Abstract
Background
A cornerstone of surgical residency training is an educational program that produces highly skilled and effective surgeons. Training structures are constantly being revised due to evolving program structures, shifting workforces, and variability in the clinical environment. This has resulted in significant heterogeneity in all surgical resident education, training tools utilized, and measures of training efficacy.
Methods
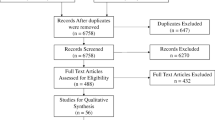
We systematically reviewed educational interventions for technical skills in neurosurgery published across PubMed, Embase, and Web of Science over four decades. We extracted general characteristics of each surgical training tool while categorizing educational interventions by modality and neurosurgical application.
Results
We identified 626 studies which developed surgical training tools across eight different training modalities: textbooks and literature (11), online resources (53), didactic teaching and one-on-one instruction (7), laboratory courses (50), cadaveric models (63), animal models (47), mixed reality (166), and physical models (229). While publication volume has grown exponentially, a majority of studies were cited with relatively low frequency. Most training programs were published in the development and validation phase with only 2.1% of tools implemented long-term. Each training modality expressed unique strengths and limitations, with limited data reported on the educational impact connected to each training tool.
Conclusions
Numerous surgical training tools have been developed and implemented across residency training programs. Though many creative and cutting-edge tools have been devised, evidence supporting educational efficacy and long-term application is lacking. Increased utilization of novel surgical training tools will require validation of metrics used to assess the training outcomes and optimized integration with clinical practice.



Similar content being viewed by others
Data Availability
In cases where specific datasets or materials are referenced in this paper, we have provided appropriate citations and references to the original sources and included papers.
References
Aboud E, Aboud G, Al-Mefty O et al (2015) New laboratory model for neurosurgical training that simulates live surgery. J Neurosurg 123(5):1339–1346. https://doi.org/10.3171/2014.12.JNS141551
Alotaibi FE, AlZhrani GA, Mullah MAS et al (2015) Assessing Bimanual Performance in Brain Tumor Resection With NeuroTouch, a Virtual Reality Simulator. Operative Neurosurg 11(1):89–98. https://doi.org/10.1227/NEU.0000000000000631
Ament JD, Kim T, Gold-Markel J et al (2017) Planning and Executing the Neurosurgery Boot Camp: The Bolivia Experience. World Neurosurg 104:407–410. https://doi.org/10.1016/j.wneu.2017.05.046
Breese R, Piazza M, Quinsey C, Blatt J (2020) Tactile Skill-Based Neurosurgical Simulators Are Effective and Inexpensive. World Neurosurg 137:319–326. https://doi.org/10.1016/j.wneu.2020.02.017
Clark AD, Guilfoyle MR, Candy NG et al (2017) Stereoscopic Three-Dimensional Neuroanatomy Lectures Enhance Neurosurgical Training: Prospective Comparison with Traditional Teaching. World Neurosurg 108:917–923. https://doi.org/10.1016/j.wneu.2017.09.019
Clifton W, Nottmeier E, Edwards S et al (2019) Development of a Novel 3D Printed Phantom for Teaching Neurosurgical Trainees the Freehand Technique of C2 Laminar Screw Placement. World Neurosurg 129:e812–e820. https://doi.org/10.1016/j.wneu.2019.06.038
Derossis AM, Bothwell J, Signman HH et al (1998) Th effect of practice on performance in a laparoscopic simulator. Surg Endosc 12(9):1117–1120. https://doi.org/10.1007/s004649900796
Fernandez G, Page DW, Coe NP et al (2012) Boot cAMP: educational outcomes after 4 successive years of preparatory simulation-based training at onset of internship. J Surg Educ 69(2):242–248. https://doi.org/10.1016/j.jsurg.2011.08.007
Franasiak JM, Craven R, Gehrig PA (2013) Feasibility and effectiveness of an ergonomics training program to address high rates of strain among robotic surgeons. J Minim Invasive Gynecol 20(6):S80. https://doi.org/10.1016/j.jmig.2013.08.260
Grantcharov TP (2008) Is virtual reality simulation an effective training method in surgery? Nat Clin Pract Gastroenterol Hepatol 5(5):232–233. https://doi.org/10.1038/ncpgasthep1101
Gurusamy Aggarwal R, Palanivelu L et al (2008) Systematic review of randomized controlled trials on the effectiveness of virtual reality training for laparoscopic surgery. Br J Surg 95(9):1088–1097. https://doi.org/10.1002/bjs.6344
Han E, Yeo S, Kim M et al (2019) Medical education trends for future physicians in the era of advanced technology and artificial intelligence: an integrative review. BMC Med Educ 19(1):460. https://doi.org/10.1186/s12909-019-1891-5
