Abstract
Purpose
The association between perimenopausal depression and many chronic conditions among women has been well-established. However, the role of depression during perimenopause in the progression of multiple chronic conditions (multimorbidity) remains poorly understood.
Material and methods
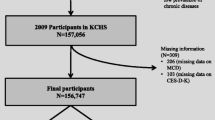
A total of 1,216 community-dwelling women in their perimenopause period between 2010 and 2016 were enrolled in our analysis, and followed up for the progression of multimorbidity. Depression, as well as its severity, was evaluated by the Center for Epidemiologic Studies Depression 10-item scale (CES-D-10). Progression of multimorbidity was defined as the first report of two or more chronic conditions for participants without multimorbidity or the new report of one or more conditions for those with multimorbidity. Univariable and multivariable Cox proportional hazards model and the restricted cubic spline regression model were performed to assess the prospective association between perimenopausal depression and the progression of multimorbidity.
Results
A total of 480 (39.5%) women reported depression during perimenopause, and 529 (43.5%) women progressed to multimorbidity. After adjusting for socio-demographic and lifestyle factors, perimenopausal depression was independently associated with the progression of multimorbidity (hazard ratio [HR]: 1.34; 95% confidence interval [CI]: 1.13 to 1.60). Moreover, the severity of depression was positively and linearly associated with the progression of multimorbidity (P < 0.05).
Conclusions
Our finding reveals a prospective association between perimenopausal depression and the progression of multimorbidity, indicating interventions targeting perimenopausal depression may reduce the burden of chronic diseases and multimorbidity in women’s post-menopausal life.



Similar content being viewed by others
Data Availability
All data used in this analysis are publicly available from the website of the China Health and Retirement Longitudinal Study (CHARLS): http://charls.pku.edu.cn/en/.
References
Auro K et al (2014) A metabolic view on menopause and ageing. Nat Commun 5:4708. https://doi.org/10.1038/ncomms5708
Auteri M, Zizzo MG, Serio R (2015) GABA and GABA receptors in the gastrointestinal tract: from motility to inflammation. Pharmacol Res 93:11–21. https://doi.org/10.1016/j.phrs.2014.12.001
Barnett K, Mercer SW, Norbury M, Watt G, Wyke S, Guthrie B (2012) Epidemiology of multimorbidity and implications for health care, research, and medical education: a cross-sectional study. The Lancet 380:37–43. https://doi.org/10.1016/S0140-6736(12)60240-2
Beaumont J-F, Charest A-S (2012) Bootstrap variance estimation with survey data when estimating model parameters. Comput Stat Data Anal 56:4450–4461. https://doi.org/10.1016/j.csda.2012.03.011
Boey KW (1999) Cross-validation of a short form of the CES-D in Chinese elderly. Int J Geriatr Psychiatry 14:608–617. https://doi.org/10.1002/(SICI)1099-1166(199908)14:8%3c608::AID-GPS991%3e3.0.CO;2-Z
Calderón-Larrañaga A et al (2018) Rapidly developing multimorbidity and disability in older adults: does social background matter? J Intern Med 283:489–499. https://doi.org/10.1111/joim.12739
Cheng HG, Chen S, McBride O, Phillips MR (2016) Prospective relationship of depressive symptoms, drinking, and tobacco smoking among middle-aged and elderly community-dwelling adults: Results from the China Health and Retirement Longitudinal Study (CHARLS). J Affect Disord 195:136–143. https://doi.org/10.1016/j.jad.2016.02.023
Cheng ST, Chan AC (2005) The Center for Epidemiologic Studies Depression Scale in older Chinese: thresholds for long and short forms. Int J Geriatr Psychiatry 20:465–470. https://doi.org/10.1002/gps.1314
Davern PJ, Chowdhury S, Jackson KL, Nguyen-Huu TP, Head GA (2014) GABAA receptor dysfunction contributes to high blood pressure and exaggerated response to stress in Schlager genetically hypertensive mice. J Hypertens 32:352–362. https://doi.org/10.1097/hjh.0000000000000015
de Kruif M, Spijker AT, Molendijk ML (2016) Depression during the perimenopause: A meta-analysis. J Affect Disord 206:174–180. https://doi.org/10.1016/j.jad.2016.07.040
De Leo V, Morgante G, Musacchio MC, Faldini E, Delia A, Petraglia F (2006) The safety of veralipride. Expert Opin Drug Saf 5:695–701. https://doi.org/10.1517/14740338.5.5.695
Ditmars HL, et al. (2021). Associations between depression and cardiometabolic health: A 27-year longitudinal study. Psychol Med, 1–11. https://doi.org/10.1017/s003329172000505x
Efron B, Tibshirani RJ (1993) An introduction to the Bootstrap. Chapman and Hall/CRC, vol 23. https://doi.org/10.1201/9780429246593
Eskola PJ et al (2015) Depression and Insulin Resistance: Additional Support for the Novel Heuristic Model in Perimenopausal Depression. Am J Psychiatry 172:796–797. https://doi.org/10.1176/appi.ajp.2015.15030377
Fortin M, Stewart M, Poitras ME, Almirall J, Maddocks H (2012) A systematic review of prevalence studies on multimorbidity: toward a more uniform methodology. Ann Fam Med 10:142–151. https://doi.org/10.1370/afm.1337
García-Montero, C et al (2022). The Problem of Malnutrition Associated with Major Depressive Disorder from a Sex-Gender Perspective. Nutrients, 14. https://doi.org/10.3390/nu14051107
Georgakis MK et al (2016) Association of Age at Menopause and Duration of Reproductive Period With Depression After Menopause: A Systematic Review and Meta-analysis. JAMA Psychiat 73:139–149. https://doi.org/10.1001/jamapsychiatry.2015.2653
Hughes MJ, McGettrick HM, Sapey E (2020). Shared mechanisms of multimorbidity in COPD, atherosclerosis and type-2 diabetes: the neutrophil as a potential inflammatory target. Eur Respir Rev, 29. https://doi.org/10.1183/16000617.0102-2019.
