Abstract
Objectives
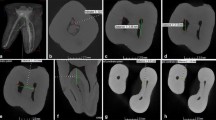
The present study aimed to evaluate the frequency, position, and length of radicular pulp calcifications in three-rooted maxillary first molars using micro-computed tomography.
Materials and methods
Two hundred three-rooted maxillary first molars were scanned at a pixel size of 10 µm and reconstructed using similar parameters. Three-dimensional models of the mesiobuccal (MB1, MB2, MB3), distobuccal (DB), and palatal (P) canals were qualitatively evaluated for discontinuity in the canal path. Transaxial and sagittal cross-sectional images of the roots were further screened, and the complete obliteration of the canal lumen by pulp calcification was identified when the canal had similar radiodensity to the surrounding dentine. Then, the number, position, and length of the calcifications were recorded for each root. Intra-observer agreement was performed using Cohen’s kappa test, while one-way ANOVA and Duncan tests compared the lengths of calcifications among the canals, with α = 5%.
Results
Intra-observer agreement was perfect for identification of pulp calcifications (ĸ = 1.0; p = 0.000). MB2 and MB3 canals accounted for the highest percentage frequency of calcifications distributed throughout the canal path. In the MB1, DB, and P canals, they occurred mainly at the apical third. Lengths of calcifications were greater in the MB3 (0.89 ± 0.81 mm) and MB2 (0.82 ± 0.93 mm) canals than in the MB1 (0.39 ± 0.32 mm), DB (0.34 ± 0.22 mm), and P (0.28 ± 0.22 mm) canals (p < 0.05).
Conclusion
MB2 and MB3 canals accounted for the highest frequency and length of radicular pulp calcifications. In the MB1, DB, and P canals, calcifications occurred mostly at the apical third, while in the MB2 and MB3, most of calcifications were observed at the orifice level and along the canal path.
Clinical relevance
In maxillary first molars, radicular pulp calcifications are mainly located at the apical third of the MB1, DB, and P canals, while in the MB2 and MB3 canals, most of them are at the orifice level or along the canal path.


Similar content being viewed by others
References
Carvalho TS, Lussi A (2017) Age-related morphological, histological and functional changes in teeth. J Oral Rehabil 44:291–298. https://doi.org/10.1111/joor.12474
McCabe P, Dummer PMH (2012) Pulp canal obliteration: an endodontic diagnosis and treatment challenge. Int Endod J 45:177–197. https://doi.org/10.1111/j.1365-591.2011.01963.x
Bastos JV, Côrtes MIS (2018) Pulp canal obliteration after traumatic injuries in permanent teeth - scientific fact or fiction? Braz Oral Res 32:e75. https://doi.org/10.1590/1807-3107bor-2018.vol32.0075
Chen B, Szabo D, Shen Y, Zhang D, Li X, Ma J, Haapasalo M (2020) Removal of calcifications from distal canals of mandibular molars by a non-instrumentational cleaning system: a micro-CT study. Aust Endod J 46:11–16. https://doi.org/10.1111/aej.12376
Tamse A, Kaffe I, Littner M, Shani R (1982) Statistical evaluation of radiologic survey of pulp stones. J Endod 8:455–458. https://doi.org/10.1016/S0099-2399(82)80150-7
Moss-Salentijn L, Klyvert MH (1983) Epithelially induced denticles in the pulps of recently erupted, noncarious human premolars. J Endod 9:554–560. https://doi.org/10.1016/S0099-2399(83)80060-0
Baghdady VS, Ghose LJ, Nahoom HY (1988) Prevalence of pulp stones in a teenage Iraqi group. J Endod 14:309–311. https://doi.org/10.1016/S0099-2399(88)80032-3
Şener S, Cobankara FK, Akgünlü F (2009) Calcifications of the pulp chamber: prevalence and implicated factors. Clin Oral Invest 13:209–215. https://doi.org/10.1007/s00784-008-0212-x
Goga R, Chandler NP, Oginni AO (2008) Pulp stones: a review. Int Endod J 41:457–468. https://doi.org/10.1111/j.1365-2591.2008.01374.x
Luukko K, Kettunen P, Fristad I, Berggreen E (2011) Structure and functions of the dentin-pulp complex. In: Hargreaves KM, Cohen S (eds) Cohen’s Pathways of the Pulp, 10th edn. Mosby, St. Louis, pp 283–348
da Silva EJNL, Prado MC, Queiroz PM, Nejaim Y, Brasil DM, Groppo FC, Haiter-Neto F (2017) Assessing pulp stones by cone-beam computed tomography. Clin Oral Investig 21:2327–2333. https://doi.org/10.1007/s00784-016-2027-5
Taşsöker M, Magat G, Şener S (2018) A comparative study of cone-beam computed tomography and digital panoramic radiography for detecting pulp stones. Imaging Sci Dent 48:201–212. https://doi.org/10.5624/isd.2018.48.3.201
