Abstract
Objectives
This study aimed to assess the effects of revascularisation and apexification procedures on biomechanical behaviour of immature teeth using 3-dimensional finite element analysis (3D FEA).
Materials and methods
Five 3D FEA permanent maxillary incisor models were developed from CBCT scans and available literature data: Model MT: Mature tooth, Model IT: Immature tooth (Cvek’s stage 3), Model AT: Apexified tooth-mineral trioxide aggregate (MTA) apexification, Model RTB: Revascularised tooth with blood, and Model RTS: Revascularised tooth with supplementary scaffold. Using FEA, a masticatory load of 240N at 120° was simulated, and the Von Mises and maximum principal stresses within the models were evaluated. Failure index (FI) and weakening% were also calculated for each model.
Results
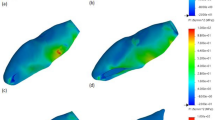
On dentinal stress analysis, model MT (96.16MPa) and IT (158.38MPa) had lowest and highest stress values, respectively. Among the experimental groups, model RTS (131.12MPa) had lower stresses than AT (136.33MPa) and RTB (133.7MPa), with no significant difference among the three. Peak dentinal stresses in all the models were observed in the cervical third of the root and near the apical opening in model IT. The extent of high dentinal stress area in model RTB and RTS was lesser than that of AT. The FI and weakening% values were highest for model AT followed by RTB and RTS, among the experimental groups. However, all these treatments strengthened an immature tooth by more than 20%.
Conclusions
AT, RTB, and RTS treatments lowered the stress values and risk of fracture in immature teeth with no significant difference among the three groups.
Clinical relevance
Stress distribution evaluation following revascularisation/apexification was essential, with potential to influence clinical decision-making. MTA apexification and revascularisation with blood clot/supplementary scaffold lowered the stresses in immature teeth, with no significant difference among the three.


Similar content being viewed by others
References
Trope M (2010) Treatment of the immature tooth with a non-vital pulp and apical periodontitis. Dent Clin North Am 54:313–324. https://doi.org/10.1016/j.cden.2009.12.006
Mente J, Hage N, Pfefferle T, Koch MJ, Dreyhaupt J, Staehle HJ, Friedman S (2009) Mineral trioxide aggregate apical plugs in teeth with open apical foramina: a retrospective analysis of treatment outcome. J Endod 35:1354–1358. https://doi.org/10.1016/j.joen.2009.05.025
Iwaya SI, Ikawa M, Kubota M (2001) Revascularization of an immature permanent tooth with apical periodontitis and sinus tract. Dent Traumatol 17:185–187. https://doi.org/10.1034/j.1600-9657.2001.017004185.x
Chueh LH, Huang GT (2006) Immature teeth with periradicular periodontitis or abscess undergoing apexogenesis: a paradigm shift. J Endod 32:1205–1213. https://doi.org/10.1016/j.joen.2006.07.010
Lolato A, Bucchi C, Taschieri S, Kabbaney AE, Fabbro MD (2016) Platelet concentrates for revitalization of immature necrotic teeth: a systematic review of the clinical studies. Platelets 27:383–392. https://doi.org/10.3109/09537104.2015.1131255
Jiang X, Liu H, Peng C (2017) Clinical and radiographic assessment of the efficacy of a collagen membrane in regenerative endodontics: a randomized, controlled clinical trial. J Endod 43:1465–1471. https://doi.org/10.1016/j.joen.2017.04.011
Martin G, Ricucci D, Gibbs JL, Lin LM (2013) Histological findings of revascularized/revitalized immature permanent molar with apical periodontitis using platelet-rich plasma. J Endod 39:138–144. https://doi.org/10.1016/j.joen.2012.09.015
Lei L, Chen Y, Zhou R, Huang X, Cai Z (2015) Histologic and immunohistochemical findings of a human immature permanent tooth with apical periodontitis after regenerative endodontic treatment. J Endod 41:1172–1179. https://doi.org/10.1016/j.joen.2015.03.012
Ho SP, Yu B, Yun W, Marshall GW, Ryder MI, Marshall SJ (2009) Structure, chemical composition and mechanical properties of human and rat cementum and its interface with root dentin. Acta Biomater 5:707–718. https://doi.org/10.1016/j.actbio.2008.08.013
Nagy MM, Tawfik HE, Hashem AA, Abu-Seida AM (2014) Regenerative potential of immature permanent teeth with necrotic pulps after different regenerative protocols. J Endod 40:192–198. https://doi.org/10.1016/j.joen.2013.10.027
