Abstract
Objectives
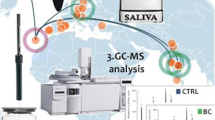
Endogenous substances have been analyzed in biological samples in order to be related with metabolic dysfunctions and diseases. The study aimed to investigate profiles of volatile organic compounds (VOCs) from fresh and incubated saliva donated by healthy controls, individuals with oral tissue lesions and with oral cancer, in order to assess case-specific biomarkers of oxidative stress.
Materials and methods
VOCs were pre-concentrated using headspace-solid phase microextraction and analyzed using gas chromatography-mass spectrometry. Then, VOCs positively modulated by incubation process were subtracted, yielding profiles with selected features. Principal component analysis and hierarchical cluster analysis were used to inspect data distribution, while univariate statistics was applied to indicate potential markers of oral cancer. Machine learning algorithm was implemented, aiming multiclass prediction.
Results
The removal of bacterial contribution to VOC profiles allowed the obtaining of more specific case-related patterns. Artificial neural network model included 9 most relevant compounds (1-octen-3-ol, hexanoic acid, E-2-octenal, heptanoic acid, octanoic acid, E-2-nonenal, nonanoic acid, 2,4-decadienal and 9-undecenoic acid). Model performance was assessed using 10-fold cross validation and receiver operating characteristic curves. Obtained overall accuracy was 90%. Oral cancer cases were predicted with 100% of sensitivity and specificity.
Conclusions
The selected VOCs were ascribed to lipid oxidation mechanism and presented potential to differentiate oral cancer from other inflammatory conditions.
Clinical relevance
These results highlight the importance of interpretation of saliva composition and the clinical value of salivary VOCs. Elucidated metabolic alterations have the potential to aid the early detection of oral cancer and the monitoring of oral lesions.









Similar content being viewed by others
References
Clish CB (2015) Metabolomics: an emerging but powerful tool for precision medicine. Mol Case Stud 1:a000588. https://doi.org/10.1101/mcs.a000588
Sandlers Y (2017) The future perspective: metabolomics in laboratory medicine for inborn errors of metabolism. Transl Res 189:65–75. https://doi.org/10.1016/j.trsl.2017.06.005
Buszewski B, Kęsy M, Ligor T, Amann A (2007) Human exhaled air analytics: biomarkers of diseases. Biomed Chromatogr 21:553–566. https://doi.org/10.1002/bmc.835
Hakim M, Broza YY, Barash O, Peled N, Phillips M, Amann A, Haick H (2012) Volatile organic compounds of lung cancer and possible biochemical pathways. Chem Rev 112:5949–5966. https://doi.org/10.1021/cr300174a
Monedeiro F, dos Reis RB, Peria FM, Sares CTG, de Martinis BS (2020) Investigation of sweat VOC profiles in assessment of cancer biomarkers using HS-GC-MS. J Breath Res 14:026009. https://doi.org/10.1088/1752-7163/ab5b3c
Liguori I, Russo G, Curcio F, Bulli G, Aran L, Della-Morte D, Gargiulo G, Testa G, Cacciatore F, Bonaduce D, Abete P (2018) Oxidative stress, aging, and diseases. Clin Interv Aging 13:757–772. https://doi.org/10.2147/CIA.S158513
Khanna H, Karki K, Pande D, et al (2014) Inflammation, free radical damage, Oxidative Stress and Cancer Interdiscip J Microinflammation 01: https://doi.org/10.4172/ijm.1000109
Davies K (2001) Oxidative stress, antioxidant defenses, and damage removal, repair, and replacement systems. IUBMB Life 50:279–289. https://doi.org/10.1080/713803728