Jagtap BL, Prasad BS, Chaudhury S (2016) Psychiatric morbidity in perimenopausal women. Ind Psychiatry J 25:86–92. https://doi.org/10.4103/0972-6748.196056
Jiang CH, Zhu F, Qin TT (2020) Relationships between Chronic Diseases and Depression among Middle-aged and Elderly People in China: A Prospective Study from CHARLS. Curr Med Sci 40:858–870. https://doi.org/10.1007/s11596-020-2270-5
Kochar B et al (2018) Depression Is Associated With More Aggressive Inflammatory Bowel Disease. Am J Gastroenterol 113:80–85. https://doi.org/10.1038/ajg.2017.423
Lee SP, Sung I-K, Kim JH, Lee S-Y, Park HS, Shim CS (2015) The effect of emotional stress and depression on the prevalence of digestive diseases. Journal of Neurogastroenterology and Motility 21:273–282. https://doi.org/10.5056/jnm14116
Li H et al (2019) Association of Depressive Symptoms With Incident Cardiovascular Diseases in Middle-Aged and Older Chinese Adults. JAMA Netw Open 2:e1916591. https://doi.org/10.1001/jamanetworkopen.2019.16591
Liu Y et al (2020) Gut Microbiome Fermentation Determines the Efficacy of Exercise for Diabetes Prevention. Cell Metab 31:77-91.e75. https://doi.org/10.1016/j.cmet.2019.11.001
Lu MC, Guo HR, Lin MC, Livneh H, Lai NS, Tsai TY (2016) Bidirectional associations between rheumatoid arthritis and depression: a nationwide longitudinal study. Sci Rep 6:20647. https://doi.org/10.1038/srep20647
Lui Filho JF, Baccaro LF, Fernandes T, Conde DM, Costa-Paiva L, Pinto Neto AM (2015) Factors associated with menopausal symptoms in women from a metropolitan region in Southeastern Brazil: a population-based household survey. Rev Bras Ginecol Obstet 37:152–158. https://doi.org/10.1590/so100-720320150005282
Luo H et al (2018) Obesity and the onset of depressive symptoms among middle-aged and older adults in China: evidence from the CHARLS. BMC Public Health 18:909–909. https://doi.org/10.1186/s12889-018-5834-6
Muka T, Oliver-Williams C, Colpani V, Kunutsor S, Chowdhury S, Chowdhury R, Kavousi M, Franco OH (2016) Association of Vasomotor and other menopausal symptoms with risk of cardiovascular disease: a systematic review and meta-analysis. PLoS One 11(6):e0157417. https://doi.org/10.1371/journal.pone.0157417
Ouyang P, Sun W (2019) Depression and sleep duration: findings from middle-aged and elderly people in China. Public Health 166:148–154. https://doi.org/10.1016/j.puhe.2018.10.007
Parry BL (2010) Optimal management of perimenopausal depression. Int J Womens Health 2:143–151. https://doi.org/10.2147/ijwh.s7155
Reiche EMV, Nunes SOV, Morimoto HK (2004) Stress, depression, the immune system, and cancer. Lancet Oncol 5:617–625
Rocca WA et al (2016) Accelerated Accumulation of Multimorbidity After Bilateral Oophorectomy: A Population-Based Cohort Study. Mayo Clin Proc 91:1577–1589. https://doi.org/10.1016/j.mayocp.2016.08.002
Rocca WA et al (2018) Loss of Ovarian Hormones and Accelerated Somatic and Mental Aging. Physiology (bethesda) 33:374–383. https://doi.org/10.1152/physiol.00024.2018
Rubinow DR, Girdler SS (2011) Hormones, heart disease, and health: individualized medicine versus throwing the baby out with the bathwater. Depress Anxiety 28:E1-e15. https://doi.org/10.1002/da.20833
Rudzinskas S, Hoffman JF, Martinez P, Rubinow DR, Schmidt PJ, Goldman D (2021) In vitro model of perimenopausal depression implicates steroid metabolic and proinflammatory genes. Mol Psychiatry 26:3266–3276. https://doi.org/10.1038/s41380-020-00860-x
Rymer J, Morris EP (2000) "Extracts from “Clinical evidence”: Menopausal symptoms. BMJ 321:1516–1519. https://doi.org/10.1136/bmj.321.7275.1516
Santoro N (2016) Perimenopause: From Research to Practice. J Womens Health (larchmt) 25:332–339. https://doi.org/10.1089/jwh.2015.5556
Shang X, Peng W, Hill E, Szoeke C, He M, Zhang L (2020) Incidence, Progression, and Patterns of Multimorbidity in Community-Dwelling Middle-Aged Men and Women. Front Public Health 8:404. https://doi.org/10.3389/fpubh.2020.00404
