Abstract
Objectives
Periodontitis is a local inflammatory disease of high prevalence worldwide. Increasing evidence has shown its association with cardiovascular diseases. While high-density lipoprotein is an important protective factor in preventing cardiovascular diseases, this study aims to examine whether high-density lipoprotein cholesterol (HDL-C) level is associated with different status of periodontitis.
Materials and methods
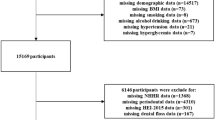
A total of 874 Chinese retirees (≥ 60 years of age) with different statuses of periodontitis were enrolled. Periodontal clinical data were collected to define periodontal disease severity (no, mild-moderate, severe). Peripheral blood was collected for serum lipid profile analysis. Linear and logistic regression analysis with adjustment for potential confounders (gender, age, BMI, alcohol intake, exercise frequency, smoking habits) were used to determine the association of periodontitis with HDL-C.
Results
After adjustments for confounders, linear regression analyses revealed a significant relationship between the decreased HDL-C and periodontitis severity (p < 0.05). Although the multivariable-adjusted ORs of decreased HDL-C were not statistically significant, logistic regression analyses showed Chinese elderly with severe periodontitis had higher odds of exhibiting clinically abnormal HDL-C levels than those without periodontitis.
Conclusions
The elderly population with periodontitis showed HDL-C levels significantly lower than those without periodontitis. The severity of periodontitis was positively correlated with serum HDL-C levels.
Clinical relevance
Periodontitis reduces HDL-C level in the elderly population, indicating that oral health should be paid attention to in the prevention and treatment of dyslipidemia.
Similar content being viewed by others
References
Kinane DF, Stathopoulou PG, Papapanou PN (2017) Periodontal diseases. Nat Rev Dis Primers 3:17038
Global Burden of Disease Study 2013 Collaborators (2015) Global, regional, and national incidence, prevalence, and years lived with disability for 301 acute and chronic diseases and injuries in 188 countries, 1990–2013: a systematic analysis for the Global Burden of Disease Study 2013. Lancet 386(9995):743–800
Jiao J, Jing W, Si Y et al (2021) The prevalence and severity of periodontal disease in Mainland China: data from the Fourth National Oral Health Survey (2015–2016). J Clin Periodontol 48(2):168–179
Schenkein HA, Papapanou PN, Genco R, Sanz M (2020) Mechanisms underlying the association between periodontitis and atherosclerotic disease. Periodontol 2000 83(1):90–106. https://doi.org/10.1111/prd.12304
Sanz M, Marco Del Castillo A, Jepsen S et al (2020) Periodontitis and cardiovascular diseases: consensus report. J Clin Periodontol 47(3):268–288
Tonetti MS, Van Dyke TE (2013) Working group 1 of the joint EFPAAPw Periodontitis and atherosclerotic cardiovascular disease: consensus report of the Joint EFP/AAP Workshop on Periodontitis and Systemic Diseases. J Clinl Periodontol 40(1Suppl 14):S24–S29
Sen S, Giamberardino LD, Moss K et al (2018) Periodontal disease, regular dental care use, and incident ischemic stroke. Stroke 49(2):355–362
Herrera D, Molina A, Buhlin K (2000) Klinge B (2020) Periodontal diseases and association with atherosclerotic disease. Periodontol 83(1):66–89
Genco RJ (2000) Sanz M (2020) Clinical and public health implications of periodontal and systemic diseases: An overview. Periodontol 83(1):7–13
Kapila YL (2000) (2021) Oral health’s inextricable connection to systemic health: special populations bring to bear multimodal relationships and factors connecting periodontal disease to systemic diseases and conditions. Periodontol 87(1):11–16
