Abstract
Background
Nonbacterial osteitis (NBO), a term referring to sterile bone lesions with nonspecific histopathological features of inflammation, may be either unifocal or multifocal, acute (≤6 months) or chronic, and recurrent. Only when the condition is chronic, recurrent, and multifocal is it appropriate to use the term chronic recurrent multifocal osteomyelitis (CRMO). We present our clinical experience as the largest reported series of children with NBO to date.
Methods
We report a retrospective clinical, histopathological, and radiological study of 41 children with nonbacterial osteitis.
Results
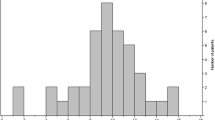
Of 41 children (2–16 years of age) diagnosed with NBO in our institution over the last 6 years, 21 (51%) had recurrent disease and 18 (44%) had multifocal disease. The most common bones affected were the clavicle, femur, and tibia (in order of decreasing prevalence) accounting for 44 (63%) of a total of 70 lesions. Only one individual had SAPHO syndrome (synovitis, acne, pustulosis, hyperostosis, osteitis) and no other patients had evidence of bowel or skin disease. In the absence of evidence for an infective etiology, we recommend nonsteroidal anti-inflammatory agents as the firstline therapy and bisphosphonates only in cases of resistant disease.
Conclusions
On the basis of our findings, we propose using a patient questionnaire and protocol for investigating and managing patients who present with NBO to orthopedic surgeons. We predict that this will benefit patients with this disorder by improving our knowledge of the presenting signs and symptoms and related disorders, rationalizing the therapeutic approach, and allowing us to learn about the natural history of the disease.
Similar content being viewed by others
References
El-Shanti HI, Ferguson PJ. Chronic recurrent multifocal osteomyelitis: a concise review and genetic update. Clin Orthop 2007;462:11–19.
Jansson A, Renner ED, Ramser J, Mayer A, Haban M, Meindl A, et al. Classification of nonbacterial osteitis: retrospective study of clinical, immunological and genetic aspects in 89 patients. Rheumatology (Oxf) 2007;46:154–160.
Hayem G, Bouchaud-Chabot A, Benali K, Roux S, Palazzo E, Silberman-Hoffman O, et al. SAPHO syndrome: a long term follow-up study of 120 cases. Semin Arthritis Rheum 1999;29:159–171.
Earwaker JW, Cotten A. SAPHO: syndrome or concept? Imaging findings. Skeletal Radiol 2003;32:311–327.
Girschick HJ, Huppertz HI, Harmsen D, Krauspe R, Müller-Hermelink HK, Papadopoulos T. Chronic recurrent multifocal osteomyelitis in children: diagnostic value of histopathology and microbial testing. Hum Pathol 1999;30:59–65.
Girschick HJ, Raab P, Surbaum S, Trusen A, Kirschner S, Schneider P et al. Chronic nonbacterial osteomyelitis in children. Ann Rheum Dis 2005;64:279–285.
Huber AM, Lam PY, Duffy CM, Yeung RS, Ditchfield M, Laxer D, et al. Chronic recurrent multifocal osteomyelitis: clinical outcomes after more than five years of follow-up. J Pediatr 2002;141:198–203.
Mollan RA, Craig BF, Biggart JD. Chronic sclerosing osteomyelitis: an unusual case. J Bone Joint Surg Br 1984;66:583–585.
Hummell DS, Anderson SJ, Wright PF, Cassell GH, Waites KB. Chronic recurrent multifocal osteomyelitis: are mycoplasmas involved? N Engl J Med 1987;317:510–511.
Waldvogel K, Regnery RL, Anderson BE, Caduff R, Caduff J, Nadal D. Disseminated cat-scratch disease: detection of Rochalimaea henselae in affected tissue. Eur J Paediatr 1994;153:23–27.
Poujol A, Toesca S, Di Marco JN, Rimet Y, Tissot Dupont H, Macé L, et al. Recurrent osteitis and Coxiella burnetii: the relation to chronic recurrent multifocal osteomyelitis. Arch Pediatr 1998;5:291–294.
Vittecoq O, Said LA, Michot C, Mejjad O, Thomine JM, Mitrofanoff P, et al. Evolution of chronic recurrent multifocal osteitis toward spondylarthropathy over the long term. Arthritis Rheum 2000;43:109–119.
Bousvaros A, Marcon M, Treem W, Waters P, Issenman R, Couper R, et al. Chronic recurrent multifocal osteomyelitis associated with chronic inflammatory bowel disease in children. Dig Dis Sci 1999;44:2500–2507.
Bazrafshan A, Zanjani KS. Chronic recurrent multifocal osteomyelitis associated with ulcerative colitis: a case report. J Pediatr Surg 2000;35:1520–1522.
Schilling F, Marker-Hermann E. Chronic recurrent multifocal osteomyelitis in association with chronic inflammatory bowel disease: enteropathic CRMO. Z Rheumatol 2003;62:527–538 (in German).
Bognar M, Blake W, Agudelo C. Chronic recurrent multifocal osteomyelitis associated with Crohn’s disease. Am J Med Sci 1998;315:133–135.
Ferguson PJ, Bing X, Vasef MA, Ochoa LA, Mahgoub A, Waldschmidt TJ, et al. A missense mutation in pstpip2 is associated with the murine autoinflammatory disorder chronic multifocal osteomyelitis. Bone 2006;38:41–47.
Golla A, Jansson A, Ramser J, Hellebrand H, Zahn R, Meitinger T, et al. Chronic recurrent multifocal osteomyelitis (CRMO): evidence for a susceptibility gene located on chromosome 18q21.3–18q22. Eur J Hum Genet 2002;10:217–221.
Ferguson PJ, Chen S, Tayeh MK, Ochoa L, Leal SM, Pelet A, et al. Homozygous mutations in LPIN2 are responsible for the syndrome of chronic recurrent multifocal osteomyelitis and congenital dyserythropoietic anaemia (Majeed syndrome). J Med Genet 2005;42:551–557.
Galeazzi M, Gasbarrini G, Ghirardello A, Grandemange S, Hoffman HM, Manna R, et al. Autoinflammatory syndromes. Clin Exp Rheumatol 2006;24(suppl 40):S79–85.
Ferguson PJ, El-Shanti HI. Autoinflammatory bone disorders. Curr Opin Rheumatol 2007;19:492–498.
Deutschmann A, Mache CJ, Bodo K, Zebedin D, Ring E. Successful treatment of chronic recurrent multifocal osteomyelitis with tumor necrosis factor-alpha blockage. Pediatrics 2005;116:1231–1233.
Carpenter E, Jackson MA, Friesen CA, Scarbrough M, Roberts CC. Crohn’s associated chronic recurrent multifocal osteomyelitis responsive to infliximab. J Pediatr 2004;144:541–544.
Author information
Authors and Affiliations
About this article
Cite this article
Gikas, P.D., Islam, L., Aston, W. et al. Nonbacterial osteitis: a clinical, histopathological, and imaging study with a proposal for protocol-based management of patients with this diagnosis. J Orthop Sci 14, 505–516 (2009). https://doi.org/10.1007/s00776-009-1381-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00776-009-1381-4