Abstract
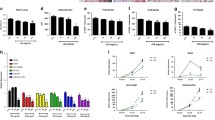
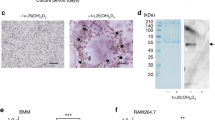
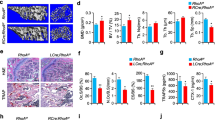
Bone is continuously remodeled by bone formation and resorption, and cooperative bone metabolism is precisely regulated to maintain homeostasis. Osteoclasts, which are responsible for bone resorption, are differentiated through multiple steps that include cell fusion at the last step of differentiation, yielding multinuclear cells. However, the factors involved in and the precise mechanism of cell fusion are still unknown. To determine the molecules involved in osteoclast fusion, we examined the effect of lysophosphatidic acid (LPA), which has been reported to participate in the progression of cancer bone metastasis. LPA had no effect on osteoclast formation and bone resorption under receptor activator of nuclear factor kappa B ligand (RANKL) conditions, whereas LPA stimulated osteoclast fusion, thereby causing increased osteoclast diameter and bone resorptive capacity under a RANKL-limited condition. This result encouraged us to assess what molecules are needed for LPA-stimulated osteoclast fusion. Interestingly, LPA stimulated osteoclast stimulatory transmembrane protein (OC-STAMP) and P2X7 receptor mRNA expression during osteoclast fusion under a RANKL limiting condition. siRNA-induced OC-STAMP or P2X7 receptor knockdown significantly suppressed the LPA-stimulated increase in osteoclast diameter and bone resorptive capacity in differentiating cultures. Using cyclosporin A as an inhibitor, we revealed that NF-ATc1 directly regulates OC-STAMP and P2X7 receptor expression during LPA-stimulated osteoclast fusion. These results suggest that LPA is a critical regulator of osteoclast fusion by inducing the OC-STAMP and P2X7 receptor. Therefore, LPA signaling might be useful to help understand their effects on osteoclast formation and as a therapeutic target for patients with pathologically increased osteoclast formation.




Similar content being viewed by others
References
Teitelbaum SL (2000) Bone resorption by osteoclasts. Science 289:1504–1508
Quinn JM, Gillespie MT (2005) Modulation of osteoclast formation. Biochem Biophys Res Commun 328:739–745
Suda T, Kobayashi K, Jimi E, Udagawa N, Takahashi N (2001) The molecular basis of osteoclast differentiation and activation. Novartis Found Symp 232:235–247
Kim MS, Day CJ, Morrison NA (2005) MCP-1 is induced by receptor activator of nuclear factor-{kappa}B ligand, promotes human osteoclast fusion, and rescues granulocyte macrophage colony-stimulating factor suppression of osteoclast formation. J Biol Chem 280:16163–16169
Helming L, Gordon S (2009) Molecular mediators of macrophage fusion. Trends Cell Biol 19:514–522
Yagi M, Miyamoto T, Sawatani Y, Iwamoto K, Hosogane N, Fujita N, Morita K, Ninomiya K, Suzuki T, Miyamoto K, Oike Y, Takeya M, Toyama Y, Suda T (2005) DC-STAMP is essential for cell–cell fusion in osteoclasts and foreign body giant cells. J Exp Med 202:345–351
MacLauchlan S, Skokos EA, Meznarich N, Zhu DH, Raoof S, Shipley JM, Senior RM, Bornstein P, Kyriakides TR (2009) Macrophage fusion, giant cell formation, and the foreign body response require matrix metalloproteinase 9. J Leukoc Biol 85:617–626
Kukita T, Wada N, Kukita A, Kakimoto T, Sandra F, Toh K, Nagata K, Iijima T, Horiuchi M, Matsusaki H, Hieshima K, Yoshie O, Nomiyama H (2004) RANKL-induced DC-STAMP is essential for osteoclastogenesis. J Exp Med 200:941–946
Yang M, Birnbaum MJ, MacKay CA, Mason-Savas A, Thompson B, Odgren PR (2008) Osteoclast stimulatory transmembrane protein (OC-STAMP), a novel protein induced by RANKL that promotes osteoclast differentiation. J Cell Physiol 215:497–505
Ke HZ, Qi H, Weidema AF, Zhang Q, Panupinthu N, Crawford DT, Grasser WA, Paralkar VM, Li M, Audoly LP, Gabel CA, Jee WS, Dixon SJ, Sims SM, Thompson DD (2003) Deletion of the P2X7 nucleotide receptor reveals its regulatory roles in bone formation and resorption. Mol Endocrinol 17:1356–1367
Falzoni S, Chiozzi P, Ferrari D, Buell G, Di Virgilio F (2000) P2X(7) receptor and polykarion formation. Mol Biol Cell 11:3169–3176
