Abstract
Objectives
Pain and trismus are the most common postoperative complications following a surgical removal of the lower third molar. This randomized, double-blind, placebo-controlled clinical trial evaluated the effect of orally administrated magnesium on postoperative pain and trismus after surgical removal of the lower third molars.
Materials and methods
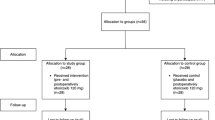
The study was conducted on 80 participants who were divided into two groups. Each group took different oral forms of magnesium citrate. Participants in both groups had their two lower molars surgically removed. For one randomly selected third molar, participants received either magnesium citrate tablets or lozenges. For the surgical removal of the lower third molar of the opposite side, the participants received either placebo tablets or lozenges. The data were analyzed using the Wilcoxon signed-ranked test, the Mann-Whitney U test, and the Spearman rank-order correlation with the level of significance set at p < 0.05. This manuscript was written in accordance with the Consort recommendation.
Results
The results show a statistically significant lower pain level at all tested times (24 h, 48 h, and 72 h postoperatively) for participants who used magnesium preparations in lozenges (p = 0.012, p = 0.013, and p ≤ 0.001) as well as in tablet form (p ≤ 0.001) compared to placebo. The results also show a statistically significant greater mouth opening ability at all tested times (24 h, 48 h, and 72 h postoperatively) between magnesium preparations and the placebo (p ≤ 0.001).
Conclusion
Orally administered magnesium (either lozenges or tablets) before and after a lower third molar surgical removal significantly reduces pain intensity and the degree of trismus in the postoperative period.
Clinical relevance
Based on the results of the study, oral magnesium could be used in the oral and maxillofacial surgery to reduce postoperative complications after surgical removal of the lower third molars.
Trial registration
This study is registered on http:clinicaltrials.gov under protocol no. NCT03398382.


Similar content being viewed by others
References
Marciani RD (2007) Third molar removal: an overview of indications, imaging, evaluation, and assessment of risk. Oral Maxillofac Surg Clin North Am 19:1–13
Jokic D, Macan D, Peric B, Tadic M, Biocic J, Danic P, Brajdic D (2013) Ambulatory oral surgery: 1-year experience with 11680 patients from Zagreb district, Croatia. Croat Med J 54:49–54
Garcia Garcia A, Gude Sampedro F, Gandara Rey J, Gallas Torreira M (1997) Trismus and pain after removal of impacted lower third molars. J Oral Maxillofac Surg 55:1223–1236
Yuasa H, Sugiura M (2004) Clinical postoperative findings after removal of impacted mandibular third molars: prediction of postoperative facial swelling and pain based on preoperative variables. Br J Oral Maxillofac Surg 42:209–214
Baqain ZH, Karaky AA, Sawair F, Khraisat A, Duaibis R, Rajab LD (2008) Frequency estimates and risk factors for postoperative morbidity after third molar removal: a prospective cohort study. J Oral Maxillofac Surg 66:2276–2283
Coulthard P, Bailey E, Esposito M, Furness S, Renton TF, Worthington HV (2014) Surgical techniques for the removal of mandibular wisdom teeth. Cochrane Database Syst Rev:CD004345
Matijevic M, Uzarevic Z, Gvozdic V, Mikelic VM, Leovic D, Macan D (2013) The influence of surgical experience, type of instructions given to patients and patient sex on postoperative pain intensity following lower wisdom tooth surgery. Acta Clin Croat 52:23–28
Bortoluzzi MC, Guollo A, Capella DL (2011) Pain levels after third molar surgical removal: an evaluation of predictive variables. J Contemp Dent Pract 12:239–244
Colorado-Bonnin M, Valmaseda-Castellon E, Berini-Aytes L, Gay-Escoda C (2006) Quality of life following lower third molar removal. Int J Oral Maxillofac Surg 35:343–347
Snyder M, Shugars DA, White RP, Phillips C (2005) Pain medication as an indicator of interference with lifestyle and oral function during recovery after third molar surgery. J Oral Maxillofac Surg 63:1130–1137
Ong CK, Seymour RA (2008) An evidence-based update of the use of analgesics in dentistry. Periodontol 2000(46):143–164
