Abstract
Background
The weakening of paraspinal muscles in the paravertebral area may play a role in developing central lumbar spinal stenosis, resulting in lower back discomfort.
Objective
The study thoroughly examined the correlation between the Oswestry Disability Index, Dural Sac cross-sectional area, Schizas grading Scale, Body Mass Index, and the cross-sectional areas of Erector Spinae, Multifidus, and Psoas muscles. The findings were also compared between patients with central Lumbar Spinal Stenosis and healthy individuals.
Study design
Retrospective monocentric observational study.
Methods
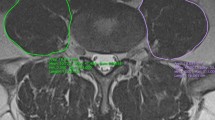
The study recruited 168 consecutive patients aged 60 or older diagnosed with central Lumbar Spinal Stenosis between January 2020 and July 2022. The patients’ condition was evaluated by administering a preoperative Oswestry Disability Index questionnaire, measuring their Body Mass Index, and performing preoperative Magnetic Resonance Imaging. The analyzed parameters were the cross-sectional area of paraspinal muscles at the L4-L5 level, dural sac cross-sectional area, and Schizas grading Scale at the most stenotic level, using multiple linear univariate analyses. Two groups of healthy individuals were recruited: Group A (under 60 years old) and Group B (over 60 years old). The same data extrapolated from these groups were compared with those of patients with central lumbar stenosis using a two-tailed Mann-Whitney test.
Results
As the Erector Spinae degenerates, the Oswestry Disability Index tends to increase. Similarly, an increase in Body Mass Index is often accompanied by a decrease in the cross-sectional area of the Erector Spinae. Low dural sac cross-sectional area is statistically linked to a reduced Multifidus cross-sectional area. Interestingly, the Schizas grading scale does not appear to correlate with changes in the cross-sectional area of the paraspinal muscles. Additionally, there is no significant difference in the cross-sectional area of the Psoas muscle between individuals with central lumbar spinal stenosis and healthy individuals.
Conclusions
Our study found that degeneration of the Erector Spinae plays a crucial role in the progression of perceived disability in Lumbar Spinal Stenosis. Prospective studies should investigate the long-term evolution of paraspinal muscles in decompressed patients.





Similar content being viewed by others
References
Abbas J et al (2016) Paraspinal muscles density: a marker for degenerative lumbar spinal stenosis? BMC Musculoskelet Disord 17:1–8
Backstrom KM, Whitman JM, Flynn TW (2011) Lumbar spinal stenosis-diagnosis and management of the aging spine. Man Ther 16(4):308–317
Bumann H et al (2020) Severity of degenerative lumbar spinal stenosis affects pelvic rigidity during walking. Spine J 20(1):112–120
Dahlqvist JR et al (2017) Fat Replacement of Paraspinal Muscles with Aging in Healthy Adults. Med Sci Sports Exerc 49(3):595–601
Fairbank JC, Pynsent PB (2000) The Oswestry disability index. Spine 25(22):2940–2953
Faur C et al (2019) Correlation between multifidus fatty atrophy and lumbar disc degeneration in low back pain. BMC Musculoskelet Disord 20(1):1–6
FM SP, Colares GM, Freire de Carvalho J (2021) High Prevalence of Metabolic Syndrome in Patients with Lumbar Spinal Stenosis: Association with Diabetes and Elevated Body Mass Index. Isr Med Assoc J 23(12):766–772
Fraser JF et al (2003) Pathogenesis, presentation, and treatment of lumbar spinal stenosis associated with coronal or sagittal spinal deformities. Neurosurg Focus 14(1):1–9
Han G et al (2021) Imaging evaluation of fat infiltration in paraspinal muscles on MRI: a systematic review with a focus on methodology. Orthop Surg 13(4):1141–1148
Kalichman, L., E. Carmeli, and E. Been, The association between imaging parameters of the paraspinal muscles, spinal degeneration, and low back pain. Biomed Res Int, 2017. 2017.
Katz JN, Harris MB (2008) Lumbar spinal stenosis. N Engl J Med 358(8):818–825
Kim H et al (2013) Asymmetry of the cross-sectional area of paravertebral and psoas muscle in patients with degenerative scoliosis. Eur Spine J 22:1332–1338
Korovessis PG, Stamatakis MV (1996) Prediction of scoliotic Cobb angle with the use of the scoliometer. Spine 21(14):1661–1666
Mehra A et al (2008) Oswestry Disability Index scoring made easy. Ann R Coll Surg Engl 90(6):497–499
Park MS et al (2018) Paraspinal muscles of patients with lumbar diseases. J Neurol Surg A Cent Eur Neurosurg 79(04):323–329
Ranger TA et al (2017) Are the size and composition of the paraspinal muscles associated with low back pain? A systematic review. Spine J 17(11):1729–1748
Salimi H et al (2021) Trunk muscle mass measured by bioelectrical impedance analysis reflecting the cross-sectional area of the paravertebral muscles and back muscle strength: a cross-sectional analysis of a prospective cohort study of elderly population. J Clin Med 10(6):1187
Schizas C et al (2010) Qualitative grading of severity of lumbar spinal stenosis based on the morphology of the dural sac on magnetic resonance images. Spine 35(21):1919–1924
Zaina F et al (2016) Surgical versus non-surgical treatment for lumbar spinal stenosis. Cochrane Database Syst Rev 1
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics approval
The ethical review process and approval by our ethics committee were not required for the present study because it is a retrospective study. Furthermore, the research data analysis has no effect on the participants and their medical care.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Conflict of interest
The authors declare no competing interests.
Additional information
Comments
The authors have chosen to include paraspinal - cross section area as a whole. If we consider carefully there may be different ratio of muscle fibres and fat, in the axial images of stenotic lumbar segment, in each patient. This aspect may influence the results of this study. Further sutdies should consider this aspect. In my opinion, hypotrophy of the erector spine muscle and the intermuscluar fat are factors that contribute to the instability and consequently progressive stenosis of that segment of vertebral column.
Ridvan Alimehmeti
Tirana, Albania
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Corazzelli, G., Capece, M., Meglio, V. et al. Multiple univariate analysis of radiologic and clinical features on 168 patients with lumbar spinal stenosis: what is the role of the erector spinae in the development of a patient’s disability?. Acta Neurochir 165, 3947–3957 (2023). https://doi.org/10.1007/s00701-023-05863-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00701-023-05863-5