Abstract
Background
Transcranial anterior clinoidectomy is a conventional microsurgical approach for treatment of paraclinoid aneurysms. The endoscopic endonasal approach (EEA) is an alternative method for clipping intracranial aneurysms. No analysis has been conducted to anatomically compare approaches with respect to treating paraclinoid aneurysms. The surgical anatomical exposures of the paraclinoid region during transcranial extradural anterior clinoidectomy (EAC) and the endoscopic endonasal transplanum-cavernous approach (EETC) are described and quantitatively assessed.
Method
Seven cadaveric heads underwent EAC and EETC. Measurements included the area of exposure, volume of surgical freedom, angle of attack, ophthalmic artery (OphA) origin, and coronal exposure angle of the internal carotid artery (ICA).
Results
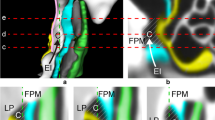
The EETC provided a larger area of exposure than the EAC (100.1±24.9 vs 76.1±12.9 mm2, p = 0.04). The EAC provided a higher volume of surgical freedom and greater angle of attack than the EETC in all neurovascular parameters, including the OphA, superior hypophyseal artery (SHA), distal ICA, and distal dural ring (all p < 0.001). The OphA origin was intradural in 85.7% and extradural in 14.3% of specimens. With regard to the coronal angle of exposure, the EAC exposed the OphA and SHA in the upper lateral quadrant (67.9±7.8° and 80.6±4.5°, respectively) and the distal ICA in the upper medial and upper lateral quadrants (92±7.5°). The EEA exposed the OphA, SHA, and distal ICA in the upper medial and lower medial quadrants (130.4±10.7°, 68.4±10.8°, and 58±11.4°, respectively).
Conclusions
The EAC and EETC each offer specific advantages for paraclinoid region exposure. The EAC is appropriate for paraclinoid aneurysms that occur at the dorsolateral surface of the paraclinoid ICA. The EETC is an alternative approach for aneurysms that occur along medial surface of the paraclinoid ICA (e.g., carotid cave and SHA aneurysms). The EETC provides greater surgical exposure to the medial aspect of the paraclinoid ICA.






Similar content being viewed by others
Data availability
The data supporting this study are available on request.
Code availability
N/A.
Abbreviations
- CSF:
-
Cerebrospinal fluid
- DDR:
-
Distal dural ring
- EAC:
-
Extradural anterior clinoidectomy
- EEA:
-
Endoscopic endonasal approach
- EETC:
-
Endoscopic endonasal transplanum-cavernous approach
- ICA:
-
Internal carotid artery
- IHA:
-
Inferior hypophyseal artery
- OphA:
-
Ophthalmic artery
- PCoA:
-
Posterior communicating artery
- SHA:
-
Superior hypophyseal artery
References
Barami K, Hernandez VS, Diaz FG, Guthikonda M (2003) Paraclinoid Carotid Aneurysms: Surgical Management, Complications, and Outcome Based on a New Classification Scheme. Skull Base 13:31–41
Cironi KA, Decater T, Iwanaga J, Dumont AS, Tubbs RS (2020) Arterial Supply to the Pituitary Gland: A Comprehensive Review. World Neurosurg 142:206–211
Daou B, Atallah E, Chalouhi N, Starke RM, Oliver J, Montano M, Jabbour P, Rosenwasser RH, Tjoumakaris SI (2018) Aneurysms with persistent filling after failed treatment with the Pipeline embolization device. J Neurosurg:1–7
Essayed WI, Singh H, Lapadula G, Almodovar-Mercado GJ, Anand VK, Schwartz TH (2017) Endoscopic endonasal approach to the ventral brainstem: anatomical feasibility and surgical limitations. J Neurosurg 127:1139–1146
Gardner PA, Vaz-Guimaraes F, Jankowitz B, Koutourousiou M, Fernandez-Miranda JC, Wang EW, Snyderman CH (2015) Endoscopic Endonasal Clipping of Intracranial Aneurysms: Surgical Technique and Results. World Neurosurg 84:1380–1393
Germanwala AV, Zanation AM (2011) Endoscopic endonasal approach for clipping of ruptured and unruptured paraclinoid cerebral aneurysms: case report. Neurosurgery 68:234–239; discussion 240
