Abstract
Background
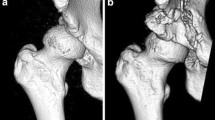
Satisfactory intermediate-term results after an eccentric rotational acetabular osteotomy (ERAO) for the treatment of early osteoarthritis secondary to developmental dysplasia of the hip (DDH) have been reported. The purpose of this study was to investigate whether a minimum joint space width (JSW) in patients with advanced osteoarthritis secondary to DDH influences intermediate-term clinical and radiographic outcomes after performing an ERAO.
Methods
A total of 113 patients (116 hips) with a JSW of ≤3 mm were consecutively treated by ERAO for advanced osteoarthritis of the hip and then were followed for more than 5 years. Based on the preoperative JSW, the patients were divided into three groups: minimum JSW of ≤1 mm (JS1 group); JSW >1 mm but ≤2 mm (JS2 group); JSW > 2 mm but ≤3 mm (JS3 group). The average ages of the JS1, JS2, and JS3 patients were 40, 44, and 43 years, respectively. The average follow-up period was 10.6 years.
Results
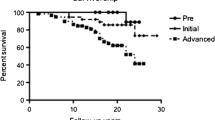
Overall conversion to total hip arthroplasty (THA) was performed in 14 joints. According to a Kaplan-Meier survivorship analysis at 15 years after the index operation, 96% of the patients with a JSW of >2 mm (JS3 group) did not require conversion to THA.
Conclusions
A JSW of >2 mm before surgery is considered essential to obtain an excellent intermediate-term result following performance of an ERAO.
Similar content being viewed by others
References
Cooperman DR, Wallensten R, Stulberg SD. Acetabular dysplasia in the adult. Clin Orthop 1983;175:79–85.
Hartofilakidis G, Karachalios T, Zacharakis N. Low friction arthroplasty in young patients with osteoarthritis: a 12- to 24-year clinical and radiographic follow-up study of 84 cases. Clin Orthop 1997;341:51–54.
Aldinger PR, Thomsen M, Mau H, Ewerbeck V, Breusch SJ. Cementless Spotorno tapered titanium stems: excellent 10–15-year survival in 141 young patients. Acta Orthop Scand 2003;74:253–258.
Kearns SR, Jamal B, Rorabeck CH, Bourne RB. Factors affecting survival of uncemented total hip arthroplasty inpatients 50 years or younger. Clin Orthop 2006;453:103–109.
Schramm M, Hohmann D, Radespiel-Troger M, Pitt RP. Treatment of the dysplastic acetabulum with Wagner spherical osteotomy. J Bone J Surg Am 2003;85:808–814.
Miller NH, Krisman SG, Kamaric E, Noble PC. Long-term results of the dial osteotomy in the treatment of high-grade acetabular dysplasia. Clin Orthop 2005;433:115–123.
Ninomiya S, Tagawa H. Rotational acetabular osteotomy for the dysplastic hip. J Bone Joint Surg Am 1986;66:430–436.
Nakamura S, Ninomiya S, Takatori Y, Morimoto S, Umeyama T. Long-term outcome of rotational acetabular osteotomy. 145 hips followed for 10–23 years. Acta Orthop Scand 1998;69:259–265.
Ganz R, Klaue K, Vinh TS, Mast JW. A new periacetabular osteotomy for the treatment of hip dysplasias. Clin Orthop 1988;232:26–36.
Trousdale RT, Ekkernkamp A, Ganz R, Wallrichs SL. Periacetabular and intertrochanteric osteotomy for the treatment of osteoarthrosis in dysplastic hips. J Bone Joint Surg Am 1995;77:73–85.
Hasegawa Y, Iwase T, Kitamura S, Yamauchi K, Sakano S, Iwata H. Eccentric rotational acetabular osteotomy for acetabular dysplasia: followup of 132 hips for 5 to 10 years. J Bone Joint Surg Am 2002;84:404–410.
Hasegawa Y, Masui T, Yamaguchi J, Suzuki S, Kawabe K. Osteoarthritis following eccentric rotational acetabular osteotomy. Clin Orthop 2007;459:207–215.
Kleuver M, Koojiman MAP, Pavlov PW, Veth RPH. Triple osteotomy of the pelvis for acetabular dysplasia: results at 8 to 15 years. J Bone Joint Surg Br 1997;79:225–229.
Migaud H, Chantelot C, Giraud F, Fontine C. Long-term survivorship of hip shelf arthroplasty and Chiari osteotomy in adults. Clin Orthop 2004;418:81–86.
Yasunaga Y, Takahashi K, Ochi M, Ikuta Y, Hisatome T, Nakashiro J, et al. Rotational acetabular osteotomy in patients forty-six years of age or older: comparison with younger patients. J Bone J Surg Am 2003;85:266–272.
Koga H, Matubara M, Suzuki K, Morita S, Muneta T. Factors which affect the progression of osteoarthritis after rotational acetabular osteotomy. J Bone Joint Surg Br 2003;85:963–968.
Nozawa M, Shitoto K, Matsuda K, Maezawa K, Kurosawa H. Rotational acetabular osteotomy for acetabular dysplasia: a follow-up more than ten years. J Bone Joint Surg Br 2002;84:59–65.
Wiberg G. Studies on dysplastic acetabular and congenital subluxation of the hip joint: with special reference to the complication of osteoarthritis. Acta Chir Scand 1939;58(suppl):5–135.
Heyman CH, Herndon CH. Legg-Perthes disease: a method for measurement of roentgenographic results. J Bone Joint Surg Am 1950;32:767–768.
Harris WH. Traumatic arthritis of the hip after dislocation and acetabular fracture: treatment by mold arthroplasty — an endresult study using a new method of new result evaluation. J Bone Joint Surg Am 1969;51:737–755.
Yasunaga Y, Ochi M, Terayama H, Tanaka R, Yamasaki T, Ishii Y. Rotational acetabular osteotomy for advanced osteoarthritis secondary to dysplasia of the hip. J Bone Joint Surg Am 2006;88:1915–1919.
Armand M, Lepisto J, Tallroth K, Elias J, Chao E. Outcome of periacetabular osteotomy: joint contact pressure calculation using standing AP radiographs, 12 patients followed for average 2 years. Acta Orthop Scand 2005;76:303–313.
Nakamura Y, Naito M, Akiyoshi Y, Shitama T. Acetabular cysts heal after successful periacetabular osteomy. Clin Orthop 2006; 454:120–126.
Author information
Authors and Affiliations
About this article
Cite this article
Hasegawa, Y., Kanoh, T., Seki, T. et al. Joint space wider than 2 mm is essential for an eccentric rotational acetabular osteotomy for adult hip dysplasia. J Orthop Sci 15, 620–625 (2010). https://doi.org/10.1007/s00776-010-1508-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00776-010-1508-7