Milcent CPF, da Silva TG, Baika LM, Grassi MT, Carneiro E, Franco A, de Lima AAS (2019) Morphologic, structural, and chemical properties of pulp stones in extracted human teeth. J Endod 45:1504–1512. https://doi.org/10.1016/j.joen.2019.09.009
Langeland K, Rodrigues H, Dowden W (1974) Periodontal disease, bacteria, and pulpal histopathology. Oral Surg Oral Med Oral Pathol 37:257–270. https://doi.org/10.1034/j.1600-051x.2002.290801.x
Li L, Zhu YQ, Jiang L, Peng W, Ritchie HH (2011) Hypoxia promotes mineralization of human dental pulp cells. J Endod 37:799–802. https://doi.org/10.1016/j.joen.2011.02.028
Fleig S, Attin T, Jungbluth H (2017) Narrowing of the radicular pulp space in coronally restored teeth. Clin Oral Invest 21:1251–1257. https://doi.org/10.1007/s00784-016-1899-8
Bernick S, Nedelman C (1975) Effect of aging on the human pulp. J Endod 1:88–94. https://doi.org/10.1016/S0099-2399(75)80024-0
Kannan S, Kannepady SK, Muthu K, Jeevan MB, Thapasum A (2015) Radiographic assessment of the prevalence of pulp stones in Malaysians. J Endod 41:333–337. https://doi.org/10.1016/j.joen.2014.10.015
Çolak H, Çelebi AA, Hamidi MM, Bayraktar Y, Çolak T, Uzgur R (2012) Assessment of the prevalence of pulp stones in a sample of Turkish central anatolian population. Sci World J 804278:1–7. https://doi.org/10.1100/2012/804278
De-Deus G, Belladonna FG, Cavalcante DM, Simoes-Carvalho M, Silva E, Carvalhal JCA, Zamolyi RQ, Lopes RT, Versiani MA, Dummer PMH, Zehnder M (2021) Contrast-enhanced micro-CT to assess dental pulp tissue debridement in root canals of extracted teeth: a series of cascading experiments towards method validation. Int Endod J 54:279–293. https://doi.org/10.1111/iej.13408
Yang YM, Guo B, Guo LY, Yang Y, Hong X, Pan HY, Zou WL, Hu T (2016) CBCT-aided microscopic and ultrasonic treatment for upper or middle thirds calcified root canals. Biomed Res Int 2016:1–9. https://doi.org/10.1155/2016/4793146
Ball RL, Barbizam JV, Cohenca N (2013) Intraoperative endodontic applications of cone-beam computed tomography. J Endod 39:548–557. https://doi.org/10.1016/j.joen.2012.11.038
Hsieh CY, Wu YC, Su CC, Chung MP, Huang RY, Ting PY, Lai CK, Chang KS, Tsai YC, Shieh YS (2018) The prevalence and distribution of radiopaque, calcified pulp stones: A cone-beam computed tomography study in a northern Taiwanese population. J Dent Sci 13:138–144. https://doi.org/10.1016/j.jds.2017.06.005
Zhang D, Chen J, Lan G, Li M, An J, Wen X, Liu L, Deng M (2017) The root canal morphology in mandibular first premolars: a comparative evaluation of cone-beam computed tomography and micro-computed tomography. Clin Oral Investig 21:1007–1012. https://doi.org/10.1007/s00784-016-1852-x
Borges CC, Estrela C, Decurcio DA, Pécora JD, Sousa-Neto MD, Rossi-Fedele G (2020) Cone-beam and micro-computed tomography for the assessment of root canal morphology: a systematic review. Braz Oral Res 34:e056. https://doi.org/10.1590/1807-3107bor-2020.vol34.0056
Ordinola-Zapata R, Bramante CM, Versiani MA, Moldauer BI, Topham G, Gutmann JL, Nuñez A, Duarte MA, Abella F (2017) Comparative accuracy of the clearing technique, CBCT and Micro-CT methods in studying the mesial root canal configuration of mandibular first molars. Int Endod J 50:90–96. https://doi.org/10.1111/iej.12593
Markvart M, Bjørndal L, Darvann TA, Larsen P, Dalstra M, Kreiborg S (2012) Three-dimensional analysis of the pulp cavity on surface models of molar teeth, using X-ray micro-computed tomography. Acta Odontol Scand 70:133–139. https://doi.org/10.3109/00016357.2011.600707
Park JW, Lee JK, Ha BH, Choi JH, Perinpanayagam H (2009) Three-dimensional analysis of maxillary first molar mesiobuccal root canal configuration and curvature using micro–computed tomography. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 108:437–442
Berès F, Isaac J, Mouton L, Rouzière S, Berdal A, Simon S, Dessombz A (2016) Comparative physicochemical analysis of pulp stone and dentin. J Endod 42:432–438. https://doi.org/10.1016/j.joen.2015.11.007
Jannati R, Afshari M, Moosazadeh M, Allahgholipour SZ, Eidy M, Hajihoseini M (2019) Prevalence of pulp stones: a systematic review and meta-analysis. J Evid Based Med 12:133–139. https://doi.org/10.1111/jebm.12331
Shahbazian M, Vandewoude C, Wyatt J, Jacobs R (2014) Comparative assessment of panoramic radiography and CBCT imaging for radiodiagnostics in the posterior maxilla. Clin Oral Invest 18:293–300. https://doi.org/10.1007/s00784-013-0963-x
