Abstract
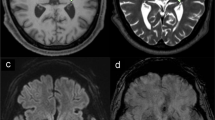
We report a patient with tremor-dominant Parkinson’s disease who had a mild cavitation bioeffect during magnetic resonance–guided focused ultrasound thalamotomy. During the aligning phase with low-energy sonication, cavitation caused mild dysarthria and paresthesia, prompting treatment cessation. At the same time, tremor and rigidity improved. MRI revealed extensive high-intensity lesions in the thalamus 1 day after the procedure followed by steroid infusion, which resulted in resolution of adverse events. Tremor and rigidity improved 1.5 years after the procedure. Although cavitation can relieve tremors and rigidity, it should be carefully monitored due to potential permanent adverse events by unpredictable and unknown behaviors.





Similar content being viewed by others
Abbreviations
- AC:
-
Anterior commissure
- DRTT:
-
Dentato-rubro-thalamic tract
- DTT:
-
Diffusion tensor tractography
- DWI:
-
Diffusion-weighted image
- FA:
-
Fractional anisotropy
- FUS:
-
Focused ultrasound
- GPi:
-
Globus pallidus interna
- MRgFUS:
-
Magnetic resonance–guided focused ultrasound
- MRI:
-
Magnetic resonance imaging
- PC:
-
Posterior commissure
- TDPD:
-
Tremor-dominant Parkinson’s disease
- T2WI:
-
T2-weighted image
- VIM:
-
Ventral intermediate nucleus
- Vc:
-
Ventral caudal nucleus
- Vo:
-
Ventro-oral nucleus
References
Arvanitis CD, Vykhodtseva N, Jolesz F, Livingstone M, McDannold N (2016) Cavitation-enhanced nonthermal ablation in deep brain targets: feasibility in a large animal model. J Neurosurg 124:1450–1459. https://doi.org/10.3171/2015.4.Jns142862
Bader KB, Vlaisavljevich E, Maxwell AD (2019) For whom the bubble grows: physical principles of bubble nucleation and dynamics in histotripsy ultrasound therapy. Ultrasound Med Biol 45:1056–1080. https://doi.org/10.1016/j.ultrasmedbio.2018.10.035
Chevillet JR, Khokhlova TD, Giraldez MD, Schade GR, Starr F, Wang YN, Gallichotte EN, Wang K, Hwang JH, Tewari M (2017) Release of cell-free microRNA tumor biomarkers into the blood circulation with pulsed focused ultrasound: a noninvasive, anatomically localized, molecular liquid biopsy. Radiology 283:158–167. https://doi.org/10.1148/radiol.2016160024
Elias WJ, Lipsman N, Ondo WG, Ghanouni P, Kim YG, Lee W, Schwartz M, Hynynen K, Lozano AM, Shah BB, Huss D, Dallapiazza RF, Gwinn R, Witt J, Ro S, Eisenberg HM, Fishman PS, Gandhi D, Halpern CH, Chuang R, Butts Pauly K, Tierney TS, Hayes MT, Cosgrove GR, Yamaguchi T, Abe K, Taira T, Chang JW (2016) A randomized trial of focused ultrasound thalamotomy for essential tremor. N Engl J Med 375:730–739. https://doi.org/10.1056/NEJMoa1600159
Gateau J, Aubry JF, Pernot M, Fink M, Tanter M (2011) Combined passive detection and ultrafast active imaging of cavitation events induced by short pulses of high-intensity ultrasound. IEEE Trans Ultrason Ferroelectr Freq Control 58:517–532. https://doi.org/10.1109/tuffc.2011.1836
Hardy J (2004) Historical background of stereotactic surgery: reflections on stereotactic surgery and the introduction of microelectrode recording in montreal. Neurosurgery 54:1508–1510. https://doi.org/10.1227/01.neu.0000125546.23705.22. (discussion 1510-1501)
Hynynen K (1991) The threshold for thermally significant cavitation in dog’s thigh muscle in vivo. Ultrasound Med Biol 17:157–169. https://doi.org/10.1016/0301-5629(91)90123-e
Jeanmonod D, Werner B, Morel A, Michels L, Zadicario E, Schiff G, Martin E (2012) Transcranial magnetic resonance imaging-guided focused ultrasound: noninvasive central lateral thalamotomy for chronic neuropathic pain. Neurosurg Focus 32:E1. https://doi.org/10.3171/2011.10.Focus11248
Jung NY, Park CK, Kim M, Lee PH, Sohn YH, Chang JW (2018) The efficacy and limits of magnetic resonance-guided focused ultrasound pallidotomy for Parkinson's disease: a Phase I clinical trial. J Neurosurg 1–9. https://doi.org/10.3171/2018.2.Jns172514
Khokhlova VA, Bailey MR, Reed JA, Cunitz BW, Kaczkowski PJ, Crum LA (2006) Effects of nonlinear propagation, cavitation, and boiling in lesion formation by high intensity focused ultrasound in a gel phantom. J Acoust Soc Am 119:1834–1848. https://doi.org/10.1121/1.2161440
Miller MW, Miller DL, Brayman AA (1996) A review of in vitro bioeffects of inertial ultrasonic cavitation from a mechanistic perspective. Ultrasound Med Biol 22:1131–1154. https://doi.org/10.1016/s0301-5629(96)00089-0
Nyborg WL (2001) Biological effects of ultrasound: development of safety guidelines. Part II: general review. Ultrasound Med Biol 27:301–333. https://doi.org/10.1016/s0301-5629(00)00333-1
Ohl CD, Arora M, Ikink R, de Jong N, Versluis M, Delius M, Lohse D (2006) Sonoporation from jetting cavitation bubbles. Biophys J 91:4285–4295. https://doi.org/10.1529/biophysj.105.075366
Tyler WJ (2011) Noninvasive neuromodulation with ultrasound? A continuum mechanics hypothesis. Neuroscientist 17:25–36. https://doi.org/10.1177/1073858409348066
Xu Z, Carlson C, Snell J, Eames M, Hananel A, Lopes MB, Raghavan P, Lee CC, Yen CP, Schlesinger D, Kassell NF, Aubry JF, Sheehan J (2015) Intracranial inertial cavitation threshold and thermal ablation lesion creation using MRI-guided 220-kHz focused ultrasound surgery: preclinical investigation. J Neurosurg 122:152–161. https://doi.org/10.3171/2014.9.Jns14541
Ye PP, Brown JR, Pauly KB (2016) Frequency dependence of ultrasound neurostimulation in the mouse brain. Ultrasound Med Biol 42:1512–1530. https://doi.org/10.1016/j.ultrasmedbio.2016.02.012
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection, and analysis were performed by Toshio Yamaguchi, Masayuki Nakano, Jinichi Sasanuma, Masahito Takasaki, Futaba Maki, Sakae Hino, Mayumi Kaburagi, Ken Iijima, Hirokazu Iwamuro, and Kazuo Watanabe. The first draft of the manuscript was written by Toshio Yamaguchi, and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethical approval
All procedures performed were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Consent to participate/consent to publish
The patient has consented to the submission of the case report for submission to the journal.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Yamaguchi, T., Nakano, M., Sasanuma, J. et al. Cavitation with low-energy sonication during focused ultrasound thalamotomy for a patient with tremor-dominant Parkinson’s disease: a potential risk. Acta Neurochir 165, 1195–1200 (2023). https://doi.org/10.1007/s00701-023-05551-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00701-023-05551-4