Abstract
Background
The treatment of intracranial aneurysms has predominantly shifted towards endovascular strategies, but complex cases still necessitate microsurgery. Preoperative stimulation can be beneficial for inexperienced young neurosurgeons in preparing for safe microsurgery.
Method
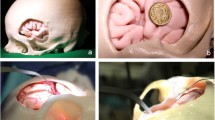
A 72-year-old female with a left irregular fetal posterior cerebral artery (PCA) aneurysm underwent clipping repair. Microsoft HoloLens 2, utilizing mixed reality technology, was employed for preoperative stimulation and anatomical study. During the operation, we successfully identified the planned relationship between the aneurysm and the fetal PCA. The patient was cured without any complications.
Conclusion
We hope that this report will highlight the significance of Microsoft HoloLens 2 in microsurgical planning and education.



Similar content being viewed by others
Data availability
N.A.
Code availability
N.A.
References
Golshani K, Ferrell A, Zomorodi A, Smith TP, Britz GW (2010) A review of the management of posterior communicating artery aneurysms in the modern era. Surg Neurol Int 1:88
Kikuta Y, Yamaguchi K, Ishikawa T, Funatsu T, Okada Y, Kawamata T (2021) Selection of approach and bypass for fetal-type posterior cerebral artery aneurysm: illustrative cases. J Neurosurg Case Lessons 1:CASE21240
Lambert SL, Williams FJ, Oganisyan ZZ, Branch LA, Mader EC Jr (2016) Fetal-type variants of the posterior cerebral artery and concurrent infarction in the major arterial territories of the cerebral hemisphere. J Investig Med High Impact Case Rep 4:2324709616665409
Lv X, Li Y, Yang X, Jiang C, Wu Z (2012) Potential proneness of fetal-type posterior cerebral artery to vascular insufficiency in parent vessel occlusion of distal posterior cerebral artery aneurysms. J Neurosurg 117:284–287
Ten Brinck MFM, Rigante L, Shimanskaya VE, Bartels R, Meijer FJA, Wakhloo AK, de Vries J, Boogaarts HD (2021) Limitations of flow diverters in posterior communicating artery aneurysms. Brain Sci 11
Funding
This study was sponsored by the Shanghai Municipal Alliance for Clinical Competence Improvement and Advancement in Neurosurgery (SHDC22021303), the Fujian Province Science and Technology Innovation Joint Fund (No. 2021Y9135), and the Pudong New Area Science and Technology Development Fund (No. PKX2020-R03).
Author information
Authors and Affiliations
Contributions
Xiaorong Yan, MD, PhD: Original draft, data collecting, writing—review and editing. Zhiyi Yuan, M.Eng: Conceptualization, writing—review and editing.
Zixiao Yang, MD, PhD: Data collecting, writing—review and editing.
Jianping Song, MD, PhD: Conceptualization, supervision, writing—review and editing, project administration.
Corresponding author
Ethics declarations
Ethics approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. The study was approved by Huashan Hospital Institutional Review Board (HIRB), Fudan University, Shanghai, China.
Consent to participate
Informed consent was obtained from the patient included in the study.
Consent for publication
It represents a video of a surgical case. The patient gave approval for this publication.
Competing interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Key points
1. Complex intracranial aneurysms that may not be safely treated with endovascular procedures still require microsurgical treatment.
2. The fetal PCA directly supplies the occipital lobe from anterior circulation, resulting in vascular insufficiency if occluded.
3. Microsurgical expertise remains necessary in developing countries where the cost of endovascular technologies is prohibitive.
4. In the case of a wide-neck fetal PCA aneurysm, endovascular coiling may have a higher risk of recurrence, and stenting may pose a risk of fetal PCA occlusion, making microsurgical clipping a preferred option.
5. Mixed reality technology may help simulate the surgical procedure and anatomy and teach surgical nuances.
6. Patients should be informed about the risks of intraoperative rupture, injury to the fetal PCA, and potential impairment to the oculomotor nerve.
7. Transcranial electrophysiological monitoring and ICGVA are essential adjunct tools during intracranial aneurysm microsurgery.
8. Extreme care must be taken not to occlude the proximal fetal PCA during aneurysm repair.
9. The irregular shape of the aneurysm may indicate adherence to the tentorium, requiring precise and fast clipping to avoid tearing the dome of the aneurysmal sac.
10. Intraoperative imaging and follow-up are necessary to confirm the aneurysm’s total occlusion and the fetal PCA’s patency.
Supplementary Information
Below is the link to the electronic supplementary material.
Supplementary file1 (52.7 MB)
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Yan, X., Yuan, Z., Yang, Z. et al. How I do it? Preoperative Microsoft HoloLens 2 planning-assisted surgical clipping of a fetal posterior cerebral artery aneurysm. Acta Neurochir 165, 3371–3374 (2023). https://doi.org/10.1007/s00701-023-05810-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00701-023-05810-4