Frijhoff J, Winyard PG, Zarkovic N, Davies SS, Stocker R, Cheng D, Knight AR, Taylor EL, Oettrich J, Ruskovska T, Gasparovic AC, Cuadrado A, Weber D, Poulsen HE, Grune T, Schmidt HHHW, Ghezzi P (2015) Clinical relevance of biomarkers of oxidative stress. Antioxid Redox Signal 23:1144–1170. https://doi.org/10.1089/ars.2015.6317
Ferlay J, Colombet M, Soerjomataram I, Mathers C, Parkin DM, Piñeros M, Znaor A, Bray F (2019) Estimating the global cancer incidence and mortality in 2018: GLOBOCAN sources and methods. Int J Cancer 144:1941–1953. https://doi.org/10.1002/ijc.31937
Neville BW, Day TA (2002) Oral Cancer and precancerous lesions. CA Cancer J Clin 52:195–215. https://doi.org/10.3322/canjclin.52.4.195
Rivera C (2015) Essentials of oral cancer. Int J Clin Exp Pathol 8:11884–11894. https://doi.org/10.5281/zenodo.192487
van der Waal I, de Bree R, Brakenhoff R, Coebergh J (2011) Early diagnosis in primary oral cancer: is it possible? Med Oral Patol Oral Cir Bucal 16:e300–e305. https://doi.org/10.4317/medoral.16.e300
Pfaffe T, Cooper-White J, Beyerlein P, Kostner K, Punyadeera C (2011) Diagnostic potential of saliva: current state and future applications. Clin Chem 57:675–687. https://doi.org/10.1373/clinchem.2010.153767
Milanowski M, Pomastowski P, Ligor T, Buszewski B (2017) Saliva – volatile biomarkers and profiles. Crit Rev Anal Chem 47:251–266. https://doi.org/10.1080/10408347.2016.1266925
Caporossi L, Santoro A, Papaleo B (2010) Saliva as an analytical matrix: state of the art and application for biomonitoring. Biomarkers 15:475–487. https://doi.org/10.3109/1354750X.2010.481364
Bosch JA (2014) The use of saliva markers in psychobiology: mechanisms and methods. In: Monographs in Oral Science. S. Karger AG, pp. 99–108
Chiappin S, Antonelli G, Gatti R, De Palo EF (2007) Saliva specimen: a new laboratory tool for diagnostic and basic investigation. Clin Chim Acta 383:30–40. https://doi.org/10.1016/j.cca.2007.04.011
Bhattarai KR, Kim H-R, Chae H-J (2018) Compliance with saliva collection protocol in healthy volunteers: strategies for managing risk and errors. Int J Med Sci 15:823–831. https://doi.org/10.7150/ijms.25146
Buszewski B, Milanowski M, Ligor T, Pomastowski P (2017) Investigation of bacterial viability from incubated saliva by application of flow cytometry and hyphenated separation techniques. Electrophoresis 38:2081–2088. https://doi.org/10.1002/elps.201700057
Monedeiro F, Milanowski M, Ratiu I-A, Zmysłowski H, Ligor T, Buszewski B (2019) VOC profiles of saliva in assessment of halitosis and submandibular abscesses using HS-SPME-GC/MS technique. Molecules 24:2977. https://doi.org/10.3390/molecules24162977
Roager HM, Licht TR (2018) Microbial tryptophan catabolites in health and disease. Nat Commun 9:3294. https://doi.org/10.1038/s41467-018-05470-4
Audrain B, Farag MA, Ryu CM, Ghigo JM (2015) Role of bacterial volatile compounds in bacterial biology. FEMS Microbiol Rev 39:222–233. https://doi.org/10.1093/femsre/fuu013
Denawaka CJ, Fowlis IA, Dean JR (2016) Source, impact and removal of malodour from soiled clothing. J Chromatogr A 1438:216–225. https://doi.org/10.1016/j.chroma.2016.02.037
Schulz S, Dickschat JS (2007) Bacterial volatiles: the smell of small organisms. Nat Prod Rep 24:814–842. https://doi.org/10.1039/b507392h
Windey K, De Preter V, Verbeke K (2012) Relevance of protein fermentation to gut health. Mol Nutr Food Res 56:184–196. https://doi.org/10.1002/mnfr.201100542
Montel MC, Masson F, Talon R (1998) Bacterial role in flavour development. Meat Sci 49:S111–S123. https://doi.org/10.1016/S0309-1740(98)90042-0
Lamberet G, Auberger B, Bergère JL (1997) Aptitude of cheese bacteria for volatile S -methyl thioester synthesis I. effect of substrates and pH on their formation by Brevibacterium linens GC171. Appl Microbiol Biotechnol 47:279–283. https://doi.org/10.1007/s002530050927