Shieh A et al (2022) Associations of Age at Menopause With Postmenopausal Bone Mineral Density and Fracture Risk in Women. J Clin Endocrinol Metab 107:e561–e569. https://doi.org/10.1210/clinem/dgab690
Smarr KL, Keefer AL (2011) Measures of depression and depressive symptoms: Beck Depression Inventory-II (BDI-II), Center for Epidemiologic Studies Depression Scale (CES-D), Geriatric Depression Scale (GDS), Hospital Anxiety and Depression Scale (HADS), and Patient Health Questionnaire-9 (PHQ-9). Arthritis Care Res 63:S454–S466. https://doi.org/10.1002/acr.20556
Soares CN (2013) Depression in Peri- and Postmenopausal Women: Prevalence, Pathophysiology and Pharmacological Management. Drugs Aging 30:677–685. https://doi.org/10.1007/s40266-013-0100-1
Stekhoven DJ, Bühlmann P (2012) MissForest–non-parametric missing value imputation for mixed-type data. Bioinformatics 28:112–118. https://doi.org/10.1093/bioinformatics/btr597
Tang R et al (2020) Relationships Between Vasomotor Symptoms and Mood in Midlife Urban Chinese Women: Observations in a Prospective Study. J Clin Endocrinol Metab 105. https://doi.org/10.1210/clinem/dgaa554.
Timur S, Sahin NH (2010) The prevalence of depression symptoms and influencing factors among perimenopausal and postmenopausal women. Menopause 17:545–551. https://doi.org/10.1097/gme.0b013e3181cf8997
Vivian-Taylor J, Hickey M (2014) Menopause and depression: is there a link? Maturitas 79:142–146. https://doi.org/10.1016/j.maturitas.2014.05.014
Wang J, Wu X, Lai W, Long E, Zhang X, Li W, Zhu Y, Chen C, Zhong X, Liu Z, Wang D, Lin H (2017) Prevalence of depression and depressive symptoms among outpatients: a systematic review and meta-analysis. BMJ open 7(8):e017173. https://doi.org/10.1136/bmjopen-2017-017173
Xu X, Jones M, Mishra GD (2020) Age at natural menopause and development of chronic conditions and multimorbidity: results from an Australian prospective cohort. Hum Reprod 35:203–211. https://doi.org/10.1093/humrep/dez259
Xu X, Mishra GD, Jones M (2017) Evidence on multimorbidity from definition to intervention: An overview of systematic reviews. Ageing Res Rev 37:53–68. https://doi.org/10.1016/j.arr.2017.05.003
Yuan X, Liu T, Wu L, Zou Z-Y, Li C (2015) Validity of self-reported diabetes among middle-aged and older Chinese adults: the China Health and Retirement Longitudinal Study. BMJ Open 5:e006633–e006633. https://doi.org/10.1136/bmjopen-2014-006633
Zhao Y, Hu Y, Smith JP, Strauss J, Yang G (2014) Cohort profile: the China Health and Retirement Longitudinal Study (CHARLS). Int J Epidemiol 43:61–68. https://doi.org/10.1093/ije/dys203
Zhou L, Ma X, Wang W (2021) Relationship between Cognitive Performance and Depressive Symptoms in Chinese Older Adults: The China Health and Retirement Longitudinal Study (CHARLS). J Affect Disord 281:454–458. https://doi.org/10.1016/j.jad.2020.12.059
Acknowledgements
The authors thank the participants and staff of the China Health and Retirement Longitudinal Study (CHARLS) team for their valuable contributions.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
XX contributed the study conceptualization and supervised the project. BY and MC carried out the data analyses. BY wrote the initial draft of the manuscript, YZ, JT and CC revised the manuscript critically. All authors contributed to and have approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
All other authors declare that they have no conflicts of interest.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Bingqi Ye and Yaguan Zhou contributed equally as co-first authors.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Ye, B., Zhou, Y., Chen, M. et al. The association between depression during perimenopause and progression of chronic conditions and multimorbidity: results from a Chinese prospective cohort. Arch Womens Ment Health 26, 697–705 (2023). https://doi.org/10.1007/s00737-023-01354-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00737-023-01354-9