Summary
Background
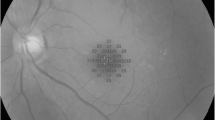
Part of multimodal imaging in patients with macular hole and epiretinal membrane is often microperimetry, a method to measure the central sensitivity of the retina. A study by Richter-Mueksch et al. with the microperimeter MP‑1 (Nidek Technologies Srl, Vigonza, Italy) reported that visual acuity alone underestimates the benefit of surgery and that more patients show improvement in microperimetry postoperatively. The aim of this study was to confirm these results with the microperimeter MP‑3 (Nidek Co., LTD., Aichi, Japan) currently in use at our institution.
Methods
A retrospective data analysis was performed of patients who underwent surgery for epiretinal membrane or macular hole from January 2020 to December 2022 and who underwent pre- and postoperative microperimetry.
Results
Overall, 18 patients who underwent microperimetry pre- and postoperatively were included in this analysis. The mean age was 71 years and 67% of the patients were female. Five patients had surgery due to macular hole and 13 patients due to epiretinal membrane. There was a significant increase in visual acuity postoperatively (p = 0.01, z = −2.57, r = −0.61). The median visual acuity was 0.4 logMAR preoperatively and 0.2 logMAR postoperatively. Total mean retinal sensitivity showed no statistically significant change; however, the central mean retinal sensitivity within a 4° fixation point circle showed significant improvement postoperatively (p = 0.04, z = 2.84, r = 0.67).
Conclusion
In summary, there was a significant improvement in visual acuity postoperatively, but only a significant increase in retinal sensitivity centrally, whereas overall retinal sensitivity did not show a statistically significant increase.
Zusammenfassung
Hintergrund
Teil der multimodalen Bildgebung bei Patient*innen mit Makulaforamen und epiretinaler Membran (ERM) ist oft die Mikroperimetrie, eine Methode, um die zentrale Sensitivität der Retina zu messen. Richter-Mueksch et al. zeigten in einer Studie mit dem Mikroperimeter MP‑1 (Nidek Technologies Srl, Vigonza, Italien), dass mit der alleinigen Visusbestimmung der Nutzen einer Operation unterschätzt wird und mehr Patient*innen postoperativ eine Verbesserung in der Mikroperimetrie aufweisen. Ziel der Studie war es, diese Ergebnisse mit dem aktuell an der Abteilung der Autoren in Verwendung befindlichen Mikroperimeter MP‑3 (Nidek Co., LTD., Aichi, Japan) zu bestätigen.
Methoden
Eine retrospektive Datenanalyse erfolgte an Patient*innen, die von Januar 2020 bis Dezember 2022 aufgrund einer epiretinalen Membran bzw. eines Makulaforamens operiert worden sind und bei denen eine prä- und postoperative Mikroperimetrie durchgeführt wurde.
Ergebnisse
In die Studie wurden 18 Patient*innen, bei denen prä- und postoperativ eine Mikroperimetrie erfolgte, eingeschlossen. Das mittlere Alter betrug 71 Jahre, 67 % der Patient*innen waren weiblich. Aufgrund eines Makulaforamens wurden 5, aufgrund einer ERM 13 Patient*innen operiert. Es zeigte sich postoperativ ein signifikanter Anstieg des Visus (p = 0,01; z = −2,57; r = −0,61). Der mediane Visus betrug präoperativ 0,4 logMAR und postoperativ 0,2 logMAR. Die gesamte mittlere retinale Sensitivität zeigte keine statistisch signifikante Veränderung, während die zentrale mittlere retinale Sensitivität in einem 4°-Fixationsradius postoperativ eine signifikante Verbesserung aufwies (p = 0,04; z = 2,84; r = 0,67).
Schlussfolgerung
Zusammenfassend zeigte sich postoperativ eine signifikante Visusverbesserung, ein signifikanter Anstieg der retinalen Sensitivität fand sich jedoch nur zentral, während die retinale Sensitivität insgesamt keinen statistisch signifikanten Anstieg aufwies.





Similar content being viewed by others
References
Duker JS, Kaiser PK, Binder S, De Smet MD, Gaudric A, Reichel E, et al. The international vitreomacular traction study group classification of vitreomacular adhesion, traction, and macular hole. Ophthalmology. 2013;120(12):2611–9.
Meuer SM, Myers CE, Klein BEK, Swift MK, Huang Y, Gangaputra S, et al. The epidemiology of vitreoretinal interface abnormalities as detected by SD-OCT: the beaver dam eye study. Ophthalmology. 2015;122(4):787.