Sourabié AM, Spinnler H-E, Bourdat-Deschamps M, Tallon R, Landaud S, Bonnarme P (2012) S-methyl thioesters are produced from fatty acids and branched-chain amino acids by brevibacteria: focus on l-leucine catabolic pathway and identification of acyl–CoA intermediates. Appl Microbiol Biotechnol 93:1673–1683. https://doi.org/10.1007/s00253-011-3500-3
Mayank R, Ranjan A, Moholkar VS (2013) Mathematical models of ABE fermentation: review and analysis. Crit Rev Biotechnol 33:419–447. https://doi.org/10.3109/07388551.2012.726208
Russmayer H, Marx H, Sauer M (2019) Microbial 2-butanol production with Lactobacillus diolivorans. Biotechnol Biofuels 12:262. https://doi.org/10.1186/s13068-019-1594-5
Milanowski M, Monedeiro F, Złoch M, Ratiu IA, Pomastowski P, Ligor T, de Martinis BS, Buszewski B (2019) Profiling of VOCs released from different salivary bacteria treated with non-lethal concentrations of silver nitrate. Anal Biochem 578:36–44. https://doi.org/10.1016/j.ab.2019.05.007
Hazelwood LA, Daran J-M, van Maris AJA, Pronk JT, Dickinson JR (2008) The Ehrlich pathway for fusel alcohol production: a century of research on Saccharomyces cerevisiae metabolism. Appl Environ Microbiol 74:2259–2266. https://doi.org/10.1128/AEM.02625-07
Rojo F (2009) Degradation of alkanes by bacteria. Environ Microbiol 11:2477–2490. https://doi.org/10.1111/j.1462-2920.2009.01948.x
Kotani T, Kawashima Y, Yurimoto H, Kato N, Sakai Y (2006) Gene structure and regulation of alkane monooxygenases in propane-utilizing Mycobacterium sp. TY-6 and Pseudonocardia sp. TY-7. J Biosci Bioeng 102:184–192. https://doi.org/10.1263/jbb.102.184
Schulz H (1991) Beta oxidation of fatty acids. Biochim Biophys Acta - Lipids Lipid Metab 1081:109–120. https://doi.org/10.1016/0005-2760(91)90015-A
Swinnen JV, Brusselmans K, Verhoeven G (2006) Increased lipogenesis in cancer cells: new players, novel targets. Curr Opin Clin Nutr Metab Care 9:358–365. https://doi.org/10.1097/01.mco.0000232894.28674.30
Zaidi N, Lupien L, Kuemmerle NB, Kinlaw WB, Swinnen JV, Smans K (2013) Lipogenesis and lipolysis: the pathways exploited by the cancer cells to acquire fatty acids. Prog Lipid Res 52:585–589. https://doi.org/10.1016/j.plipres.2013.08.005
Jelski W, Szmitkowski M (2008) Alcohol dehydrogenase (ADH) and aldehyde dehydrogenase (ALDH) in the cancer diseases. Clin Chim Acta 395:1–5. https://doi.org/10.1016/j.cca.2008.05.001
Chocolatewala N, Chaturvedi P, Desale R (2010) The role of bacteria in oral cancer. Indian J Med Paediatr Oncol 31:126–131. https://doi.org/10.4103/0971-5851.76195
Gaonkar P, Patankar S, Tripathi N, Sridharan G (2018) Oral bacterial flora and oral cancer: the possible link? J Oral Maxillofac Pathol 22:234–238. https://doi.org/10.4103/jomfp.JOMFP_89_16
Hooper SJ, Crean S-J, Fardy MJ, Lewis MAO, Spratt DA, Wade WG, Wilson MJ (2007) A molecular analysis of the bacteria present within oral squamous cell carcinoma. J Med Microbiol 56:1651–1659. https://doi.org/10.1099/jmm.0.46918-0
Elfaki I, Mir R, Almutairi FM, Abu Duhier FM (2018) Cytochrome P450: polymorphisms and roles in cancer, diabetes and atherosclerosis. Asian Pac J Cancer Prev 19:2057–2070. https://doi.org/10.22034/APJCP.2018.19.8.2057
Hernando-Rodriguez M, Rey-Barja N, Marichalar-Mendia X, Rodriguez-Tojo MJ, Acha-Sagredo A, Aguirre-Urizar JM (2012) Role of cytochrome P-450 genetic polymorphisms in oral carcinogenesis. J Oral Pathol Med 41:1–8. https://doi.org/10.1111/j.1600-0714.2011.01067.x
Miekisch W, Schubert JK, Noeldge-Schomburg GF (2004) Diagnostic potential of breath analysis—focus on volatile organic compounds. Clin Chim Acta 347:25–39. https://doi.org/10.1016/J.CCCN.2004.04.023