Indo M, Tsutsumi K, Shin M (2011) The practice of knots untying technique using a 10-0 nylon suture and gauze to cope with technical difficulties of microvascular anastomosis. World Neurosurg 75(1):87–89. https://doi.org/10.1016/j.wneu.2010.07.030
Koivula A, Räsänen P, Sarpila O (2019) Examining Social Desirability Bias in Online and Offline Surveys. Int Conf Human-Computer Inter 11566. https://doi.org/10.1007/978-3-030-22646-6_11
Moiraghi A, Perin A, Sicky N et al (2020) EANS Basic Brain Course (ABC): combining simulation to cadaver lab for a new concept of neurosurgical training. Acta Neurochir 162(3):453–460. https://doi.org/10.1007/s00701-020-04216-w
Olabe J, Olabe J, Sancho V (2009) Human cadaver brain infusion model for neurosurgical training. Surg Neurol 72(6):700–702. https://doi.org/10.1016/j.surneu.2009.02.028
Ortiz-Garcia J, Doerrler M, Douglas P et al (2016) Simulation-based training in brain death determination incorporating family discussion: A pilot project. Neurology 86(16). https://doi.org/10.4300/JGME-D-18-00185.1
Page MJ, McKenzie JE, Bossuyt PM et al (2021) The PRISMA 2020 statement: An updated guideline for reporting systematic reviews. PLoS Med 18(3):e1003583. https://doi.org/10.1371/journal.pmed.1003583
Park JJ, Tiefenbach J, Demetriades AK (2022) The role of artificial intelligence in surgical simulation. Front Med Technol 4:1076755. https://doi.org/10.3389/fmedt.2022.1076755
Reddy PP, Reddy TP, Jennifer RF et al (2011) The impact of the alexander technique on improving posture and surgical ergonomics during minimally invasive surgery: pilot study. J Urol 186(4S):1658–1662. https://doi.org/10.1016/j.juro.2011.04.013
Saltarelli AJ, Roseth CJ, Saltarelli W (2014) Human cadavers Vs. multimedia simulation: A study of student learning in anatomy. Anat Sci Educ 7(5). https://doi.org/10.1002/ase.1429
Samuel N, Alotaibi NM, Lozano AM (2017) YouTube as a Source of Information on Neurosurgery. World Neurosurg 105:394–398. https://doi.org/10.1016/j.wneu.2017.05.111
Selden NR, Barbaro N, Origitano TC et al (2011) Fundamental skills for entering neurosurgery residents: report of a Pacific region "boot camp" pilot course, 2009. Neurosurgery 68:759–764. https://doi.org/10.1227/NEU.0b013e3182077969
Stienen MN, Bartek J Jr, Czabanka MA et al (2019) Neurosurgical procedures performed during residency in Europe-preliminary numbers and time trends. Acta Neurochir 161(5):843–853. https://doi.org/10.1007/s00701-019-03888-3
Stienen MN, Netuka D, Demetriades AK et al (2016) Neurosurgical resident education in Europe—results of a multinational survey. Acta Neurochir 158:3–15. https://doi.org/10.1007/s00701-015-2632-0
Stienen MN, Netuka D, Demetriades AK et al (2016) Working time of neurosurgical residents in Europe—results of a multinational survey. Acta Neurochir 158:17–25. https://doi.org/10.1007/s00701-015-2633-z
Takahashi M, Okudera H (2014) Neuroresuscitation simulation training courses in Japan. Neuroepidemiology 43(2):104. https://doi.org/10.1159/000369115
Thawani JP, Ramayya AG, Abdullah KG et al (2016) Resident simulation training in endoscopic endonasal surgery utilizing haptic feedback technology. J Clin Neurosci 34:112–116. https://doi.org/10.1016/j.jocn.2016.05.036
Ward M, Ward B, Abraham M et al (2019) The Educational Quality of Neurosurgical Resources on YouTube. World Neurosurg 130:e660–e665. https://doi.org/10.1016/j.wneu.2019.06.184
Acknowledgements
The authors thank Emma Schmidt for the artistic illustration in this paper.
Code availability
The code utilized for data visualization is available upon request.
Author information
Authors and Affiliations
Contributions
Study conception, design, and search strategy: L.B., W.L.B. Literature search, screening, and data extraction: L.B., R.P., N.N., M.A., L.M. Study screening conflict resolution: W.L.B. Data analysis, interpretation, manuscript production: L.B., R.P., W.L.B. All authors had full access to data included in this manuscript.
Corresponding author
Ethics declarations
Ethics approval
This article does not contain any studies with human participants performed by any of the authors.
Consent to participate
This declaration is not applicable to this study
Consent for publication
All authors approved this manuscript for publication.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
ESM 1
(DOCX 122 kb)
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Banko, L., Patel, R.V., Nawabi, N. et al. Strategies to improve surgical technical competency: a systematic review. Acta Neurochir 165, 3565–3572 (2023). https://doi.org/10.1007/s00701-023-05868-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00701-023-05868-0