Horiuchi T, Tanaka Y, Kusano Y, Yako T, Sasaki T, Hongo K (2009) Relationship between the ophthalmic artery and the dural ring of the internal carotid artery. J Neurosurg 111:119–123
Houlihan LM, Naughton D, Preul MC (2021) Volume of Surgical Freedom: The Most Applicable Anatomical Measurement for Surgical Assessment and 3-Dimensional Modeling. Front Bioeng Biotechnol 9:628797
Kamide T, Burkhardt JK, Tabani H, Safaee M, Lawton MT (2020) Microsurgical Clipping Techniques and Outcomes for Paraclinoid Internal Carotid Artery Aneurysms. Oper Neurosurg (Hagerstown) 18:183–192
Kamide T, Tabani H, Safaee MM, Burkhardt JK, Lawton MT (2018) Microsurgical clipping of ophthalmic artery aneurysms: surgical results and visual outcomes with 208 aneurysms. J Neurosurg 129:1511–1521
Kassam AB, Gardner PA, Mintz A, Snyderman CH, Carrau RL, Horowitz M (2007) Endoscopic endonasal clipping of an unsecured superior hypophyseal artery aneurysm. Technical note J Neurosurg 107:1047–1052
Koutourousiou M, Fernandez-Miranda JC, Vaz-Guimaraes Filho F, de Almeida JR, Wang EW, Snyderman CH, Gardner PA (2017) Outcomes of Endonasal and Lateral Approaches to Petroclival Meningiomas. World Neurosurg 99:500–517
Kutty RK, Kumar A, Yamada Y, Kawase T, Tanaka R, Miyatani K, Higashiguchi S, Ravishankar V, Takizawa K, Kato Y (2020) Visual Outcomes after Surgery for Paraclinoid Aneurysms: A Fujita Experience. Asian J Neurosurg 15:363–369
Lai LT, Morgan MK, Snidvongs K, Chin DC, Sacks R, Harvey RJ (2013) Endoscopic endonasal transplanum approach to the paraclinoid internal carotid artery. J Neurol Surg B Skull Base 74:386–392
Lanzino G, Crobeddu E, Cloft HJ, Hanel R, Kallmes DF (2012) Efficacy and safety of flow diversion for paraclinoid aneurysms: a matched-pair analysis compared with standard endovascular approaches. AJNR Am J Neuroradiol 33:2158–2161
Martinez-Perez R, Hardesty DA, Silveira-Bertazzo G, Albonette-Felicio T, Carrau RL, Prevedello DM (2021) Safety and effectiveness of endoscopic endonasal intracranial aneurysm clipping: a systematic review. Neurosurg Rev 44:889–896
Matano F, Tanikawa R, Kamiyama H, Ota N, Tsuboi T, Noda K, Miyata S, Matsukawa H, Murai Y, Morita A (2016) Surgical Treatment of 127 Paraclinoid Aneurysms with Multifarious Strategy: Factors Related with Outcome. World Neurosurg 85:169–176
Matsukawa H, Tanikawa R, Kamiyama H, Tsuboi T, Noda K, Ota N, Miyata S, Takeda R, Tokuda S (2016) Risk Factors for Visual Impairments in Patients with Unruptured Intradural Paraclinoid Aneurysms Treated by Neck Clipping without Bypass Surgery. World Neurosurg 91:183–189
Montaser AS, Prevedello DM, Gomez M, Lima L, Beer-Furlan A, Servian D, Otto BA, Carrau RL (2020) Extended Endoscopic Endonasal Clipping of Intracranial Aneurysms: An Anatomic Feasibility Study. World Neurosurg 133:e356–e368
Nowicki KW, Johnson SA, Goldschmidt E, Balzer J, Gross BA, Friedlander RM (2020) Visual Evoked Potentials and Intraoperative Awakening in Ophthalmic Artery Sacrifice During Aneurysm Clipping: 2 Cases and Literature Review. World Neurosurg 139:395–400
Ota N, Petrakakis I, Noda K, Miyazaki T, Kondo T, Kinoshita Y, Kamiyama H, Tokuda S, Tanikawa R (2020) Predictor of Visual Impairment Following Paraclinoid Aneurysm Surgery: Special Consideration of Surgical Microanatomy Related to Paraclinoid Structures. Oper Neurosurg (Hagerstown) 20:45–54
Otani N, Mori K, Wada K, Tomiyama A, Toyooka T, Takeuchi S, Nakao Y, Yamamoto T, Arai H (2020) Limited Indications for Clipping Surgery of Paraclinoid Aneurysm Based on Long-Term Visual Morbidity. World Neurosurg 134:e153–e161
Otani N, Toyooka T, Mori K (2019) Surgery of Paraclinoid Aneurysm. In: July J, Wahjoepramono EJ (eds) Neurovascular Surgery: Surgical Approaches for Neurovascular Diseases. Springer Singapore Singapore, pp 105–115
Otani N, Toyooka T, Takeuchi S, Tomiyama A, Nakao Y, Yamamoto T, Wada K, Mori K (2018) Less Invasive Modified Extradural Temporopolar Approach for Paraclinoid Lesions: Operative Technique and Surgical Results in 80 Consecutive Patients. J Neurol Surg B Skull Base 79:S347–S355
