Abstract
Objectives
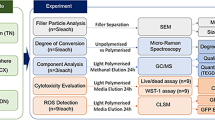
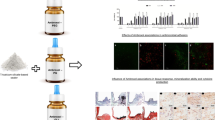
Due to incomplete curing and material degradation, cells in the oral cavity may be exposed to monomers and filler particles from dental composite fillings. The objective of the present study was to investigate if combined exposures to particles and a methacrylate monomer from composite fillings resulted in additive effects on the macrophage immune response.
Material and methods
Two filler particles, Nanosilica (12 nm) and Quartz (1 μm), were studied at concentrations 0.5–4 μg/cm2, while the methacrylate monomer triethyleneglycol dimethacrylate (TEGDMA) was applied at 5 and 50 μM. RAW 264.7 macrophages were exposed to monomers and/or particles for 24 h, with a subsequent 24 h combined exposure to monomers and/or particles and the bacterial factor lipopolysaccharide (LPS) to stimulate an immune response. Release of the pro-inflammatory cytokines interleukin-1β (IL-1β) and tumor necrosis factor-α (TNF-α) were measured as well as the cellular viability.
Results
Co-exposure to Nanosilica and Quartz resulted in an additive attenuation of the LPS-induced IL-1β release. Moreover, co-exposure to TEGDMA and both types of filler particles also resulted in an additive attenuation, although with a weak synergistic trend. The cellular viability and TNF-α release were not significantly affected by the exposures.
Conclusion
The present findings emphasize the necessity of considering effects of combined exposure to dental degradation products in future risk assessments.
Clinical relevance
Attenuated cytokine release could have implications for the macrophage immune response and result in impaired bacterial clearance. Further studies are necessary to determine implications for formation of dental biofilms and caries development.





Similar content being viewed by others
References
Madianos PN, Bobetsis YA, Kinane DF (2005) Generation of inflammatory stimuli: how bacteria set up inflammatory responses in the gingiva. J Clin Periodontol 32(Suppl 6):57–71
Ara T, Kurata K, Hirai K, Uchihashi T, Uematsu T, Imamura Y, Furusawa K, Kurihara S, Wang PL (2009) Human gingival fibroblasts are critical in sustaining inflammation in periodontal disease. J Periodontal Res 44:21–27
Roberts HC, Moseley R, Sloan AJ, Youde SJ, Waddington RJ (2008) Lipopolysaccharide alters decorin and biglycan synthesis in rat alveolar bone osteoblasts: consequences for bone repair during periodontal disease. Eur J Oral Sci 116:207–216
Sun Y, Shu R, Li CL, Zhang MZ (2010) Gram-negative periodontal bacteria induce the activation of Toll-like receptors 2 and 4, and cytokine production in human periodontal ligament cells. J Periodontol 81:1488–1496
Glauser MP (1996) The inflammatory cytokines. New developments in the pathophysiology and treatment of septic shock. Drugs 52(Suppl 2):9–17
Sun Y, Li H, Yang MF, Shu W, Sun MJ, Xu Y (2012) Effects of Aging on Endotoxin Tolerance Induced by Lipopolysaccharides derived from Porphyromonas gingivalis and Escherichia coli. PloS ONE 7:e39224
Hopkins SJ (2003) The pathophysiological role of cytokines. Legal Med 5(Suppl 1):S45–S57
Mizgerd JP, Spieker MR, Doerschuk CM (2001) Early response cytokines and innate immunity: essential roles for TNF receptor 1 and type I IL-1 receptor during Escherichia coli pneumonia in mice. J Immunol 166:4042–4048
Fortin D, Vargas MA (2000) The spectrum of composites: new techniques and materials. J Am Dent Assoc 131(Suppl):26S–30S
Chen MH (2010) Update on dental nanocomposites. J Dent Res 89:549–560
Van Landuyt KL, Nawrot T, Geebelen B, De Munck J, Snauwaert J, Yoshihara K, Scheers H, Godderis L, Hoet P, Van Meerbeek B (2011) How much do resin-based dental materials release? A meta-analytical approach. Dent Mater 27:723–747
Pelka M, Distler W, Petschelt A (1999) Elution parameters and HPLC-detection of single components from resin composite. Clin Oral Investig 3:194–200
Shin MA, Drummond JL (1999) Evaluation of chemical and mechanical properties of dental composites. J Biomed Mater Res 48:540–545
Beyth N, Bahir R, Matalon S, Domb AJ, Weiss EI (2008) Streptococcus mutans biofilm changes surface-topography of resin composites. Dent Mater 24:732–736
Helmis CG, Tzoutzas J, Flocas HA, Halios CH, Stathopoulou OI, Assimakopoulos VD, Panis V, Apostolatou M, Sgouros G, Adam E (2007) Indoor air quality in a dentistry clinic. Sci Total Environ 377:349–365
Krifka S, Petzel C, Hiller KA, Frank EM, Bosl C, Spagnuolo G, Reichl FX, Schmalz G, Schweikl H (2010) Resin monomer-induced differential activation of MAP kinases and apoptosis in mouse macrophages and human pulp cells. Biomaterials 31:2964–2975