Ulusoy AT, Turedi I, Cimen M, Cehreli ZC (2019) Evaluation of blood clot, platelet-rich plasma, platelet-rich fibrin, and platelet pellet as scaffolds in regenerative endodontic treatment: a prospective randomized trial. J Endod 45:560–566. https://doi.org/10.1016/j.joen.2019.02.002
Kupczik K (2008) Virtual biomechanics: basic concepts and technical aspects of finite element analysis in vertebrate morphology. J Anthropol Sci 86:193–198
Zelic K, Vukicevic A, Jovicic G, Aleksandrovic S, Filipovic N, Djuric M (2015) Mechanical weakening of devitalized teeth: three-dimensional finite element analysis and prediction of tooth fracture. Int Endod J 48:850–863. https://doi.org/10.1111/iej.12381
Cvek M (1992) Prognosis of luxated non-vital maxillary incisors treated with calcium hydroxide and filled with gutta-percha. A retrospective clinical study. Endod Dent Traumatol 8:45–55. https://doi.org/10.1111/j.1600-9657.1992.tb00228.x
Jeeruphan T, Jantarat J, Yanpiset K, Suwannapan L, Khewsawai P, Hargreaves KM (2012) Mahidol study 1: comparison of radiographic and survival outcomes of immature teeth treated with either regenerative endodontic or apexification methods: a retrospective study. J Endod 38:1330–1336. https://doi.org/10.1016/j.joen.2012.06.028
Zhang YR, Du W, Zhou XD, Yu HY (2014) Review of research on the mechanical properties of the human tooth. Int J Oral Sci 6:61–69. https://doi.org/10.1038/ijos.2014.21
Rees JS, Jacobsen PH (1993) The elastic moduli of enamel and dentine. Clin Mater 14:35–39. https://doi.org/10.1016/0267-6605(93)90045-9
Lin S-L, Lee S-Y, Lin Y-C, Huang Y-H, Yang J-C, Huang H-M (2014) Evaluation of mechanical and histological properties of cryopreserved human premolars under short-term preservation: a preliminary study. J Dent Sci 9:244–248. https://doi.org/10.1016/j.jds.2013.04.010
Ruse ND (2008) Propagation of erroneous data for the modulus of elasticity of periodontal ligament and gutta percha in FEM/FEA papers: a story of broken links. Dent Mater 24:1717–1719. https://doi.org/10.1016/j.dental.2008.04.006
Weinstein AM, Klawitter JJ, Cook SD (1980) Implant-bone interface characteristic of bioglass dental implants. J Biomed Mater Res 14:23–29. https://doi.org/10.1002/jbm.820140104
Haecker CJ, Garboczi EJ, Bullard JW, Bohn RB, Sun Z, Shah SP, Voigt T (2005) Modeling the linear elastic properties of Portland cement paste. Cem Conc Res 35:1948–1960. https://doi.org/10.1016/j.cemconres.2005.05.001
Sabbagh J, Vreven J, Leloup G (2002) Dynamic and static moduli of elasticity of resin-based materials. Dent Mater 18:64–71. https://doi.org/10.1016/s0109-5641(01)00021-5
Christie TE (1977) Cephalometric patterns of adults with normal occlusion. Angle Orthod 47:128–135. https://doi.org/10.1043/0003-3219(1977)047<0128:CPOAWN>2.0.CO;2
Paphangkorakit J, Osborn JW (1997) The effect of pressure on a maximum incisal bite force in man. Arch Oral Bio 42:11–17. https://doi.org/10.1016/s0003-9969(96)00106-9
Haines DJ (1968) Physical properties of human tooth enamel and enamel sheath material under load. J Biomech 1:117–125. https://doi.org/10.1016/0021-9290(68)90014-6
Carvalho RM, Santiago SL, Fernandes CA, Suh BI, Pashley DH (2000) Effects of prism orientation on tensile strength of enamel. J Adhes Dent 2:251–257
Sano H, Ciucchi B, Matthews WG, Pashley DH (1994) Tensile properties of mineralized and demineralized human and bovine dentin. J Dent Res 73:1205–1211. https://doi.org/10.1177/00220345940730061201
Nalla RK, Kinney JH, Marshall SJ, Ritchie RO (2004) On the in vitro fatigue behavior of human dentin: effect of mean stress. J Dent Res 83:211–215. https://doi.org/10.1177/154405910408300305
Gateno J, Xia J, Teichgraeber JF, Rosen A (2003) A new technique for the creation of a computerized composite skull model. J Oral Maxillofac Surg 61:222–227. https://doi.org/10.1053/joms.2003.50033
Choi AH, Conway RC, Ben-Nissan B (2014) Finite-element modeling and analysis in nanomedicine and dentistry. Nanomedicine (London) 9:1681–1695. https://doi.org/10.2217/nnm.14.75
Wilson S, Smith GA, Preisch J, Casamassimo PS (1997) Epidemiology of dental trauma treated in an urban pediatric emergency department. Pediatr Emerg Care 13:12–15. https://doi.org/10.1097/00006565-199702000-00004
Pietrzak G, Curnier A, Botsis J, Scherrer S, Wiskott A, Belser U (2002) A nonlinear elastic model of the periodontal ligament and its numerical calibration for the study of tooth mobility. Comput Methods Biomech Biomed Engin 5:91–100. https://doi.org/10.1080/10255840290032117
