcome of single-implant restorations as tooth replacements: a long-term follow-up study. Clin Implant Dent Relat Res 2:209–218. https://doi.org/10.1111/j.1708-8208.2000.tb00119.x
Merickse-Stern R, Aerni D, Geering AH, Buser D (2001) Long-term evaluation of non-submerged hollow cylinder implants. Clinical and radiographic results. Clin Oral Implants Res 12:252–259. https://doi.org/10.1034/j.1600-0501.2001.012003252.x
Jemt T, Johansson J (2006) Implant treatment in the edentulous maxillae: a 15-year follow-up study on 76 consecutive patients provided with fixed prostheses. Clin Implant Dent Relat Res 8:61–69. https://doi.org/10.1111/j.1708-8208.2006.00003.x
Varga E Jr, Antal M, Major L, Kiscsatári R, Braunitzer G, Piffkó J (2020) Guidance means accuracy: a randomized clinical trial on free-hand versus guided dental implantation. Clin Oral Implants Res 31:417–430. https://doi.org/10.1111/clr.13578
Guentsch A, Sukhtankar L, An H, Luepke PG (2020) Precision and trueness of implant placement with and without static surgical guides: an in vitro study. J Prosthet Dent 3:30424–30428. https://doi.org/10.1016/j.prosdent.2020.06.015
Sigcho López DA, García I, Da Silva Salomao G, Cruz Laganá D (2019) Potential deviation factors affecting stereolithographic surgical guides: a systematic review. Implant Dent 28:68–73. https://doi.org/10.1097/ID.0000000000000853
Zhou W, Liu Z, Song L, Kuo CL, Shafer DM (2018) Clinical factors affecting the accuracy of guided implant surgery-a systematic review and meta-analysis. J Evid Based Dent Pract 18:28–40. https://doi.org/10.1016/j.jebdp.2017.07.007
Sarment DP, Sukovic P, Clinthorne N (2003) Accuracy of implant placement with a stereolithographic surgical guide. Int J Oral Maxillofac Implants 18:571–577
Bouserhal C, Jacobs R, Quirynen M, van Steenberghe D (2002) Imaging technique selection for the preoperative planning of oral implants: a review of the literature. Clin Implant Dent Relat Res 4:156–172. https://doi.org/10.1111/j.1708-8208.2002.tb00167.x
Lee SJ, Toothaker RW (1998) Computed tomographic scan template for maximum accuracy of reformatted CT scan images. J Prosthodont 7:261–264. https://doi.org/10.1111/j.1532-849x.1998.tb00215.x
McGivney GP, Haughton V, Strandt JA, Eichholz JE, Lubar DM (1986) A comparison of computer-assisted tomography and data-gathering modalities in prosthodontics. Int J Oral Maxillofac Implants 1:55–68
Ben Yehuda D, Weber HP, Finkelman M, Sicilia E, Muftu A, Chochlidakis K, Papaspyridakos P (2020) Accuracy of guided implant surgery in 25 edentulous arches: a laboratory observational study. J Prosthodont 29:718–724. https://doi.org/10.1111/jopr.13224
Hultin M, Svensson KG, Trulsson M (2012) Clinical advantages of computer-guided implant placement: a systematic review. Clin Oral Implant Res 23:124–135. https://doi.org/10.1111/j.1600-0501.2012.02545.x
Pimkhaokham A, Jiaranuchart S, Kaboosaya B, Arunjaroensuk S, Subbalekha K, Mattheos N (2022) Can computer-assisted implant surgery improve clinical outcomes and reduce the frequency and intensity of complications in implant dentistry? A critical review. Periodontol 2000. https://doi.org/10.1111/prd.12458. Online ahead of print
Romandini M, Ruales-Carrera E, Sadilina S, Hämmerle CHF, Sanz M (2022) Minimal invasiveness at dental implant placement: a systematic review with meta-analyses on flapless fully guided surgery. Periodontol 2000. https://doi.org/10.1111/prd.12440. Online ahead of print
Chackartchi T, Romanos GE, Parkanyi L, Schwarz F, Sculean A (2022) Reducing errors in guided implant surgery to optimize treatment outcomes 2000. Periodontol 88(1):64–72. https://doi.org/10.1111/prd.12411
Tarnow DP, Cho SC, Wallace SS (2000) The effect of inter-implant distance on the height of inter-implant bone crest. J Periodontol 71:546–549