Noda M, Wataha JC, Lockwood PE, Volkmann KR, Kaga M, Sano H (2003) Sublethal, 2-week exposures of dental material components alter TNF-alpha secretion of THP-1 monocytes. Dent Mater 19:101–105
Bolling AK, Samuelsen JT, Morisbak E, Ansteinsson V, Becher R, Dahl JE, Mathisen GH (2013) Dental monomers inhibit LPS-induced cytokine release from the macrophage cell line RAW264.7. Toxicol Lett 216:130–138
Amakawa K, Terashima T, Matsuzaki T, Matsumaru A, Sagai M, Yamaguchi K (2003) Suppressive effects of diesel exhaust particles on cytokine release from human and murine alveolar macrophages. Exp Lung Res 29:149–164
Mundandhara SD, Becker S, Madden MC (2006) Effects of diesel exhaust particles on human alveolar macrophage ability to secrete inflammatory mediators in response to lipopolysaccharide. Toxicol In Vitro 20:614–624
Eckhardt A, Harorli T, Limtanyakul J, Hiller KA, Bosl C, Bolay C, Reichl FX, Schmalz G, Schweikl H (2009) Inhibition of cytokine and surface antigen expression in LPS-stimulated murine macrophages by triethylene glycol dimethacrylate. Biomaterials 30:1665–1674
Krifka S, Hiller KA, Bolay C, Petzel C, Spagnuolo G, Reichl FX, Schmalz G, Schweikl H (2012) Function of MAPK and downstream transcription factors in monomer-induced apoptosis. Biomaterials 33:740–750
Zheng D, Wang N, Wang X, Tang Y, Zhu L, Huang Z, Tang H, Shi Y, Wu Y, Zhang M, Lu B (2012) Effects of the interaction of TiO2 nanoparticles with bisphenol A on their physicochemical properties and in vitro toxicity. J Hazard Mater 199–200:426–432
Altenburger R, Scholz S, Schmitt-Jansen M, Busch W, Escher BI (2012) Mixture toxicity revisited from a toxicogenomic perspective. Environ Sci Technol 46:2508–2522
Allouni ZE, Cimpan MR, Hol PJ, Skodvin T, Gjerdet NR (2009) Agglomeration and sedimentation of TiO2 nanoparticles in cell culture medium. Colloids Surf B: Biointerfaces 68:83–87
Kocbach A, Totlandsdal AI, Lag M, Refsnes M, Schwarze PE (2008) Differential binding of cytokines to environmentally relevant particles: a possible source for misinterpretation of in vitro results? Toxicol Lett 176:131–137
Laetz CA, Baldwin DH, Collier TK, Hebert V, Stark JD, Scholz NL (2009) The synergistic toxicity of pesticide mixtures: implications for risk assessment and the conservation of endangered Pacific salmon. Environ Health Perspect 117:348–353
Heil TL, Volkmann KR, Wataha JC, Lockwood PE (2002) Human peripheral blood monocytes versus THP-1 monocytes for in vitro biocompatibility testing of dental material components. J Oral Rehabil 29:401–407
Hornung V, Bauernfeind F, Halle A, Samstad EO, Kono H, Rock KL, Fitzgerald KA, Latz E (2008) Silica crystals and aluminum salts activate the NALP3 inflammasome through phagosomal destabilization. Nat Immunol 9:847–856
Becker S, Mundandhara S, Devlin RB, Madden M (2005) Regulation of cytokine production in human alveolar macrophages and airway epithelial cells in response to ambient air pollution particles: further mechanistic studies. Toxicol Appl Pharmacol 207:269–275
Guo B, Zebda R, Drake SJ, Sayes CM (2009) Synergistic effect of co-exposure to carbon black and Fe2O3 nanoparticles on oxidative stress in cultured lung epithelial cells. Part Fibre Toxicol 6:4 doi:10.1186/1743-8977-6-4
Berg JM, Ho S, Hwang W, Zebda R, Cummins K, Soriaga MP, Taylor R, Guo B, Sayes CM (2010) Internalization of carbon black and maghemite iron oxide nanoparticle mixtures leads to oxidant production. Chem Res Toxicol 23:1874–1882
Christen V, Crettaz P, Oberli-Schrammli A, Fent K (2012) Antiandrogenic activity of phthalate mixtures: validity of concentration addition. Toxicol Appl Pharmacol 259:169–176
Hehlgans T, Pfeffer K (2005) The intriguing biology of the tumour necrosis factor/tumour necrosis factor receptor superfamily: players, rules and the games. Immunology 115:1–20
Barksby HE, Nile CJ, Jaedicke KM, Taylor JJ, Preshaw PM (2009) Differential expression of immunoregulatory genes in monocytes in response to Porphyromonas gingivalis and Escherichia coli lipopolysaccharide. Clin Exp Immunol 156:479–487
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Mathisen, G.H., Ansteinsson, V., Samuelsen, J.T. et al. TEGDMA and filler particles from dental composites additively attenuate LPS-induced cytokine release from the macrophage cell line RAW 264.7. Clin Oral Invest 19, 61–69 (2015). https://doi.org/10.1007/s00784-014-1212-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-014-1212-7