McKibbin M, Farragher TM, Shickle D. Monocular and binocular visual impairment in the UK Biobank study: prevalence, associations and diagnoses. BMJ Open Ophthalmol. 2018;3(1):76.
Benson WE, Cruickshanks KC, Fong DS, Williams GA, Bloome MA, Frambach DA, et al. Surgical management of macular holes: a report by the American Academy of Ophthalmology. Ophthalmology. 2001;108(7):1328–35.
Matoba R, Morizane Y. Surgical treatment of epiretinal membrane. Acta Med Okayama. 2021;75(4):403–13.
Oh H. Idiopathic macular hole. Dev Ophthalmol. 2014;54:150–8.
Huang Q, Li J. With or without internal limiting membrane peeling during idiopathic epiretinal membrane surgery: a meta-analysis. PLoS One. 2021. https://pubmed.ncbi.nlm.nih.gov/33465119/. Accessed 11 Jan 2023.
Ducloyer JB, Ivan J, Poinas A, Lebreton O, Bonissent A, Fossum P, et al. Does internal limiting membrane peeling during epiretinal membrane surgery induce microscotomas on microperimetry? Study protocol for PEELING, a randomized controlled clinical trial. Trials. 2020. https://pubmed.ncbi.nlm.nih.gov/32513229/. Accessed 11 Jan 2023.
Yu JG, Wang J, Xiang Y. Inverted internal limiting membrane flap technique versus internal limiting membrane peeling for large macular holes: a meta-analysis of randomized controlled trials. Ophthalmic Res. 2021;64(5):713–22.
Blautain B, Glacet-Bernard A, Blanco-Garavito R, Toutée A, Jung C, Ortoli M, et al. Long-term follow-up of retinal sensitivity assessed by microperimetry in patients with internal limiting membrane peeling. Eur J Ophthalmol. 2022;32(1):539–45.
Leisser C, Palkovits S, Hienert J, Ullrich M, Zwickl H, Georgiev S, et al. Effect of iatrogenic traction during macular peeling surgery on postoperative microperimetry. Ophthalmic Res. 2021;64(2):273–9.
Pradhan D, Agarwal L, Joshi I, Kushwaha A, Aditya K, Kumari A. Internal limiting membrane peeling in macular hole surgery. Ger Med Sci. 2022. https://pubmed.ncbi.nlm.nih.gov/35813123/. Accessed 11 Jan 2023.
Wons J, Pfister IB, Anastasi S, Steinhauer S, Niderprim SA, Garweg JG. Functional outcome after macular hole surgery: comparison of standard perimetry with microperimetry. Clin Ophthalmol. 2022;16:2235–43.
Richter-Mueksch S, Vécsei-Marlovits PV, Sacu SG, Kiss CG, Weingessel B, Schmidt-Erfurth U. Functional macular mapping in patients with vitreomacular pathologic features before and after surgery. Am J Ophthalmol. 2007. https://pubmed.ncbi.nlm.nih.gov/17509512/. Accessed 11 Jan 2023.
Dal Vecchio M, Lavia C, Nassisi M, Grignolo FM, Fea AM. Microperimetric assessment after epiretinal membrane surgery: 4‑year follow-up. J Ophthalmol. 2016. https://pubmed.ncbi.nlm.nih.gov/27088008/. Accessed 11 Jan 2023.
Xu Z, Mao J, Lao J, Deng X, Liu C, Xu J, et al. Macular retinal sensitivity and microvasculature changes before and after vitrectomy in idiopathic macular epiretinal membrane with classification. Ophthalmologica. 2021;244(6):569–80.
Feng J, Yang X, Xu M, Wang Y, Shi X, Zhang Y, et al. Association of microvasculature and macular sensitivity in idiopathic macular epiretinal membrane: using OCT angiography and microperimetry. Front Med (Lausanne). 2021. https://pubmed.ncbi.nlm.nih.gov/34869402/. Accessed 11 Jan 2023.
Springer C, Bültmann S, Völcker HE, Rohrschneider K. Fundus perimetry with the micro perimeter 1 in normal individuals: comparison with conventional threshold perimetry. Ophthalmology. 2005;112(5):848–54.
Yang Y, Dunbar H. Clinical perspectives and trends: microperimetry as a trial endpoint in retinal disease. Ophthalmologica. 2021;244(5):418.
Qi Y, Wang Z, Li SM, You Q, Liang X, Yu Y, et al. Effect of internal limiting membrane peeling on normal retinal function evaluated by microperimetry‑3. BMC Ophthalmol. 2020;20(1).