Lemaire I, Falzoni S, Leduc N, Zhang B, Pellegatti P, Adinolfi E, Chiozzi P, Di Virgilio F (2006) Involvement of the purinergic P2X7 receptor in the formation of multinucleated giant cells. J Immunol 177:7257–7265
Pellegatti P, Falzoni S, Donvito G, Lemaire I, Di Virgilio F (2011) P2X7 receptor drives osteoclast fusion by increasing the extracellular adenosine concentration. FASEB J 25:1264–1274
Grey A, Chen Q, Callon K, Xu X, Reid IR, Cornish J (2002) The phospholipids sphingosine-1-phosphate and lysophosphatidic acid prevent apoptosis in osteoblastic cells via a signaling pathway involving G(i) proteins and phosphatidylinositol-3 kinase. Endocrinology 143:4755–4763
Masiello LM, Fotos JS, Galileo DS, Karin NJ (2006) Lysophosphatidic acid induces chemotaxis in MC3T3-E1 osteoblastic cells. Bone (NY) 39:72–82
Panupinthu N, Rogers JT, Zhao L, Solano-Flores LP, Possmayer F, Sims SM, Dixon SJ (2008) P2X7 receptors on osteoblasts couple to production of lysophosphatidic acid: a signaling axis promoting osteogenesis. J Cell Biol 181:859–871
Karagiosis SA, Karin NJ (2007) Lysophosphatidic acid induces osteocyte dendrite outgrowth. Biochem Biophys Res Commun 357:194–199
Kim K, Lee SH, Ha Kim J, Choi Y, Kim N (2008) NFATc1 induces osteoclast fusion via up-regulation of Atp6v0d2 and the dendritic cell-specific transmembrane protein (DC-STAMP). Mol Endocrinol 22:176–185
Nair SP, Meghji S, Wilson M, Reddi K, White P, Henderson B (1996) Bacterially induced bone destruction: mechanisms and misconceptions. Infect Immun 64:2371–2380
Boyle WJ, Simonet WS, Lacey DL (2003) Osteoclast differentiation and activation. Nature (Lond) 423:337–342
Bar-Shavit Z (2007) The osteoclast: a multinucleated, hematopoietic-origin, bone-resorbing osteoimmune cell. J Cell Biochem 102:1130–1139
Mills GB, May C, McGill M, Roifman CM, Mellors A (1988) A putative new growth factor in ascitic fluid from ovarian cancer patients: identification, characterization, and mechanism of action. Cancer Res 48:1066–1071
Xu Y, Gaudette DC, Boynton JD, Frankel A, Fang XJ, Sharma A, Hurteau J, Casey G, Goodbody A, Mellors A, Holub BJ, Mills GB (1995) Characterization of an ovarian cancer activating factor in ascites from ovarian cancer patients. Clin Cancer Res 1:1223–1232
Xu Y, Shen Z, Wiper DW, Wu M, Morton RE, Elson P, Kennedy AW, Belinson J, Markman M, Casey G (1998) Lysophosphatidic acid as a potential biomarker for ovarian and other gynecologic cancers. JAMA 280:719–723
Moolenaar WH (2000) Development of our current understanding of bioactive lysophospholipids. Ann NY Acad Sci 905:1–10
Hurst-Kennedy J, Boyan BD, Schwartz Z (2009) Lysophosphatidic acid signaling promotes proliferation, differentiation, and cell survival in rat growth plate chondrocytes. Biochim Biophys Acta 1793:836–846
Boucharaba A, Serre CM, Grès S, Saulnier-Blache JS, Bordet JC, Guglielmi J, Clézardin P, Peyruchaud O (2004) Platelet-derived lysophosphatidic acid supports the progression of osteolytic bone metastases in breast cancer. J Clin Invest 114:1714–1725
Boucharaba A, Serre CM, Guglielmi J, Bordet JC, Clézardin P, Peyruchaud O (2006) The type 1 lysophosphatidic acid receptor is a target for therapy in bone metastases. Proc Natl Acad Sci USA 103:9643–9648
Lapierre DM, Tanabe N, Pereverzev A, Spencer M, Shugg RP, Dixon SJ, Sims SM (2010) Lysophosphatidic acid signals through multiple receptors in osteoclasts to elevate cytosolic calcium concentration, evoke retraction, and promote cell survival. J Biol Chem 285:25792–25801
McMichael BK, Meyer SM, Lee BS (2010) c-Src-mediated phosphorylation of thyroid hormone receptor-interacting protein 6 (TRIP6) promotes osteoclast sealing zone formation. J Biol Chem 285:26641–26651
David M, Wannecq E, Descotes F, Jansen S, Deux B, Ribeiro J, Serre CM, Grès S, Bendriss-Vermare N, Bollen M, Saez S, Aoki J, Saulnier-Blache JS, Clézardin P, Peyruchaud O (2010) Cancer cell expression of autotaxin controls bone metastasis formation in mouse through lysophosphatidic acid-dependent activation of osteoclasts. PLoS ONE 5:e9741