Amorfini L, Migliorati M, Drago S, Silvestrini-Biavati A (2017) Immediately loaded implants in rehabilitation of the maxilla: a two-year randomized clinical trial of guided surgery versus standard procedure. Clin Implant Dent Relat Res 19:280–295. https://doi.org/10.1111/cid.12459
Pozzi A, Tallarico M, Marchetti M, Scarfò B, Esposito M (2014) Computer-guided versus free-hand placement of immediately loaded dental implants: 1-year post-loading results of a multicentre randomised controlled trial. Eur J Oral Implantol 7:229–242
D’Haese J, Van de Velde T, Komiyama A, Hultin M, De Bruyn H (2012) Accuracy and complications using computerdesigned stereolithographic surgical guides for oral rehabilitation by means of dental implants: a review of the literature. Clin Implant Dent Relat Res 14:321–335. https://doi.org/10.1111/j.1708-8208.2010.00275.x
Tahmaseb A, Wismeijer D, Coucke W, Derksen W (2014) Computer technology applications in surgical implant dentistry: a systematic review. Int J Oral Maxillofac Implants 29:25–42. https://doi.org/10.11607/jomi.2014suppl.g1.2
Voulgarakis A, Strub JR, Att W (2014) Outcomes of implants placed with three different flapless surgical procedures: a systematic review. Int J Oral Maxillofac Surg 43:476–486. https://doi.org/10.1016/j.ijom.2013.10.024
Lin GH, Chan HL, Bashutski JD, Oh TJ, Wang HL (2014) The effect of flapless surgery on implant survival and marginal bone level: a systematic review and meta-analysis. J Periodontol 85:e91–e103. https://doi.org/10.1902/jop.2013.130481
Moraschini V, Velloso G, Luz D, Porto Barboza E (2015) Implant survival rates, marginal bone level changes, and complications in full-mouth rehabilitation with flapless computer-guided surgery: a systematic review and meta-analysis. Int J Oral Maxillofac Surg 44:892–901. https://doi.org/10.1016/j.ijom.2015.02.013
Naeini EN, Atashkadeh M, De Bruyn H, D’Haese J (2020) Narrative review regarding the applicability, accuracy, and clinical outcome of flapless implant surgery with or without computer guidance. Clin Implant Dent Relat Res 22:454–467. https://doi.org/10.1111/cid.12901
Jung R, Schneider D, Ganeles J, Wismeijer D, Zwahlen M, Hammerle CH, Tahmaseb A (2009) Computer technology applications in surgical implant dentistry: a systematic review. Int J Oral Maxillofac Implants 24:92–109
Schneider D, Marquardt P, Zwahlen M, Jung RE (2009) A systematic review on the accuracy and the clinical outcome of computer-guided template-based implant dentistry. Clin Oral Implants Res 4:73–86
Chambrone L, Zucchelli G (2022) Why is there a lack of evidence regarding errors and complications in periodontal and implant therapy? Periodontol 2000. https://doi.org/10.1111/prd.12445. Online ahead of print
Soares MM, Harari ND, Cardoso ES, Manso MC, Conz MB, Vidigal GM Jr (2012) An in vitro model to evaluate the accuracy of guided surgery systems. Int J Oral Maxillofac Implants 27:824–831
Szklo R, Nieto FJ (2000) Epidemiology beyond the basis, 4th edn. Aspen Publications
Óbice ALS, Correa MG, Feng HS, Ribeiro FV, Cirano FR, Casati MZ, Pimentel SP (2019) The impact of implant abutment surface treatment with TiO2 on peri-implant levels of angiogenesis and bone-related markers: a randomized clinical trial. Int J Oral Maxillofac Surg 48:962–970. https://doi.org/10.1016/j.ijom.2018.12.012
Gargallo-Albiol J, Barootchi S, Marqués-Guasch J, Wang HL (2020) Fully guided versus half-guided and freehand implant placement: systematic review and meta-analysis. Int J Oral Maxillofac Implants 35:1159–1169. https://doi.org/10.11607/jomi.7942
Vercruyssen M, Cox C, Naert I, Jacobs R, Teughels W, Quirynen M (2016) Accuracy and patient centered outcome variables in guided implant surgery: a RCT comparing immediate with delayed loading. Clin Oral Implants Res 27:1–6. https://doi.org/10.1111/clr.12583