Goel VK, Khera SC, Gurusami S, Chen RCS (1992) Effect of cavity depth on stresses in a restored tooth. J Prosthet Dent 67:174–183. https://doi.org/10.1016/0022-3913(92)90449-k
Fill TS, Carey JP, Toogood RW, Major PW (2011) Experimentally determined mechanical properties of, and models for, the periodontal ligament: critical review of current literature. J Dent Biomech 2011:312980. https://doi.org/10.4061/2011/312980
Belli S, Eraslan O, Eskitascioglu G (2016) Effect of root filling on stress distribution in premolars with endodontic-periodontal lesion: a finite elemental analysis study. J Endod 42:150–155. https://doi.org/10.1016/j.joen.2015.09.010
Poiate IA, Vasconcellos AB, Poiate Junior E, Dias KR (2009) Stress distribution in the cervical region of an upper central incisor in a 3D finite element model. Braz Oral Res 23:161–168. https://doi.org/10.1590/s1806-83242009000200012
Geramy A, Sharafoddin F (2003) Abfraction: 3D analysis by means of the finite element method. Quintessence Int 34:526–533
Jamshidi D, Homayouni H, Majd NM, Shahabi S, Arvin A, Omidi BR (2018) Impact and fracture strength of simulated immature teeth treated with mineral trioxide aggregate apical plug and fiber post versus revascularization. J Endod 44:1878–1882. https://doi.org/10.1016/j.joen.2018.09.008
Torabinejad M, Nosrat A, Verma P, Udochukwu O (2017) Regenerative endodontic treatment or mineral trioxide aggregate apical plug in teeth with necrotic pulps and open apices: a systematic review and meta-analysis. J Endod 43:1806–1820. https://doi.org/10.1016/j.joen.2017.06.029
Brito-Júnior M, Pereira RD, Veríssimo C, Soares CJ, Faria-e-Silva AL, Camilo CC, Sousa-Neto MD (2014) Fracture resistance and stress distribution of simulated immature teeth after apexification with mineral trioxide aggregate. Int Endod J 47:958–966. https://doi.org/10.1111/iej.12241
Bucchi C, Marcé-Nogué J, Galler KM, Widbiller M (2019) Biomechanical performance of an immature maxillary central incisor after revitalization: a finite element analysis. Int Endod J 52:1508–1518. https://doi.org/10.1111/iej.13159
Belli S, Eraslan O, Eskitaşcıoğlu G (2018) Effect of different treatment options on biomechanics of immature teeth: a finite element stress analysis study. J Endod 44:475–479. https://doi.org/10.1016/j.joen.2017.08.037
Wang XJ, Thibodeau B, Trope M, Lin LM, Huang GT (2010) Histologic characterization of regenerated tissues in canal space after the revitalization/revascularization procedure of immature dog teeth with apical periodontitis. J Endod 36:56–63. https://doi.org/10.1016/j.joen.2009.09.039
Rasmussen S, Patchin R, Scott DB, Heuer AH (1976) Fracture properties of human enamel and dentin. J Dent Res 55:154–164. https://doi.org/10.1177/00220345760550010901
Kim SG, Malek M, Sigurdsson A, Lin LM, Kahler B (2018) Regenerative endodontics: a comprehensive review. Int Endod J 51:1367–1388. https://doi.org/10.1111/iej.12954
Demİrel A, Bezgİn T, Sari Ş (2020) Effects of root maturation and thickness variation in coronal mta plugs under traumatic load on stress distribution in regenerative endodontic procedures: A 3D FEA study. J Endod. 47:492–499.e4. https://doi.org/10.1016/j.joen.2020.11.006
Funding
This study was funded by the Indian Council of Medical Research via the “MD/MS/DM/MCh/MDS support” grant.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Data collection, model, and result analysis were performed by Persis Anthrayose under the guidance of Ruchika Roongta Nawal, Seema Yadav, Sangeeta Talwar and Sudha Yadav. The first draft of the manuscript was written by Persis Anthrayose, and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval
This article does not contain any procedures with human participants or animals performed by any of the authors. The study was approved by the Ethics Committee of Maulana Azad Institute of Dental Sciences (Ref No- MAIDS/ Ethical Committee/ 09,2018). All applicable international, national, and/or institutional guidelines were followed.
Informed consent
For this type of study, formal consent is not required.
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
ESM 1
(PDF 167 kb)
Rights and permissions
About this article
Cite this article
Anthrayose, P., Nawal, R.R., Yadav, S. et al. Effect of revascularisation and apexification procedures on biomechanical behaviour of immature maxillary central incisor teeth: a three-dimensional finite element analysis study. Clin Oral Invest 25, 6671–6679 (2021). https://doi.org/10.1007/s00784-021-03953-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-021-03953-1