Abstract
Background
The mechanisms underlying the interaction between the local mechanical environment and fracture healing are not known. We developed a mouse femoral fracture model with implants of different stiffness, and hypothesized that differential fracture healing would result.
Methods
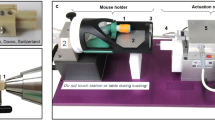
Femoral shaft fractures were created in 70 mice, and were treated with an intramedullary nail made of either tungsten (Young’s modulus = 410 GPa) or aluminium (Young’s modulus = 70 GPa). Mice were then sacrificed at 2 or 5 weeks. Fracture calluses were analyzed using standard microCT, histological, and biomechanical methods.
Results
At 2 weeks, callus volume was significantly greater in the aluminium group than in the tungsten group (61.2 vs. 40.5 mm3, p = 0.016), yet bone volume within the calluses was no different between the groups (13.2 vs. 12.3 mm3). Calluses from the tungsten group were stiffer on mechanical testing (18.7 vs. 9.7 N/mm, p = 0.01). The percent cartilage in the callus was 31.6% in the aluminium group and 22.9% in the tungsten group (p = 0.40). At 5 weeks, there were no differences between any of the healed femora.
Conclusions
In this study, fracture implants of different stiffness led to different fracture healing in this mouse fracture model. Fractures treated with a stiffer implant had more advanced healing at 2 weeks, but still healed by callus formation. Although this concept has been well documented previously, this particular model could be a valuable research tool to study the healing consequences of altered fixation stiffness, which may provide insight into the pathogenesis and ideal treatment of fractures and non-unions.



Similar content being viewed by others
References
Uhthoff HK, Finnegan MA. The role of rigidity in fracture fixation. An overview. Arch Orthop Trauma Surg. 1984;102:163–6.
Kenwright J, Gardner T. Mechanical influences on tibial fracture healing. Clin Orthop. 1998;355(Suppl):S179–90.
Epari DR, Kassi JP, Schell H, Duda GN. Timely fracture-healing requires optimization of axial fixation stability. J Bone Jt Surg Am. 2007;89:1575–85.
Claes L, Eckert-Hubner K, Augat P. The fracture gap size influences the local vascularization and tissue differentiation in callus healing. Langenbecks Arch Surg. 2003;388:316–22.
Augat P, Burger J, Schorlemmer S, Henke T, Peraus M, Claes L. Shear movement at the fracture site delays healing in a diaphyseal fracture model. J Orthop Res. 2003;21:1011–7.
Histing T, Holstein JH, Garcia P, Matthys R, Kristen A, Claes L, Menger MD, Pohlemann T. Ex vivo analysis of rotational stiffness of different osteosynthesis techniques in mouse femur fracture. J Orthop Res. 2009;27:1152–6.
Garcia P, Holstein JH, Histing T, Burkhardt M, Culemann U, Pizanis A, Wirbel RJ, Pohlemann T, Menger MD. A new technique for internal fixation of femoral fractures in mice: impact of stability on fracture healing. J Biomech. 2008;41:1689–96.
Holstein JH, Garcia P, Histing T, Kristen A, Scheuer C, Menger MD, Pohlemann T. Advances in the establishment of defined mouse models for the study of fracture healing and bone regeneration. J Orthop Trauma. 2009;23:S31–8.
Holstein JH, Menger MD, Culemann U, Meier C, Pohlemann T. Development of a locking femur nail for mice. J Biomech. 2007;40:215–9.
Bonnarens F, Einhorn TA. Production of a standard closed fracture in laboratory animal bone. J Orthop Res. 1984;2:97–101.
Manigrasso MB, O’Connor JP. Characterization of a closed femur fracture model in mice. J Orthop Trauma. 2004;18:687–95.
Goldberg VM, Powell A, Shaffer JW, Zika J, Bos GD, Heiple KG. Bone grafting: role of histocompatibility in transplantation. J Orthop Res. 1985;3:389–404.