Bamgbose BO, Akinwande JA, Adeyemo WL, Ladeinde AL, Arotiba GT, Ogunlewe MO (2005) Effects of co-administered dexamethasone and diclofenac potassium on pain, swelling and trismus following third molar surgery. Head Face Med 1:11
McGrath C, Comfort MB, Lo EC, Luo Y (2003) Changes in life quality following third molar surgery--the immediate postoperative period. Br Dent J 194:265–268
Kirksey MA, Haskins SC, Cheng J, Liu SS (2015) Local anesthetic peripheral nerve block adjuvants for prolongation of analgesia: a systematic qualitative review. PLoS One 10:e0137312
Danic P, Salaric I, Macan D (2017) New findings on local tramadol use in Oral surgery. Acta Stomatol Croat 51:336–344
Lopez Carriches C, Martinez Gonzalez JM, Donado Rodriguez M (2006) The use of methylprednisolone versus diclofenac in the treatment of inflammation and trismus after surgical removal of lower third molars. Med Oral Patol Oral Cir Bucal 11:E440–E445
Shulman DH, Shipman B, Willis FB (2009) Treating trismus with dynamic splinting: a case report. J Oral Sci 51:141–144
Mezitis M, Rallis G, Zachariades N (1989) The normal range of mouth opening. J Oral Maxillofac Surg 47:1028–1029
Balakrishnan G, Narendar R, Kavin T, Venkataraman S, Gokulanathan S (2017) Incidence of trismus in transalveolar extraction of lower third molar. J Pharm Bioallied Sci 9:S222–S227
Pathak S, Vashisth S, Mishra S, Singh SP, Sharma S (2014) Grading of extraction and its relationship with post-operative pain and trismus, along with proposed grading for trismus. J Clin Diagn Res 8:ZC09–ZC11
Pedersen A (1985) Interrelation of complaints after removal of impacted mandibular third molars. Int J Oral Surg 14:241–244
Konrad M, Schlingmann KP, Gudermann T (2004) Insights into the molecular nature of magnesium homeostasis. Am J Physiol Renal Physiol 286:F599–F605
Guerrera MP, Volpe SL, Mao JJ (2009) Therapeutic uses of magnesium. Am Fam Physician 80:157–162
Workinger JL, Doyle RP, Bortz J (2018) Challenges in the diagnosis of magnesium status. Nutrients 10(9):1202
Institute of Medicine (US) Standing Committee on the Scientific Evaluation of Dietary Reference Intakes (1997) Dietary reference intakes for calcium, phosphorus, magnesium, vitamin D, and fluoride. The National Academies Collection: Reports funded by National Institutes of Health. Washington, DC
Walker AF, Marakis G, Christie S, Byng M (2003) Mg citrate found more bioavailable than other Mg preparations in a randomised, double-blind study. Magnes Res 16:183–191
Wilimzig C, Latz R, Vierling W, Mutschler E, Trnovec T, Nyulassy S (1996) Increase in magnesium plasma level after orally administered trimagnesium dicitrate. Eur J Clin Pharmacol 49:317–323
Kara H, Sahin N, Ulusan V, Aydogdu T (2002) Magnesium infusion reduces perioperative pain. Eur J Anaesthesiol 19:52–56
Ryu JH, Kang MH, Park KS, Do SH (2008) Effects of magnesium sulphate on intraoperative anaesthetic requirements and postoperative analgesia in gynaecology patients receiving total intravenous anaesthesia. Br J Anaesth 100:397–403
Schulz-Stubner S, Wettmann G, Reyle-Hahn SM, Rossaint R (2001) Magnesium as part of balanced general anaesthesia with propofol, remifentanil and mivacurium: a double-blind, randomized prospective study in 50 patients. Eur J Anaesthesiol 18:723–729
Na HS, Ryu JH, Do SH (2011) The role of magnesium in pain. In: Vink R, Nechifor M, editors. Magnesium in the central nervous system [internet]. Adelaide (AU): University of Adelaide Press; 2011. Available from: https://www.ncbi.nlm.nih.gov/books/NBK507245/
Dickenson AH (1995) Spinal cord pharmacology of pain. Br J Anaesth 75:193–200
McCartney CJ, Sinha A, Katz J (2004) A qualitative systematic review of the role of N-methyl-D-aspartate receptor antagonists in preventive analgesia. Anesth Analg 98:1385–1400
Carlton SM, Zhou S, Coggeshall RE (1998) Evidence for the interaction of glutamate and NK1 receptors in the periphery. Brain Res 790:160–169
Borazan H, Kececioglu A, Okesli S, Otelcioglu S (2012) Oral magnesium lozenge reduces postoperative sore throat: a randomized, prospective, placebo-controlled study. Anesthesiology 117:512–518
Yousef AA, Al-deeb AE (2013) A double-blinded randomised controlled study of the value of sequential intravenous and oral magnesium therapy in patients with chronic low back pain with a neuropathic component. Anaesthesia 68:260–266