Liu L, Wang Z, Yu Y, Yang X, Qi B, Zhang K, et al. Microstructural and microperimetric comparison of internal limiting membrane peeling and insertion in large idiopathic macular hole. BMC Ophthalmol. 2023;23(1).
Wrzesinska D, Nowomiejska K, Nowakowska D, Brzozowska A, Avitabile T, Reibaldi M, et al. Vertical and horizontal M‑charts and microperimetry for assessment of the visual function in patients after vitrectomy with ILM peeling due to stage 4 macular hole. J Ophthalmol. 2019;2019.
Sborgia G, Niro A, Sborgia A, Albano V, Tritto T, Sborgia L, et al. Inverted internal limiting membrane-flap technique for large macular hole: a microperimetric study. Int J Retina Vitreous. 2019. https://pubmed.ncbi.nlm.nih.gov/31641530/. Accessed 2 Aug 2023.
Dalan D, Jaishankar D, Madhu A, Mani K, Ratra D. Macular function assessment by multifocal electroretinogram and microperimetry in macular hole and correlation with visual acuity. Nepal J Ophthalmol. 2020;12(23):7–16.
Nam SW, Byun Z, Ham DI, Kong M. Microperimetric evaluation for different methods of epiretinal membrane surgery. BMC Ophthalmol. 2023. https://pubmed.ncbi.nlm.nih.gov/37386389/. Accessed 2 Aug 2023.
Osada U, Kunikata H, Yasuda M, Hashimoto K, Nishiguchi KM, Nakazawa T. Association of retinal vessel density with retinal sensitivity in surgery for idiopathic epiretinal membrane. Graefes Arch Clin Exp Ophthalmol. 2020;258(9):1911–20.
Sato T, Yamauchi-Mori R, Yamamoto J, Hayashi K. Longitudinal change in retinal nerve fiber layer thickness and its association with central retinal sensitivity after epiretinal membrane surgery. Asia Pac J Ophthalmol. 2022;11(3):279–86.
Wu Y, Chen Y, Mao J, Ye X, Chen H, Xu Z, et al. Long-term quantitative analysis of inner retinal dimples and visual function post internal limiting membrane peeling in macular diseases. Ophthalmol Ther. 2023. https://pubmed.ncbi.nlm.nih.gov/37943480/. Accessed 23 Nov 2023.
Russo A, Morescalchi F, Gambicorti E, Cancarini A, Costagliola C, Semeraro F. Epiretinal membrane removal with foveal-sparing internal limiting membrane peeling: a pilot study. Retina. 2019;39(11):2116–24.
Ripandelli G, Scarinci F, Piaggi P, Guidi G, Pileri M, Cupo G, et al. Macular pucker: to peel or not to peel the internal limiting membrane? A microperimetric response. Retina. 2015;35(3):498–507.
Díaz-Valverde A, Wu L. To peel or not to peel the internal limiting membrane in idiopathic epiretinal membranes. Retina. 2018;38(Suppl 1):S5–S11.
Chatziralli IP, Theodossiadis PG, Steel DHW. Internal limiting membrane peeling in macular hole surgery; why, when, and how? Retina. 2018;38(5):870–82.
Khodabande A, Mahmoudi A, Faghihi H, Bazvand F, Ebrahimi E, Riazi-Esfahani H, et al. Outcomes of idiopathic full-thickness macular hole surgery: comparing two different ILM peeling sizes. J Ophthalmol. 2020. https://pubmed.ncbi.nlm.nih.gov/32908679/. Accessed 28 Nov 2023.
Aydin A, Kocak I, Aykan U, Can G, Sabahyildizi M, Ersanli D. The influence of the learning effect on automated perimetry in a Turkish population. J Fr Ophtalmol. 2015;38(7):628–32.
Wong EN, De Soyza JDA, Mackey DA, Constable IJ, Chen FK. Intersession test-retest variability of microperimetry in type 2 macular telangiectasia. Transl Vis Sci Technol. 2017. https://pubmed.ncbi.nlm.nih.gov/29242756/. Accessed 23 Nov 2023.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
S.N. Mehany, B. Weingessel and V. Vécsei-Marlovits declare that they have no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Mehany, S.N., Weingessel, B. & Vécsei-Marlovits, V. Pre- and postoperative microperimetry in patients with epiretinal membrane and macular hole. Spektrum Augenheilkd. (2024). https://doi.org/10.1007/s00717-024-00568-1
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00717-024-00568-1