Vercruyssen M, Van De Wiele G, Teughels W, Naert I, Jacobs R, Quirynen M (2014) Implant- and patient-centred outcomes of guided surgery, a 1-year follow-up: an RCT comparing guided surgery with conventional implant placement. J Clin Periodontol 41:1154–1160. https://doi.org/10.1111/jcpe.12305
Magrin GL, Rafael SNF, Passoni BB, Magini RS, Benfatti CAM, Gruber R, Peruzzo DC (2020) Clinical and tomographic comparison of dental implants placed by guided virtual surgery versus conventional technique: a split-mouth randomized clinical trial. J Clin Periodontol 47:120–128. https://doi.org/10.1111/jcpe.13211
Chen Z, Li J, Sinjab K, Mendoca G, Yu H, Wang H (2018) Accuracy of flap immediate implant placement in anterior maxilla using computer-assisted versus free-hand surgery: a cadaver study. Clin Oral Implants Res 29:1186–1194. https://doi.org/10.1111/clr.13382
Bover-Ramos F, Viña-Almunia J, Cervera-Ballestr J, Peñarrocha-Diago M, García-Mira B (2017) Accuracy of implant placement with computer-guided surgery: a systematic review and meta-analysis comparing cadaver, clinical, and in vitro studies. Int J Oral Maxillofac Implants 33:101–115. https://doi.org/10.11607/jomi.5556
Arisan V, Karabuda CZ, Özdemir T (2010) Implant surgery using bone- and mucosa-supported stereolithographic guides in totally edentulous jaws: surgical and post-operative outcomes of computer-aided vs. standard techniques. Clin Oral Implants Res 21:980–988. https://doi.org/10.1111/j.1600-0501.2010.01957.x
Pettersson A, Komiyama A, Hultin M, Näsström K, Klinge B (2012) Accuracy of virtually planned and template guided implant surgery on edentate patients. Clin Implant Dent Relat Res 14:527–537. https://doi.org/10.1111/j.1708-8208.2010.00285.x
Vercruyssen M, Laleman I, Jacobs R, Quirynen M (2015) Computer-supported implant planning and guided surgery: a narrative review. Clin Oral Implants Res 26:69–76. https://doi.org/10.1111/clr.12638
Verhamme LM, Meijer GJ, Boumans T, Schutyser F, Bergé SJ, Maal TJJ (2013) A clinically relevant validation method for implant placement after virtual planning. Clin Oral Implants Res 24:1265–1272. https://doi.org/10.1111/j.1600-0501.2012.02565.x
Vieira DM, Sotto-Maior BS, Barros CA, Reis ES, Francischone CE (2013) Clinical accuracy of flapless computer-guided surgery for implant placement in edentulous arches. Int J Oral Maxillofac Implants 28:1347–1351. https://doi.org/10.11607/jomi.3156
Choi W, Nguyen B, Doan A (2017) Freehand versus guided surgery: factors influencing accuracy of dental implant placement. Implant Dent 26:500–509. https://doi.org/10.1097/ID.0000000000000620
Vermeulen J (2017) The accuracy of implant placement by experienced surgeons: guided vs freehand approach in a simulated plastic model. Int J Oral Maxillofac Implants 32:617–624. https://doi.org/10.11607/jomi.5065
Raico Gallardo YN, da Silva-Olivio IRT, Mukai E, Morimoto S, Sesma N, Cordaro L (2017) Accuracy comparison of guided surgery for dental implants according to the tissue of support: a systematic review and meta-analysis. Clin Oral Implants Res 28:602–612. https://doi.org/10.1111/clr.12841
Cassetta M, Di Mambro A, Giansanti M, Stefanelli LV, Cavallini C (2013) The intrinsic error of a stereolithographic surgical template in implant guided surgery. Int J Oral Maxillofac Surg 42:264–275. https://doi.org/10.1016/j.ijom.2012.06.010
Laleman I, Bernard L, Vercruyssen M, Jacobs R, Bornstein M, Quirynen M (2017) Guided implant surgery in the edentulous maxilla: a systematic review. Int J Oral Maxillofac Implants 31:103–117. https://doi.org/10.11607/jomi