Romani R, Elsharkawy A, Laakso A, Kangasniemi M, Hernesniemi J (2012) Complications of anterior clinoidectomy through lateral supraorbital approach. World Neurosurg 77:698–703
Silva MA, See AP, Dasenbrock HH, Patel NJ, Aziz-Sultan MA (2017) Vision outcomes in patients with paraclinoid aneurysms treated with clipping, coiling, or flow diversion: a systematic review and meta-analysis. Neurosurg Focus 42:E15
Silva MA, See AP, Khandelwal P, Mahapatra A, Frerichs KU, Du R, Patel NJ, Aziz-Sultan MA (2018) Comparison of flow diversion with clipping and coiling for the treatment of paraclinoid aneurysms in 115 patients. J Neurosurg:1–8
Tayebi Meybodi A, Borba Moreira L, Little AS, Lawton MT, Preul MC (2018) Anatomical assessment of the endoscopic endonasal approach for the treatment of paraclinoid aneurysms. J Neurosurg 131:1734–1742
Truong HQ, Borghei-Razavi H, Najera E, Igami Nakassa AC, Wang EW, Snyderman CH, Gardner PA, Fernandez-Miranda JC (2018) Bilateral coagulation of inferior hypophyseal artery and pituitary transposition during endoscopic endonasal interdural posterior clinoidectomy: do they affect pituitary function? J Neurosurg 131:141–146
Truong HQ, Lieber S, Najera E, Alves-Belo JT, Gardner PA, Fernandez-Miranda JC (2018) The medial wall of the cavernous sinus. Part 1: Surgical anatomy, ligaments, and surgical technique for its mobilization and/or resection. J Neurosurg 131:122–130
Unnithan AS, Omofoye O, Lemos-Rodriguez AM, Sreenath SB, Doan V, Zanation AM, Recinos P, Sasaki-Adams DM (2016) The Expanded Endoscopic Endonasal Approach to Anterior Communicating Artery Aneurysms: A Cadaveric Morphometric Study. World Neurosurg 89:26–32
Xiao LM, Tang B, Xie SH, Huang GL, Wang ZG, Zeng EM, Hong T (2018) Endoscopic Endonasal Clipping of Anterior Circulation Aneurysm: Surgical Techniques and Results. World Neurosurg 115:e33–e44
Yamada Y, Ansari A, Sae-Ngow T, Tanaka R, Kawase T, Kalyan S, Kato Y (2019) Microsurgical Treatment of Paraclinoid Aneurysms by Extradural Anterior Clinoidectomy: The Fujita Experience. Asian J Neurosurg 14:868–872
Acknowledgements
We thank the staff of Neuroscience Publications at Barrow Neurological Institute for assistance with manuscript preparation and David Naughton for the volume of surgical freedom calculation software.
Funding
This study was supported by funds from the Newsome Chair in Neurosurgery Research held by Dr. Preul at Barrow Neurological Institute and from the Barrow Neurological Foundation.
Author information
Authors and Affiliations
Contributions
TL, ST, IA, and MCP contributed to the study conception and design. Material preparation, data collection, and analysis were performed by TL, ST, IA, JHJ, and LMH. The first draft of the manuscript was written by TL and MCP. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval
This was a laboratory study. There is no research ethics committee involvement.
Consent to participate
The manuscript does not contain clinical studies or patient data.
Consent for publication
The manuscript does not contain clinical studies or patient data.
Conflict of interest
The authors declare no competing interests. This research was presented in part as an e-poster at the American Association of Neurological Surgeons 2021 virtual meeting, August 21–25, 2021.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Vascular Neurosurgery- Aneurysm
Rights and permissions
About this article
Cite this article
Loymak, T., Tungsanga, S., Abramov, I. et al. Extradural anterior clinoidectomy versus endoscopic transplanum-transcavernous approach to the paraclinoid region: quantitative anatomical exposure analysis. Acta Neurochir 164, 1055–1067 (2022). https://doi.org/10.1007/s00701-022-05172-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00701-022-05172-3