Shen X, Wan C, Ramaswamy G, Mavalli M, Wang Y, Duvall CL, Deng LF, Guldberg RE, Eberhart A, Clemens TL, Gilbert SR. Prolyl hydroxylase inhibitors increase neoangiogenesis and callus formation following femur fracture in mice. J Orthop Res. 2009;27:1298–305.
Gardner MJ, van der Meulen MC, Carson J, Zelken J, Ricciardi BF, Wright TM, Lane JM, Bostrom MP. Role of parathyroid hormone in the mechanosensitivity of fracture healing. J Orthop Res. 2007;25:1474–80.
Ogasawara A, Nakajima A, Nakajima F, Goto K, Yamazaki M. Molecular basis for affected cartilage formation and bone union in fracture healing of the streptozotocin-induced diabetic rat. Bone. 2008;43:832–9.
Palomares KT, Gleason RE, Mason ZD, Cullinane DM, Einhorn TA, Gerstenfeld LC, Morgan EF. Mechanical stimulation alters tissue differentiation and molecular expression during bone healing. J Orthop Res. 2009;27:1123–32.
Shomento SH, Wan C, Cao X, Faugere MC, Bouxsein ML, Clemens TL, Riddle RC. Hypoxia-inducible factors 1alpha and 2alpha exert both distinct and overlapping functions in long bone development. J Cell Biochem. 2010;109:196–204.
Rundle CH, Wang X, Wergedal JE, Mohan S, Lau KH. Fracture healing in mice deficient in plasminogen activator inhibitor-1. Calcif Tissue Int. 2008;83:276–84.
Augat P, Simon U, Liedert A, Claes L. Mechanics and mechano-biology of fracture healing in normal and osteoporotic bone. Osteoporos Int. 2005;16(Suppl 2):S36–43.
Perren SM. Evolution of the internal fixation of long bone fractures. The scientific basis of biological internal fixation: choosing a new balance between stability and biology. J Bone Jt Surg Br. 2002;84:1093–110.
Lienau J, Schell H, Duda GN, Seebeck P, Muchow S, Bail HJ. Initial vascularization and tissue differentiation are influenced by fixation stability. J Orthop Res. 2005;23:639–45.
Glowacki J. Angiogenesis in fracture repair. Clin Orthop Relat Res. 1998; (355 Suppl):S82–9.
Brighton CT, Krebs AG. Oxygen tension of healing fractures in the rabbit. J Bone Jt Surg Am. 1972;54:323–32.
Gerstenfeld LC, Cullinane DM, Barnes GL, Graves DT, Einhorn TA. Fracture healing as a post-natal developmental process: molecular, spatial, and temporal aspects of its regulation. J Cell Biochem. 2003;88:873–84.
Allen FD, Hung CT, Pollack SR, Brighton CT. Serum modulates the intracellular calcium response of primary cultured bone cells to shear flow. J Biomech. 2000;33:1585–91.
Pavalko FM, Norvell SM, Burr DB, Turner CH, Duncan RL, Bidwell JP. A model for mechanotransduction in bone cells: the load-bearing mechanosomes. J Cell Biochem. 2003;88:104–12.
Acknowledgments
We thank Tarpit Patel, M.S., for assistance with microCT analysis and mechanical testing, which were supported in part by NIH/NIAMS grants P30AR057235 (Washington University Core Center for Musculoskeletal Biology and Medicine).
Conflict of interest
MJG is a consultant for Synthes, Amgen, and DGIMed. No outside funding was received in support of this work.
Author information
Authors and Affiliations
Corresponding author
About this article
Cite this article
Gardner, M.J., Putnam, S.M., Wong, A. et al. Differential fracture healing resulting from fixation stiffness variability: a mouse model. J Orthop Sci 16, 298–303 (2011). https://doi.org/10.1007/s00776-011-0051-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00776-011-0051-5