GBD (2017) Causes of Death Collaborators (2018) Global, regional, and national age-sex-specific mortality for 282 causes of death in 195 countries and territories, 1980–2017: a systematic analysis for the Global Burden of Disease Study 2017. Lancet 392(10159):1736–1788
Sharrett AR, Ballantyne CM, Coady SA et al (2001) Coronary heart disease prediction from lipoprotein cholesterol levels, triglycerides, lipoprotein(a), apolipoproteins A-I and B, and HDL density subfractions: The Atherosclerosis Risk in Communities (ARIC) Study. Circulation 104(10):1108–1113
Barter P, Gotto AM, LaRosa JC et al (2007) HDL cholesterol, very low levels of LDL cholesterol, and cardiovascular events. N Engl J Med 357(13):1301–1310
Rosenson RS, Brewer HB Jr, Chapman MJ et al (2011) HDL measures, particle heterogeneity, proposed nomenclature, and relation to atherosclerotic cardiovascular events. Clin Chem 57:392–410
Rye KA, Barter PJ (2014) Cardioprotective functions of HDLs. J Lipid Res 55(2):168–179
Banu S, Jabir NR, Mohan R et al (2015) Correlation of Toll-like receptor 4, interleukin-18, transaminases, and uric acid in patients with chronic periodontitis and healthy adults. J Periodontol 86(3):431–439
Kumar KR, Ranganath V, Naik R, Banu S, Nichani AS (2014) Assessment of high-sensitivity C-reactive protein and lipid levels in healthy adults and patients with coronary artery disease, with and without periodontitis—a cross-sectional study. J Periodontal Res 49(6):836–844
Sridhar R, Byakod G, Pudakalkatti P, Patil R (2009) A study to evaluate the relationship between periodontitis, cardiovascular disease and serum lipid levels. Int J Dent Hyg 7(2):144–150
Joseph R, Nath SG, Joseraj MG (2011) Elevated plasma homocysteine levels in chronic periodontitis: a hospital-based case-control study. J Periodontol 82(3):439–444
Taleghani F, Shamaei M, Shamaei M (2010) Association between chronic periodontitis and serum lipid levels. Acta Med Iran 48(1):47–50
Jaramillo A, Lafaurie GI, Millán LV et al (2013) Association between periodontal disease and plasma levels of cholesterol and triglycerides. Colomb Med (Cali) 44:80–86
Kuwabara M, Kuwabara R, Niwa K et al (2018) Different risk for hypertension, diabetes, dyslipidemia, and hyperuricemia according to level of body mass index in Japanese and American Subjects. Nutrients 10(8):1011
Li W, Shi D, Song W et al (2019) A novel U-shaped relationship between BMI and risk of generalized aggressive periodontitis in Chinese: a cross-sectional study. J Periodontol 90(1):82–89
Vodnala D, Rubenfire M, Brook RD (2012) Secondary causes of dyslipidemia. Am J Cardiol 110(6):823–825
Amaral Cda S, Vettore MV, Leão A (2009) The relationship of alcohol dependence and alcohol consumption with periodontitis: a systematic review. J Dent 37(9):643–651
Moradinazar M, Pasdar Y, Najafi F et al (2020) Association between dyslipidemia and blood lipids concentration with smoking habits in the Kurdish population of Iran. BMC Public Health 20(1):673
Leite FRM, Nascimento GG, Scheutz F, López R (2018) Effect of smoking on periodontitis: a systematic review and meta-regression. Am J Prev Med 54(6):831–841
Lee JB, Yi HY, Bae KH (2013) The association between periodontitis and dyslipidemia based on the Fourth Korea National Health and Nutrition Examination Survey. J Clin Periodontol 40(5):437–442
Lee S, Im A, Burm E, Ha M (2018) Association between periodontitis and blood lipid levels in a Korean population. J Periodontol 89(1):28–35
Han SJ, Yi YJ, Bae KH (2020) The association between periodontitis and dyslipidemia according to smoking and harmful alcohol use in a representative sample of Korean adults. Clin Oral Investig 24(2):937–944
Tran DT, Gay I, Du XL et al (2014) Assessment of partial-mouth periodontal examination protocols for periodontitis surveillance. J Clin Periodontol 41(9):846–852
Joint committee for guideline revision (2018) 2016 Chinese guidelines for the management of dyslipidemia in adults. J Geriatr Cardiol 15(1):1–29