Vohra F, Al-Kheraif AA, Almas K, Javed F (2015) Comparison of crestal bone loss around dental implants placed in healed sites using flapped and flapless techniques: a systematic review. J Periodontol 86:185–191. https://doi.org/10.1902/jop.2014.140355
Cai H, Liang X, Sun DY (2020) Chen JY (2020) Long-term clinical performance of flapless implant surgery compared to the conventional approach with flap elevation: a systematic review and meta-analysis. World J Clin Cases 8:1087–1103. https://doi.org/10.12998/wjcc.v8.i6.1087
Tsoukaki M, Kalpidis CDR, Sakellari D, Tsalikis L, Mikrogiorgis G, Konstantinidis A (2013) Clinical, radiographic, microbiological, and immunological outcomes of flapped vs. flapless dental implants: a prospective randomized controlled clinical trial. Clin Oral Implants Res 24:969–976. https://doi.org/10.1111/j.1600-0501.2012.02503.x
Huang B, Meng H, Piao M, Xu L, Zhang L, Zhu W (2012) Influence of placement depth on bone remodeling around tapered internal connection implant: a clinical and radiographic study in dogs. J Periodontol 83:1164–1171. https://doi.org/10.1902/jop.2012.110617
Pessoa RS, Sousa RM, Pereira LM, Neves FD, Bezerra FJB, Jaecques SVN, Sloten JV, Quirynen M, Teughels W, Spin-Neto R (2017) Bone remodeling around implants with external hexagon and morse-taper connections: a randomized, controlled, split-mouth, clinical trial. Clin Implant Dent Related Res 19:97–110. https://doi.org/10.1111/cid.12437
Zhou M, Zhou H, Li SY, Yang XB, Geng YM, Che YJ (2021) Accuracy of Implant placement guided with surgical template: an in vitro and in vivo Study. Int J Periodont Restor Dent 41:e55–e62. https://doi.org/10.11607/prd.4570
Lei Q, Chen J, Jiang J, Fu X, Lin H, Cai Z (2013) Comparison of soft tissue healing around implants in beagle dogs: flap surgery versus flapless surgery. Oral Surg Oral Med Oral Pathol Oral Radiol 115:e21–e27. https://doi.org/10.1016/j.oooo.2011.11.025
Luther G, Wagner ER, Zhu G, Kang Q, Luo Q, Lamplot J, Bi Y, Luo X, Luo J, Teven C, Shi Q, Kim SH, Gao JL, Huang E, Yang K, Rames R, Liu X, Li M, Hu N, Liu H, Su Y, Chen L, He BC, Zuo GW, Deng ZL, Reid RR, Luu HH, Haydon RC, He TC (2011) BMP-9 induced osteogenic differentiation of mesen-chymal stem cells: molecular mechanism and therapeutic potential. Curr Gene Ther 11:229–240. https://doi.org/10.2174/156652311795684777
Quirynen M, Van Assche N (2011) Microbial changes after full-mouth tooth extraction, followed by 2-stage implant placement. J Clin Periodontol 38:581–589. https://doi.org/10.1111/j.1600-051X.2011.01728.x
Quirynen M, De Soete M, Dierickx K, van Steenberghe D (2001) The intra-oral translocation of periodontopathogens jeopardises the outcome of periodontal therapy. A review of the literature. J Clin Periodontol 28:499–507. https://doi.org/10.1034/j.1600-051x.2001.028006499.x
Slots J (2002) Selection of antimicrobial agents in periodontal therapy. J Period Res 37:389–398. https://doi.org/10.1034/j.1600-0765.2002.00004.x
Quirynen M, Vogels R, Pauwels M, Haffajee AD, Socransky SS, Uzel NG, van Steenberghe D (2005) Initial subgingival colonization of ‘pristine’ pockets. J Dental Res 84:340–344. https://doi.org/10.1177/154405910508400409
Quirynen M, Vogels R, Peeters W, van Steenberghe D, Naert I, Haffajee A (2006) Dynamics of initial subgingival colonization of ‘pristine’ peri-implant pockets. Clin Oral Implants Res 17:25–37. https://doi.org/10.1111/j.1600-0501.2005.01194.x
Mombelli A, Buser D, Lang NP (1998) Colonization of osseointegrated titanium implants in edentulous patients Early results. Oral Microbiol Immunol 3:113–120. https://doi.org/10.1111/j.1399-302x.1988.tb00095.x
Apse P, Ellen RP, Overall CM, Zarb GA (1989) Microbiota and crevicular fluid collagenase activity in the osseointegrated dental implant sulcus: a comparison of sites in edentulous and partially edentulous patients. J Periodontal Res 24:96–105. https://doi.org/10.1111/j.1600-0765.1989.tb00863.x