Burke FM, Samarawickrama DY (1995) Progressive changes in the pulpo-dentinal complex and their clinical consequences. Gerodontology 12:57–66. https://doi.org/10.1111/j.1741-2358.1995.tb00132.x
Gautam S, Galgali SR, Sheethal HS, Priya NS (2017) Pulpal changes associated with advanced periodontal disease: a histopathological study. J Oral Maxillofac Pathol 21:58–63. https://doi.org/10.4103/0973-029X.203795
Fatemi K, Disfani R, Zare R, Moeintaghavi A, Ali SA, Boostani HR (2012) Influence of moderate to severe chronic periodontitis on dental pulp. J Indian Soc of Periodontol 16:558–561. https://doi.org/10.4103/0972-124X.106911
Czarnecki RT, Schilder H (1979) A histological evaluation of the human pulp in teeth with varying degrees of periodontal disease. J Endod 5:242–253. https://doi.org/10.1016/S0099-2399(79)80018-7
Torabinejad M, Kiger RD (1985) A histologic evaluation of dental pulp tissue of a patient with periodontal disease. Oral Surg Oral Med Oral Pathol 59:198–200. https://doi.org/10.1016/0030-4220(85)90018-0
Tang L, Sun TQ, Gao XJ, Zhou XD, Huang DM (2011) Tooth anatomy risk factors influencing root canal working length accessibility. Int J Oral Sci 3:135–140. https://doi.org/10.4248/IJOS11050
Wu D, Shi W, Wu J, Wu Y, Liu W, Zhu Q (2011) The clinical treatment of complicated root canal therapy with the aid of a dental operating microscope. Int Dent J 61:261–266. https://doi.org/10.1111/j.1875-595X.2011.00070.x
Akerblom A, Hasselgren G (1988) The prognosis for endodontic treatment of obliterated root canals. J Endod 14:565–567. https://doi.org/10.1016/s0099-2399(88)80092-x
Kiefner P, Connert T, ElAyouti A, Weiger R (2017) Treatment of calcified root canals in elderly people: a clinical study about the accessibility, the time needed and the outcome with a three-year follow-up. Gerodontology 34:164–170. https://doi.org/10.1111/ger.12238
Ordinola-Zapata R, Martins JNR, Plascencia H, Versiani MA, Bramante CM (2020) The MB3 canal in maxillary molars: a micro-CT study. Clin Oral Invest 24:4109–4121. https://doi.org/10.1007/s00784-020-03284-7
Yoshioka T, Kikuchi I, Fukumoto Y, Kobayashi C (2005) Suda H (2005) Detection of the second mesiobuccal canal in mesiobuccal roots of maxillary molar teeth ex vivo. Int Endod J 38:124–128. https://doi.org/10.1111/j.1365-2591.2004.00918.x
Costa FFNP, Pacheco-Yanes J, Siqueira JF Jr, Oliveira ACS, Gazzaneo I, Amorim CA, Santos PHB, Alves FR (2019) Association between missed canals and apical periodontitis. Int Endod J 52:400–406. https://doi.org/10.1111/iej.13022
do Carmo WD, Verner FS, Aguiar LM, Visconti MA, Ferreira MD, Lacerda MFLS, Junqueira RB (2021) Missed canals in endodontically treated maxillary molars of a Brazilian subpopulation: prevalence and association with periapical lesion using cone-beam computed tomography. Clin Oral Investig 25:2317–2323. https://doi.org/10.1007/s00784-020-03554-4
Karabucak B, Bunes A, Chehoud C, Kohli MR, Setzer F (2016) Prevalence of apical periodontitis in endodontically treated premolars and molars with untreated canal: a cone-beam computed tomography study. J Endod 42:538–541. https://doi.org/10.1016/j.joen.2015.12.026
Coutinho-Filho TS, Gurgel-Filho ED, Souza-Filho FJ, Silva EJNL (2012) Preliminary investigation to achieve patency of MB2 canal in maxillary molars. Braz J Oral Sci 11:373–376
Shi X, Zhao S, Wang W, Jiang Q, Yang X (2018) Novel navigation technique for the endodontic treatment of a molar with pulp canal calcification and apical pathology. Aust Endod J 44:66–70. https://doi.org/10.1111/aej.12207
Jain SD, Carrico CK, Bermanis I (2020) 3-Dimensional accuracy of dynamic navigation technology in locating calcified canals. J Endod 46:839–845. https://doi.org/10.1016/j.joen.2020.03.014
Funding
This study was supported by the Scientific and Technological Research Council of Turkey-TUBİTAK (grant no. 117S139).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval
The study protocol was approved by the local university clinical research ethical board with the approval number KAEK 2015/408.
Informed consent
Informed consent was obtained from each patient.
Conflict of interest
The authors declare that there is no conflict of interest.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Keleş, A., Keskin, C. & Versiani, M.A. Micro-CT assessment of radicular pulp calcifications in extracted maxillary first molar teeth. Clin Oral Invest 26, 1353–1360 (2022). https://doi.org/10.1007/s00784-021-04109-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-021-04109-x