Wurzenberger M, Grosch W (1984) The formation of 1-octen-3-ol from the 10-hydroperoxide isomer of linoleic acid by a hydroperoxide lyase in mushrooms (Psalliota bispora). Biochim Biophys Acta - Lipids Lipid Metab 794:25–30. https://doi.org/10.1016/0005-2760(84)90293-5
Cabre A, Girona J, Vallve J-C et al (2003) Cytotoxic effects of the lipid peroxidation product 2,4-decadienal in vascular smooth muscle cells. Atherosclerosis 169:245–250. https://doi.org/10.1016/S0021-9150(03)00196-5
Haze S, Gozu Y, Nakamura S, Kohno Y, Sawano K, Ohta H, Yamazaki K (2001) 2-Nonenal newly found in human body odor tends to increase with aging. J Invest Dermatol 116:520–524. https://doi.org/10.1046/j.0022-202x.2001.01287.x
Jayasena DD, Ahn DU, Nam KC, Jo C (2013) Flavour chemistry of chicken meat: a review. Asian Australas J Anim Sci 26:732–742. https://doi.org/10.5713/ajas.2012.12619
Schaich KM, Shahidi F, Zhong Y, Eskin NAM (2013) Lipid oxidation. In: Eskin NA, Shahidi F (eds) Biochemistry of foods, 3rd ed. Elsevier, Cambridge, pp 419–478
Park Y-S, Lek S (2016) Artificial neural networks. In: Jørgensen SE (ed) Developments in Environmental Modelling, 1 st. Elsevier B.V., pp 123–140
Beck MW (2018) NeuralNetTools : visualization and analysis tools for neural networks. J Stat Softw 85:1–20. https://doi.org/10.18637/jss.v085.i11
Waris G, Ahsan H (2006) Reactive oxygen species: role in the development of cancer and various chronic conditions. J Carcinog 5:14. https://doi.org/10.1186/1477-3163-5-14
Pereira JAM, Porto-Figueira P, Taware R, Sukul P, Rapole S, Câmara JS (2020) Unravelling the potential of salivary volatile metabolites in oral diseases. A Review. Molecules 25:3098. https://doi.org/10.3390/molecules25133098
Taware R, Taunk K, Pereira JAM, Shirolkar A, Soneji D, Câmara JS, Nagarajaram HA, Rapole S (2018) Volatilomic insight of head and neck cancer via the effects observed on saliva metabolites. Sci Rep 8:17725. https://doi.org/10.1038/s41598-018-35854-x
Shigeyama H, Wang T, Ichinose M, Ansai T, Lee SW (2019) Identification of volatile metabolites in human saliva from patients with oral squamous cell carcinoma via zeolite-based thin-film microextraction coupled with GC–MS. J Chromatogr B 1104:49–58. https://doi.org/10.1016/j.jchromb.2018.11.002
Funding
The work was supported by the Nicolaus Copernicus University. The author has obtained financial resources for conducting scientific research under the research grant for young researchers from abroad awarded by the Rector of the Nicolaus Copernicus University pursuant to Order no. MNZ/03/2019.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Author Fernanda Monedeiro declares that she has no conflict of interest. Author Maciej Monedeiro-Milanowski declares that he has no conflict of interest. Author Hubert Zmysłowski declares that he has no conflict of interest. Author Bruno Spinosa De Martinis declares that he has no conflict of interest. Author Bogusław Buszewski declares that he has no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. The study was approved by the Ethical Committee from the Nicolaus Copernicus University of Toruń (Decision Number KB 323/2017).
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
ESM 1
(DOCX 143 kb)
Rights and permissions
About this article
Cite this article
Monedeiro, F., Monedeiro-Milanowski, M., Zmysłowski, H. et al. Evaluation of salivary VOC profile composition directed towards oral cancer and oral lesion assessment. Clin Oral Invest 25, 4415–4430 (2021). https://doi.org/10.1007/s00784-020-03754-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-020-03754-y