Quirynen M, Listgarten MA (1990) The distribution of bacterial morphotypes around natural teeth and titanium implants ad modum Bra°nemark. Clin Oral Implants Res 4:8–12. https://doi.org/10.1034/j.1600-0501.1990.010102.x
Mombelli A, Mericske-Stern R (1990) Microbiological features of stable osseointegrated implants used as abutments for overdentures. Clin Oral Implants Res 1:1–7. https://doi.org/10.1034/j.1600-0501.1990.010101.x
Papaioannou W, Quirynen M, Nys M, van Steenberghe D (1995) The effect of periodontal parameters on the subgingival microbiota around implants. Clin Oral Implants Res 6:197–204. https://doi.org/10.1034/j.1600-0501.1995.060401.x
Danser MM, Van Winkelhoff AJ, Van der Velden U (1997) Periodontal bacteria colonizing oral mucous membranes in edentulous patients wearing dental implants. J Periodontol 68:209–216. https://doi.org/10.1902/jop.1997.68.3.209
Lee KH, Tanner ACR, Maiden MFJ, Weber HP (1999) Pre- and post-implantation microbiota of the tongue, teeth, and newly-placed implants. J Clin Periodontol 26:822–832. https://doi.org/10.1111/j.1600-051x.1999.tb02527.x
Slots J (2004) Research, Science and Therapy Committee Systemic antibiotics in periodontics. J Periodontol 75:1553–1565. https://doi.org/10.1902/jop.2004.75.11.1553
Lee KH, Maiden MFJ, Tanner ACR, Weber HP (1999) Microbiota of successful osseointegrated dental implants. J Periodontol 70:131–138. https://doi.org/10.1902/jop.1999.70.2.131
Hultin M, Gustafsson A, Hallstrom H, Johansson LA, Ekfeldt A, Klinge B (2002) Microbiological findings and host response in patients with peri-implantitis. Clin Oral Implants Res 13:349–358. https://doi.org/10.1034/j.1600-0501.2002.130402.x
Funding
This study was supported by the São Paulo Research Foundation (FAPESP; São Paulo, SP, Brazil; processes 2018/05376–2).
Author information
Authors and Affiliations
Contributions
LMN: worked at the experimental phase (clinical procedures and patient recruitment).
EKM: worked at experimental phase (clinical procedures and patient recruitment).
MGC: drafting the work.
FRV: analysis, and interpretation of data for the work and laboratorial analysis.
FRC: substantial contributions to the conception or design of the work.
SPP: final approval of the version to be published and clinical procedures.
MZC: final approval of the version to be published and agreement to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
All authors agree to be personally accountable for the author’s own contributions and for ensuring that questions related to the accuracy or integrity of any part of the work, even ones in which the author was not personally involved, are appropriately investigated, resolved, and documented in the literature.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
All eligible patients were thoroughly informed of the nature, potential risks, and benefits of their participation in the study and signed an informed consent document. This study was approved by the ethics committee of Paulista University (2.059.143).
Conflict of interest
The authors declare no conflict of interest.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The original version of this article was revised: This article was originally published with some of the text, table headings and table references need to be corrected. Additionally, figure 4 also needs to be replaced.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Nomiyama, L.M., Matumoto, E.K., Corrêa, M.G. et al. Comparison between flapless-guided and conventional surgery for implant placement: a 12-month randomized clinical trial. Clin Oral Invest 27, 1665–1679 (2023). https://doi.org/10.1007/s00784-022-04793-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-022-04793-3