Adamopoulos IE, Chao CC, Geissler R, Laface D, Blumenschein W, Iwakura Y, McClanahan T, Bowman EP (2010) Interleukin-17A upregulates receptor activator of NF-kappaB on osteoclast precursors. Arthritis Res Ther 12:R29
Madyastha PR, Yang S, Ries WL, Key LL Jr (2000) IFN-gamma enhances osteoclast generation in cultures of peripheral blood from osteopetrotic patients and normalizes superoxide production. J Interferon Cytokine Res 20:645–652
Lam J, Takeshita S, Barker JE, Kanagawa O, Ross FP, Teitelbaum SL (2000) TNF-alpha induces osteoclastogenesis by direct stimulation of macrophages exposed to permissive levels of RANK ligand. J Clin Invest 106:1481–1488
Akatsu T, Takahashi N, Debari K, Morita I, Murota S, Nagata N, Takatani O, Suda T (1989) Prostaglandins promote osteoclast-like cell formation by a mechanism involving cyclic adenosine 3′,5′-monophosphate in mouse bone marrow cell cultures. J Bone Miner Res 4:29–35
Islam S, Hassan F, Tumurkhuu G, Dagvadorj J, Koide N, Naiki Y, Mori I, Yoshida T, Yokochi T (2007) Bacterial lipopolysaccharide induces osteoclast formation in RAW 264.7 macrophage cells. Biochem Biophys Res Commun 360:346–351
Hotokezaka H, Sakai E, Ohara N, Hotokezaka Y, Gonzales C, Matsuo K, Fujimura Y, Yoshida N, Nakayama K (2007) Molecular analysis of RANKL-independent cell fusion of osteoclast-like cells induced by TNF-alpha, lipopolysaccharide, or peptidoglycan. J Cell Biochem 101:122–1234
Kim MH, Park M, Baek SH, Kim HJ, Kim SH (2011) Molecules and signaling pathways involved in the expression of OC-STAMP during osteoclastogenesis. Amino Acids 40:1447–1459
Agrawal A, Buckley KA, Bowers K, Furber M, Gallagher JA, Gartland A (2010) The effects of P2X7 receptor antagonists on the formation and function of human osteoclasts in vitro. Purinergic Signal 6:307–315
Gartland A, Buckley KA, Bowler WB, Gallagher JA (2003) Blockade of the pore-forming P2X7 receptor inhibits formation of multinucleated human osteoclasts in vitro. Calcif Tissue Int 73:361–369
Takayanagi H, Kim S, Koga T, Nishina H, Isshiki M, Yoshida H, Saiura A, Isobe M, Yokochi T, Inoue J, Wagner EF, Mak TW, Kodama T, Taniguchi T (2002) Induction and activation of the transcription factor NFATc1 (NFAT2) integrate RANKL signaling in terminal differentiation of osteoclasts. Dev Cell 3:889–901
Hirotani H, Tuohy NA, Woo JT, Stern PH, Clipstone NA (2004) The calcineurin/nuclear factor of activated T cells signaling pathway regulates osteoclastogenesis in RAW264.7 cells. J Biol Chem 279:13984–13992
Crotti TN, Flannery M, Walsh NC, Fleming JD, Goldring SR, McHugh KP (2006) NFATc1 regulation of the human beta3 integrin promoter in osteoclast differentiation. Gene (Amst) 372:92–102
Ikeda F, Nishimura R, Matsubara T, Hata K, Reddy SV, Yoneda T (2006) Activation of NFAT signal in vivo leads to osteopenia associated with increased osteoclastogenesis and bone-resorbing activity. J Immunol 177:2384–2390
Sumoto M, Kogawa M, Wada S, Takayanagi H, Tsujimoto M, Katayama S, Hisatake K, Nogi Y (2004) Essential role of p38 mitogen-activated protein kinase in cathepsin K gene expression during osteoclastogenesis through association of NFATc1 and PU.1. J Biol Chem 279:45969–45979
Miyamoto H, Suzuki T, Miyauchi Y, Iwasaki R, Kobayashi T et al (2012) Osteoclast stimulatory transmembrane protein and dendrite cell-specific transmembrane protein cooperatively modulate cell–cell fusion to form osteoclasts and foreign body giant cells. J Bone Miner Res 27:1289–1297
Acknowledgments
This research was supported by Basic Science Research Program through the National Research Foundation of Korea (NRF) funded by the Ministry of Education, Science and Technology (2012R1A1A2040564).
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
About this article
Cite this article
Hwang, Y.S., Ma, GT., Park, KK. et al. Lysophosphatidic acid stimulates osteoclast fusion through OC-STAMP and P2X7 receptor signaling. J Bone Miner Metab 32, 110–122 (2014). https://doi.org/10.1007/s00774-013-0470-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00774-013-0470-9