Mayo Clinic Staff (2021) High Cholesterol diagnosis and treatment. Mayo Clinic. https://www.mayoclinic.org/diseases-conditions/high-blood-cholesterol/diagnosis-treatment/drc-20350806. Accessed 1 Feb 2022
Anagnostis P, Stevenson JC, Crook D et al (2015) Effects of menopause, gender and age on lipids and high-density lipoprotein cholesterol subfractions. Maturitas 81(1):62–68
Feng L, Nian S, Tong Z et al (2020) Age-related trends in lipid levels: a large-scale cross-sectional study of the general Chinese population. BMJ Open 10(3):e034226
Pollock RD, Carter S, Velloso CP et al (2015) An investigation into the relationship between age and physiological function in highly active older adults. J Physiol 593(3):657–680
Rando TA, Chang HY (2012) Aging, rejuvenation, and epigenetic reprogramming: resetting the aging clock. Cell 148(1–2):46–57
Liu J, Wu Y, Ding Y, Meng S, Ge S, Deng H (2010) Evaluation of serum levels of C-reactive protein and lipid profiles in patients with chronic periodontitis and/or coronary heart disease in an ethnic Han population. Quintessence Int 41(3):239–247
Monteiro AM, Jardini MA, Alves S et al (2009) Cardiovascular disease parameters in periodontitis. J Periodontol 80(3):378–388
Nepomuceno R, Pigossi SC, Finoti LS et al (2017) Serum lipid levels in patients with periodontal disease: a meta-analysis and meta-regression. J Clin Periodontol 44(12):1192–1207
Ylöstalo PV, Knuuttila ML (2006) Confounding and effect modification: possible explanation for variation in the results on the association between oral and systemic diseases. J Clin Periodontol 33(2):104–108
Nibali L, D’Aiuto F, Griffiths G et al (2007) Severe periodontitis is associated with systemic inflammation and a dysmetabolic status: a case-control study. J Clin Periodontol 34(11):931–937
Duzagac E, Cifcibasi E, Erdem MG et al (2016) Is obesity associated with healing after non-surgical periodontal therapy? A local vs systemic evaluation. J Periodontal Res 51(5):604–612
Leite AC, Carneiro VM, Guimarães Mdo C (2014) Effects of periodontal therapy on C-reactive protein and HDL in serum of subjects with periodontitis. Rev Bras Cir Cardiovasc 29(1):69–77
Magán-Fernández A, Papay-Ramírez L, Tomás J et al (2014) Association of simvastatin and hyperlipidemia with periodontal status and bone metabolism markers. J Periodontol 85:1408–1415
Owens JD, Dowsett SA, Eckert GJ et al (2003) Partial-mouth assessment of periodontal disease in an adult population of the United States. J Periodontol 74(8):1206–1213
Kingman A, Susin C, Albandar JM (2008) Effect of partial recording protocols on severity estimates of periodontal disease. J Clin Periodontol 35:659–667
Peres MA, Peres KG, Cascaes AM et al (2012) Validity of partial protocols to assess the prevalence of periodontal outcomes and associated sociodemographic and behavior factors in adolescents and young adults. J Periodontol 83(3):369–378
Funding
The authors received financial support from Natural Science Foundation of Zhejiang Province (LZY21F030002), the Fundamental Research Funds for the Zhejiang Provincial Universities (2021XZZX033), and China Oral Health Foundation (A2021-008).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval
This study was approved by the Ethics Committee of Stomatology Hospital affiliated to Zhejiang University School of Medicine (No.2019-003).
Informed consent
Written informed consent was obtained from all the participants.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Zhu, H., Ye, G., Xie, Y. et al. Association of high-density lipoprotein cholesterol and periodontitis severity in Chinese elderly: a cross-sectional study. Clin Oral Invest 26, 4753–4759 (2022). https://doi.org/10.1007/s00784-022-04439-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-022-04439-4