Jager-Wittenaar H, Dijkstra PU, Vissink A, van Oort RP, Roodenburg JL (2009) Variation in repeated mouth-opening measurements in head and neck cancer patients with and without trismus. Int J Oral Maxillofac Surg 38:26–30
Weber C, Dommerich S, Pau HW, Kramp B (2010) Limited mouth opening after primary therapy of head and neck cancer. Oral Maxillofac Surg 14:169–173
Bondok RS, Abd El-Hady AM (2006) Intra-articular magnesium is effective for postoperative analgesia in arthroscopic knee surgery. Br J Anaesth 97:389–392
Ghezel-Ahmadi V, Ghezel-Ahmadi D, Schirren J, Tsapopiorgas C, Beck G, Bolukbas S (2019) Perioperative systemic magnesium sulphate to minimize acute and chronic post-thoracotomy pain: a prospective observational study. J Thorac Dis 11:418–426
Taheri A, Haryalchi K, Mansour Ghanaie M, Habibi Arejan N (2015) Effect of low-dose (single-dose) magnesium sulfate on postoperative analgesia in hysterectomy patients receiving balanced general anesthesia. Anesthesiol Res Pract 2015:306145
Ryu JH, Sohn IS, Do SH (2009) Controlled hypotension for middle ear surgery: a comparison between remifentanil and magnesium sulphate. Br J Anaesth 103:490–495
Seyhan TO, Tugrul M, Sungur MO, Kayacan S, Telci L, Pembeci K, Akpir K (2006) Effects of three different dose regimens of magnesium on propofol requirements, haemodynamic variables and postoperative pain relief in gynaecological surgery. Br J Anaesth 96:247–252
Oguzhan N, Gunday I, Turan A (2008) Effect of magnesium sulfate infusion on sevoflurane consumption, hemodynamics, and perioperative opioid consumption in lumbar disc surgery. J Opioid Manag 4:105–110
Vlok R, Melhuish TM, Chong C, Ryan T, White LD (2017) Adjuncts to local anaesthetics in tonsillectomy: a systematic review and meta-analysis. J Anesth 31:608–616
Shetty KP, Satish SV, Kilaru KR, Sardar P, Luke AM (2015) Comparison of anesthetic efficacy between lidocaine with and without magnesium sulfate USP 50% for inferior alveolar nerve blocks in patients with symptomatic irreversible pulpitis. J Endod 41:431–433
Sirvinskas E, Laurinaitis R (2002) Use of magnesium sulfate in anesthesiology. Medicina (Kaunas) 38:695–698
Potter JD, Robertson SP, Johnson JD (1981) Magnesium and the regulation of muscle contraction. Fed Proc 40:2653–6265
Ceneviva GD, Thomas NJ, Kees-Folts D (2003) Magnesium sulfate for control of muscle rigidity and spasms and avoidance of mechanical ventilation in pediatric tetanus. Pediatr Crit Care Med 4:480–484
Sonna LA, Hirshman CA, Croxton TL (1996) Role of calcium channel blockade in relaxation of tracheal smooth muscle by extracellular Mg2+. Am J Phys 271:L251–L257
Eby GA (2006) Rescue treatment and prevention of asthma using magnesium throat lozenges: hypothesis for a mouth-lung biologically closed electric circuit. Med Hypotheses 67:1136–1141
D'Angelo EK, Singer HA, Rembold CM (1992) Magnesium relaxes arterial smooth muscle by decreasing intracellular Ca2+ without changing intracellular Mg2+. J Clin Invest 89:1988–1994
Chiu HY, Yeh TH, Huang YC, Chen PY (2016) Effects of intravenous and oral magnesium on reducing migraine: a meta-analysis of randomized controlled trials. Pain Physician 19:E97–E112
Funding
This study was funded by the researcher himself.
Author information
Authors and Affiliations
Contributions
All authors contributed to the data collection and analysis, the writing of this article, and the approval of the final version for publication.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest.
Ethical approval
The protocol of the study was reviewed and approved by the Ethics Committee of the School of Dental Medicine, Zagreb, Croatia (No. 05-PA-15-3/2017). The study was conducted by the ethical standards of the institutional research committee and the 1964 Declaration of Helsinki and its later amendments or comparable ethical standards.
Informed consent
All participants gave their informed consent before they were included in the study.
Consent to submit the manuscript
Consent to submit has been received from all authors.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Jerkovic, D., Tadin, A., Gavic, L. et al. Effect of orally administered magnesium on postoperative pain level and trismus after surgical removal of the lower third molars: a randomized, double-blind, placebo-controlled trial. Clin Oral Invest 24, 4649–4659 (2020). https://doi.org/10.1007/s00784-020-03335-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-020-03335-z